BELL PALSY: ACUTE ONSET PERIPHERAL FACIAL NERVE PALSY WITH NO APPARENT CAUSE
KEY POINTS
- The acute onset of a peripheral facial nerve palsy does not require magnetic resonance imaging or computed tomography study.
- Peripheral facial nerve palsy that presents with a different timetable, recurs, has associated spasticity, or does not recover requires very detailed magnetic resonance and computed tomography studies of the facial nerve to search for a structural lesion that is very likely to be present in those atypical settings for Bell palsy.
- Imaging can be very helpful to triage patients with peripheral facial nerve palsy to the next best step in the diagnostic process when the presentation is atypical for Bell palsy.
INTRODUCTION
Etiology
Bell palsy is likely to be a viral neuritis or an ischemic event incited by nerve swelling due to an inflammatory viral neuritis. There is substantial indirect evidence of this etiology, and it seems to be the most likely cause.
Prevalence and Epidemiology
This is a relatively common sporadic disease that is more common in adults than in children.
Clinical Presentation
The patient suffers an acute onset of a partial or complete peripheral (all of the muscles on one side of the face) facial nerve palsy. There may be associated periodic pain. There are typically no other signs or symptoms except for a possible zoster outbreak in the external auditory canal or conchal bowl. In particular, there must be no other signs of central nervous system disease, more particularly including those suggesting an abnormality in the cerebellopontine angle.
Bell palsy must never be confused with a facial nerve palsy of slow, progressive, or “stuttering” onset. Also, recurrent or persistent peripheral facial nerve palsy or palsy associated with spasticity should not be considered a “Bell palsy” until it is proven by a very carefully executed imaging evaluation not to be due to a structural lesion of the facial nerve. The presence of other cranial neuropathies might be found with facial palsy due to zoster infection, but multiple neuropathies also heighten concern of a structural compressive and/or infiltrative lesion.
PATHOPHYSIOLOGY
Anatomy
A diligent search of the entire course of the facial nerve is essential for evaluating imaging studies performed in patients with suspected Bell palsy, which is a diagnosis of exclusion only. It relies on excluding causative structural compressive and/or infiltrative lesion pathology with a high degree of confidence except for minor nerve swelling or enhancement that may be detected as evidence of nerve inflammation.
The computed tomography (CT) and magnetic resonance (MR) anatomy of the facial nerve must be completely understood, including its brain stem nucleus, course through the brain stem, its cisternal segment, its course through the internal auditory canal and entire facial canal, and its entire course and distribution beyond the stylomastoid foramen. One must also understand the normal range of perineural facial nerve vascular plexus enhancement from the first genu to the stylomastoid foramen. This anatomy is presented in detail in Chapter 104 (Figs. 104.51–104.54) and Chapter 175 (Figs 175.8, 175.9, 175.15, and 175.16).
Pathology and Patterns of Disease
Bell palsy is likely to be a viral neuritis or an ischemic event incited by nerve swelling due to an inflammatory viral neuritis. There is substantial indirect evidence of this etiology, and it seems to be the most likely cause.1,2
The virus is most likely to be in the herpes family, either herpes simplex or the varicella-zoster virus. It may be that the virus itself injures the nerve, or the inflammation caused by a viral infection causes nerve swelling that produces an ischemic neuropathy from the labyrinthine segment distally since that segment is the tightest part of the facial canal. This is the same theory that suggests if a facial nerve is traumatized by blunt-force injury, the labyrinthine segment must be included in any planned surgical decompression.
The facial nerve will become inflamed and edematous in the early stages of disease. Various degrees of axonal changes may occur depending on the severity of the insult. The muscles of facial expression comprising most of the bulk of the superficial musculoaponeurotic system may go through the process of denervation atrophy. The muscles may enhance acutely and subacutely and then decrease in bulk and become fat replaced.
Pathologically Altered Function
All of the muscles on one side of the face (including those of the forehead) will become completely or partially paralyzed. Preservation of function of the upper facial muscles suggests central pathology.
IMAGING APPROACH
Techniques and Relevant Aspects
In general, CT and magnetic resonance imaging (MRI) in this condition requires the highest possible spatial resolution. These issues related to optimal protocol development are discussed in detail in conjunction with general CT and MR parameters in Chapters 1 through 3.
Specific protocols for MR and CT studies for investigating facial nerve problems in general appear in Appendixes A and B. The facial nerve is typically studied with dedicated contrast-enhanced studies of the temporal bone, especially when the patient is acutely symptomatic. These studies must also include the entire peripheral course of the facial nerve as well as the posterior fossa. In clinical settings atypical for Bell palsy, these studies may need to be repeated. Negative studies do not exclude the possibility of an early structural lesion. Clinical circumstances should guide the diagnostic approach. Surgical exploration might still be required in cases highly suspicious for a compressive and/or infiltrative lesion with negative imaging.
Pros and Cons
MRI should be done first since it most confidently excludes causative pathology at all segments (i.e., the brain stem, cisternal, exit canal/foramen, and extracranial segments) of the nerve from its brain stem nucleus to the parotid gland. MRI is more sensitive than CT for excluding intra-axial pathology such as demyelinating disease, pia-arachnoid diseases, and small neoplasms of the nerve that might involve the cisternal segment or the segment within the internal auditory canal as well as perineural spread of cancer.
CT may be done as a supplement to most confidently exclude similar pathology within the facial canal from the labyrinthine segment to the stylomastoid foramen and beyond the parotid gland distally. This supplemental imaging may be done as a routine study or only when MR findings are suspicious for a lesion other than inflammatory enhancement. More typically, supplemental CT is done when the onset of symptoms is atypical for Bell palsy and the cause is not established by MRI or the MRI is suspicious for a cause but not definitive. For instance, both CT and MRI may be necessary in the case of ossifying hemangioma or minor thickening of the facial nerve within and beyond the parotid gland as a result of perineural tumor spread.
Controversies
Most treating physicians will not image a patient with acute onset of peripheral facial nerve palsy because about 75% of these palsies will be transient and will begin to recover in 4 to 6 weeks whether or not they are treated with steroids or antiviral medications and show no atypical subsequent characteristics such as recurrence of weakness. Few would suggest studying all patients with acute onset peripheral facial nerve palsy regardless of the pattern of onset of the facial weakness. Early imaging sometimes leads to excessive anxiety about normal variations or minor findings consistent with a viral neuritis such as perigeniculate enhancement.
MANIFESTATIONS OF DISEASE
Acute Onset of a Peripheral Facial Nerve Palsy
Computed Tomography
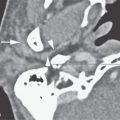
CT will virtually always be normal. If performed, it must, however, be used to exclude structural lesions affecting the facial nerve. If such a lesion (e.g., compressive cholesteatoma) is found, then this is not Bell palsy.
Magnetic Resonance
MRI will usually be normal. It may show minimal enlargement and increased enhancement of the affected facial nerve (Fig. 127.1), especially in the perigeniculate region, that may persist up to 1 year (Fig. 127.1K). Sometimes, this is actually a normal variation. If performed, MRI must be used to exclude structural lesions affecting the facial nerve other than minimal enhancement and enlargement limited to its course in the temporal bone. If a structural lesion (e.g., perineural spread of skin cancer) beyond that is found, then this is not Bell palsy.
DIFFERENTIAL DIAGNOSIS
From Clinical Data
The patient suffers the acute onset of a partial or complete peripheral (all of the muscles on one side of the face) facial nerve palsy. There may be associated pain around the ear. There really should be no other signs or symptoms. In particular, there must be no other signs of central nervous system disease.
Bell palsy must never be confused with a peripheral facial nerve palsy of slow, progressive, or stuttering onset. Also, recurrent or persistent peripheral facial nerve palsy or associated spasticity should never be considered a Bell palsy until it is proven not to be due to a compressive and/or infiltrative lesion of the facial nerve. Conditions with these types of clinical characteristics atypical for Bell palsy will very often be the result of benign or malignant neoplasms and a handful of other causes that may occur anywhere along the nerve from its nucleus to its peripheral distribution.3 Rarely, an acute brain stem event will present as only a facial nerve palsy (Fig. 127.2).
From Supportive Diagnostic Techniques
MRI may show minimal enlargement and slightly increased enhancement of or around the facial nerve, especially at the geniculate ganglion. Otherwise, imaging is used to exclude structural pathology of some other etiology (Chapters 128–131). A normal MR and CT in the proper clinical setting will confirm the diagnosis of a true Bell palsy.
Conditions that might mimic enhancement due to viral neuritis are perineural spread of cancer and other inflammatory enhancement such as that due to Lyme disease4 (Fig. 127.3). If significant pathology other than viral neuritis is suspected, there should be appropriate clinical testing (e.g., Lyme titers and careful history taking for removal of possibly cancerous skin lesions) and careful clinical follow-up sometimes including follow-up imaging.


FIGURE 127.1. Magnetic resonance imaging findings in four patients with the acute onset of a right-sided peripheral facial nerve (Bell) palsy. A–D: Patient 1. Contrast-enhanced T1-weighted (T1W) images showing typical contiguous enhancement of the facial nerve (arrows) from the internal auditory canal fundus to the second genu compared to the normal left side (arrowhead). C–H: Patient 2. Contrast-enhanced T1W images with abnormal enhancement of the right distal intracanalicular, labyrinthine, tympanic, and mastoid segment (arrows) compared to the normal perineural plexus enhancement on the left (arrowheads). I, J: Patient 3. Three-dimensional T1W images showing the facial nerve enhancement involving the entire descending segment (arrows) and continuing beyond the stylomastoid foramen to involve the nerve within the parotid gland (arrowheads in I). The main trunk of the nerve enhances within the parotid gland (arrows in J). K: Patient 4. The enhancement of the facial nerve on the right (arrows) compared to the normal descending segment on the left (arrowheads) persisted for over a year. The patient eventually recovered all facial nerve function.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree