FACIAL NERVE: INFECTIOUS AND NONINFECTIOUS INFLAMMATORY CONDITIONS
KEY POINTS
- The acute onset of an isolated peripheral facial nerve palsy does not require magnetic resonance imaging or computed tomography study unless there is reason to believe that there is an underlying infectious (other than viral) cause that must be treated with haste.
- Peripheral facial nerve palsy that presents with a different timetable, recurs, or does not recover requires very detailed magnetic resonance imaging and computed tomography studies of the facial nerve to hunt for a structural lesion that is very likely to be present in those atypicalsettings for Bell palsy.
- Atypical presentations of peripheral facial nerve palsy may be due to specifically treatable infectious and noninfectious inflammatory diseases.
- Imaging can be very helpful to triage patients with peripheral facial nerve palsy to the next best step in the diagnostic process.
The most common inflammatory condition of the facial nerve is viral neuritis. This condition will typically lead to the acute onset of peripheral facial nerve palsy, which is discussed in Chapter 127. This distinction is made because other inflammatory conditions include serious complications of infectious disease such as acute otomastoiditis or conditions that may require other specific therapies such as Wegener granulomatosis or Lyme disease. For the purposes of this chapter, these conditions are grouped into the two broad categories of infectious and noninfectious inflammatory diseases since the etiologies considerably vary while the imaging features vary little.
ANATOMIC AND DEVELOPMENTAL CONSIDERATIONS
Applied Anatomy
A diligent search of the entire course of the facial nerve is essential for evaluating imaging studies performed in patients with a peripheral facial nerve deficit believed to be due to an inflammatory condition. The presentation of these nonviral inflammations may mimic Bell palsy. Bell palsy is only a diagnosis of exclusion in a patient with a slow or stuttering onset or nonresolving peripheral facial nerve palsy; thus, it is important to establish whether imaging findings suggest an alternative diagnosis to such a likely acute or subacute viral infection (Fig. 129.1). This distinction relies heavily on excluding causative pathology, whether inflammatory or neoplastic, with a high degree of confidence.1,2
The computed tomography (CT) and magnetic resonance imaging (MRI) anatomy of the facial nerve must be completely understood, including its brain stem nucleus, course through the brain stem, its cisternal segment, its course through the internal auditory canal (IAC) and entire facial canal, and its entire course and distribution beyond the stylomastoid foramen. This anatomy is presented in detail in Figures 104.51–104.54, 175.8, 175.9, 175.15, and 175.16 and Chapters 104 and 175.
IMAGING APPROACH
Techniques and Relevant Aspects
CT and MRI in this anatomic region requires the highest possible spatial resolution. These issues for proper protocol development are discussed with general magnetic resonance (MR) and CT parameters in Chapters 1 through 3.
Specific protocols for CT and MR studies for investigating facial nerve problems in general appear in Appendixes A and B. The facial nerve is typically studied with dedicated contrast-enhanced studies of the temporal bone, especially when the patient is acutely symptomatic. These studies must also include the entire peripheral course of the facial nerve as well as the posterior fossa. In clinical settings atypical for Bell palsy (Chapter 127) or otherwise suggestive of a structural lesion, these studies may need to be repeated at clinically reasonable intervals.
Pros and Cons
MRI should be done first since it most confidently excludes causative pathology at all segments (i.e., the brain stem, cisternal, exit canal/foramen, and extracranial segments) of the nerve from its brain stem nucleus to the parotid gland (Figs. 129.2 and 129.3). MRI is more sensitive than CT for excluding intra-axial pathology such as demyelinating disease, pia-arachnoid diseases, and small neoplasms of the nerve that might involve the cisternal segment or the segment within the IAC as well as perineural spread of cancer.
CT may be done as a supplement to most confidently exclude similar pathology within the facial canal from the labyrinthine segment to the stylomastoid foramen and beyond the parotid gland distally (Fig. 129.1). This supplemental imaging may be done as a routine study or only when MRI findings are suspicious for a lesion other than inflammatory enhancement. More typically, supplemental CT is done when the onset of symptoms is atypical for Bell palsy and the cause is not established by MRI or the MRI is suspicious for a cause but not definitive.
If there is obvious potentially acute or subacute infectious disease involving the temporal bone, such as acute otomastoiditis or necrotizing otitis externa (NOE), a CT should be done initially.

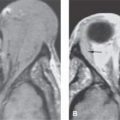
FIGURE 129.1. Chronic otitis media and cholesteatoma complicated with facial paralysis. Computed tomography showing erosive infectious middle ear and mastoid disease eroding the facial nerve canal at the anterior genu (A) and descending segment (black arrow in B) and of the sigmoid plate (white arrow in B).


FIGURE 129.2. Two patients with intra-axial causes of facial nerve paralysis. A–D: Patient 1, a 25-year-old woman with a single multiple sclerosis plaque. A: the T2-weighted image, (B) and non–contrast-enhanced and contrast-enhanced (C–D) T1-weighted (T1W) images show the enhancing lesion involving the right facial nerve root entry zone. E–G: Patient 2, presenting with bilateral peripheral facial nerve dysfunction and ocular dysmotility. All images are contrast enhanced and T1 weighted, showing focal enhancing brain stem lesions. In (E), the right facial nucleus and left facial nerve root entry zone are shown. In (F), the left facial nerve root entry zone is confirmed. In (G), the dorsal brain stem is shown. (NOTE: Lyme disease was the primary working differential in both cases, but multiple sclerosis was confirmed clinically and by cerebrospinal fluid analysis in Patient 1, and viral brain stem encephalitis was confirmed in Patient 2.

FIGURE 129.3. Meningeal disease causing multiple cranial nerve deficits—diffuse basilar meningeal enhancement as well as enhancement of sixth through eighth cranial nerve in a patient with tuberculous meningitis.
If a disease process such as NOE or skull base osteomyelitis is established as the cause of facial nerve deficit, then radionuclide studies may be used to monitor the response of the disease to specific antimicrobial therapy (Fig. 192.4). Radionuclide studies are nonspecific in these diseases and are not generally useful for initial diagnosis.
Controversies
Few treating physicians would suggest studying all patients with peripheral facial nerve palsy regardless of the pattern of onset of the facial weakness. For instance, most treating physicians will not image a patient with acute onset of peripheral facial nerve palsy because about 75% of these palsies will be transient and will begin to resolve within 4 to 6 weeks whether or not they are treated with steroids or antiviral medications.
If the onset is slow or “stuttering,” associated with spasticity, or associated with signs and/or symptoms of possible causative pathology such as otomastoiditis, the patient should be studied with meticulous high-resolution CT and/or MRI promptly at the time of initial evaluation. Nonresolving peripheral facial nerve palsy or one that recurs is virtually always studied with imaging.
SPECIFIC DISEASE/CONDITION
Infectious Conditions Other Than Viral (Herpetic) Neuritis
Etiology
Acute suppurative (pyogenic) bacterial infections of the middle ear and mastoid, including acute otitis media and acute otomastoiditis, can cause facial nerve dysfunction; this is a medical emergency. Chronic infections such as NOE (Chapter 114) are complicated by facial nerve dysfunction if not treated properly. Other chronic infections are more difficult to diagnose. As well, other organisms as diverse as blastomycosis, actinomycosis, and various fungi can involve the facial nerve when they cause skull base osteomyelitis. Lyme disease may result in unilateral or bilateral facial nerve dysfunction as a presenting complaint. Syphilis, schistosomiasis, and tuberculosis can cause facial nerve dysfunction, but this will commonly involve more than one cranial nerve and have other neurologic or systemic manifestations.
Prevalence and Epidemiology
These infections are all relatively uncommon causes of facial nerve dysfunction. Their prevalence in patients with underlying or causative disease will follow that of the population at risk for those diseases; for instance, younger children and young adults are at more risk for acute otomastoiditis, and the same is true for diabetics and for those with NOE. The risk of Lyme disease follows that of likely geographic exposure.
Clinical Presentation
The patient usually suffers the acute onset of a partial or complete peripheral (all of the muscles on one side of the face) facial nerve palsy. There may be other signs or symptoms of associated or causative pathology. In particular, there may be indications of otomastoid or extensive skull base disease or of central nervous system disease—for instance, those suggesting meningeal or brain stem involvement.
Bell palsy must never be confused with a facial nerve palsy of slow, progressive, or stuttering onset as is frequently the clinical course present in nonviral infections. Also, recurrent or persistent peripheral facial nerve palsy should not be considered a “Bell palsy” until it is proven not to be due to an inflammatory or neoplastic lesion of the facial nerve by a very carefully executed imaging evaluation.
Pathophysiology and Patterns of Disease
Infectious neuritis will cause the nerve to become inflamed and edematous. It may be that the offending infectious agent itself injures the nerve directly or the swelling caused by an infection produces varying degrees of axonal injury from the labyrinthine segment distally since the labyrinthine segment is the tightest part of the facial canal. This is the same theory that suggests if a facial nerve traumatized by blunt-force or penetrating injury is to be decompressed, it must be released through and including its labyrinthine segment. The presence of gross bony facial canal dehiscence is only sometimes associated with palsy, so other mechanisms of disease such as associated thrombophlebitis, a compression within an intact canal due to swelling, are involved.
The facial nerve that was inflamed and edematous in the early stages of disease will eventually become atrophic once the infection is resolved. The muscles of facial expression comprising most of the bulk of the superficial musculoaponeurotic system (SMAS) will go through the process of denervation atrophy. The muscles may enhance acutely and subacutely and then decrease in bulk and become fat replaced.
Manifestations and Findings
Computed Tomography and Magnetic Resonance
CT is usually normal if pathology is intrinsic to the nerve; if there is not underlying temporal bone pathology; or if the causative pathology involves the segment of the nerve in the IAC, cisternal segment, or brain stem. If performed, both CT and MRI must be used in a manner that excludes structural lesions affecting the facial nerve—infectious or not. If positive, both modalities will demonstrate structural pathology along the course of the nerve as diverse as otomastoiditis, focal erosion of the bone facial canal (Figs. 129.1, 129.4 and 129.5), and abnormal meningeal enhancement (Fig. 129.3).
MRI may be normal. However, it will usually be abnormal, showing some degree of enlargement and abnormal enhancement of the affected facial nerve or surrounding the course of nerve if the causative pathology involves the segment of the facial nerve in the IAC, cistern, or brain stem (Figs. 129.2 and 129.3)
The basic patterns of both inflammatory and other diseases are discussed in detail in representative chapters in Section II, and the patterns of other etiologies of facial deficits are described in Chapters 127 through 132.
Nuclear Medicine
If a disease process such as NOE or skull base osteomyelitis is established as the cause of facial nerve deficit, then radionuclide studies may be used to monitor the response of the disease to specific antimicrobial therapy. Radionuclide studies are nonspecific in these diseases and are not generally useful for the initial diagnosis.
Differential Diagnosis
From Clinical Data
The patient may suffer a partial or complete peripheral (all of the muscles on one side of the face) facial nerve palsy. If acute and there are no other signs or symptoms, this is likely a viral neuritis and can be properly referred to as a likely Bell palsy.
Bell palsy must never be confused with a peripheral facial nerve palsy of slow, progressive, or stuttering onset. If there are other signs of central nervous system disease, the potential differential diagnosis is relatively large, including demyelinating disease; Lyme disease; various causes of meningeal infection; and a variety of neoplastic conditions that might involve the nerve, meninges, and brain. Also, recurrent or persistent peripheral facial nerve palsy should never be considered a Bell palsy until it is proven not to be due to a structural lesion of the facial nerve. Conditions with these types of clinical characteristics atypicalfor Bell palsy will very often be the result of benign or malignant neoplasms and a handful of other causes that may occur anywhere along the nerve from its nucleus to its peripheral distribution.
Importantly, there may be clear clinical signs and symptoms that suggest a treatable and perhaps emergent clinical causation such as acute otomastoiditis, NOE, or other skull base osteomyelitis. Clinical settings that place the patient at risk for tuberculosis, syphilis, Lyme disease, or a monophasic demyelinating process such as acute disseminated encephalomyelitis are important historic factors, although an isolated facial nerve deficit is not commonly the presenting complaint of such diseases.

FIGURE 129.4. Complicated infectious disease. A diabetic with long-standing necrotizing external otitis on the left presenting with ipsilateral acute facial nerve paralysis. A: Computed tomography (CT) in a bone window setting showing opacification of the external auditory canal (EAC) and mastoid and erosion of the anterior wall of the EAC (arrow). Reactive sclerotic changes are seen in the petrous apex, clivus, and sphenoid. B: CT in a soft tissue window setting (B) and T1-weighted images before (C) and after (D) contrast showing extension of soft tissue changes to the stylomastoid fat pad where the facial nerve was involved.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree