This article presents clinical characteristics and radiologic features of congenital cervical cystic masses, among them thyroglossal duct cysts, cystic hygromas, branchial cleft cysts, and the some of the rare congenital cysts, such as thymic and cervical bronchogenic cysts. The imaging options and the value of each for particular masses, as well as present clinical and radiologic images for each, are discussed.
Congenital cervical cystic masses comprise an uncommon group of lesions that is usually encountered during infancy and childhood. The prevalence of these lesions varies from common (thyroglossal duct cysts, branchial cleft cysts, and cystic hygromas) to very rare (thymic and cervical bronchogenic cysts). The absolute number remains unknown. Thyroglossal duct (TGD) cysts are the most common mass found in the midline of the neck in children. Anomalies of the branchial apparatus include branchial, thymic, and parathyroid anomalies, which may manifest as cysts, sinuses, fistulae, and ectopic glands.
Clinical history and physical examination of the patient are important elements in the evaluation of a suspected congenital neck mass ( Table 1 ). Familiarity with the embryology and anatomy of the cervical region frequently allows the differential diagnosis to be narrowed. Congenital cervical cystic lesions are usually slow-growing masses and typically cause symptoms only due to enlargement or infection. A painless soft or fluctuant cervical mass is the first clinical manifestation in most cases.
| Lesion | Peak Prevalence (Age in Years) | Sex Predilection | Usual Location |
|---|---|---|---|
| Thyroglossal duct cyst | <10 | Equal | Hyoid level or below (80%), within 2 cm of midline |
| Branchial cleft cyst | |||
| First | Middle age | F > M | Parotid, external auditory canal |
| Second | 10–40 | Equal | Upper neck, mandibular angle, lateral to carotid vessels |
| Third | 10–30 | — | Left posterior cervical triangle |
| Fourth | Any age | — | Sinus tract arising from left pyriform sinus |
| Cystic hygroma | <2 | Equal | Posterior cervical triangle, oral cavity |
| Dermoid cyst | 10–30 | Equal | Floor of mouth |
| Epidermoid cyst | Infancy | Equal | Floor of mouth |
| Thymic cyst | 2–13 | M > F | Low anterolateral neck (L > R) |
| Bronchogenic cyst | Any age | M > F | Low anterolateral neck |
Following physical examination, ultrasonography (US) is usually performed. US helps to confirm the cystic nature of the lesion and extent of the mass, and to demonstrate its relationship to surrounding normal structures. Computed tomography (CT) also provides this information, and is ideally suited for evaluation of larger masses that cannot be entirely visualized with US. Moreover, CT is superior for detecting calcification and, when contrast material is administered, the vascularity of lesions. Magnetic resonance (MR) imaging demonstrates the full extent of the mass and provides important supplemental information for accurate preoperative planning. This information can be especially relevant in cases of extension into the mediastinum or deep spaces of the neck. Furthermore, MR imaging offers superior resolution for evaluating masses located in anatomically complex areas, such as the floor of the mouth.
Thyroglossal duct cyst
Embryology
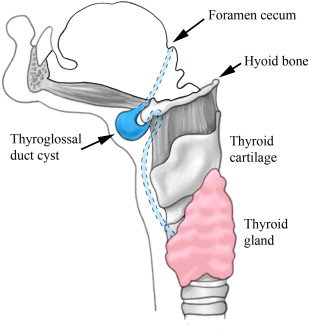
During the fourth week of gestation, the thyroid gland originates as a diverticulum from the floor of the pharynx (tuberculum impar) at a site that later becomes the foramen cecum of the base of the tongue. The gland then grows caudally into the loose prepharyngeal connective tissues, just anterior to or through the eventual location of the hyoid bone, to rest in the lower midline of the neck. As the gland moves downward, it leaves behind an epithelial trace attached to the foramen cecum, known as the thyroglossal tract. The thyroglossal tract runs ventral to the developing hyoid bone, then assumes a curved course behind it, as the hyoid bone rotates and takes its adult position. It then continues downward anterior to the thyrohyoid membrane. The thyroglossal duct generally obliterates between the fifth and tenth week of gestation, leaving behind a proximal remnant at the foramen cecum (at the base of the tongue) and a distal remnant (pyramidal lobe of the thyroid). The duct is intimately associated with developing hyoid bone, either within the periosteum of the hyoid bone or even passing through it. Failure of the thyroglossal duct to obliterate before the formation of the mesodermal anlage of the hyoid bone results in its persistence during development and after birth. An embryologically defined line extending from the tongue base to the thyroid gland determines the site of anomalies of the thyroglossal duct ( Fig. 1 ). The majority of thyroglossal duct cysts are either juxtahyoid or infrahyoid.
Thyroglossal duct anomalies constitute the vast majority of congenital midline cervical masses seen in children, accounting for 70% of congenital neck anomalies, and the second most common benign neck mass in pediatric patients after benign lymphadenopathy. About 50% of patients present before 20 years of age, with a second group of patients presenting in young adulthood. No gender predilection has been reported. Rare cases of hereditary thyroglossal duct cysts have been reported; typically these cysts have an autosomal dominant pattern of transmission and occur in prepubertal girls.
Clinical Characteristics
TGD cysts are epithelial remnants of the thyroglossal tract located adjacent to the hyoid bone (60%), between the hyoid bone and base of the tongue (24%), between the hyoid bone and pyramidal lobe of the thyroid gland (13%); the remainder are intralingual (3%). TGD cysts are located in the midline (75%) or slightly off-midline (25%) in the anterior neck, usually within 2 cm of the midline. Of the lesions in a paramedian location, most will occur on the left for unclear reasons.
The TGD cyst arises as a cystic expansion of a remnant of the thyroglossal duct tract. The stimulus for the expansion is not known; one postulate is that lymphoid tissue is associated with the tract hypertrophies at the time of a regional infection, thereby occluding the tract with resultant cyst formation. The majority of patients have a history of a preceding upper respiratory tract infection. A retention phenomenon with blocked thyroglossal duct and accumulation of secretions has been described as another possibility.
Patients with TGD cysts usually present with a palpable asymptomatic midline neck mass in a pediatric or young adult patient at or below the level of the hyoid bone. Midline location and close association with the hyoid bone are the only nearly universal traits of these lesions. The mass moves during swallowing or on protrusion of the tongue, due to its attachment to the tongue via the tract of thyroid descent. Some patients will have neck or throat pain, or dysphagia. Up to half of TGD cysts are not diagnosed until adult life. TGD anomalies occur in approximately 7% of the population, although only a minority of these is ever symptomatic. The tract can lie dormant for years or even decades until a stimulus leads to cystic dilation. Many cystic remnants of the thyroglossal tract are never detected clinically. Infection can sometimes cause the transient appearance of a mass or enlargement of the cyst, at times with periodic recurrences. Spontaneous drainage may also occur.
Approximately 15% to 33.8% of thyroglossal anomalies present as fistulae. The fistulous openings are almost always considered to be a secondary feature, resulting from infection with either a spontaneous or a surgical drainage. Congenital fistulae in the newborn have been described. Approximately 1% to 2% of patients presenting with TGD cysts have an ectopic thyroid gland within the wall of the cyst.
Radiologic Features
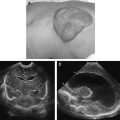
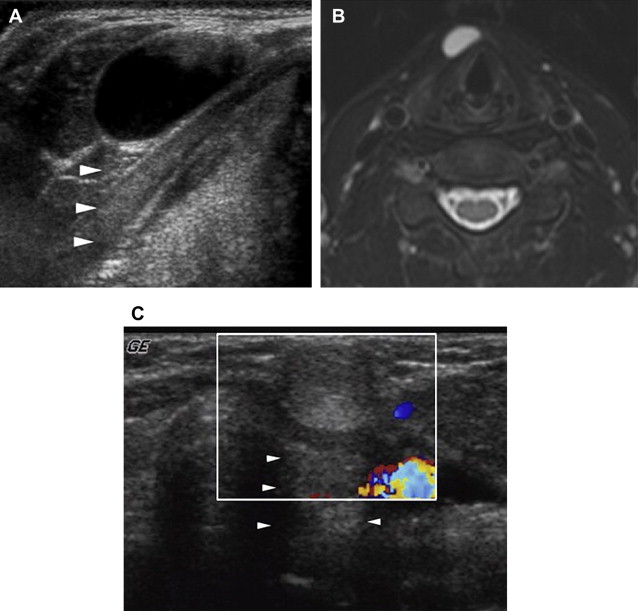
At sonography, TGD cysts have a variable, complex sonographic pattern ranging from a typical anechoic to pseudosolid appearance. The finding of an anechoic mass with no perceptible or thin outer wall in the midline anterior neck is characteristic of a thyroglossal duct cyst ( Fig. 2 A, B). However, this classic appearance is seen in less than half of the cases. More commonly, these cysts appear as homogeneous or heterogeneous complex hypoechoic masses, often with increased through-transmission. The cysts may have variable degrees of fine to coarse internal echoes and, infrequently, septa. Hyperechoic, pseudosolid appearance is occasionally seen in adults; however, their cystic nature is only confirmed with posterior enhancement or shift of the lesion’s content after application of transducer pressure (see Fig. 2 C). There is no correlation between the sonographic appearance and pathologic evidence of hemorrhage, infection, and inflammation. Heterogeneity seen in thyroglossal duct cysts on sonography is more likely due to the proteinaceous content of the fluid secreted from the cyst wall rather than to infection. Preoperative sonographic visualization of normal thyroid tissue is sufficient to exclude a diagnosis of ectopic thyroid tissue and obviates routine thyroid scintigraphy.
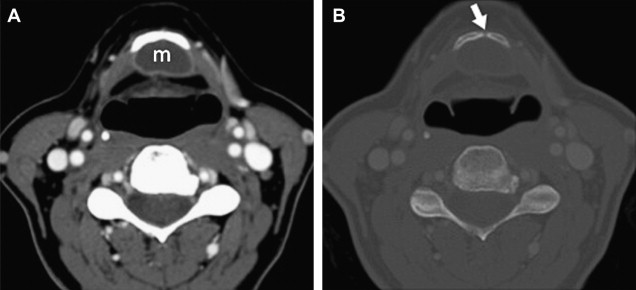
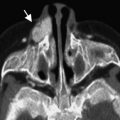
A low-density cystic midline mass is usually seen on CT scan along the expected course of the thyroglossal duct with a smooth, thin, well-defined wall ( Fig. 3 ). The mass has homogeneous low attenuation, the values of which correspond to those of fluid (10–18 HU). Elevated attenuation values of the fluid cyst reflect increased protein content and generally correlate with a history of prior infection. Although thyroglossal duct cysts are usually unilocular, septations may be seen occasionally. A peripheral rim of enhancement is usually seen on contrast-enhanced scans. The fascial planes adjacent to the cyst can be preserved. Abnormal fascial planes, manifesting as thickening of the platysma or strap muscle with cutaneous thickening and induration of the subcutaneous fat, are usually related to postinflammatory changes ( Fig. 4 ).