CERVICAL ESOPHAGUS: INTRODUCTION
IMAGING APPROACH
Techniques and Relevant Aspects
The cervical esophagus is studied in essentially the same manner as the neck is generally evaluated with magnetic resonance imaging (MRI) and computed tomography (CT). There is little or no use for ultrasound in studying the esophagus unless endoluminal ultrasound is considered, but the use of that technique is beyond the scope of this resource. The principles of using these studies are reviewed in Chapter 149. Specific problem-driven protocols for CT and MRI are presented in Appendixes A and B.
The approach with radionuclide studies depends on the aim of the examination. Most of the current usage is limited to cancer evaluation with fluorine-18 2-fluoro-2-deoxy-D-glucose positron emission tomography (FDG-PET).
Pros and Cons
Indications for Study
Evaluating the Extent of Known Cervical Esophageal Cancer and Related Regional Lymph Node Metastases
Both CT and magnetic resonance (MR) can supply information needed by the clinician for optimal treatment planning. CT studies are easier to execute and are more reproducible than MRI because of the short data acquisition time that results in less image motion degradation; however, this is much less a problem in the low neck than in the upper part of the infrahyoid neck. Multidetector computed tomography (MDCT) systems also now offer high-quality multiplanar imaging, with the image quality equal to or exceeding that of multiplanar MR images. MRI has a distinct advantage for evaluating invasion of surrounding structures including the larynx, hypopharynx, trachea, thyroid gland, and carotid artery.
Evaluation of Submucosal or Periesophageal Masses of Uncertain Etiology
Both CT and MR can be used to demonstrate the presence, nature, and extent of a submucosal mass lesion. In most cases, a CT study is adequate for all of these tasks. A variety of sometimes unusual lesions, either benign or malignant, can be encountered in this clinical context. As the initial biopsy results may be inconclusive or negative, MR may be used in an attempt to further characterize the lesion. In young patients, MR might be preferred because of the absence of ionizing radiation.
Throat Pain, Dysphagia, and Odynophagia
CT is the preferred modality for these studies since it not only provides a good evaluation of the cervical esophagus but also the hypopharynx and surrounding structures that might lead to such symptoms. Adjunctive MRI may be used instead of MRI or in cases wherein CT is suspicious but not definitive for the diagnosis of a mass that might be related to the esophagus. Neither study excludes mucosal disease, which certainly can cause such symptoms.
Esophageal Trauma
CT is the preferred modality for this study, as it can be performed more simply than MRI in the acute or immediate subacute clinical setting. It simultaneously allows a thorough evaluation of the other neck structures, including soft tissue injury that might be associated with pharyngeal tears, vascular injury, and cervical spine injuries, among others. It is also better for identifying gas and retained foreign bodies; this is especially useful in the evaluation of a potentially swallowed foreign body.
Functional Studies
Water-soluble contrast and barium studies remain the preferred studies for gross screening for perforations or false passages, functional disorders, and mucosal lesions.
NORMAL ANATOMY
General Description
The junctions of the larynx and trachea, as well as that of the esophagus and hypopharynx, occur at the same level in the visceral compartment of the infrahyoid neck (Figs. 221.1–221.3). The cricoid cartilage is its most prominent landmark and easy-to-recognize structure to identify this transition. The cricoid is easily recognized as it surrounds the airway posteriorly since it is the only complete ring in the airway.
The hypopharyngeal walls are continuous with the cervical esophagus below (Figs. 221.1–221.4). The transition to cervical esophagus begins below the arytenoids and is about 3 to 4 cm in length; this is the postcricoid portion of the hypopharynx (Figs. 221.1–221.3). The lower 1 to 2 cm of this is often referred to as the cricopharyngeus muscle. Like the Passavant ridge, this is really only a specialized sphincterlike area of the inferior constrictor, and the “cricopharyngeus muscle” is not really a separate muscle. It is a functional zone of the inferior constrictor. There are natural areas of dehiscence where these muscles overlap and are penetrated by neurovascular bundles. The best known of these is the Killian-Jamieson area at the lowermost portion of the inferior constrictor muscle, which is the site of origin of a Zenker diverticulum. There has been much description of the exact anatomy responsible for diverticuli in this region. It is likely enough that the diagnostic imager understands that these occur at the esophageal verge or inlet (Fig. 221.5).


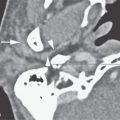
FIGURE 221.1. A series of whole organ sections and computed tomography (CT) images demonstrating anatomic relationships of the cervical esophagus to the hypopharynx. A: Sagittal whole organ section showing the cricoid cartilage (C) as a major landmark in the hypopharynx to cervical esophagus transition. The top and bottom of the cricoid cartilage are shown by the black arrows. The postcricoid portion of the hypopharynx is shown by the white arrows. The white arrowhead shows the lumen of the postcricoid portion of the hypopharynx as, at the bottom of the cricoid cartilage, it becomes the esophageal verge (EV) as it merges with the cervical esophagus (E). (T, trachea.) B: Sagittal reformation of a contrast-enhanced CT study. The patient performed a slight Valsalva maneuver while holding his breath so that the pyriform sinus (PYS) apex would not be visible. The top and bottom of the cricoid cartilage are shown by the black arrows to define the postcricoid portion of the hypopharynx (PC) and its transition to the cervical esophagus (E) at the cricotracheal junction (white line). C: A whole organ section wherein the orange line shows the extent of visceral fascia at this level. The inferior margin of the cricoid cartilage marks the transition of the postcricoid portion of the hypopharynx to the esophageal verge (PC-EV). Note that the inferior constrictor muscles still retain an attachment to the laryngeal skeleton at this level (black arrowheads). Understanding this anatomy and its transition to the cervical esophagus is essential knowledge for proper treatment planning in hypopharyngeal and cervical esophageal cancer. D: A whole organ section just above the thoracic inlet showing the trachea (T) as an incomplete cartilage ring with a partially mucosal (arrowhead) and partially muscular (black arrow) posterior membranous wall. The esophagus (E), defined by its thick muscular wall (white arrows) and mucosa (black arrowhead), lies in the midline posteriorly. The recurrent laryngeal nerves (white arrows) are important adjacent structures lying in the tracheoesophageal grooves (white arrows). E: Non–contrast-enhanced CT image of patient who had suffered trauma and resulting mediastinal and cervical emphysema. The trachea (T) and esophagus (E) can be seen as the primary structures in the visceral compartment of the neck at the thoracic inlet.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree