Abstract
First clinically described in 1961 by Hirschhorn and subsequently in 1965 by Wolf, the 4p deletion syndrome, or Wolf-Hirschhorn Syndrome (WHS), is the first example of a classic human chromosomal deletion syndrome. This rare condition, characterized by severe prenatal onset growth restriction, typical facial features, and severe seizures, is well described in the pediatric literature. Accounts of its prenatal presentation and diagnosis based on ultrasound findings and confirmatory genetic testing are more limited and consist of isolated case reports and small case series. Although more than 50% of deletions are visible by standard karyotyping, use of fluorescence in situ hybridization (FISH) and the now recommended array-based copy-number analysis or chromosomal microarray analysis (CMA) have improved the diagnosis of chromosome 4p deletions that cause WHS. Recently, noninvasive prenatal screening for microdeletion syndromes on cell-free fetal DNA (cffDNA) in maternal plasma has been developed and is being introduced in the clinic. This has widened the prenatal ascertainment for 4p deletion syndrome to a broader screen for potentially affected fetuses even in the absence of sonographic findings. Hence, practitioners should be familiar with the features of WHS syndrome that are detectable by prenatal imaging and those that are not prenatally observable, its prognosis, and the implications for perinatal management and counseling when a 4p deletion is detected prenatally.
Keywords
Wolf-Hirschhorn syndrome, 4p deletion, growth restriction, characteristic facial features, variable congenital anomalies
Introduction
First clinically described in 1961 by Hirschhorn and subsequently in 1965 by Wolf, the 4p deletion syndrome, or Wolf-Hirschhorn Syndrome (WHS), is the first example of a classic human chromosomal deletion syndrome. This rare condition, characterized by severe prenatal findings and confirmatory genetic testing, is more limited and consists of isolated case reports and small case series. Although more than 50% of deletions are visible by standard karyotyping, use of fluorescence in situ hybridization (FISH) and the now recommended array-based copy-number analysis or chromosomal microarray analysis (CMA) have improved the diagnosis of chromosome 4p deletions that cause WHS. Recently, noninvasive prenatal screening for microdeletion syndromes on cell-free fetal DNA (cffDNA) in maternal plasma have been developed and are being introduced into practice. This has widened the prenatal ascertainment for 4p deletion syndrome to a broader screen for potentially affected fetuses even in the absence of sonographic findings. Hence practitioners should be familiar with WHS syndrome features that are detectable by prenatal imaging and those that are not prenatally observable, its prognosis, and the implications for perinatal management and counseling when a 4p deletion is detected prenatally.
Disorder
Definition
The 4p deletion syndrome is a heterozygous deletion syndrome of variable size of the short arm of chromosome 4 with a core phenotype of severe prenatal and postnatal growth restriction, distinctive craniofacial features of prominent glabella, wide nasal bridge with beaked nose, high forehead, hypertelorism, downturned corners of the mouth and short philtrum (referred to as “Greek warrior helmet” face), together with moderate to profound developmental delay, intellectual disability, and severe seizures. The 4p deletion syndrome is also variably associated with congenital abnormalities detectable by prenatal ultrasound (US), of which many are thought to result from midline fusion defects. Postnatally, low muscle mass, hypotonia, and feeding difficulties are common. Other features include immunoglobulin abnormalities, eye and ear abnormalities, and hearing loss. Developmental prognosis is poor, and there is increased risk for early childhood death.
Prevalence and Epidemiology
The 4p deletion syndrome is rare, with an estimated prevalence of 0.2–0.5 : 10,000 and a 2 : 1 female-to-male ratio. The 4p deletion can be de novo in about 50% to 60% with low recurrence risk, or can be the result of an unbalanced translocation in 40% to 50%, which is associated with partial trisomy of another region. Parents who carry balanced translocations involving 4p16.3 have an increased risk of affected offspring with an inherited unbalanced translocation.
Etiology and Pathophysiology
The 4p deletion syndrome is caused by monosomy of part of the short arm of chromosome 4, encompassing the 4p16.3 critical region. About 50% to 60% of individuals have a simple deletion, and 40% to 50% have an unbalanced translocation with duplication of another region. In a recent survey on 109 cases, 32% were caused by an unbalanced translation; 75% of deletions encompassed the entire critical region, of which 43% were associated with duplication of other regions and 8% of adjacent regions. The Wolf-Hirschhorn syndrome critical region (WHSCR) has been narrowed down to two regions within 4p16.3, containing multiple genes, several of which, such as WHSCR1, LETM1, have been investigated for their role in the different clinical features. Prenatal genetic diagnosis by G-banded karyotyping detects the 50% to 60% of deletions that are larger than 5 Mb, and FISH with WHSCR-specific probes can detect 90% of suspected cases. However, CMA, the recommended analysis for pregnancies with major anomalies, is the most effective for detecting 4p deletions, particularly in cases with low clinical suspicion or with small deletions that do not include the region targeted by the FISH probes. Although noninvasive screening for microdeletion syndromes, including 4p deletion, has recently become available, it does not replace diagnostic testing for pregnancies with fetal abnormalities. All patients with positive results from such screening should be offered diagnostic testing by amniocentesis or CVS, with CMA as the genetic test of choice.
Manifestations of Disease
Clinical Presentation
The 4p deletion syndrome has a complex and variable phenotype. Most prenatally diagnosed cases are associated with severe early-onset growth restriction and microcephaly that persist postnatally. Other more variable findings (many of which have been reported prenatally) include craniofacial asymmetry, dolichocephaly, hypertelorism, wide nasal bridge, cystic hygroma or increased nuchal fold thickness, thin corpus callosum, ventriculomegaly, and hypotonia, micrognathia, cleft lip/palate, abnormally positioned ears, midline scalp defects, cardiac defects, diaphragmatic hernia, variable intestinal defects, renal and urinary tract anomalies (horseshoe kidney, vesicoureteral reflux, renal agenesis, cystic dysplasia, bladder exstrophy), hypospadias, single umbilical artery, and skeletal abnormalities (talipes, scoliosis, split hand). The cardiac defects are usually not complex and include ventricular or atrial septum defects, but others, like hypoplastic left heart and tetralogy of Fallot, have been reported. Postnatal complications include severe early-onset seizures, hypotonia, reduced muscle mass, severe feeding and swallowing difficulties, poor growth, and moderate to profound intellectual disability. Affected children also have hearing loss, eye abnormalities, immunoglobulin deficiencies, and a predisposition to hematopoietic dysfunction and hepatic adenomas. There is increased risk for early death, and one-third of affected individuals die by 2 years of age, but with supportive treatments, survival into adulthood is possible.
Imaging Technique and Findings
Ultrasound.
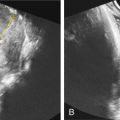
The prenatal US findings of 4p deletion syndrome are listed in Table 155.1 . The most common findings are early-onset severe intrauterine growth restriction (IUGR) that persists postnatally, and microcephaly. The IUGR is symmetrical and can be associated with abnormal umbilical artery Doppler indices, decreased fetal movements, and oligohydramnios. Most 4p deletions occur de novo, thus affected individuals are usually born to low-risk parents. With the increasingly common practice of noninvasive screening of pregnancies for microdeletions, recognition of associated US features will benefit interpretation of positive screens within the clinical context. Features reported in the literature include cerebellar hypoplasia, cystic hygroma ( Fig. 155.1 ), microcephaly ( Fig. 155.2 ), cleft lip and palate ( Fig. 155.3 ), micrognathia ( Fig. 155.4 ), hypertelorism ( Fig. 155.5 ), absent nasal bone ( Fig. 155.6 ), tetralogy of Fallot ( Fig. 155.7 ), echogenic bowel ( Fig. 155.8 ), pyelectasis and other renal anomalies, clubfeet ( Fig. 155.9 ), ambiguous genitalia ( Fig. 155.10 ), and single umbilical artery ( Fig. 155.11 ).
|