CNS Imaging Manifestations of Toxic, Metabolic, and Systemic Pathologies
Sathish Kumar Dundamadappa
Aly H. Abayazeed
Prachi Dubey
QUESTIONS
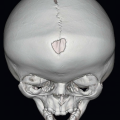
1 A 60-year-old female with acute-onset movement disorder presents for evaluation; CT and MR are performed (key images are shown below). Past medical history is significant for hypertension and type 2 DM; both are not well controlled on medication.
|
1a Based on the available clinical information and the above images, what is the most likely systemic abnormality expected in this patient?
A. Elevated ammonia levels
B. Hypertensive crisis
C. Nonketotic hyperglycemia
D. Respiratory acidosis
View Answer
1a Answer C. Nonketotic hyperglycemia. This appearance is not typical for a hypertensive hemorrhage, attenuation is lower for hemorrhage, and morphology is not compatible with a hematoma. There are no corroborating clinical findings to support a hyperammonemic state or substrates for respiratory acidosis.
1b What is the usual expected clinical course after correction of the systemic abnormality?
A. Permanent residual movement dysfunction
B. Parkinsonian rigidity
C. Complete resolution of symptoms
D. Progressive neurologic deficit
View Answer
1b Answer C. Complete resolution of symptoms. Imaging findings and movement abnormalities resolve with treatment and correction of hyperglycemia. Rarely, imaging findings can persist for a longer time.
|
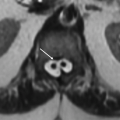
Imaging Findings: There is hyperintensity on T1w image (A), hypointensity on T2w image (B), and high attenuation on CT within the caudate and putamen (C), significantly more striking on the left. Findings are most likely to represent hyperglycemia-related changes in the current clinical setting.
Discussion: Nonketotic hyperglycemia with acute-onset hemiballismus-hemichorea.
Nonketotic hyperglycemia with acute-onset hemiballismus-hemichorea is usually caused by lesions in contralateral basal ganglia. Those lesions, which are caused by nonketotic hyperglycemia, are characterized by T1 hyperintensity, and are commonly seen in elderly patients with diabetes, more so in females and Asian population. The exact pathogenesis is uncertain. The proposed etiologies include altered metabolism, petechial hemorrhages, and accumulation of gemistocytic astrocytes.
Putamen is the most commonly involved region, followed by caudate nucleus. Globus pallidus and midbrain involvement can also be seen. The lesions are usually unilateral. T1 hyperintensity in the involved regions without mass effect or abnormal enhancement is the characteristic finding. T2-weighted images can be hypointense or isointense. Mild degree of blooming can be seen on susceptibility images. Mild reduction in ADC can also be seen. CT demonstrates hyperdensity. Imaging findings and movement abnormalities usually resolve with treatment and correction of hyperglycemia.
Differential diagnosis: Other cause of T1 hyperintensity in basal ganglia: the most common in being hepatic encephalopathy. Clinical history can help in differentiation.
References: Priola AM, Gned D, Veltri A, et al. Case 204: nonketotic hyperglycemia-induced hemiballism-hemichorea. Radiology 2014;271(1):304-308. doi: 10.1148/radiol.14120840
Rumboldt Z, Castillo M, Huang B, et al., eds. Brain imaging with MRI and CT: an image pattern approach. Cambridge, UK: Cambridge University Press, 2012.
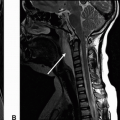
2 A 45-year-old chronic alcoholic with malnutrition presents with acute alteration of mental status. Key images from MRI are shown below.
|
2a What is the most likely biochemical abnormality explaining these changes in the current clinical setting?
A. Thiamine deficiency
B. Vitamin B12 deficiency
C. Hyperammonemia
D. Hyponatremia
View Answer
2a Answer A. Thiamine deficiency. In the clinical setting of chronic alcoholism and malnutrition, the signal changes shown in the medial thalami, dorsal medulla, and mammillary body are typical for Wernicke encephalopathy because of thiamine deficiency. Another classic location is periaqueductal gray matter not shown in this case.
2b If left untreated in the chronic phase, the patient may develop which of the following conditions?
A. Transient global amnesia
B. Delirium tremens
C. Korsakoff psychosis
D. Chronic traumatic encephalopathy
View Answer
2b Answer C. Korsakoff psychosis. In the chronic phase, patients may develop confabulation, amnestic episodes with memory loss, and difficulty learning new information.
|
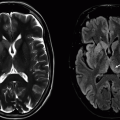
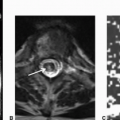
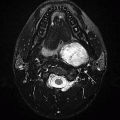
Imaging Findings: There is FLAIR hyperintense signal present in the medial thalami and dorsal medulla bilaterally (A and B). Restricted diffusion is seen in bilateral medial thalami and mammillary bodies (C and D). These findings in the current clinical setting are suggestive of Wernicke encephalopathy, because of thiamine deficiency. Note that low signal on ADC map must be assessed to confirm restricted diffusion (images not shown here).
Discussion: Wernicke encephalopathy.
Wernicke encephalopathy (WE) is an acute neurologic disorder caused by thiamine deficiency. There is about 17% mortality, and the prognosis depends on the timing of thiamine supplementation. The classic clinical triad of “ocular dysfunction, altered consciousness, and ataxia” is only seen in a minority of patients, and neuroimaging plays a critical role in diagnosis.
Deficiency of thiamine is commonly seen in alcoholics (related to dietary deficiency, and not to alcohol per se) and in other disorders associated with malnutrition or decreased absorption (malignancy, GI surgeries, etc.).
Imaging reflects intracellular as well as extracellular edema (cytotoxic and vasogenic edema) and break in blood-brain barrier. Typically, the abnormality is bilaterally symmetrical and the sites involved are periaqueductal gray matter, medial thalami, periventricular region of the third ventricle, tectal plate, and mammillary bodies. Basal ganglia involvement is more common in children.
CT has limited sensitivity for WE and shows hypodensity in involved areas. Long TR MR images (T2/FLAIR) are most sensitive and show hyperintensity in the involved areas. Diffusion restriction (reversible cytotoxic edema) can be seen in acute stages. Some of these regions (typically the mammillary bodies) can show contrast enhancement.
Differential diagnoses:
Artery of percheron infarction: Different clinical presentation. Medial thalamic and mesencephalic involvement seen. The other sites that can be involved with WE are spared.
Deep vein thrombosis: Swelling is more pronounced. Hemorrhage is more common. Deep vein thrombosis can be demonstrated on venogram and with lesser sensitivity in routine imaging.
Osmotic demyelination syndrome: More prominent pontine involvement. Basal ganglia and external capsule are often affected. Can coexist with WE.
Acute disseminated encephalomyelitis (ADEM): Multifocal involvement in white and gray matter.
Variant Creutzfeldt-Jakob disease: Abnormality in thalamic pulvinar, basal ganglia, and cortex. Persistent and more striking diffusion restriction.
Thalamic involvement in hypoxic-ischemic encephalopathy: Clinical picture other sites of involvement that are typical for diffuse ischemic injury including the cortical ribbon and hippocampi.
Metronidazole toxicity: Sites of involvement in the posterior fossa are similar to WE, particularly cerebellar dentate involvement.
References: Ha ND, Weon YC, Jang JC, et al. Spectrum of MR imaging findings in Wernicke encephalopathy: are atypical areas of involvement only present in nonalcoholic patients? AJNR Am J Neuroradiol 2012;33(7):1398-1402. doi: 10.3174/ajnr.A2979
Rumboldt Z, Castillo M, Huang B, et al., eds. Brain imaging with MRI and CT: an image pattern approach. Cambridge, UK: Cambridge University Press, 2012.
Zuccoli G, Pipitone N. Neuroimaging findings in acute Wernicke’s encephalopathy: review of the literature. AJR Am J Roentgenol 2009;192(2):501-508. doi: 10.2214/AJR.07.3959
Zuccoli G, Santa Cruz D, Bertolini M, et al. MR imaging findings in 56 patients with Wernicke encephalopathy: nonalcoholics may differ from alcoholics. AJNR Am J Neuroradiol 2009;30(1):171-176. doi: 10.3174/ajnr.A1280
3 A 25-year-old man was rescued from a residential fire with impaired consciousness and seizures. An MRI was performed; key images are shown below.
|
3a What is the characteristic structure involved with this condition?
A. Internal capsule
B. Caudate nucleus
C. Putamen
D. Globus pallidus (GP)
View Answer
3a Answer D. Globus pallidus (GP). This the most characteristic structure involved with CO poisoning. The clinical history of exposure to fumes in the fire makes this the most likely consideration.
3b What is the most likely diagnosis?
A. Carbon monoxide poisoning
B. Nitrous oxide poisoning
C. Methanol poisoning
D. Opioid overdose
View Answer
3b Answer A. Carbon monoxide poisoning. As explained above, it is the most likely reason for this appearance in the current clinical setting. Nitrous oxide poisoning typically results in neurotoxicity because of vitamin B12 inhibition; the pattern of abnormalities is very similar to vitamin B12 deficiency, such as the presence of dorsal column involvement in the spinal cord. Methanol tends to favor putaminal involvement, and opioid overdose can lead to a pattern similar to hypoxic-ischemic encephalopathy.
|
Imaging Findings: There is FLAIR hyperintensity in the region of globus pallidus (A) and corresponding restricted diffusion seen on DWI (B) and ADC map (C).
Discussion: Carbon Monoxide Poisoning.
Carbon monoxide (CO) is the most common lethal poison worldwide, either suicidal or accidental inhalation. Mechanism of injury is both hypoxic and cellular toxicity.
Its affinity to hemoglobin is about 250 times that of oxygen. Formation of carboxyhemoglobin reduces oxygen-carrying capacity of the blood, causing tissue hypoxia. Cardiotoxicity can result in ischemia, contributing to hypoxic-ischemic damage.
The globus pallidus is the most common and characteristic site of involvement.
Acute and intense poisoning can also result in involvement of other basal ganglia structures, thalami, cortex, hippocampi, brainstem, and cerebellum. In this situation, the pattern can be similar to diffuse ischemic injury from other causes.
In subacute stage, typically 2 to 3 weeks following the insult, up to a third of patients develop leukoencephalopathy related to myelin break down. Bilateral nearly symmetrical lesions are present commonly involving centrum semiovale and periventricular white matter. If the injury is severe, subcortical and posterior fossa white matter can also be involved.
In acute stages, the involved regions are hypodense on CT, hypointense on T1, and hyperintense on T2 and show restricted diffusion. Hemorrhagic products, if present, can result on heterogeneous appearance and some T1 shortening. Acute/subacute stage can show inhomogeneous or peripheral mild contrast enhancement. White matter injury shows up as diffuse T2 hyperintensity and exhibits mild diffusion restriction in early stages. In late stages, atrophy ensues if there is severe enough injury, as a sequel of neuronal necrosis and apoptosis.
Differential considerations:
Cyanide poisoning: Can look identical. Hemorrhagic necrosis of putamen is more commonly seen with cyanide and methanol poisoning.
Diffuse hypoxic-ischemic injury: Preferential globus pallidal involvement is unlikely.
Methanol intoxication: Characteristic putaminal necrosis. Globus pallidus is typically spared. White matter involvement may be seen with methanol.
Mitochondrial disorders, Leigh disease: Younger age group. Putaminal and brainstem involvement is more common.
References: Kinoshita T, Sugihara S, Matsusue E, et al. Pallidoreticular damage in acute carbon monoxide poisoning: diffusion-weighted MR imaging findings. AJNR Am J Neuroradiol 2005;26(7):1845-1848.
Lo CP, Chen SY, Lee KW, et al. Brain injury after acute carbon monoxide poisoning: early and late complications. AJR Am J Roentgenol 2007;189(4):W205-W211. doi: 10.2214/AJR.07.2425
Rumboldt Z, Castillo M, Huang B, et al, eds. Brain imaging with MRI and CT: an image pattern approach, 1st ed. Cambridge, UK: Cambridge University Press, 2012.
4 A middle-aged man “found down” on the side walk was brought to the ER. Initial EKG shows sinus tachycardia and nonspecific T-wave changes. A head CT was performed; key images are shown below.
|
4a Which of the following is the most likely diagnosis?
A. Wilson Disease
B. CO monoxide poisoning
C. Postictal change
D. Methanol toxicity
View Answer
4a Answer D. Methanol toxicity. Of the available options, the prominent putaminal and white matter involvement is most commonly seen with methanol toxicity.
4b Further investigation reveals severe metabolic acidosis. What structure is at particularly high risk for involvement with this condition?
A. Cerebellum
B. Thalami
C. Hippocampus
D. Optic nerve
View Answer
4b Answer D. Optic nerve.
|
Imaging Findings: There is bilateral putaminal hypodensity and hypoattenuation in frontal subcortical and deep white matter on CT.
Discussion: Methanol is found in antifreeze solutions, varnishes, and paint fuel and also in bootlegged alcohol. Poisoning can result from intentional or accidental ingestion. Its metabolites formic acid/formate ion are responsible for toxicity by mitochondrial enzyme inhibition and resultant tissue hypoxia and also by causing metabolic acidosis.
Bilateral putaminal necrosis is the typical imaging presentation. Nonhemorrhagic lesions show CT hypodensity, T2 hyperintensity, T1 hypointensity, and diffusion restriction. Associated hemorrhage is quite common. Optic nerve involvement is common and may show up on dedicated imaging as T2 hyperintensity. The less common sites of involvement are globus pallidus, brainstem, subcortical white matter, and rarely peripheral lesions without central involvement. Peripheral mild contrast enhancement can be seen in acute/subacute stages.
The exact reason for putaminal predilection is not known. The proposed theories include high metabolic rate, venous drainage pattern, and high regional accumulation of methanol.
Differential Diagnosis:
Diffuse ischemic injury: Generally bilateral, involvement of basal ganglia and cortical ribbon, T2 hyperintensity, and T1 hypointensity with diffusion restriction. History of a contributory event such as cardiac arrest, drug overdose, or drowning can be helpful.
Cyanide poisoning: Also has characteristic putaminal involvement; however, white matter changes are more typical with methanol poisoning.
Mitochondrial disorders: Pediatric population is more commonly affected. Movement disorder is not a common presenting symptom.
Wilson disease: Putaminal T2 hyperintensity is also common in Wilson disease. Other common areas of involvement include caudate, globus pallidus, and ventrolateral thalamus. Rarely cortical/subcortical region, brainstem, and cerebellar vermis may also be involved.
References: Gupta N, Sonambekar AA, Daksh SK, et al. A rare presentation of methanol toxicity. Ann Indian Acad Neurol 2013;16(2):249-251. doi: 10.4103/0972-2327.112484
Zakharov S, Kotikova K, Vaneckova M, et al. Acute methanol poisoning: prevalence and predisposing factors of haemorrhagic and non-haemorrhagic brain lesions. Basic Clin Pharmacol Toxicol 2016;119(2):226-238. doi: 10.1111/bcpt.12559
5 A 60-year-old male patient presents with an abnormal MRI; key images are shown below.
|
5a What is the most likely history in this patient?
A. Recent upper respiratory tract viral infection
B. Rapidly progressive cognitive decline
C. Recent liver transplant
D. Recently diagnosed small cell lung cancer
View Answer
5a Answer C. Recent liver transplant. The images show central pontine signal changes, typically seen with osmotic demyelination, which may occur in posttransplant setting. Recent upper respiratory tract viral infection history is typically seen with acute disseminated encephalomyelitis (ADEM). The images are not typical for Creutzfeldt-Jakob disease or paraneoplastic limbic encephalitis to suggest options B and D, respectively.
5b Following images are from a different patient with the same history. What is the most likely diagnosis?
|
A. Creutzfeldt-Jakob disease
B. Osmotic demyelination
C. Paraneoplastic limbic encephalitis
D. Acute disseminated encephalomyelitis
View Answer




5b Answer B. Osmotic demyelination. It is to be emphasized that although central pontine involvement is typical, extrapontine and mixed central and extrapontine involvement may also be seen with osmotic demyelination, as shown in this companion case.
Imaging Findings: Figure 1. Axial T2-weighted imaging demonstrates increased signal in the pons with sparing of the periphery and corticospinal tracts (A) and associated restricted diffusion (B), consistent with central pontine myelinolysis (osmotic demyelination).
Figure 2. FLAIR hyperintensity seen in bilateral thalami, bilateral insular, and cerebellar regions, compatible with a combination of pontine and extrapontine myelinolysis.
Discussion: Osmotic demyelination.
Osmotic demyelination is a rare disorder commonly in middle-aged patients characterized by symmetrical and noninflammatory demyelination involving pons and extrapontine sites (pontine and extrapontine myelinolysis). It is thought to be caused by aggressive correction of hyper- or hyposmolar states. The classic clinical scenario is rapid correction of hyponatremia (by more than 12 mmol/L/day) in an alcoholic. Though rapid correction of hyponatremia is the classic scenario, the disease can be seen in other osmolar abnormalities and in chronic diseases. Isonatremia doesn’t rule out the disease. Associated conditions include malnutrition, prolonged diuretic use, liver failure, organ transplant, and extensive burns.
Pons is the classical site of involvement.
Pontine tegmentum and corticospinal tracts are generally spared. Extrapontine involvement is fairly common, with an incidence close to that of pontine involvement, but is generally seen with pontine involvement. The sites commonly involved are cerebellum, basal ganglia, thalami, external capsule, lateral geniculate bodies, hippocampi, and cerebral gray-white junction. The periventricular and subpial sites are typically spared. Isolated extrapontine disease is seen in a minority, about 20%.
Histologic studies have shown that oligodendroglial cells are most susceptible to CPM-related osmotic stresses.
Conventional imaging findings (MR and CT) typically lag clinical manifestations, limiting the utility of imaging in early diagnosis of CPM. CT is insensitive and can show symmetrical hypodensities in the involved regions. MRI is the investigation of choice. DWI can show restriction as soon as 24 hours following clinical symptoms, the diffusion restriction resolving over 1 to 2 weeks. T2 signal abnormality develops over several days following clinical symptoms. MR imaging findings include symmetric signal intensity abnormality in the central pons on T2-weighted and FLAIR imaging. This may progress to classic hyperintense “trident-shaped” central pontine abnormality, with sparing of the ventrolateral pons and corticospinal tracts, which can appear as “snake eye.” In subacute stages, mild peripheral or ill-defined enhancement can be seen in a small percentage of patients.
The clinical presentation is variable and depends on the site of involvement. “Biphasic presentation” (initial encephalopathy followed by improvement with correction of osmolyte disturbance and then sudden deterioration) is often seen. The pontine involvement is characterized by tetraplegia, bulbar and pseudobulbar palsies, altered mental status, and coma. Movement disorders can be seen with basal ganglia involvement. Historically, the disease was thought have a dismal prognosis. But recent literature points to variable prognosis, with up to 50% patient survival, many without long-term adverse effects. Extent of imaging abnormality does not predict clinical outcome. Patients who survive show residual signal abnormality or cavitation in the pons.
Differential diagnoses:
Pontine infarction: Generally reaches anterior pontine margin and rarely symmetrical.
Demyelination: Rarely symmetrical and typical morphology and distribution can be seen in supratentorial white matter lesions.
Neoplasm: Generally pontine glioma is a disease of the young. Associated pontine enlargement is typical.
References: Abbott R, Silber E, Felber J, et al. Osmotic demyelination syndrome. BMJ 2005;331(7520):829-830.
Alleman AM. Osmotic demyelination syndrome: central pontine myelinolysis and extrapontine myelinolysis. Semin Ultrasound CT MR 2014;35(2):153-159. doi: 10.1053/j.sult.2013.09.009
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree