The primary goal of motion preservation surgery in the spine is to maintain normal or near normal motion in an attempt to prevent adverse outcomes commonly seen with conventional spinal fusion, most notably the development of adjacent-level degenerative disc disease. Several different surgical approaches have been developed to preserve motion in the lumbar spine, including total disc replacement, partial disc (nucleus) replacement, interspinous spacers, dynamic stabilization devices, and total facet replacement devices. The design of devices varies greatly. The devices are created using a similar rationale but are unique in design relative to their lumbar counterparts.
Key points
- •
The primary goal of motion preservation surgery is to maintain normal or near normal motion in an attempt to prevent adverse outcomes commonly seen with conventional spinal fusion, most notably the development of adjacent-level degenerative disc disease.
- •
There are several different approaches developed to preserve motion in the lumbar spine, including total disc replacement, partial disc (nucleus) replacement, interspinous spacers, dynamic stabilization devices, and total facet replacement devices.
- •
The design of lumbar total disc replacement devices varies greatly. Commonly seen complications include subsidence, migration, fracture, heterotopic ossification, and even adjacent-segment degeneration.
- •
Cervical motion preservation surgery primarily consists of total disc replacement. The devices are created using a similar rationale but are unique in design relative to their lumbar counterparts.
Discectomy and spinal fusion is considered the gold standard for the treatment of symptomatic degenerative disc disease. Though often effective in the short term, it is not without significant morbidity. Perhaps one of the most commonly recognized adverse outcomes of spinal fusion is the development of degenerative disc disease at the level(s) adjacent to a spinal fusion procedure.
Motion preservation surgery in the spine, while not a novel concept, has seen a significant increase in use during the last decade, particularly with respect to disc arthroplasty (total disc replacement) devices in the cervical and lumbar spine. The goal of motion preservation surgery, in general, is to closely replicate normal or near normal biomechanics in an effort to restore patient mobility and minimize the development of clinically significant adjacent-segment disc disease.
Although relatively new in the spine, motion preservation surgery is a well-established surgical technique in the appendicular skeleton, and the benefits of hip and knee joint replacement, among others, are clearly recognized. The spinal motion segment, or functional spinal unit, is more complex than the appendicular joints. The functional spinal unit is effectively composed of 3 joints: the disc space and 2 facet joints. As such, the relatively simple principles of replacing a single joint in the appendicular skeleton are not applicable, and the complex interaction among these 3 articulating components must be taken into consideration before surgical intervention. As a result, there is a vast array of devices available in spinal motion preservation surgery, particularly in the lumbar spine. In the lumbar spine, devices can be loosely grouped into anterior and posterior motion-preserving devices. Cervical motion preservation surgery presents with more limited options and mainly consists of total disc replacement (TDR).
In the lumbar spine, anterior motion preservation devices, or devices intended to replicate the normal motion of the disc space, include TDR and partial disc (nucleus) replacement. TDR is a well-established surgical technique with a multitude of devices available. Although cervical and lumbar TDR procedures are designed with the same rationale (ie, replace the abnormal disc while restoring near normal biomechanics), the devices are distinctly unique in design and, in many cases, the frequency and specific type of postoperative complications. In partial disc replacement, the diseased nucleus pulposus is replaced or augmented with an injectable or preformed device ( Fig. 1 ). The complex, preformed partial disc replacement devices require relatively invasive surgery while some of the injectable materials can be administered through a minimally invasive percutaneous approach. The goal of partial disc replacement is to increase disc space height and maintain near normal motion in an attempt to minimize the development of adjacent-segment disease.
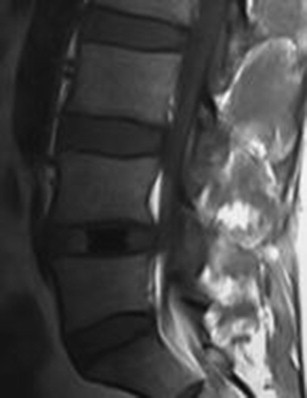
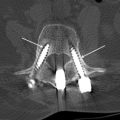
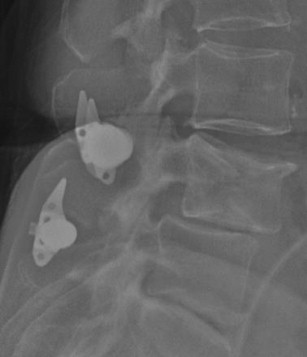
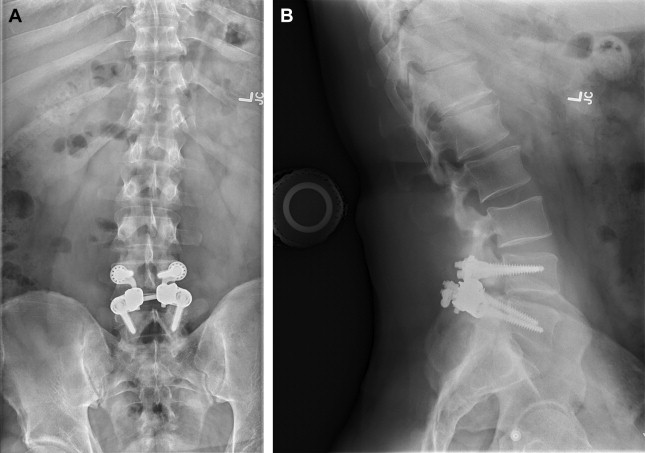
There are several types of posterior motion preservation devices, including interspinous spacers, dynamic stabilization screws and rods, and total facet replacement. Interspinous spacers ( Fig. 2 ) are devices placed between the spinous processes of adjacent levels. The primary goal of this procedure is to increase disc space height in an attempt to decrease canal stenosis and relieve neurogenic claudication. This procedure is relatively noninvasive, particularly in comparison with TDR, and typically does not preclude other types of surgery in the event of failure. Dynamic stabilization devices are similar to traditional pedicle screw-and-rod constructs in many aspects. These devices, however, are not rigid, allowing for a small amount of movement through mobile portions of the screws or rods. The goal of these devices is to stabilize the spine while simultaneously allowing for a small amount of motion. Facet replacement is a relatively invasive procedure whereby a laminectomy and bilateral facetectomy is performed and a prosthetic facet device implanted ( Fig. 3 ). The goal of facet replacement is to relieve canal and foraminal stenosis while maintaining some degree of motion at the affected level.
Motion preservation surgery of the spine is a complex, constantly evolving field. While the general principles of spinal motion preservation surgery remain relatively constant, many of the specific devices in use as recently as 2 to 3 years ago are no longer clinically available, having failed clinical trials, lost funding, or been simply deemed ineffective. New devices enter clinical trials every year. Given the dynamic nature of this field, the remainder of this article emphasizes TDR. TDR is the most commonly performed of the motion-preserving surgeries. There are many established cervical and lumbar TDR devices, several of which have been approved by the Food and Drug Administration (FDA) for clinical use in the United States. As a result, there are many large randomized controlled trials documenting the surgeries and comparing TDR with conventional fusion.
Lumbar total disc replacement
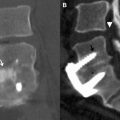
Lumbar TDR devices vary widely in shape and composition. Some, like the Charité device (DePuy Spine, Raynham, MA), have a 3-component design with metal endplates and a polyethylene liner. Others, like the FlexiCore device (Stryker Spine, Summit, NJ) are a 2-part, metal-only design that uses a ball-and-socket type articulation between the endplates. Some of the endplates of these devices are relatively flat and must use small “teeth” along the endplates to maintain purchase with the adjacent vertebral body; this is seen, for example, in the Charité device ( Fig. 4 ). Others, like the ProDisc-L device (Synthes Spine USA Products LLC, West Chester, PA), use large, vertical endplate keels to maintain purchase.
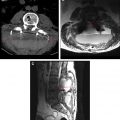
Most of these devices require an invasive anterior approach. The exception is NuVasive’s XL TDR (Nuvasive Manufacturing LLC, Fairborn, OH), which is implanted indirectly through a far-lateral approach ( Fig. 5 ). TDR surgeries in general are relatively invasive, and revision is often difficult in the event of hardware failure.
From an imaging standpoint it is important for the radiologist to be aware of the potential complications of TDR. In the immediate postoperative setting the radiologist should be able to identify surgical complications related to the approach. Most of these are implanted from an anterior approach, and complications including inadvertent peritoneal entry and vascular injury, though rare, can occur in the postoperative setting. In the case of the Nuvasive device a far-lateral approach is used, and the radiologist should search for retroperitoneal or inadvertent peritoneal complications related to the lateral approach. Other early complications include fracture of the vertebral body/endplates from aggressive implantation, and this should be investigated in the symptomatic postoperative patient ( Table 1 ).
| Early | Hemorrhage, vascular injury, infection, peritoneal entry, vertebral fracture |
| Late | Subsidence of implant, implant migration, heterotopic ossification, adjacent-level degenerative disc disease |
Chronic complications include subsidence, migration, and the development of heterotopic ossification and adjacent-level disease. Subsidence refers to the slow settling of the device into the endplates. Most of the surface area of the device will contact the softer bone located central to the outer ring apophysis. Subsidence is particularly prevalent in cases where implant is undersized and the footplate of the device is significantly smaller than the surface area of the adjacent vertebral body. Migration is relatively uncommon but can, like subsidence, occur in the setting of undersized devices. In cases of migration, the compressive forces of the vertebral bodies do not have sufficient strength to contain the device within the disc space. Migration is typically along the operative path, and migration into the paraspinal soft tissues or psoas muscle can potentially occur if a far-lateral approach is used. Many devices use endplate keels ( Fig. 6 ) or small teeth to minimize migration. Heterotopic ossification refers to the gradual development of heterotopic bone along the periphery of the interspace. Often this is asymptomatic, and is only significant from an imaging standpoint. With significant heterotopic ossification there can, in some cases, be limitation of the range of motion, and in severe cases there can even be bridging bone with autofusion.