|
WHO Grade |
Histologic hallmark |
Molecular alteration |
Anatomic location |
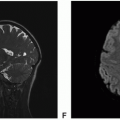
Imaging hallmark |
Meningothelial |
I |
Medium-sized epithelioid tumor cells, abundant eosinophilic cytoplasm; Epithelioid, largely uniform cells with oval nuclei forming lobules demarcated by collagenous septa |
Monosomy 22 |
Parasagittal |
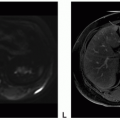
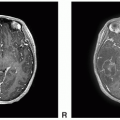
Most common subtype; classic imaging features-homogeneously enhancing dural based mass with isointense T1 and T2 signal |
Fibrous or fibroblastic |
I |
Spindle cells with intercellular collagen |
NF2
EMA |
Convexity |
Dark on T2 |
Transitional |
I |
Meningothelial, fibrous and transitional patterns; whorls and psammoma bodies; Lobular and fascicular foci of cells with conspicuous tight whorls and psammoma bodies |
NF2 |
Parasagittal |
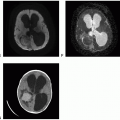
Partially calcified |
Psammomatous |
I |
Psammoma bodies, calcified masses; Confluent psammoma bodies replacing tumor cells and forming irregular calcified masses and bone |
– |
Thoracic spine |
Heavily calcified mass |
Angiomatous |
I |
Numerous blood vessels in greater proportion than tumor mass |
Aneuploid, polysomies chromo-somes 5,13,20 |
Convexity |
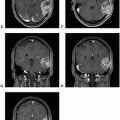
Marked tumor hypervascularity; prominent peritumoral edema |
Microcystic |
I |
Spider-like cells with long thin processes; Cells with thin, elongated processes encompassing microcysts and creating a cobweb-like background |
– |
Convexity |
Hyperintense on T2 & hypointense on T1; prominent peritumoral edema; micro- and macrocystic changes |
Secretory |
I |
Pseudo-psammoma bodies with acid-Schiff-positive eosinophilic secretions and immunoreactivity for carcinoembryonic antigen and cytokeratin |
KLF4 K409Q, TRAF7 mutations |
Skull base |
Prominent peritumoral edema |
Lymphoplasmacyte-rich |
I |
Dense infiltrates of lymphocytes & plasma cells; Chronic inflammatory infiltrates |
– |
Convexity, skull base, parasagittal, spine |
Markedly reduced on diffusion due to high cellularity |
Metaplastic |
I |
Focal or widespread mesenchymal components- cartilaginous/chondroid, osseous, lipomatous, xanthomatous, myxoid patterns |
– |
Convexity |
Scattered areas if calcium and fat within the tumor |
Chordoid |
II |
Physaliferous-like cells resembling chordoma; Cords or trabeculae of eosinophilic, vacuolated cells set in an abundant mucoid matrix |
– |
– |
High on T2 |
Clear cell |
II |
Polygonal cells with clear cytoplasm; prominent interstitial & perivascular hyalinization; pattern-less or sheeting architecture, glycogen-rich cytoplasm and prominent perivascular and interstitial collagen |
Switch/Sucrose non-fermentable (SWI/SNF) Related, Matrix Associated, Actin Dependent Regulator of Chromatin, Subfamily E, Member 1 mutations |
Spine, posterior fossa |
High on T2 with exuberant cystic architecture |
Atypical |
II |
Meningothelial cells invading into brain parenchyma; Increased mitotic activity, brain invasion with increased cellularity, small cells with a high nuclear-to-cytoplasmic ratio, prominent nucleoli, sheeting and foci of necrosis |
Loss: 1p, 6q, 10, 14q, 18q
Gain: 1q, 9q, 12q, 15q, 17q, 20q |
– |
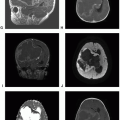
Irregular border with neighboring brain |
Papillary |
III |
Epithelioid tumor cells in a papillary or pseudopapillary pattern |
– |
Intraventricular, tuberculum sellae |
Lobular contour; lack of dural tail |
Rhabdoid |
III |
Rhabdoid cells with eccentric vesicular nuclei & prominent eosinophilic paranuclear inclusions |
SMARCB1 retained |
– |
Reduced on diffusion; marked peritumoral edema; irregular border with neighboring brain |
Anaplastic (malignant) |
III |
Cellular anaplasia and excessive mitoses |
LOSS: 22q, 1p, 6q, 10, 14q, 18q, 9p; NF2 & TERT mutations |
– |
Reduced on diffusion; irregular border with neighboring brain; metastases to lung or liver |