▪ Pediatric Radiology As a Potential Career
Most pediatric radiologists are very happy with both their jobs and career choice. There are a number of attractive aspects about pediatric radiology. First, one of the most important elements of job satisfaction is the quality of the interactions one has with the people with whom one works. In general the physicians who choose to go into pediatric subspecialties, as well as other health care workers who choose to work at pediatric institutions, tend to be nice people. Aggressive, power-hungry people tend not to want to work with children. This makes a huge difference in the quality of daily life. In addition, pediatric subspecialists seem to rely on the opinions of pediatric radiologists more than many of their adult subspecialist counterparts. Similarly, pediatric radiology does not seem to have the same number of turf battles that many adult-oriented departments have.
Another unique feature of pediatric radiology is that one gets to be a “general specialist.” Pediatric radiology is a small part of medical imaging overall, and in this sense the pediatric radiologist is very much a subspecialist. Compared with general radiologists who must have a working knowledge of a daunting amount of information, most pediatric radiologists feel comfortable that they have an adequate command of the knowledge they need to provide outstanding care. At the same time, pediatric radiologists are generalists in the sense that many pediatric radiologists deal with all modalities and organ systems. They get the best of both worlds. It is also possible in pediatric radiology to become a sub-subspecialist, such as a pediatric neuroradiologist, pediatric interventional radiologist, pediatric cardiac imager, or pediatric fetal imager.
The most powerful and fulfilling aspect of becoming a pediatric health care provider is probably the satisfaction that comes from working with and for children. Few activities are more rewarding than helping children and their families. There are many other attractive aspects of pediatric care. First, most kids recover from their illnesses, as compared with elderly adults. Most pediatric illnesses are not self-induced. Pediatric diseases are highly varied and interesting. In addition, pediatric conditions are being increasingly recognized as important precursors to adult illnesses that cause significant morbidity and mortality—obesity, osteoporosis, and glucose intolerance. Finally, children and their families are highly appreciative of pediatricians’ help.
▪ Introduction: Special Considerations in Pediatric Imaging
Many issues are unique to the imaging of children as compared with that of adults. Imaging examinations that are easily carried out in adults require special adjustments to be successfully achieved in children. The rotating resident on a pediatric imaging rotation and the general radiologist who occasionally images children must be prepared to deal with these issues and to adjust imaging techniques to safely and successfully obtain imaging examinations. In this introductory chapter, several of the general issues that can arise when imaging children are addressed briefly.
Relationship Between Imager and Parents
In both pediatric and adult patient care situations, there are family members with whom the imager must interact. However, in the pediatric setting there are several unique features in the relationship among imager, patient, and family. When caring for children, communication more often takes place between the radiologist and parent than between the radiologist and patient. Obviously, communication directly with the child is also paramount to success. In addition, the degree of interaction between the imager and the child-parent unit may be greater in the pediatric setting than in the adult setting because of associated issues, such as the potential need for sedation, the need for consent from the parent rather than the child (if the child is a minor), and the need for intense explanation of the procedure on the levels of both the child and the parent. Most people are also much more inquisitive and protective when their children are involved. Because of these reasons, descriptions of what to expect during the visit to the imaging area may have to be more detailed when dealing with pediatric patients and their parents.
The stress level of parents when their child is or may be ill is immense, and such stress often brings out both the best and worst in people. Because of the intense bonds between most parents and their children, the relationship between imager and parents is most successful when the radiologist exercises marked empathy, patience, professionalism, and effective communication.
Professionalism and Effective Communication
It is interesting to note that in pediatric health care most of the complaints by parents and families are not related to technical errors; they are more commonly related to issues of professionalism and communication. Of reported parent complaints 30% are related to poor communication and unprofessional behavior. In addition, practicing effective communication has been shown to have multiple positive outcomes, including better patient outcome, decreased cost, increased patient and family satisfaction, and decreased chance of litigation in the presence of adverse events.
Although physicians are referred to as health care professionals, historically they have not received formal training in professionalism and communication, have had poor role models, and have been seen as individual practitioners rather than as members of health care teams. Radiology departments and individual radiologists must be proactive in making improvements in this area. Having a program to improve and standardize interactions with families can be helpful. Scripting expected interactions can help improve patient and family interactions, such as defining how physicians introduce themselves to patients and families (including stating positions and roles in the upcoming procedure), as well as behaviors to avoid (such as stating that the patient’s ordering physician does not know how to order or that one does not have time to talk to a referring physician because one is too busy). Scripting both the type of conversation and process in general is also very helpful for the delivery of difficult news, such as defining the process for communicating with the family when a child is diagnosed with a new tumor.
Inability to Cooperate
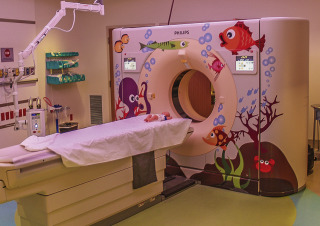
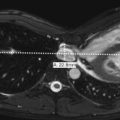
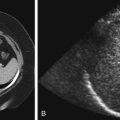
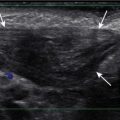
Infants and young children are commonly unable to cooperate with requirements that typically are easily met by adults. For example, they may be unable to keep still, remain in a certain position, concentrate for more than a brief moment, or breath-hold. Children of various ages have unique limitations. Infants and toddlers are unable to stay still, whereas 3-year-olds are more apt to refuse to cooperate. These limitations affect almost all pediatric imaging examinations: radiography, fluoroscopy, ultrasound, computed tomography (CT), magnetic resonance imaging (MRI), nuclear imaging, and interventional radiology. There are a number of potential solutions that can be helpful in these situations. Commonly employed techniques include distracting the child, providing child-friendly surroundings ( Figs. 1-1 through 1-7 ), immobilization, and sedation.