Abstract
The Maintenance of Certification (MOC) program includes four parts. The fourth part is Practice Quality Improvement (PQI). The American Board of Radiology (ABR) lists several activities from which diplomates can choose in fulfilling the Part 4 requirements. A diplomate can complete PQI projects as an individual, in a group, or through an institution or organization. Completing at least one PQI project or activity is mandatory in each 3-year cycle. Diplomates who choose to do PQI projects may use any standard quality improvement methodology (including, but not limited to, plan-do-study-act [PDSA], Lean and Six Sigma, failure mode and effects analysis, and root cause analysis) to meet the MOC Part 4 requirements. Individual PQI projects consist of baseline and post-PQI PDSA cycles. Radiologists who choose to participate as a group should meet the standards for group PQI projects defined by the ABR. A few leading institutions have been approved by the ABR for MOC Part 4 credit. Quality improvement programs at these institutions encourage groups of multidisciplinary healthcare providers to participate together in projects of mutual interest. Implementing quality improvement projects can change the behavior of subjects. Investigators should be familiar with this phenomenon when performing and interpreting PQI projects.
Keywords
Maintenance of Certificate, Part 4 Maintenance of Certificate, practice quality improvement, quality and safety, quality improvement methodologies, practice quality improvement projects, practice quality improvement activities
Introduction
In 2012, the American Board of Radiology (ABR) implemented a new Maintenance of Certification (MOC) process, known as Continuous Certification, for all participating diplomates. Every year on March 15, the ABR looks back at the previous 3 years for each diplomate to consider if he or she is meeting the MOC requirements.
All diplomates who hold continuous certificates issued in 2012 or after or time-limited certificates are automatically enrolled in the MOC program when they obtain their certification. Diplomates who hold lifetime certificates may voluntarily enroll in the program to enter the MOC process. The MOC program is designed to continuously evaluate the following six essential competencies:
- 1.
Medical knowledge
- 2.
Patient care and procedural skills
- 3.
Interpersonal and communication skills
- 4.
Professionalism
- 5.
Practice-based learning and improvement
- 6.
Systems-based practice
The MOC program consists of four parts:
- 1.
Professional Standing
- 2.
Lifelong Learning and Self-Assessment
- 3.
Cognitive Expertise
- 4.
Practice Quality Improvement (PQI)
The ABR lists several activities in which diplomates can participate to fulfill the Part 4 requirements. Prior to 2016, completing at least one PQI project or activity was mandatory in each 3-year cycle. Currently, a PQI project is one of two activities that demonstrate the diplomate’s commitment to and participation in quality improvement, and thus to satisfying the ABR MOC Part 4 requirements. Diplomates who choose to do a PQI project may use any standard quality improvement methodology (including, but not limited to, plan-do-study-act [PDSA], Lean and Six Sigma, failure mode and effects analysis [FMEA], and root cause analysis) to meet the MOC Part 4 requirements. Participatory Quality Improvement Activities are also available in which the diplomate engages as a volunteer or by duty during his or her workday. These activities are reasonably expected to contribute directly to or increase the likelihood of advancement or improvement of quality and/or safety in healthcare at the local or national level. This chapter focuses primarily on the elements of a PQI project that satisfy the MOC Part 4 requirements.
Tools to Investigate Quality Problems in Radiology
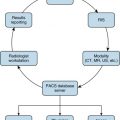
Several tools can help radiologists find opportunities to improve quality and safety in their practice. These tools include surveys, flowcharts or process maps, safety incident reporting or error reporting systems, chart reviews and investigation of compliance with national patient safety goals, analyzing radiology report addenda, and brainstorming with colleagues.
There are seven basic graphical tools that can be used to depict data: (1) flowcharts, (2) cause-and-effect analysis (Ishikawa or fishbone diagrams), (3) Pareto charts, (4) check or tally sheets, (5) control charts (Shewhart or statistical process charts), (6) histograms, and (7) scatter diagrams. Scorecards and dashboards are the tools to display the data and monitor the results.
Participatory Quality Improvement Activities
Candidates must document individual active participation in any of the activities listed in Box 6.1 to fulfill the criteria for MOC Part 4.
- •
Participation as a member of an institutional/departmental clinical quality and/or safety review committee. Examples include meaningful participation as a member responsible for creating, reviewing, and/or implementing clinical quality improvement safety activities; service as a radiation safety officer.
- •
Active participation in a departmental or institutional peer-review process, including participation in data entry and evaluation, the peer-review meeting process, or ongoing professional practice evaluation.
- •
Participation as a member of a root cause analysis team evaluating a sentinel or other quality- or safety-related event.
- •
Participation in at least 25 prospective chart rounds every year (peer review of the radiation delivery plans for new cases; radiation oncology and medical physics only).
- •
Active participation in submitting data to a national registry.
- •
Publication of a peer-reviewed journal article related to quality improvement or improved safety of the diplomate’s practice content area.
- •
Invited presentation or exhibition at a national meeting of a peer-reviewed poster related to quality improvement or improved safety of the diplomate’s practice content area.
- •
Regular participation (at least 10 per year) in departmental or group conferences focused on patient safety. Examples include regular attendance at tumor boards, morbidity and mortality conferences, diagnostic/therapeutic errors conferences, interprofessional conferences, surgical/pathology correlation conferences, etc.
- •
Creation or active management of, or participation in, one of the elements of a quality or safety program. Examples include a department dashboard or scorecard, a daily management system to ensure quality and safety, and a daily readiness assessment using a huddle system.
- •
A local or national leadership role in a national/international quality improvement program, such as “Image Gently,” “Image Wisely,” “Choosing Wisely,” or other similar campaign. Local participation roles include implementation and/or maintenance of, or adherence to, program goals and/or requirements.
- •
Completion of a peer survey (focused on quality or patient safety) and resulting action plan. The survey should contain at least five quality- or patient safety–related questions and have a minimum of five survey responses.
- •
Completion of a Patient Experience-of-Care survey with individual patient feedback. The survey should contain at least five quality- or patient safety–related questions and have a minimum of 30 survey responses.
- •
Active participation in applying for or maintaining accreditation by specialty accreditation programs such as those offered by the American College of Radiology (ACR) or the American Society for Radiation Oncology.
- •
Annual participation in the required Mammography Quality Standards Act medical audit or ACR Mammography Accreditation Program.
- •
Completion of a self-directed educational project on a quality- or patient safety–related topic (medical physics only).
- •
Active participation in a National Cancer Institute cooperative group clinical trial (for diagnostic radiologists, radiation oncologists, and interventional radiologists, entry of five or more patients in a year. For medical physicists, active participation in the credentialing activities).
Practice Quality Improvement Projects
The following are examples of PQI project topics:
- •
Improving report turnaround time
- •
Improving patient access (next available appointment)
- •
Optimizing radiation dose/examination or frequency of repeat examinations
- •
Improving the time-out process for procedures
- •
Decreasing wrong patient/wrong procedure events
- •
Standardizing reports
- •
Reducing magnetic resonance imaging safety events
- •
Improving critical results notification
- •
Improving care handoffs
Methodologies to Perform Quality Improvement Projects
Root Cause Analysis
Root cause analysis is an approach that identifies an error, how the error occurred, and why the error occurred to help determine actions to minimize or prevent its recurrence. This approach requires a team of four to 10 investigators who have different roles and backgrounds. For example, if the error occurred within a department, the investigators would come from that department and be related to the event that occurred. A fishbone (or cause-and-effect) diagram is usually used, and the five whys are asked to identify the root cause of the error. The team first answers the question, “Why did this happen?” After each answer, the question is then repeated at least four more times in an attempt to drill down to the root cause.
Root cause analysis can also be done for sentinel events. The Joint Commission defines a sentinel event as a safety event that affects a patient and results in death or major harm to that patient. Organizations are strongly encouraged to report sentinel events. The Joint Commission recommends 11 steps for performing root cause analysis of sentinel events. These steps are summarized in Fig. 6.1 .