Birth-related injury is defined as any traumatic or ischemic event sustained during the process of delivery. Perinatally acquired disease processes secondary to birth-related injury can be traumatic or ischemic in nature. In this article, the authors focus on traumatic/mechanical injuries. Other diseases of the perinatal time period, including germinal matrix hemorrhages and hypoxic-ischemic encephalopathy, are beyond the objective of this review.
Birth-related injury is defined as any traumatic/ischemic event sustained during the process of delivery. In this article the authors focus on perinatally acquired disease processes secondary to birth-related injury, either traumatic or ischemic in nature. Other diseases of the perinatal time period, including germinal matrix hemorrhages and hypoxic-ischemic encephalopathy (HIE), are beyond the objective of this review.
Etiology
Birth-related injury may affect any organ system; however, because the head is the presenting body part in the majority of deliveries, and is one of the largest anatomic structures to pass through the birth canal, and does not tolerate too much molding during delivery, traumatic head injury is the most frequently encountered type of birth-related trauma. In addition, during the delivery hyperextension and shear forces at the craniocervical junction may result in additional cervical spinal cord injury. Although many traumatic head and spine injuries are benign and do not require therapy, some may require rapid diagnosis and treatment to avoid progression, permanent disability, or even death. In addition, hypoxic-ischemic injuries may be superimposed on “purely” mechanical types of injury, which may worsen functional and neurologic outcome.
Advancements in obstetric management in the last few decades have significantly decreased the incidence of birth-related deaths. Birth-related injury accounts for fewer than 2% of neonatal deaths. From 1970 to 1985, rates of newborn mortality due to birth-related trauma fell from 64.2 to 7.5 deaths per 100,000 live births, a remarkable decline of 88%. This decrease reflects, in part, the technologic advancements that allow today’s obstetrician to recognize perinatal risk factors using prenatal ultrasonography (US) and fetal monitoring prior to vaginal delivery. The use of potentially injurious instrumentation, such as forceps or vacuum delivery, has also declined.
Instrumental delivery (forceps, vacuum extraction) may be performed for fetal or maternal indications. The most common indication is a prolonged second stage of labor with fetal distress or presumed fetal compromise whereby any additional delay may result in hypoxic-ischemic neonatal brain injury or fetal death. Maternal indications include severe heart disease or cerebral vascular malformations.
Birth trauma should be suspected in cases with difficult delivery, or in the presence of predisposing maternal or neonatal risk factors. Newborn risk factors include macrosomia (>4500 g), perinatal decelerations/depression, shoulder dystocia, abnormal presentation of the fetus such as breech position, and the use of instruments during delivery. Maternal risk factors include diabetes mellitus, obesity, small pelvis, induced labor, or previous history of a macrosomic neonate. Placental abruption predisposes a significant risk for hypoxic-ischemic injury in newborns. Although many injuries are believed to occur secondary to birth-related complications, injuries in the absence of identifiable risk factors are well described, which makes their occurrence unpredictable and difficult to “catch” early.
Consequently, the true incidence of birth-related head and cervical spine injury is not well known. In asymptomatic newborns, unless they are imaged for other reasons, it is impossible to know the incidence of intracranial injuries. Increasing use of imaging modalities in asymptomatic newborns shows that even spontaneous vaginal deliveries are associated with intracranial hemorrhages ( Fig. 1 ).

Birth-related injury to the head and cervical spine may result in:
- 1.
Extracranial injuries: skin abrasions and hemorrhage between the various layers of the scalp; caput succedaneum; cephalohematoma; subgaleal hemorrhage
- 2.
Intracranial, extra-axial hemorrhage: epidural, subdural, or subarachnoid hemorrhage
- 3.
Intracranial, intra-axial hemorrhage
- a.
Cortical contusions, shear force, diffuse axonal injury, or intraparenchymal hemorrhage
- b.
Cerebral injury secondary to perinatal hypoxia-ischemia
- a.
- 4.
Skull injury: diasthesis of the sutures, and calvarial or facial fracture
- 5.
Peripheral nerve injury in the face (facial nerve palsy), and injury to the cervical spinal cord, including the brachial plexus and phrenic nerve.
The authors discuss each category separately to provide general information. In the second half of the article imaging modalities used to diagnose each pathologic condition are discussed.
Extracranial Injuries
Most newborns delivered by instrumentation, particularly after vacuum extraction, exhibit scalp injury, most of which are transient and are of no clinical significance. The incidence of scalp abrasions and lacerations after vacuum extraction is estimated at 10%. The majority are superficial and of a minor degree. The more significant injuries are related to incorrect placement of the vacuum cup, inability to achieve a correct application, excessive or poorly directed traction, cephalopelvic disproportion, or fetal coagulation defects.
Scalp lesions are classified according to the involved spaces. A proper knowledge is essential for correct characterization of the lesions. The scalp is composed of 5 layers: skin, subcutaneous fibrofatty tissue, galea aponeurotica, loose areolar connective tissue, and the periosteum of the calvarial bones. The temporalis muscle arises from the periosteum of the temporal fossa, and therefore lies beneath the galea and subgaleal space.
Caput succedaneum is a serosanguinous, extraperiosteal collection within the subcutaneous fibrofatty space between the skin and the adjacent galea aponeurotica. It presents as a soft tissue swelling with purpura/ecchymosis over the affected part of the scalp. It is caused by the mechanical trauma of the presenting part of the fetal cranium pushing through the dilating cervix. Due to its location, caput succedaneum typically extends across suture lines and usually resolves within the first few days of life. No treatment is necessary.
Subgaleal hemorrhages are located in the space between the galea aponeurosis of the scalp and the calvarial periosteum. This space extends from the orbital margins anteriorly, to the nuchal ridge posteriorly, and the temporal fascia laterally. Subgaleal hematoma presents as a firm/fluctuant mass that crosses the suture lines. Unlike cephalohematoma, subgaleal hemorrhage is superficial to the temporal muscle. The subgaleal space is composed of loose connective tissue and contains small blood vessels. Subgaleal hemorrhage is most often associated with vacuum extraction and forceps delivery in which the traction forces pull the aponeurosis from the calvarium. Typically it is clinically noted within a few hours after birth. The loose connective tissue in this space allows massive bleeding, which may result in hemorrhagic shock. Treatment is largely supportive.
Cephalohematoma is a subperiosteal bleed that accumulates between the calvarial periosteum and the adjacent outer table of the skull. It is located beneath the temporalis muscle. Cephalohematoma presents typically as a firm swelling overlying the parietal or occipital bone confined by the sutures. It occurs in approximately 2.5% of newborns, being the most common extracranial scalp injury after abrasion/lacerations. Cephalohematoma is commonly associated with forceps and breech deliveries. Often it is unilateral and is not associated with discoloration. The subperiosteal bleeding may grow slowly over a couple of days, thus may present with a few days of delay after birth. In the majority of cases, cephalohematomas resolve within a few weeks. Rarely complications may occur, such as significant blood loss or infection. Coexisting skull fractures may be present in up to 5% of the cases. Cephalohematomas occasionally may calcify and present as a “bony swelling.”
Intracranial Extra-Axial Injury
The incidence or prevalence of birth-related intracranial, extra-axial hemorrhage (subdural, epidural, or subarachnoid hemorrhage) is not well known or prospectively studied. A percentage of term newborns with intracranial hemorrhage present with clinical or neurologic symptoms such as apnea, bradycardia, and seizures that may initiate diagnostic workup. In addition, imaging studies indicate that intracranial, extra-axial hemorrhage may be found in asymptomatic newborns. The reported incidence of asymptomatic and symptomatic intracranial extra-axial hemorrhage varies from study to study, probably due to differences in the studied newborn populations and the sensitivity and timing of the used diagnostic tests.
While intracranial extra-axial injury can be observed with spontaneous vaginal delivery, additional maternal and fetal risk factors may increase the susceptibility of the neonate for perinatal intracranial injuries. Risk factors include forceps delivery, vacuum extraction, prolonged second stage (>2 hours), or fetal macrosomia. In addition, factors such as birth asphyxia, prematurity, hemorrhagic diathesis, infection, and vascular anomalies have a significant impact.
Subdural hemorrhage (SDH) is the most common intracranial extra-axial hemorrhage related to birth trauma. Pollina and colleagues reported that it accounts for 73% of intracranial birth injuries in term newborns. Although frequently related to birth trauma, SDH have been diagnosed in utero before the start of the birth process, in newborns who were delivered by caesarean section, and in asymptomatic newborns after uncomplicated vaginal deliveries. In a study by Whitby and colleagues, SDH were noted in 6.1% of uncomplicated deliveries, and follow-up magnetic resonance (MR) imaging showed resolution in all newborns by 4 weeks. All children showed normal neurologic development by 2 years of age.
In the newborns, the majority of birth-related SDH are found in the posterior fossa, along the tentorium or over the occipital-parietal lobes of the supratentorial brain (see Fig. 1 ). Isolated supratentorial SDH are quite rare. The location and extension suggests that these SDH result from nontraumatic vascular insults affecting the tributaries of the dural sinuses within the dural folds of the posterior fossa, as discussed by Volpe and others. Formerly it was believed that subdural hemorrhages resulted from a tentorial tear, from damage to the occipital sinus accompanying occipital osteodiastasis, or to a rupture of bridging superficial cerebral convexity veins. Most common clinical symptoms include apnea and seizures, focal neurologic deficits, lethargy, and hypotonia.
Many neonates with SDH are treated conservatively. Occasionally surgical intervention may be required, depending on the size and clinical symptoms such as compression of vital structures. Finally, in neonates and young babies, SDH may occur as part of the lesions encountered in nonaccidental trauma (NAI) (shaken baby). NAI is the leading cause of death and lifelong disability for neonates; half of which occur before 4 months of age.
Epidural hematomas (EDH) are venous or arterial hemorrhages located between the internal tabula and the adjacent internal periosteum of the calvarium. EDH is typically limited by the sutures. The prevalence of EDH is rare in the newborn. Tagaki and colleagues reported that EDH occurs in 2.2% of autopsies of newborns who had intracranial hemorrhage. The rarity can be explained by the absence of a middle meningeal artery groove in the neonate, which makes the artery less susceptible to skull fracture–related injury. EDH is frequently associated with skull fracture and cephalohematoma. Presenting symptoms may include increased intracranial pressure, bulging fontanel, or focal neurologic symptoms including seizures. Surgical intervention may be necessary, although Negishi and colleagues reported that outcome may be favorable without surgical treatment.
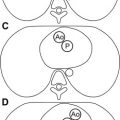
Subarachnoid hemorrhages (SAH) are located in the space between the arachnoid membrane and pia mater ( Fig. 2 ). The prevalence of symptomatic SAH has been reported to range from 1.3 per 10,000 live births in spontaneous vaginal deliveries to 2 to 3 per 10,000 live births in vacuum and forceps deliveries. Fenichel and colleagues reported primary SAH as the most common type of intracranial hemorrhage over a 5-year period among “symptomatic” term newborns (n = 22) in a neonatal intensive care unit. SAH occur more frequently as a result of prematurity and postperinatal asphyxia. In newborns, SAH is believed to result from a rupture of the fragile veins that cross the subarachnoid space, or from injury to small leptomeningeal vessels. Although a SAH may be asymptomatic, the most common presentation is seizures that often occur on the second day of life. Neurologic examination often may be normal during interictal periods; however, irritability or depressed level of consciousness may be present. An adjacent/combined cortical contusion may cause focal neurologic signs. In patients with ischemic encephalopathy, clinical deterioration may be rapid and progressive. Usually there are no long-term sequelae of minor SAH if underlying cortical injury and hypoxic injury are not present.

Intracranial Intra-Axial Injuries
Intracerebral hemorrhage (ICH) is less frequent than SDH and SAH in term newborns. Sandberg and colleagues published a large series, in which they reviewed a neurosurgical computerized database spanning more than 40 years, and identified 11 cases of intracerebral, lobar hemorrhage. Of these 11 neonates, 8 were delivered by spontaneous vaginal delivery, 2 by vacuum extraction, and 1 by cesarean section. Other than large ICH, newborns may suffer from smaller parenchymal injuries, small cortical contusions, and shear or diffuse axonal injuries. In contrast to the rarity of cases reported in the literature, ICH is not uncommon in clinical practice. The discrepancy in the reported number of cases and clinical experience can be explained by the imaging techniques that have been used in the published series. The increasing use of MR imaging sequences more sensitive to blood products such as susceptibility-weighted imaging may increase detection of birth-related intracranial injuries in the newborn ( Fig. 3 ).

Cerebral injury secondary to intrapartum hypoxia-ischemia
Hypoxic-ischemic injury is one of the most commonly recognized causes of severe, long-term neurologic deficits in children. Initial ischemic episode is followed by a “reperfusion state.” During this reperfusion state interventional procedures such as “hypothermia” can be beneficial for the neurologic outcome. Details of this topic are covered in an article by Izbudak and Grant elsewhere in this issue.
Skull Injury
Overlapping of the calvarial bones especially of the parietal bones is a normal physiologic phenomenon during delivery, allowing the neonatal head to pass the narrow birth canal ( Fig. 4 ). Postnatal residual overlap may be palpated in some newborns, which usually resolves spontaneously. Skull fractures are rarely seen after spontaneous birth. Skull fractures may occur in assisted deliveries, for example, by compression of the forceps, or from the skull pushing against the maternal symphysis or ischial spines. Skull fractures can be linear, affecting the parietal bones, or may be depressed, forming the so-called ping-pong ball type fracture. Occipital osteodiastasis is a special type of skull injury of the newborn resulting from separation of the squamous and lateral parts of the occipital bone. This injury is commonly observed in breech delivery, with anterior displacement and upward rotation of the squamous bone ; this may result in posterior fossa SDH, cerebellar contusion, or even cervicomedullary compression. Presence of cephalohematoma or SAH should raise the suspicion for skull fracture, and cross-sectional imaging should be performed.

Peripheral Nerve and Spinal Cord Injuries
Brachial plexus injury, facial nerve injury, phrenic nerve injury, or spinal cord injuries can be seen as a complication of birth.
The prevalence of brachial plexus injury is rare, and ranges from 0.1% to 0.2% of births. Risk factors include macrosomia, shoulder dystocia, instrumented deliveries, and malpresentation. The pathogenesis of injury often involves stretch injury when shoulder dystocia requires extreme lateral flexion and traction of the head. However, there are increasing reports of injury that occurs when lateral flexion and traction of the head has not been applied, such as during precipitous deliveries or when there is injury to the posterior shoulder. These findings indicate that intrauterine maladaptation may also play a role in the development of the injury. Brachial plexus injury has also been reported during the intrauterine period. Hematomas of the sternocleidomastoid muscle and fractures of the clavicle and humerus can be observed in children with brachial plexus injuries, and should be used as a lead sign to rule out brachial plexus lesions ( Fig. 5 ).