Valvular Disease
QUESTIONS
1 The Bernoulli equation is an example of the law of conservation of
A. Mass
B. Energy
C. Momentum
D. Charge
View Answer
1 Answer B. Bernoulli equation describes relationship between potential and kinetic energy. Energy can be transformed and cannot be created or destroyed. In the presence of vessel narrowing, the velocity distal to the point of narrowing must accelerate to maintain energy. Subsequently, a pressure gradient develops between the regions proximal and distal to the point of narrowing.
Reference: Miller SW. Cardiac imaging: the requisites. Philadelphia, PA: Mosby Elsevier, 2009.
2 The aortic valve has a systolic measured area of 0.7 cm2. How would you grade the severity of stenosis?
A. Normal
B. Mild
C. Moderate
D. Severe
View Answer
2 Answer D. Stenosis may be quantified using a variety of techniques including invasive hemodynamics and valve planimetry. However, the absolute value of valve area is not the primary determinant in timing of surgery, but presence/severity of clinical symptoms.
Severity grading:
Mild—Valve area exceeds 1.5 cm2; transvalvular velocity is 2.0 to 2.9 m/sec; and mean gradient is <20 mm Hg.
Moderate—Valve area is 1.0 to 1.5 cm2; transvalvular velocity is 3.0 to 3.9 m/sec; and mean gradient is 20 to 39 mm Hg
Severe—Valve area is <1.0 cm2; transvalvular velocity is ≥4 m/sec; and mean gradient is ≥40 mm Hg.
Reference: Pouleur A-C, le Polain de Waroux J-B, Pasquet A, et al. Planimetric and continuity equation assessment of aortic valve area: head to head comparison between cardiac magnetic resonance and echocardiography. J Magn Reson Imaging 2007;26(6):1436-1443. PMID: 17968960.
3 Enlargement of which cardiac structure would be the most reliable sign of pulmonary valve stenosis?
A. Right ventricle
B. Main pulmonary trunk
C. Main trunk and left pulmonary artery
D. Right and left pulmonary arteries
View Answer
3 Answer C. Enlargement of the right ventricle or the main pulmonary artery can occur in volume overload, pulmonary hypertension, or tricuspid valvular disease. Enlargement of the pulmonary trunk can also be seen in the setting of pulmonary stenosis. However, as blood crosses the stenotic pulmonic valve, there is acceleration in flow and asymmetric flow toward the left pulmonary artery with resulting asymmetric enlargement of the left pulmonary artery. Because the right pulmonary artery originates at a 90-degree angle from the main pulmonary artery, it is not exposed to this accelerated flow.
Reference: Chen JJ, Manning MA, Frazier AA, et al. CT Angiography of the cardiac valves: normal, diseased, and postoperative appearances. Radiographics 2009;29(5):1393-1412. PMID: 19755602.
4 Which of the following valvular abnormalities have the worst acute prognosis?
A. Bicuspid aortic valve
B. Drug-induced tricuspid valvulopathy
C. Infarcted papillary muscle with rupture
D. Multivalvular rheumatic fever
View Answer
4 Answer C. All of the other clinical scenarios are related to chronic valvular disease. Patients in this setting will typically have complaints of progressive dyspnea. Infarction of the papillary muscle with rupture, in the setting of myocardial infarction or trauma, is associated with acute mitral insufficiency, shortness of breath, florid pulmonary edema, significant hemodynamic compromise, and death.
Reference: Pawale A, El-Eshmawi A, Torregrossa G, et al. Ruptured papillary muscle causing acute severe mitral regurgitation. J Card Surg 2013;28(6):707. PMID: 23898857.
5 Which is the most common cause of mitral stenosis worldwide?
A. Rheumatic heart disease
B. Myxomatous degenerative disease
C. Carcinoid syndrome
D. Congenital mitral stenosis
View Answer
5 Answer A. Rheumatic heart disease (RHD) is the most common cause of mitral valve stenosis, particularly in the developing world. It usually originates as a streptococcal infection of the upper respiratory tract (rheumatic fever). Acute RHD produces a pancarditis, characterized by endocarditis, myocarditis, and pericarditis. Chronic RHD is characterized by repeated valvular inflammation with subsequent leaflet thickening, commissural fusion, and shortening and thickening of the tendinous cords.
Congenital mitral stenosis is very rare. Carcinoid valvulopathy affects primarily tricuspid and pulmonary valves. Myxomatous degeneration results in mitral valve prolapse and insufficiency.
Reference: Hughes S. Valvular heart disease. In: Suvarna SK (ed.). Cardiac pathology. London: Springer, 2013:147-161.
A. Mitral valve prolapse
B. Annular dilation
C. Congenital mitral stenosis
D. Infective endocarditis
View Answer
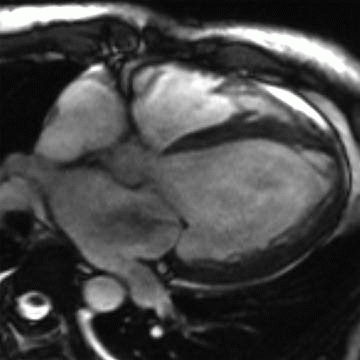
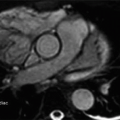
6 Answer B. Balanced steady-state free precession image demonstrates left ventricular enlargement and mitral insufficiency arising centrally from the valve. The valve leaflets are otherwise unremarkable without evidence of thickening, vegetation, or prolapse. Ventricular dilation commonly leads to subsequent annular dilatation and functional insufficiency.
The mitral valve requires coordinated function of the left atrium, mitral annulus, leaflets, papillary muscles, and left ventricle. Mitral insufficiency often results from dysfunction of one or more of these components. In the setting of ischemic cardiomyopathy, mitral annular dilation is frequently associated with alterations in the subvalvular apparatus and regional or global LV dysfunction. Isolated annular dilatation does not usually result in moderate or severe mitral insufficiency.
Reference: Otsuji Y, Kumanohoso T, Yoshifuku S, et al. Isolated annular dilation does not usually cause important functional mitral regurgitation. J Am Coll Cardiol 2002;39(10):1651-1656.
7 Which is the most common cause of pulmonic stenosis?
A. Congenital stenosis
B. Rheumatic disease
C. Degenerative thickening
D. Carcinoid syndrome
View Answer
7 Answer A. Pulmonary stenosis is a congenital disorder in 95% of cases and most often an isolated abnormality. Pulmonary stenosis can also be observed as a component of complex congenital heart disease such as tetralogy of Fallot. Acquired pulmonary stenosis whether degenerative or inflammatory is exceedingly rare. Carcinoid syndrome is also rare and typically causes valvular insufficiency.
Reference: Chen JJ, Manning MA, Frazier AA, et al. CT angiography of the cardiac valves: normal, diseased, and postoperative appearances. Radiographics 2009;29(5):1393-1412. PMID: 19755602.
8 Rheumatic disease involving the aortic valve is most commonly associated with
A. Aortic insufficiency
B. Isolated involvement
C. Bicuspid aortic valve
D. Aortic stenosis
View Answer
8 Answer D. Rheumatic heart disease may result in aortic stenosis or mixed stenosis and insufficiency. Rheumatic involvement of the mitral valve always precedes aortic involvement. Isolated aortic valve disease is very uncommon. Although insufficient valvular disease may result from calcification and fixed positioning of the valve leaflets, most cases of valvular insufficiency are related to damage to the valve leaflets or supporting apparatus.
Bicuspid aortic valves demonstrate early degeneration of the valve leaflets leading to fusion of the commissures, valvular sclerosis, and significant aortic stenosis similar to what one may see in rheumatic heart disease. However, the two entities are not closely associated.
References: Chen JJ, Manning MA, Frazier AA, et al. CT angiography of the cardiac valves: normal, diseased, and postoperative appearances. Radiographics 2009;29(5):1393-1412. PMID: 19755602.
Hughes S. Valvular heart disease. In: Suvarna SK (ed.). Cardiac pathology. London: Springer, 2013:147-161.
9 The classic diagnostic criteria for mitral valve prolapse include displacement of the mitral leaflets of
A. >1 mm beyond the annulus into the left ventricle and leaflet thickening of >3 mm
B. >5 mm beyond the annulus into the left ventricle and leaflet thickening of >2 mm
C. >3 mm beyond the annulus into the left atrium and leaflet thickening of >1 mm
D. >2 mm beyond the annulus into the left atrium and leaflet thickening of >5 mm
View Answer
9 Answer D. Mitral valve prolapse is most commonly caused by myxomatous degeneration of the valve leaflets. This is grossly characterized by thickening and redundancy of the leaflets, as well as chordal elongation and annular dilation. Echocardiographic mitral valve prolapse has since been defined as single or bileaflet prolapse at least 2 mm beyond the long-axis annular plane. Prolapse with thickening of the valve leaflets >5 mm is termed “classic” prolapse, whereas prolapse with lesser degrees of leaflet thickening is regarded as “nonclassic prolapse.”
Reference: Hayek E, Gring CN, Griffin BP. Mitral valve prolapse. Lancet 2005;365(9458):507-518.
10 Complications in infective endocarditis of the aortic valve include
A. Cardiac arrhythmias
B. Septic pulmonary emboli
C. Valvular stenosis
D. Rasmussen aneurysm
View Answer
10 Answer A. The complications of infective endocarditis (IE) depend on the virulence of the organism and may include cusp perforation, chordal rupture, aneurysmal bulging of the valve, and perivalvular abscess formation. Uncommonly, this may result in a fistulous connection between major vessels and cardiac chambers or between chambers themselves resulting into congestive heart failure. Infection extending beyond valvular tissue may also result in disruption of the conduction system with electrocardiographic conduction abnormalities and arrhythmias.
Stenosis due to IE is uncommon. Septic pulmonary emboli and Rasmussen aneurysms are complications of right-sided cardiac valves.
Reference: Karchmer CM. Infectious endocarditis. In: Bonow RO, Braunwald E (eds.). Braunwald’s heart disease: a textbook of cardiovascular medicine. Philadelphia, PA: Saunders, 2012:1540-1560.
11 Patient presents with severe left atrial enlargement and new atrial fibrillation. Given the clinical history and imaging findings, what hemodynamic consequences can occur?
|
A. Elevated right atrial pressure
B. Blunting of hepatic vein waveforms
C. Blunting of pulmonary venous waveforms
D. Increased pulmonary arterial flow
View Answer
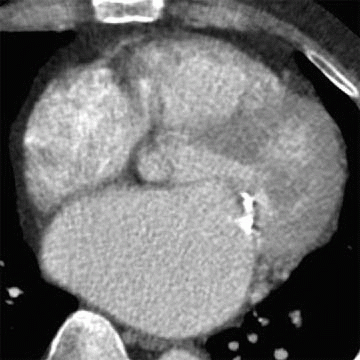
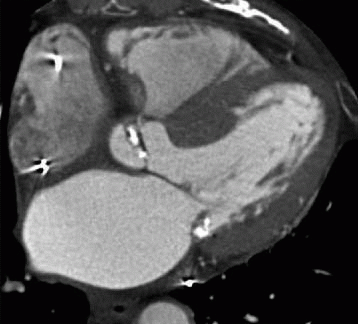
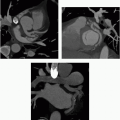
11 Answer C. Contrast-enhanced CT demonstrates significant mitral valve calcification and marked left atrial enlargement consistent with mitral stenosis.
Severe mitral stenosis results in a significant increase in left atrial pressure. This pressure is reflected backward, causing blunting of pulmonary venous waveforms and an increase in pulmonary venous, capillary, and arterial pressures and resistance. Ultimately, pulmonary hypertension develops which then eventually leads to right ventricular hypertrophy and enlargement, tricuspid regurgitation, increased right atrial pressure, and the development of right-sided heart failure.
Reference: Otto CM, Bonow RO. Valvular heart disease. In: Bonow RO, Braunwald E (eds.). Braunwald’s heart disease: a textbook of cardiovascular medicine. Philadelphia, PA: Saunders, 2012:1468-1539.
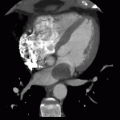
12 After obtaining a preoperative contrast-enhanced CT, an abnormality was incidentally noted on the aortic valve (below). Patient has no history of endocarditis or septicemia.
|
Given the clinical history and imaging findings, the most likely etiology would be
A. Fibroma
B. Metastasis
C. Rhabdomyosarcoma
D. Papillary fibroelastoma
View Answer
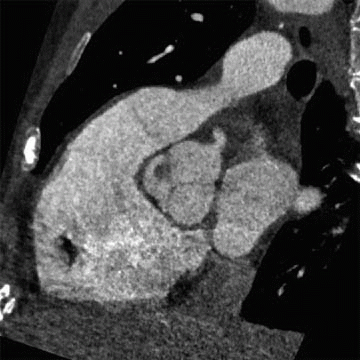
12 Answer D. MPR of cardiac-gated CT of the chest demonstrates a small well-circumscribed lesion on the aortic valve.
Papillary fibroelastomas are the third most common primary cardiac tumor in adults and the most common tumor of the cardiac valves. Papillary fibroelastomas can become quite large and occur on any valve surface or area of the endocardium. Histologically, they are composed of a core of myxoid connective tissue containing abundant mucopolysaccharide matrix and elastic fibers that is covered by a surface endothelium. Recurrences are rare, and valve-sparing surgery should be considered whenever possible, as regrowth of partially resected lesions does not always occur.
The remaining pathologies rarely involve the valves primarily.
Cardiac rhabdomyomas are the most frequently encountered primary cardiac tumor in infants and children. Cardiac rhabdomyoma arises more commonly in the ventricles, although up to 30% of cases can involve either atrium.
Patients with tuberous sclerosis have a 40% to 86% incidence of cardiac rhabdomyomas so it is an important association to screen for.
Fibromas of the heart are connective tissue tumors derived from fibroblasts and are very similar to soft tissue fibromas. About 90% of the reported cases occur in children before the age of 1 year, although fibromas can occur in any age group. Fibromas are associated with Gorlin syndrome in which patients develop odontogenic cysts, epidermal cysts, multiple nevi, and basal cell carcinomas of the skin.
Reference: Burke A, Jeudy J, Virmani R. Cardiac tumours: an update. Heart 2008;94(1):117-123.
13 A 59-year-old with chronic mitral insufficiency now presents with acute decompensation and pulmonary edema.
|
What is the most likely diagnosis?
A. Flail leaflet
B. Rheumatic mitral valve disease
C. Mitral stenosis
D. Mitral valve prolapse
View Answer
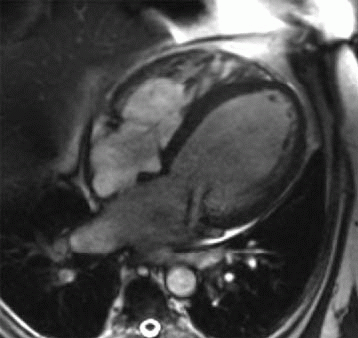
13 Answer A. Balanced steady-state free precession (b-SSFP) cardiac MR demonstrates prolapse of the anterior mitral leaflet into the left atrium consistent with a flail leaflet. This is typically secondary to rupture of a component of the mitral valve tensor apparatus (chordae tendineae and papillary muscles).
Leaflet prolapse and elongated chordae are common in degenerative mitral valve disease. Superimposed chordal rupture may develop from chronic damage resulting in a flail segment and associated severe mitral insufficiency.
Reference: Otto CM, Bonow RO. Valvular heart disease. In: Bonow RO, Braunwald E (eds.). Braunwald’s heart disease: a textbook of cardiovascular medicine. Philadelphia, PA: Saunders, 2012:1468-1539.
A. Flail leaflet
B. Rheumatic mitral valve disease
C. Mitral valve prolapse
D. Mitral regurgitation
View Answer
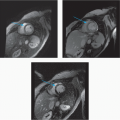
14 Answer B. CT of the chest demonstrated thickening and calcification of both mitral and aortic valve leaflets, most consistent with rheumatic heart disease.
Rheumatic fever is an immunologically mediated, multisystem inflammatory disorder that occurs after an episode of group A streptococcal pharyngitis. A rheumatic carditis occurs during the active phase of rheumatic fever and may progress over time to chronic rheumatic heart disease. Significant valve thickening and commissural fusion and thickening of the chordae tendineae are characteristic by histology.
The mitral valve is most commonly affected in 65% to 70% of cases and along with the aortic valve in another 25% of cases. Tricuspid valve involvement is infrequent, and the pulmonary valve is very rarely affected.
Reference: Schoen FJ, Mitchell RN. The heart. In: Kumar V, Abbas AK, Fausto N, et al. (eds.). Robbins and Cotran pathologic basis of disease. Saunders, 2009:529-588.
15 A 36-year-old man with severe aortic calcification and valvular stenosis is referred for preoperative coronary CT angiography. Which of the following CT imaging findings are most likely to be observed?
A. Asymmetric LV hypertrophy
B. Normal aortic valve area
C. Left atrial enlargement
D. Bicuspid valve
View Answer
15 Answer D. The abnormal morphology of a bicuspid aortic valve (BAV) results in valvular dysfunction and hemodynamic derangements. Echocardiographic studies have shown that sclerosis of the aortic cusps begins as early as the second decade of life while calcification becomes prominent in most middle-aged patients. This early degeneration may be related to more aggressive inflammatory changes of the aortic valve, characterized by increased macrophage infiltration and neovascularization.
Chronic aortic stenosis leads to ventricular pressure overload and concentric left ventricular hypertrophy will increased wall thickness and normal LV chamber size.
With worsening AS, diastolic dysfunction with impaired relaxation and increased diastolic filling pressure may result. This can lead to left atrial dilatation; however, this is a late finding in the progression of the disease.
Reference: Losenno KL, Goodman RL, Chu MWA. Bicuspid aortic valve disease and ascending aortic aneurysms: gaps in knowledge. Cardiol Res Pract 2012;2012:16. PMCID: PMC3503270.
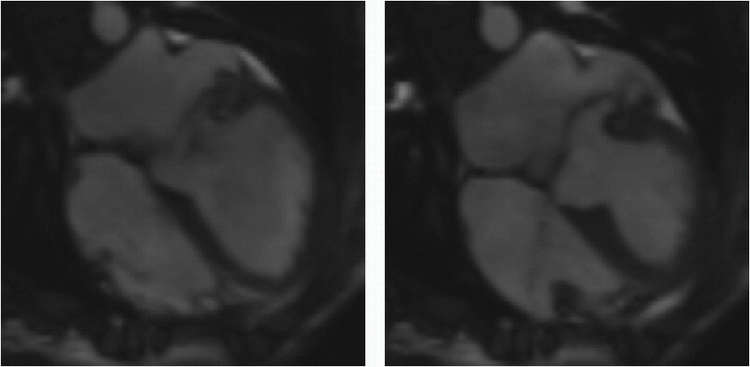
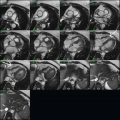
16 Horizontal long-axis images from a cardiac MR demonstrating end-diastolic (left) and end-systolic (right) MR images of the mitral valve.
|
What is the most likely diagnosis?
A. Flail leaflet
B. Rheumatic mitral valve disease
C. Mitral stenosis
D. Mitral valve prolapse
View Answer
16 Answer D. Balanced steady-state free precession images in the horizontal long axis demonstrate thickening and redundancy of the mitral valve at end diastole (left). End-systolic images (right) show prolapse of the leaflets beyond the annular plane and into the left atrium, consistent with mitral valve prolapse.
Mitral valve prolapse (MVP) is defined as single or bileaflet prolapse at least 2 mm beyond the long-axis annular plane, with or without thickening of the valve leaflets. The prevalence of prolapse is estimated at 2% to 3% and is equally distributed between men and women. Uncommonly, MVP is associated with heritable disorders of connective tissue including Marfan syndrome.
Although the great majority of persons with MVP have no untoward effects, approximately 3% develop one of four serious complications: (1) infective endocarditis, (2) mitral insufficiency, (3) stroke or other systemic infarct, or (4) arrhythmias, both ventricular and atrial.
References: Hayek E, Gring CN, Griffin BP. Mitral valve prolapse. Lancet 2005;365(9458): 507-518.
Schoen FJ, Mitchell RN. The heart. In: Kumar V, Abbas AK, Fausto N, et al. (eds.). Robbins and Cotran pathologic basis of disease. Saunders, 2009:529-588.
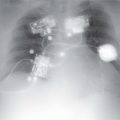
17 An 86-year-old patient with severe aortic stenosis undergoes transcatheter aortic valve implantation. The postoperative course was largely uncomplicated; however, a new left bundle branch block is observed on telemetry. Which of the following is the most likely etiology?
A. Cardiac sarcoidosis
B. Complication of TAVI surgery
C. Acute myocardial infarction
D. Drug toxicity
View Answer
17 Answer B. Transcatheter aortic valve implantation (TAVI) has become an established treatment option for patients with aortic stenosis at prohibitive risk to undergo conventional surgical aortic valve replacement. Among potential complications that may arise with TAVI surgery, new conduction abnormalities and arrhythmias frequently occur.
New left bundle branch block has been reported in 29 to 65% of patients after Medtronic CoreValve system and in 4% to 18% of patients receiving the balloon-expandable Edwards SAPIEN valve. In the PARTNER study, new-onset atrial fibrillation was present in 41% of patients acutely after TAVI and 9% within 30 days from the procedure.
Reference: van der Boon RMA, Houthuizen P, Nuis R-J, et al. Clinical Implications of conduction abnormalities and arrhythmias after transcatheter aortic valve implantation. Curr Cardiol Rep 2013;16(1):1-7.
18 What are the pathologic features that are associated with mitral stenosis?
A. Commissural fusion with subvalvular shortening of chordae
B. Myxomatous degeneration of the valve leaflets
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree