COCHLEOVESTIBULAR NERVE AND CEREBELLOPONTINE ANGLE INFECTIONS AND NONINFECTIOUS INFLAMMATORY CONDITIONS
KEY POINTS
- Magnetic resonance imaging and computed tomography are commonly performed to look for abnormalities of the cochleovestibular nerve or cerebellopontine angle.
- Pathology in this region may be diverse, but the vast majority of cases are straightforward diagnostic situations.
- Imaging can be very helpful to triage patients with cochleovestibular nerve dysfunction to the next best step in the medical decision making process.
The most common inflammatory condition of the cochleovestibular nerve (CVN) may be a viral neuritis such as that due to the herpes group, but this is only occasionally demonstrated on magnetic resonance imaging (MRI) as CVN, Scarpa ganglion, and/or labyrinthine enhancement. Viral neuritis is typically a presumptive diagnosis that cannot be confirmed clinically with certainty.
Other inflammatory conditions of the CVN may be serious complications of infectious disease such as acute otomastoiditis or conditions that may require other specific therapies such as Wegener granulomatosis or Lyme disease. For the purposes of this chapter, these conditions are grouped into the two broad categories of infectious and noninfectious inflammatory diseases since the etiologies vary considerably, while the imaging features related to the nerve itself vary little.
ANATOMIC AND DEVELOPMENTAL CONSIDERATIONS
Applied Anatomy
A diligent search of the entire course of the CVN is essential for evaluating imaging studies performed in patients with symptoms referable to the nerve. Exclusion of causative pathology with a high degree of confidence is the usual goal of the study.
In order to accomplish such a search, the computed tomography (CT) and MRI anatomy of the CVN must be completely understood, including its brain stem nucleus, its course through the brain stem, its cisternal segment, its course through the internal auditory canal (IAC), and points of distribution of its three main branches to the cochlea and vestibular system. This anatomy is presented in detail in Figures 104.11 through 104.14 and Chapter 104.
IMAGING APPROACH
Techniques and Relevant Aspects
In general MRI and CT in this anatomic region almost always requires the highest possible spatial resolution. These factors used to develop optimal protocols are discussed in detail in Chapters 1 through 3. Specific protocols for magnetic resonance (MR) and CT studies for investigating CVN problems in general appear in Appendixes A and B. Any such MR study must include a three-dimensional steady state acquisition with nominal section thickness 1 mm that can be analyzed in any plane. The same type of CT data analysis is necessary.
The CVN and cerebellopontine angle (CPA) are typically studied with dedicated contrast-enhanced studies of the temporal bone. These studies must also include definitive high-resolution images of the posterior fossa and CVN. MR studies should also always include images that are as definitive as possible for evaluating the membranous labyrinth of the inner ear and related structures such as the vestibular aqueduct. The inner ear is the “end organ” of the CVN innervation, and its status will almost always be in question when potential pathology of the CVN and CPA is suspected. Non–contrast-enhanced CT only may be used as a supplement to evaluate the inner ear anatomically, but that is the subject of pathologic processes discussed in other chapters even though they may be functionally related to CVN and CPA problems.
Pros and Cons
MRI should be done first, as it most confidently excludes causative pathology at all segments (i.e., the brain stem, cisternal, within the IAC, and intracochlear [modiolus] segments) of the CVN from its brain stem nucleus to the cochlea and vestibule. MRI is more sensitive than CT for excluding intra-axial pathology such as demyelinating disease, pia-arachnoid diseases, and small neoplasms of the nerve that might involve the cisternal segment or the segment within the IAC.
CT may be done as a supplement to most confidently exclude predisposing conditions of the middle ear and mastoid, such as sites of a primary inflammatory process or cerebrospinal fluid leakage—inner ear anatomic variants that might predispose to infection of the labyrinth and then the CVN. This supplemental imaging may be done as a routine study or only when MR findings need to be clarified with supportive bone detail.
If there is obvious potentially acute or subacute infectious disease involving the temporal bone, such as acute otomastoiditis or necrotizing otitis externa (NOE) leading to CVN dysfunction, then a CT may be done initially.
If a disease process such as NOE or skull base osteomyelitis is established as the cause of CVN dysfunction, then radionuclide studies may be used to monitor the response of the disease to specific antimicrobial therapy.
SPECIFIC DISEASE/CONDITION
Infectious Conditions of the Cochleovestibular Nerve and Cerebellopontine Angle
Etiology
Acute suppurative (pyogenic) bacterial infections of the middle ear and mastoid can cause CVN dysfunction due to involvement of the nerve and or membranous labyrinth; this is a medical emergency. Chronic infections such as NOE (Chapter 114) only infrequently are complicated by CVN dysfunction. Other chronic infections are more difficult to diagnose. Other organisms as diverse as blastomycosis and actinomycosis as well as various fungi can involve the CVN when they cause skull base osteomyelitis. More typically, pseudomonas, proteus and resistant staphylococcus, or other lesser known bacteria will cause skull base osteomyelitis with secondary cranial neuropathies. Lyme disease may result in CVN dysfunction as a presenting complaint; however, CVN symptoms will more commonly be overshadowed by the facial nerve presentation of this disease when that region of the central nervous system is involved.1,2 Syphilis3,4 schistosomiasis, Cryptococcus, and tuberculosis can cause CVN dysfunction, but these diseases will commonly involve more than one cranial nerve as a manifestation of chronic meningitis.
Prevalence and Epidemiology
These infections are all relatively uncommon causes of CVN dysfunction. Their prevalence in patients with underlying or causative disease will follow that of the population at risk for those diseases. For instance, younger children and young adults are at more risk for acute otomastoiditis; the same is true for diabetics and others with skull base osteomyelitis. The risk of conditions such as Lyme disease and schistosomiasis follows that of likely exposure to the infectious vector.
Clinical Presentation
Patients will generally present with hearing loss, tinnitus, and vertigo or balance problems and possibly facial nerve palsy. “Fullness” in the ear is another common complaint. The presentation can vary tremendously depending on the disease stage and involved site. For instance, Lyme disease may include skin and rheumatologic manifestations as well as those of the CVN.
Pathophysiology and Patterns of Disease
The nerve will become inflamed and edematous in the earlier stages of the disease. It may be that the offending infectious agent itself injures the nerve or the swelling due to an infection causes nerve swelling that produces a complicating ischemic neuropathy. A complicating labyrinthitis (Chapter 117) may also occur.
The earlier inflamed and edematous CVN may eventually become atrophic once the infection is resolved. A secondary fibro-osseous obliterative labyrinthitis may also occur (Chapter 117).
Manifestations and Findings
Computed Tomography
CT will usually be normal if there is not underlying temporal bone pathology or if the causative pathology involves the segment of the nerve in the IAC or the brain stem. CT will occasionally demonstrate inflammatory nerve changes in the CPA. If performed, it must be used to exclude structural lesions that might contribute to the mechanism of infection. If positive, it will demonstrate structural pathology along the course of the nerve as diverse as otomastoiditis, erosion of the bone, fibro-osseous changes/obliteration of the labyrinth, and abnormal meningeal enhancement (Figs. 131.1A–C). The patterns of these diseases are discussed in detail in respective chapters in Section II, and the patterns of other etiologies of CVN deficits are described in Chapters 134 and 135.
Magnetic Resonance
MRI may show a range of abnormal enlargement and increased enhancement of the affected CVN anywhere along its course (Fig. 133.2). It must also be used to exclude structural lesions affecting the cochleovestibular nerve—infectious or otherwise. If positive, it may demonstrate structural pathology along the course of the nerve as diverse as otomastoiditis, focal enhancement along any segment of the nerve, and abnormal meningeal enhancement (Figs. 117.1B–E and 117.1l). The basic patterns of both inflammatory and other diseases are discussed in detail in representative chapters in Section II, and the patterns of other etiologies of CVN deficits are described in Chapters 134 and 135.

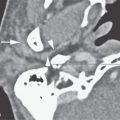
FIGURE 133.1. Computed tomography (CT) and magnetic resonance imaging findings in four patients with bacterial infectious disease of the cochleovestibular nerve and cerebellopontine angle. A, B: Patient 1. Enlargement and enhancement of the seventh and eighth cranial nerve cisternal segment caused by syphilis is seen as abnormal enhancement from their root entry zones into the internal auditory canal (IAC) (arrows). Otosyphilis may also lead to labyrinthitis and osteitis of the otic capsule. C, D: Patient 2, who presented with acute bacterial otomastoiditis and developed meningitis and hearing loss. In (C), CT study shows erosion of bone over the lateral semicircular canal (arrow) and possible labyrinthine obliteration (arrowhead) explaining how the infectious process has invaded the labyrinth. In (D), the contrast-enhanced T1-weighted (T1W) image shows enhancement in the mastoid and in the labyrinth (arrow) with spread of infection to the fundus of the IAC involving the nerves (arrowhead). E: Patient 3 developed labyrinthitis secondary to pasturella meningitis. The contrast-enhanced T1W image shows multifocal labyrinthine (arrowhead), meningeal/neural enhancement (arrow). Disease seen spreading along the pia-arachnoid in other locations was a critical differentiating feature between viral (not shown) neuritis/labyrinthitis and meningitis on the basis of imaging. F: Patient 4. Enhancement of multiple cranial nerves and basilar meningeal enhancement points toward meningeal infection. Cerebrospinal fluid analysis revealed tuberculosis.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree