Abstract
Doppler ultrasound can be used to assess vascular beds in the maternal, fetal, and placental circulation. The vessels most frequently evaluated in clinical practice are the uterine, umbilical and (fetal) middle cerebral arteries, and the ductus venosus. Evaluation of blood flow in various vascular beds, combined with clinical information, provides insight into maternal adaptation to pregnancy, placental resistance, and fetal cardiovascular status, and may therefore guide pregnancy management.
Keywords
umbilical artery Doppler, middle cerebral artery Doppler, ductus venosus Doppler, Doppler techniques
Introduction
Doppler ultrasound (US) can be used to assess waveform patterns of blood flow in various vascular beds in the maternal, fetal, and placental circulation. The information gained from the analysis of waveforms in combination with clinical factors provides insight into maternal adaptation to pregnancy, placental resistance, and fetal cardiovascular status, and thus can guide pregnancy management in many conditions. Doppler evaluation can be roughly divided into arterial, venous, or cardiac Doppler. Doppler evaluation of the uterine artery, umbilical artery (UA), middle cerebral artery (MCA), descending aorta, ductus venosus (DV), inferior vena cava, umbilical vein, and the hepatic veins provides valuable information on placental and fetal circulations in pregnancy. However, in clinical practice placental (uterine and UA Doppler), MCA, and DV Doppler are the most frequently used. Cardiac Doppler, which is used primarily for evaluation of diastolic function, global myocardial performance, and cardiac ejection force or systolic performance, is reviewed in Chapter 74 , Chapter 75 , Chapter 76 , Chapter 77 , Chapter 78 , Chapter 79 , Chapter 80 , Chapter 81 , Chapter 82 , Chapter 83 , Chapter 84 , Chapter 85 , Chapter 86 , Chapter 87 , Chapter 88 , Chapter 89 , Chapter 90 , Chapter 91 , Chapter 92 , Chapter 93 , Chapter 94 . This chapter will discuss technique and applications for the vessels most commonly examined in pregnancy: uterine, umbilical, and middle cerebral arteries, as well as the DV.
Fundamentals of Doppler Imaging
Arterial Doppler
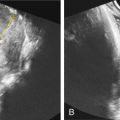
A simple way of thinking about the arterial flow waveform (in all vascular beds except the coronary) is that it depends on the forward ejection of blood from the fetal heart, the elastic properties of the vessel, and the viscosity of ejected blood. The most relevant measures are the peak systolic velocity (PSV) and the end diastolic velocity (EDV). During systole, the velocity of the blood ejected after the semilunar valve opens increases to a maximum (the PSV), evidenced as the highest point in the waveform. During diastole, when the cardiac contraction can no longer maintain forward flow against the elastic properties of the downstream vascular bed and the viscosity of the blood, flow decelerates to its nadir (the EDV), the lowest point on the arterial waveform. The EDV is primarily dependent on downstream vascular impedance, the combined result of resistance and vascular response, and to a lesser degree input pressure. Fig. 171.1 illustrates a normal arterial waveform.

Optimal measurement of flow velocity is obtained when the US beam at a zero-degree angle to the blood flow through the vessel. Under these circumstances the intensity of the reflected beam is highest, producing a high signal to noise ratio and the measured blood flow velocity corresponds to the actual velocity of red cells in the measured vessel. The Doppler equation describes how the frequency shift relates to the actual flow velocity, which is reduced by the cosine of the angle between the vessel and the US image beam. This can lead to overestimation of flow velocities unless the angle correction on the US machine is used as the incident angle increases. However, minimizing the need for angle correction is ideal, because once the angle exceeds about 20 degrees, the cosine drops rapidly with small angle changes, leading to larger error in measurements. In contrast to the semiquantitative Doppler indices, absolute blood flow quantification also requires accurate measurement of blood vessel diameter. Since consistent zero-degree incident angle insonation and accurate measurement of vessel diameter are challenging, semiquantitative, angle-independent Doppler indices are typically used in clinical practice. These indices, which are related to downstream vascular impedance, depend on the relationship between PSV and EDV (as opposed to their absolute values). They include the UA systolic/diastolic (S/D) ratio (PSV/EDV), the pulsatility index (PI) (PSV-EDV/Tmax) and the resistive index (RI) (PSV-EDV/PSV). The PI provides the least variation and margin of error, and is thus most reproducible. All of these indices decrease gradually with increasing gestational age.
The placental circulation can be evaluated with uterine artery Doppler (maternal compartment) and UA Doppler (fetal compartment of the placenta). Uterine artery Doppler targets the spiral and arcuate arteries. In very early pregnancy, the uterine arteries have high resistance and recoil, which limits blood flow into the uterus. As pregnancy progresses and the vascular tree undergoes trophoblastic transformation, the walls of these vessels become less muscular creating a low-resistance, high-capacitance system. As a result, first-trimester uterine artery waveforms demonstrate a high pulsatility index and an early diastolic notch. As normal placental development and vascular relaxation occurs, the pulsatility index decreases, and the diastolic notch disappears in the second trimester. Failure of this normal progression, as evidenced by persistent elevated uterine artery resistance and notching, suggests abnormal placental development. This is associated with an increased risk of maternal hypertension and/or placental dysfunction, as well as preeclampsia and fetal growth restriction.
UA Doppler is used to measure impedance in the fetal villous vascular tree, which is related to vascular surface area and vessel elasticity. In singleton gestation, impedance increases if there is decreased villous sprouting, villous atrophy, or placental thrombus. In monochorionic twin pregnancies, pressure from direct arterial anastomoses can create characteristic waveform patterns that are related to opposing fetal pulse pressures.
UA Doppler indices normally decline (indicating decreased impedance) as pregnancy progresses. Because of the large surface area of the villous circulation, Doppler indices do not show increased impedance until at least 30% of the villous vasculature is abnormal. Absent or reversed UA end diastolic flow is not observed until 60%–70% of the placenta is affected. It is important to recognize that the mechanisms that lead to abnormal elevation of umbilical (and uterine artery) Doppler index are the histologic properties of the placental vascular bed resulting in decreased perfusion. Risk of fetal growth restriction, nutrient deficiency, acid-base imbalance and stillbirth are related to the degree of Doppler abnormality. Identifying absent or reversed UA EDV is an important first step in the assessment of fetal status in the setting of placental dysfunction. Combination of the UA with multivessel Doppler and biophysical parameters is required to determine the optimal frequency of monitoring and identifying delivery triggers to maximize gestational age and neurodevelopment, while minimizing the risk of fetal or neonatal death.
Fig. 171.2A is an example of a normal UA waveform. Figs. 171.2B–D show increased resistance, absent EDV and reversed EDV, respectively.

The fetal cerebral circulation can be evaluated with MCA Doppler. Interpretation of the MCA Doppler must be done in the context of the clinical situation, because the waveform can be altered by several factors that may impact flow indices or blood flow speed, measured as the PSV. In response to fetal hypoxia, the cerebral vessels dilate to allow preferential shunting of oxygenated blood to the brain, resulting in an increase in EDV and a decline in the Doppler indices. In growth-restricted fetuses, this is known as brain sparing. Early changes in fetal autoregulation and redistribution of cardiac output can be apparent by examination of the cerebroplacental ratio (MCA PI/UA PI) before qualitative changes in the UA waveform are apparent. Of note, placental pathology that predominantly results in immature thick-walled villi may result in a significant decrease in oxygen and carbon dioxide diffusion but little change in villous perfusion. This makes the MCA Doppler important in the evaluation of placental function, because isolated brain sparing may be the only hint of placental dysfunction when umbilical perfusion is normal. This is of particular importance in late-onset fetal growth restriction, where redistribution of cardiac output toward the brain may be the only apparent sign of fetal compensation before overt fetal compromise, and may also predict adverse neonatal outcome in normally grown fetuses. Other factors such as fetal hypertension may also manifest as decreased cerebral flow indices. Alteration in blood viscosity impacts the MCA PSV. Acceleration of blood flow (increased PSV) is seen with fetal anemia, and conversely decreased PSV with polycythemia. Under physiologic conditions fetal partial pressure of carbon dioxide (paCO 2 ) is the primary regulator of the MCA PSV; an increase in PSV may also be seen with placental dysfunction when fetal paCO 2 is increased.
Venous Doppler
The typical venous waveform, which depends on volume pressure changes in the atria throughout the cardiac cycle, is characterized by four phases: S-wave (height of systole), V-trough (ventricular relaxation after the height of contraction), D-wave (early diastole), and a-wave (atrial systole). The first peak (S-wave) is seen after blood flow increases throughout systole to its maximum. The V-trough (end systole) follows as the ventricles relax and forward flow decreases. This marks the point at which the atrioventricular valves open as atrial pressure exceeds ventricular pressure. The D-wave (diastolic forward peak) describes the increase of forward flow during the early diastolic (passive) filling of the ventricles. This is followed by a trough corresponding to atrial systole (a-wave) when an acute rise in atrial pressure creates increased resistance to forward flow as part of active diastole (atrial contraction). Fig. 171.3 shows a normal venous waveform. All central venous vessels demonstrate this waveform and exhibit higher pulsatility the closer to the heart they are sampled. The umbilical vein is an exception because it has a constant waveform after 8 to 12 weeks of gestation because the DV attenuates retrograde atrial pressure changes to the vein.