Abstract
Patient-centered care is care organized around the patient, a model in which providers partner with patients and families to identify and satisfy patient needs and preferences. The Institute of Medicine highlighted the essential role of patient-centered care by including it as one of the committee’s six specific aims for improving healthcare. The committee’s motivation for including patient-centered care as a specific aim is well-documented patient frustration with “their inability to participate in decision-making, to obtain information they need, to be heard, and to participate in systems of care that are responsive to their needs.” Furthermore, improving the patient experience is one of the dimensions of the Institute for Healthcare Improvement’s triple aim to optimize health system performance. Recent changes in the healthcare landscape aimed at improving quality and decreasing costs are creating significant pressure on radiology practices to embed patient-centered principles in their hospital and outpatient facilities. In this chapter, we provide an overview of the dimensions of patient-centered care adapted to radiology with a discussion about opportunities to improve patient centeredness in radiology.
Keywords
Communication and health literacy, emotional support, fear and anxiety, patient-centered care, Patient comfort, respect, shared decision making
Introduction
The Institute of Medicine highlighted the essential role of patient-centered care by including it as one of the committee’s six specific aims for improving healthcare in Crossing the Quality Chasm (2001). In this report, patient-centered healthcare is defined as “providing care that is respectful of and responsive to individual patient preferences, needs, and values and ensuring that patient values guide all clinical decisions” and “encompasses qualities of compassion, empathy, and responsiveness to the needs, values, and expressed preferences of the individual patient.” The committee’s motivation for including patient-centered care as a specific aim is well-documented patient frustration with “their inability to participate in decision-making, to obtain information they need, to be heard, and to participate in systems of care that are responsive to their needs.” Patients are highly variable in their preferences, want to obtain information about their diagnosis and treatment, and often make their own decisions with guidance from their physicians. In this paradigm, it is clear that physicians cannot make the best decisions for their patients without providing information and including patients and their families in the decision-making process.
Patient-Centered Care in Radiology
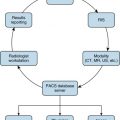
Redesigning processes to incorporate patient-centered principles in hospitals and outpatient imaging centers has received significant attention in the past several years, reflecting in part the growing need to improve patient satisfaction and demonstrate value in a healthcare system that is becoming more consumer and outcomes driven. Abujudeh’s Quality Process Map for radiology provides a visual framework that concentrates on the patient first when it comes to radiology processes ( Fig. 11.1 ). Providing a conceptual framework to help us understand the patient’s experience of illness and healthcare is a prerequisite to redesigning radiology-specific processes that take into account patients’ subjective experiences and measure satisfaction. In an effort to preserve the view that patient-centered radiology should be defined by patients , we will use the conceptual framework of patient-centered care provided by Gerteis et al. in which seven dimensions of patient-centered care are described based on extensive interviews and focus groups with patients, family members, physicians, and hospital staff.
- 1.
Respect for patients’ values, preferences, and expressed needs
- 2.
Coordination and integration of care
- 3.
Information, communication, and education
- 4.
Physical comfort
- 5.
Emotional support and alleviation of fear and anxiety
- 6.
Involvement of family and friends
- 7.
Transitions and continuity
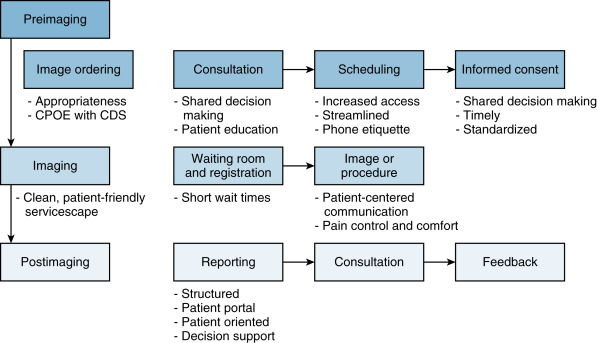
This chapter provides an overview of the first six dimensions of patient-centered care adapted to radiology followed by a discussion of opportunities to improve patient centeredness in radiology. Review and discussion of the dimension information, communication, and education are focused on communication, given the critical role of communication in promoting patient centeredness. The final dimension of patient-centered care, transitions and continuity , is not reviewed because imaging is generally considered a clinical support service, and there is limited applicability of this dimension to radiology.
Dimensions of Patient-Centered Radiology and Opportunities for Improvement
Respect for Patient Values, Preferences, and Expressed Needs
This dimension focuses on respecting patients as unique individuals. The patient’s experience of illness encompasses not only the discomfort associated with being ill but all the social and psychological consequences as well. Physicians focused on the objective tasks of diagnosis and treatment fail to adequately address the patients’ subjective experience of illness, and therein lies part of the cultural discord between patients and physicians. There are several components of this dimension: (1) involving patients in their care, which includes determining patient preferences for involvement in decision making, open discussion of alternative medical procedures, and providing information about the course of illness and prospect of recovery; (2) understanding and respecting patients’ therapeutic goals; and (3) understanding and respecting cultural beliefs and practices. These components form the foundation of patient-centered care and are broadly applicable to patient care in radiology.
Involving patients in their care can be accomplished by having radiologists or knowledgeable staff members engage in dialogue with patients about what to expect during imaging procedures and the risks and benefits of specific procedures with alternative options. A survey of patients at a cancer center indicated that 71% of patients would like explanatory brochures, 82% would like explanations from a member of the radiology team concerning the examination procedure, and 85% would like explanations from a member of the radiology team concerning possible risks. While 88% did not meet with the radiologist before the examination, 36% expressed a desire to meet with the radiologist to understand the purpose of the examination, to be reassured, and to tell the radiologist about painful zones. That proportion increased to 77% when asked if they wanted to meet with the radiologist after the examination primarily to avoid waiting for the results.
Understanding and respecting patients’ therapeutic goals is a concept that may not be considered by radiologists performing imaging studies. The critical role of patient preference in determining therapeutic goals is highlighted by a study of healthy volunteers asked to choose between radiation therapy and surgery to treat cancer of the larynx, revealing that 20% chose radiation to preserve speech even though it was associated with a significantly lower survival rate. Radiology departments may abdicate this important responsibility to referring physicians, routinely performing all imaging studies ordered with a “just do it” mentality. However, this mindset may not be consistent with patients’ goals and invariably leads to inappropriate and costly overutilization. Patients’ preferences and patient-defined outcomes can be incorporated into clinical practice guidelines, providing an opportunity for clinicians to place greater emphasis on patients’ therapeutic goals when considering treatment options.
One way to promote patient-centered care is for clinicians to practice within a shared decision-making model: decision making involves at least the health provider and the patient but may also involve family members, relatives, friends, and multiple health providers; all parties take steps to participate in the process of decision making; information sharing is requisite; and an agreed-upon shared treatment decision is made. Shared decision making involves using guided-discussion tools such as flowcharts, videotapes, and interactive presentations that organize the disease information and treatment outcomes in language that is understandable by the patient. This model should improve patients’ knowledge of options, perceptions of risks and benefits, and achieve clinical decisions that are consistent with patient values such as quality of life. This approach ensures that knowledge is shared and information flows freely between patients and radiologists, who should also strive to provide the best available scientific knowledge. Shared decision making should be practiced in every patient encounter to accommodate differences in patient preference.
Understanding and respecting cultural beliefs and practices plays a significant role in access and utilization of radiologic services, particularly for screening exams. Interventions that incorporate cultural competency have been shown to improve the quality of healthcare in minority or underserved populations, such as patient tracking and reminder systems, healthcare provider education, and offering screening services directly to patients rather than through physicians. Similar improvements have been achieved by incorporating cultural competency into the use of medical imaging for screening. Disparate breast cancer–related mortality and survival outcomes between Caucasian women and ethnic minorities have been attributed to several factors, one of which is culturally grounded beliefs that act as a barrier to participation in conventional screening mammography programs. Improvements in the utilization of screening mammography among Korean American women were achieved by using a culturally relevant intervention consisting of interactive educational sessions focused on breast cancer, early screening guidelines, and Korean cultural beliefs.
Coordination and Integration of Care
Patient concerns with coordination of clinical care typically relate to the sense that members of the clinical team are not communicating critical information to one another based on the inconsistency of the message the patient is receiving from different members of the clinical care team. In contrast, coordination of clinical support services presents a different set of challenges for radiologists because the primary customer of clinical support services is typically the referring physician. These services are usually valued by how quickly, accurately, and completely information about confirming or excluding a diagnosis is conveyed to the clinician. As a result, patients too often describe diagnostic and therapeutic procedures as painful or dehumanizing experiences. This particular problem is aptly described by Gilda Radner in her book, It’s Always Something , in which she describes her experience undergoing a barium enema during her struggle with cancer.
The technicians strapped me to a table and then put a tube in my rear end. As they poured a chalky liquid inside me and pumped gas into me so that my bowel would show up …, they were also turning me slowly around and around on the table. … I felt like I was trapped on an endless Ferris wheel with someone’s fist up my butt. You can image how much I enjoyed the barium enema. I think the word that best captures the whole event is humiliating …
A barium enema is considered a routine procedure by most radiologists, and this would have been the case with Gilda Radner as the study revealed nothing wrong. However, the factors that contribute to making the patient’s experience painful and humiliating are the assembly-line style of technicians who have not developed a relationship with the patient, inadequate explanation of the procedure, being left alone and scantily clothed in a hospital gown in waiting areas and hallways, and being told that it will not hurt when it most likely will cause pain or discomfort. It is important for providers to be acutely aware of the pain and discomfort patients experience during routine procedures and to adequately address the patient’s concerns prior to and during these procedures.
Fears that members of the clinical team are not passing along critical pieces of information to one another is another pervasive problem for radiologists. A lack of clinical history on radiology requisitions has been described as a universal problem for radiologists, and a systematic review evaluating the accuracy of diagnostic tests that are read with and without clinical information determined that clinical information improved test reading accuracy. When an important piece of information is lost or overlooked, patients see that the people taking care of them are uninformed, efforts are needlessly duplicated, procedures are delayed, and tasks are left undone. One of the greatest contributions an ordering provider can make to the radiologist’s interpretation is to provide relevant clinical information with the order. Although computerized provider order entry offers opportunities to improve clinical histories, implementation is far from perfect. As a result, healthcare providers in radiology must be vigilant in obtaining the clinical information necessary to provide accurate, high-quality interpretations for imaging examinations, which can be accomplished by interviewing patients, reviewing the electronic medical record or patient’s chart, and calling the referring physician’s office.
Communication
Effective communication between patients and caregivers addresses both technical and nontechnical aspects of healthcare. Communication about the technical aspects of care is restricted to facts, diagnoses, recommended treatments, and likelihood of recovery; in this realm, patients are less knowledgeable, more passive, and more vulnerable than providers. The nontechnical aspects of care are emphasized in patient-centered communication, which places the patient and provider on equal ground by engaging both in the discussion of deep feelings and subjective experiences. An important area for radiologists to promote patient-centered care is in the communication of imaging results directly to patients. The traditional pattern of communication through referring physicians as intermediaries devalues the patient-radiologist relationship, has the potential for delay or miscommunication, and contributes to significant (and often unnecessary) patient anxiety.
A survey of patients’ preferences in the disclosure of imaging findings shows a clear desire on the part of patients to hear the results of imaging examinations from the radiologist at the time of the procedure rather than hearing them later from the referring physician, regardless of the findings. Patients experience considerable anxiety waiting for the results of imaging procedures; half of the smokers undergoing lung cancer screening experienced discomfort waiting for results, whereas most patients undergoing imaging studies in a cancer center reported wanting to meet with the radiologist after the examination “to be reassured,” “to avoid waiting for the results,” “to have the preliminary results,” for “rapid results before the visit with the doctor,” and to know “if there is a problem.” Patients are entitled to know the results of their examination, and radiologists should provide a mechanism whereby patients can choose if they want their results delivered immediately by radiologists or available through a patient portal, although disclosing the results directly to the patient requires that the referring physician be notified promptly as well.
According to Reynolds, “Health care practitioners in any specialty must possess soft skills to provide patient-centered care.” Soft skills is a sociological term relating to an individual’s personality traits, social graces, communication skills, language, personal habits, friendliness, and optimism, which characterize one’s relationships with other people. The acronym AIDET (acknowledgment, introduce, duration, explanation, and thank you) represents a set of soft skills that can be used to improve communication between patients and healthcare providers in the radiology communication loop:
Acknowledgment : Greet and welcome the patient, apologize for delays, acknowledge concerns.
Introduce : Introduce yourself using your name and explain your role in the patient’s care.
Duration : Describe the time the patient can expect to wait for a test or procedure.
Explanation : Describe what is going to happen to the patient and what he or she can expect.
Thank You : Thank the patient for his or her cooperation and participation.
Examples of patient-centered communication skills include encouraging patients to talk about psychosocial issues, using the patient’s own words and language, using interruptions to reflect on the communication between physicians and patients, and providing information and counseling rather than asking questions and giving directions.
Language barriers contribute to health disparities in individuals with limited English proficiency and result in decreased patient satisfaction, decreased patient understanding of diagnosis and treatment, poorer adherence to treatment and follow-up for chronic illnesses, and increased medication complications. A systematic review by Karliner et al. indicates that the use of professional interpreters has positive benefits on communication with regard to errors and comprehension, use of clinical care, clinical outcomes, and satisfaction with care. According to Shams-Avari, “inexperienced interpreters have omitted questions about drug allergies; instructions for the dose, frequency and duration or antibiotics; and directions for rehydration fluids.” It is important to note that although patients may prefer to use friends or family members for medical interpretation, this practice leads to a higher frequency of errors that are significantly more likely to have clinical consequences.
Hearing and vision impairment introduce significant barriers to effective communication within the healthcare setting and require specific approaches to minimize the impact of these barriers. In a study of patients with hearing impairment, six themes revolving around ineffective communication were described. Strategies proposed by the study participants included having physicians inquire about which method of communication patients prefer and having patients repeat critical health information to identify potentially dangerous miscommunication. A study using focus groups and interviews with individuals who were blind or had low vision, some of whom were healthcare experts, identified barriers to effective care and concluded that using common courtesy and individualized communication techniques could improve healthcare experiences of blind and low-vision patients.
Health literacy is the ability to understand health information and to use that information to make good decisions about your health and medical care. Low or limited health literacy can affect a patient’s ability to fill out complex forms, locate providers and services, share personal information such as health history, manage chronic disease, and understand how to take medications. Low health literacy has been associated with higher rates of hospitalization, greater use of emergency care, lower receipt of mammography screening and influenza vaccines, poorer health status, higher mortality rates, and poorer use of healthcare services. In radiology, low health literacy could negatively impact a patient’s ability to appropriately complete contrast or magnetic resonance imaging screening forms, follow preparatory instructions prior to procedures such as a barium enema, or seek medical assistance when experiencing pain after an interventional procedure. Several strategies have been proposed to address issues related to low health literacy ( Box 11.1 ).
- •
Caregivers should focus on increasing patient recall and understanding.
- •
Information should be organized into logical blocks, and the main message should be simplified, made specific to the patient, repeated, and summarized.
- •
Patients’ understanding should be checked by asking them to repeat information in their own words.
- •
Patient-centered interviewing skills should be employed.
- •
Medical concerns should be placed in a personal context by explaining the effect of treatment on the patient’s daily activities.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree