EYE: RETINAL, CHOROIDAL, AND HYALOID DETACHMENTS
KEY POINTS
- Leukocoria is an important physical sign, and patients with this usually come to computed tomography and/or magnetic resonance imaging.
- The vast majority of detachments are imaged with ultrasound rather than with computed tomography or magnetic resonance imaging.
- Most detachments as seen on computed tomography and magnetic resonance imaging are findings associated with underlying causative pathology.
- Imaging identification of such detachments on imaging is important since it will sometimes help in critical medical decision making.
- Tumors detected by computed tomography or magnetic resonance imaging should be evaluated to determine if they are exophytic or endophytic.
- A radiodense lesion can represent either an intraocular foreign body or hemorrhage.
The conditions discussed in this chapter are associated with a wide range of causative pathology.
Ocular membrane detachments and related fluid collections sometimes represent the primary ocular pathology (Fig. 45.1). More often, with regard to computed tomography (CT) and magnetic resonance imaging (MRI) in particular, they are seen as effects of causative intraocular and extraocular pathology and should be recognized as such. At times, the therapy in these conditions will be focused on both the causative pathology and limiting the effects of secondary membrane detachments.
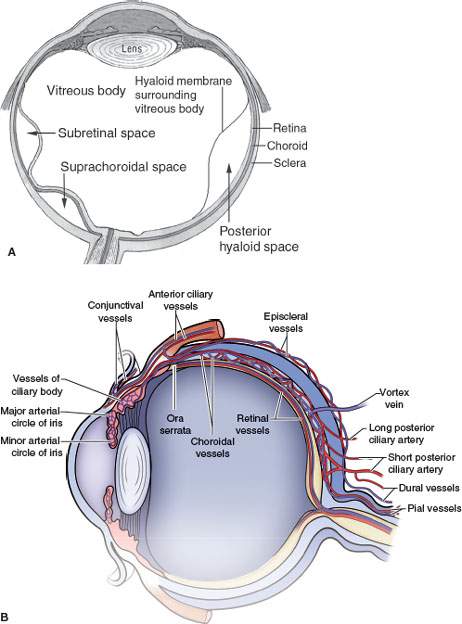
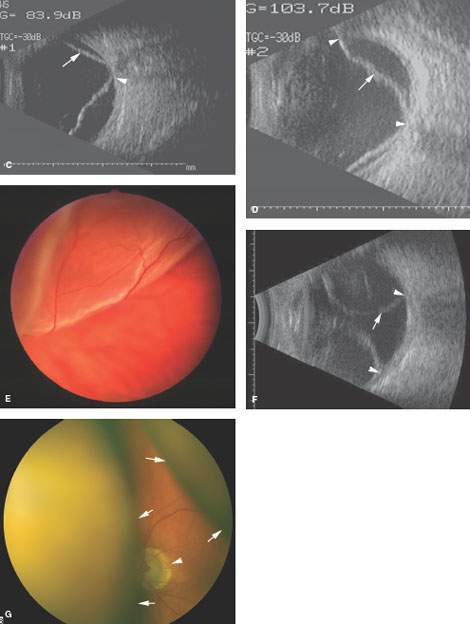
FIGURE 45.1. A: Line diagram showing various retinal layers and types of detachments. B: Anatomy of the vasculature of the eye emphasizing the relationships of the vessels to various coats of the eye and the potential role of the vascular structures producing and altering the appearance of the various types of detachments. C: Ocular ultrasound showing a retinal detachment (arrow) extending back to the optic nerve head (arrowhead). D: The same retinal detachment seen in (C), with the retina shown by the (arrow) and its attachment at the optic nerve head and ora serrata by the (arrowheads). E: Retinal detachment as seen at funduscopy. F: Ocular ultrasound of a choroidal detachment. The displaced choroidal membrane is shown by the (arrow), and its attachment lateral to the optic nerve head is shown by the (arrowheads). G: A choroidal detachment as seen at funduscopy to compare with the retinal detachment seen in (E). The margins of the displaced choroidal membrane are shown by the (arrows). Note how these terminate before reaching the optic nerve head (arrowhead). (Part A from Mancuso AM, Ojiri H, Quisling RG. Head and Neck Radiology: A Teaching File. Philadelphia: Lippincott Williams & Wilkins, 2002, with permission).
Leukocoria is a white reflex noted on funduscopic examination of the eye. It is a sign on physical examination that can be the result of intraocular tumors, detachments, and/or other inciting pathology (Fig. 45.2).
Intraocular hemorrhage as seen on CT and MRI is usually due to retinal vascular abnormality or a traumatic episode. It can, however, be confused with other conditions and may be the result of significant underlying pathology such as an intraocular mass that might be obscured by the hemorrhage.
APPLIED ANATOMY
The anatomic knowledge base for this discussion is a complete understanding of the intraocular anatomy and most specifically the attachments and relationships of the retina, choroids, and hyaloid membranes and the potential spaces lying between these structures and the vitreous body as well as their vascular relationships (Fig. 45.1). These features are discussed in detail in Chapter 44.
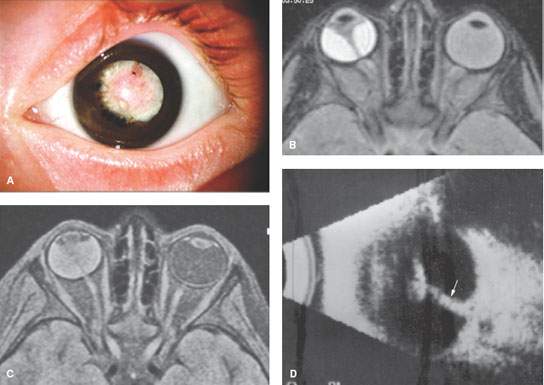
FIGURE 45.2. Images from patients with retinal detachment due to persistent hyperplastic primary vitreous. A: Clinical image of a patient with a leukocoria. B, C: Magnetic resonance imaging of a patient showing a retinal detachment with fat-suppressed images that reveal the altered appearance of fluid contents in the subretinal space depending on the pulse sequence used. D: Ocular ultrasound showing a thick band extending from the optic disc to the posterior capsule (arrow).
IMAGING APPROACH AND PROS AND CONS
Ultrasound, CT, and MRI have a role to play depending on clinical circumstances. The details of these techniques as applied to ocular pathology should be reviewed in Chapter 44, if necessary. Indication-specific protocols for CT and MRI are shown in Appendices A and B.
Ultrasound, usually performed by the ophthalmologist, may be the first and only imaging tool used to evaluate detachments (Fig. 45.1). CT and MRI are not normally obtained by the ophthalmologist to study detachments primarily unless some underlying causative pathology that requires imaging is suspected clinically. Because of this, detachments and related fluid collections are usually noted as an associated finding on CT and magnetic resonance (MR) studies.
Leukocoria as a presenting sign may be studied initially with either MRI or CT depending on the clinical suspicion of the responsible pathology (Fig. 45.2). MR images are more likely to suffer significant motion degradation and will not detect or exclude calcification with a high degree of confidence. MRI will normally be more informative with regard to the extent of the membrane detachment and more sensitive for detecting and perhaps better than CT at characterizing the underlying pathology. Sometimes, both studies are necessary.
SPECIFIC CONDITIONS
Leukocoria
Diseases presenting with leukocoria include retinoblastoma, a number of nonneoplastic diseases, and total retinal detachment. Imaging is performed primarily with the intent of distinguishing between tumor and nonneoplastic diseases. When tumor is evident, imaging contributes to determining the size and location of the lesion, which can be readily performed in the office by the ophthalmologist with ultrasound. The nonneoplastic conditions causing leukocoria include Coat disease (Fig. 45.3), persistent hyperplastic primary vitreous (PHPV) (Fig. 45.2), retinopathy of prematurity (ROP) (Fig. 45.4), Norrie disease, Warburg syndrome, and toxocara endophthalmitis. Each is described in detail in other chapters.
In most cases of leukocoria, MR and CT reveal morphologic features that distinguish the benign diseases from retinoblastoma and other tumors (Fig. 45.5). It is important to observe whether there is calcification, a mass, or spread beyond the eye and whether the size of the eye has been affected. Benign calcium deposition seldom occurs in those younger than 3 years of age, except in the context of phthisis bulbi, which is an end-stage ophthalmopathy associated with Coat disease, PHPV, trauma, or ROP. Norrie disease and Warburg syndrome exhibit bilateral ocular involvement and neurologic manifestations such as oculocerebral anomalies. ROP has a characteristic clinical history of premature birth and exposure to oxygen for immature lung disease and is almost always bilateral. Coat disease generally presents later than 18 months of age and usually has reduced globe size; subretinal effusion that will typically contain cholesterol crystals that result in dense echoes within the fluid; and no calcification until it becomes chronic, usually at well beyond 3 years of age. Retinoblastoma usually presents before 3 years of age; it typically does not reduce eye volume, but very rarely there is retinoblastoma and atrophic eye, and it may demonstrate nodular calcification. Additional distinguishing features are included in the following discussion.
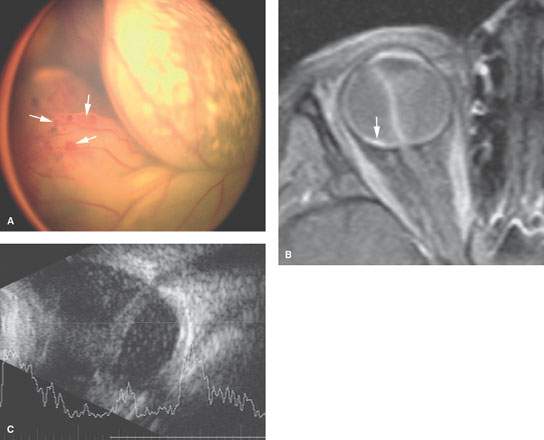
FIGURE 45.3. Retinal detachments related to Coat disease. A: Funduscopic view showing retinal detachment, with the (arrows) showing the areas of angiodysplasia related to that disease process. B: Contrast-enhanced T1-weighted fat-suppressed magnetic resonance showing complete retinal detachment. Areas of focal enhancement are present (arrow), which is consistent with the angiodysplasia that occurs in that disease. C: Ocular ultrasound shows a complete closed funnel retinal detachment with dense subretinal exudates.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree