Gastrointestinal Diseases
RADIOGRAPHIC ANATOMY OF THE GASTROINTESTINAL TRACT
Radiographic Anatomy of the Gastrointestinal Tract
A thorough understanding of the normal plain film appearance of the gastrointestinal (GI) tract is critical when evaluating for the presence of serious conditions that may affect this system. For example, swallowed air within the stomach has a different appearance than gas within the small bowel or colon. Table 30-1 reviews the plain film appearance of the GI tract.
TABLE 30-1
GASTROINTESTINAL TRACT PLAIN FILM ORGAN APPEARANCE
| Organ | Visibility | Location | Retroperitoneal Versus Intraperitoneal | Fixed Versus Mobile | Appearance Specifics | Plain Film Abnormalities |
| Esophagus | Air occasionally visible in the cervical region | Anterior and left of spine from laryngopharynx to diaphragm | Not applicable | Fixed | None on plain film | Abnormalities, including dilatation or neoplasm, may present as posterior mediastinal mass (hiatal hernia) |
| Stomach | Air in the fundus on upright with inferior fluid level; spreads to body of stomach and may outline rugae on supine image | Magenblase immediately inferior to left lung base on upright image; should not extend to midline or lateral body | Intraperitoneal | Fixed proximal and distal; mobile body | None on plain film | Displacement of magenblase laterally suggests hepatomegaly |
| Duodenum | Occasional air in bulb | Right upper quadrant medially | Retroperitoneal (most) | Fixed | None | None |
| Small bowel | Occasional air-filled small segment | Most of abdomen; jejunum primarily left upper quadrant and middle lower ileum | Intraperitoneal | Mobile | Small, thin mucosal folds | Long air-filled segments; dilated air filled (>3 cm) |
| Cecum | Fluid feces and gas bubbles mixed | Right lower quadrant (RLQ) | Intraperitoneal | Mobile, usually RLQ location | None | Distension (>10 cm risk of rupture); volvulus (“coffee bean” sign) |
| Appendix | May be visible gas in appendix | Considerable variation, although usually in RLQ | Intraperitoneal | Can move with the cecum | None | Normal or may show slight distension of adjacent ileum; possible appendicolith |
| Ascending and descending colon | Visible gas in haustra | Ascending along right flank; descending along left flank | Retroperitoneal | Fixed | Widely spaced, thick mucosal folds; lateral margin of both should be within 2 to 3 mm of adjacent flank stripe (fat plane medial to abdominal muscle wall); splenic flexure should be most superior portion of colon | Dilatation |
Cholelithiasis (Gallstones)
Background
The incidence of gallstones in patients in the United States approaches 20% of men and 35% of women by the age of 75 years;25 thus, gallstones exhibit a greater prevalence in women and in older age groups. Obesity and certain diseases also are associated with the development of gallstones (Table 30-2).
TABLE 30-2
ASSOCIATED FACTORS FOR GALLSTONE FORMATION
| Associated Factors | Comments |
| Obesity | Rapid weight loss resulting in increased risk of symptomatic gallstone formation18 |
| Increasing age | Associated with increased cholesterol secretion |
| Northern European ethnic group | Associated with increased cholesterol secretion |
| Estrogen replacement therapy and oral contraceptive use | Increases biliary output of cholesterol and also reduces synthesis of bile acid in women |
| Pregnancy | Associated with increased risk of gallstones and symptomatic gallbladder disease |
| Sickle-cell anemia or other hemolytic conditions | Hemolysis increases bilirubin excretion |
| Crohn disease | Disease of the terminal ileum causing disruption of bile acid reabsorption |
From Johnston DE, Kaplan MM: Pathogenesis and treatment of gallstones, N Engl J Med 328:412, 1993; Liddle RA, Goldstein RB, Saxton J: Gallstone formation during weight-reduction dieting, Arch Intern Med 149:1750, 1989; Tait N, Little JM: The treatment of gallstones, BMJ 311:99, 1995.
Imaging Findings
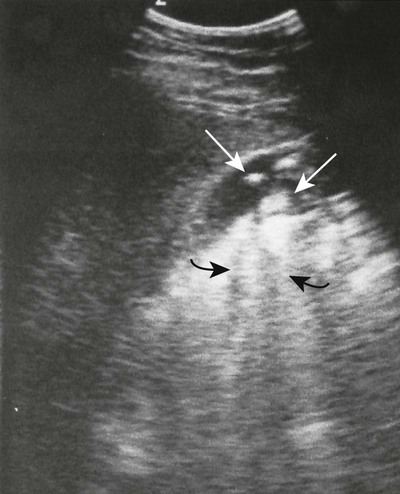
Ultrasonography generally is the preferred imaging modality for evaluating patients for possible gallstones or biliary duct obstruction. Current high-resolution, real-time ultrasonography can identify gallstones as small as 2 mm. This technique is rapid and noninvasive and does not involve ionizing radiation. Gallstones produce hyperechoic foci with acoustic shadowing, and mobility of the stone usually is apparent (Fig. 30-1).5,16 The patient should fast for 4 or more hours because these stones can be missed in a contracted gallbladder.26
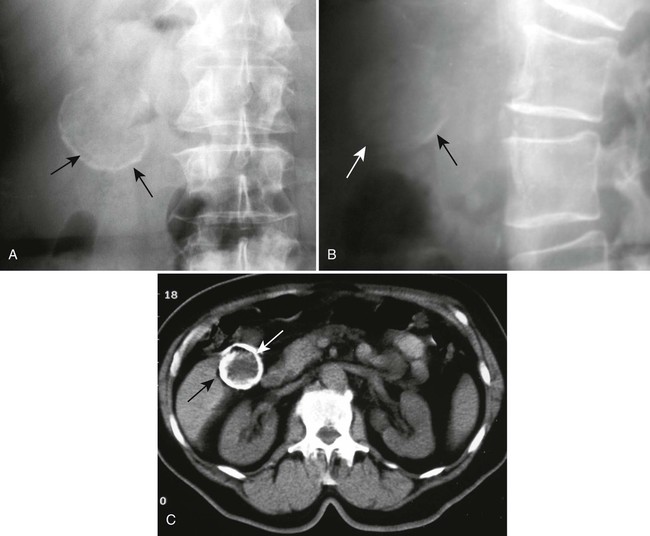
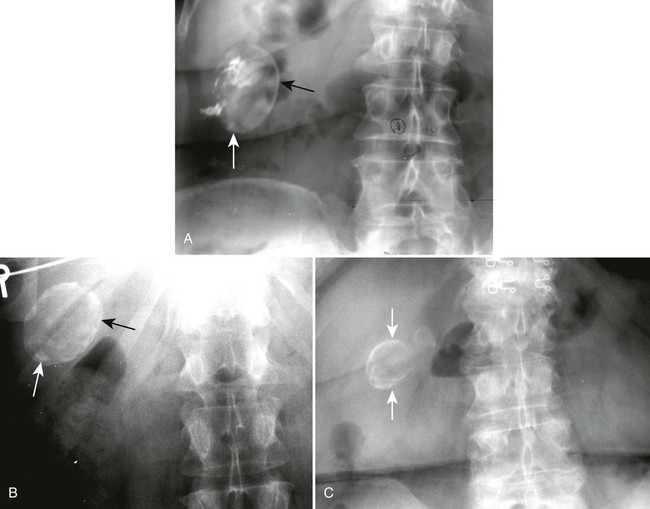
These stones may be imaged incidentally on plain film radiographs even in asymptomatic patients, but only 10% to 15% of them contain enough calcium to be visible (Figs. 30-2 through 30-4).12,32 Oral cholecystography (OCG) requires the patient to take an oral contrast agent, which is absorbed from the bowel, excreted by the liver, and concentrated in the gallbladder (except when the gallbladder cystic duct is blocked or sometimes when the gallbladder is inflamed). The gallbladder also is not seen in cases of a lack of absorption or significant liver damage.
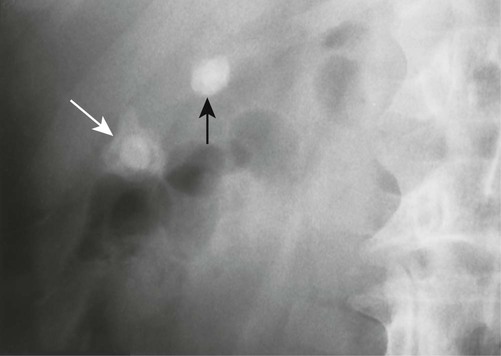
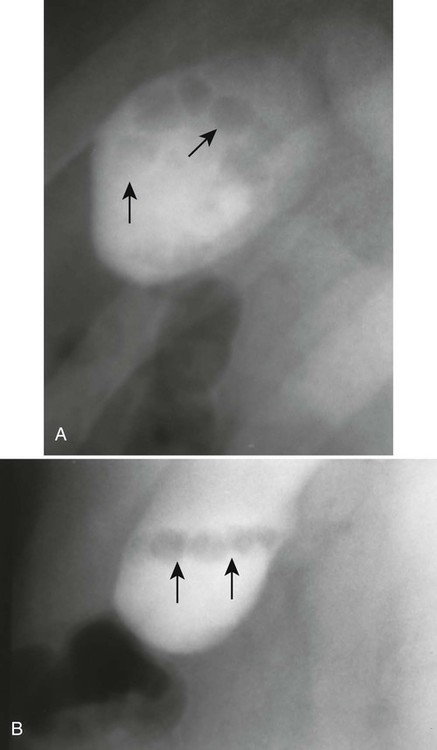
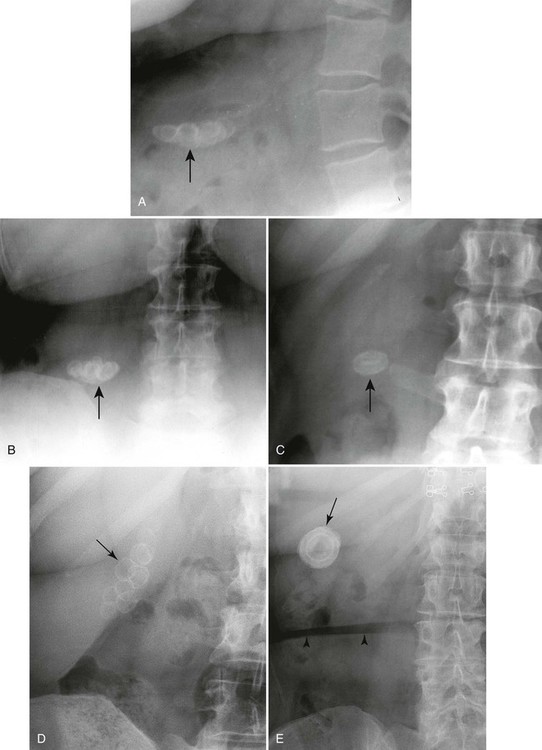
Oral cholecystography does demonstrate most gallstones, but since the development of ultrasonography to accomplish this task, it is most useful for providing information about the functional status of the gallbladder (see Fig. 30-3).7 However, the clinical utility of this is still controversial. Table 30-3 lists the imaging techniques and the limitations of each of these key modalities used in visualizing gallstones.
TABLE 30-3
LIMITATIONS OF IMAGING TECHNIQUES FOR VISUALIZING GALLBLADDER STONES
| Imaging Technique | Imaging Findings | Limitations |
| Plain film radiography | Single concretion or multiple calcific concretions; calcification may be central, homogeneous, or rim-like; when multiple, stones are often clustered together and faceted | The majority of nonopaque stones will not be visible. |
| Oral cholecystography | Single or multiple lucent-filling defects within opacified gallbladder; mobility of stones may be demonstrated by change in patient position | A number of conditions such as malabsorption, gastric outlet obstruction, inflammatory bowel disease, ileal disease, and liver disease may prevent opacification of the gallbladder. |
| Ultrasonography | Stones appear as intraluminal, echogenic, mobile foci that are gravity dependent and create an acoustic shadow | Small stones less than 2 mm in the presence of biliary sludge may prevent visualization; inadequate visualization may occur in obese patients. |
| Computed tomography (CT) | Single or multiple filling defects within gallbladder; stones may be densely calcified, rim calcified, or laminated; lucent filling defects within the bile may be seen with contrast-enhanced CT | Approximately 20% of gallstones are not identified on CT; CT is not considered a screening tool for uncomplicated cholelithiasis. |
| Magnetic resonance imaging (MRI) | Most gallstones have no signal on MRI and present as a signal void-filling defect within gallbladder. | Stones may be indistinguishable from polyps or tumors; MRI is not considered a screening tool for uncomplicated cholelithiasis. |
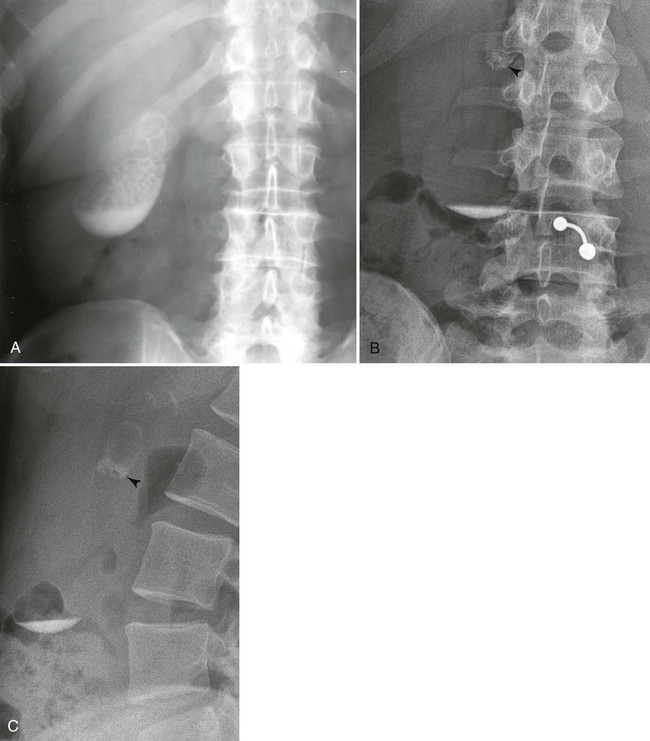
Uncommonly, a noncontrasted gallbladder forms a radiodense “milk of calcium” bile, known as limy bile syndrome, that mimics the gallbladder’s appearance during OCG (Fig. 30-5). This is thought to develop from chronic obstruction of the cystic duct by one or more gallstones in patients with chronic cholecystitis. The duct obstruction leads to decreased gland function, bile stasis, and radiographically visible accumulations of radiodense calcium carbonate in viscous intraluminal bile. Reviewing the patient’s history to exclude any recent intake of contrast material (oral or intravenous) must be accomplished before a diagnosis of limy bile syndrome can be made. On radiographs, the fluid is found in the gravity-dependent portion of the gallbladder. The ultrasound appearance is not consistent because the composition of the milk of calcium bile varies from a semisolid to fluid suspension.
“Porcelain gallbladder” describes extensive calcification of the wall of the gallbladder, also known as calcifying cholecystitis or cholecystopathic chronica calcarea (Figs. 30-6 and 30-7). Specifically, the term refers to the blue-greenish discoloration and brittle condition of the gallbladder observed during surgery. Patients generally are asymptomatic and are more commonly women (5 : 1 ratio). Concurrent gallstones are usual. A porcelain gallbladder is associated with higher incidence of adenocarcinoma of the gallbladder, typically warranting prophylactic excision. As with gallbladder stones and limy bile syndrome, a porcelain gallbladder is typically an incidental finding on plain film studies (Table 30-4).
TABLE 30-4
PLAIN FILM MANIFESTATIONS OF GALLBLADDER DISEASE
| Condition | Radiographic Findings | Comments |
| Stones | Single calcific concretion or multiple calcific concretions; calcification may be central, homogeneous, or rim-like; when multiple stones, they often are clustered together and usually faceted; on erect films, stones may be layered in the dependent portion of the gallbladder | 10% to 15% of stones are visible on plain radiographs |
| Limy bile syndrome (milk of calcium bile) | Radiopaque appearance of the gallbladder or bile ducts than may simulate contrast | Limy bile is caused by calcium carbonate precipitation in the bile; the main symptom are epigastralgia and right hypochondralgia |
| Porcelain gallbladder | Characteristic appearance is eggshell calcification in the right upper quadrant | Patients are generally asymptomatic |
Clinical Comments
Cholelithiasis usually is discovered incidentally during other studies. In the first 5 years after diagnosis, only approximately 10% of patients experience symptoms resulting from gallstones.32 Right upper quadrant pain is the most commonly reported symptom.32 The pain usually is steady, lasting for several hours. Radiation to the lower abdomen, back, or tip of the right scapula is common; vomiting may occur.5
Complications seen with gallstone disease include cholecystitis, choledocholithiasis, pancreatitis (migration of a stone to the distal common duct where the pancreatic duct enters), cholangitis, stone perforation of the duodenum or colon, and gallstone ileus (Table 30-5).2,3,5,20,32 Symptomatic gallbladder disease may require surgical intervention if nonsurgical techniques such as lithotripsy (using strong ultrasound waves to break up the stone) are ineffective, unsuitable, or unavailable.32
TABLE 30-5
COMPLICATIONS ASSOCIATED WITH GALLSTONES
| Complications | Comments |
| Acute cholecystitis | May remit temporarily but sometimes progresses to gangrene and perforation |
| Choledocholithiasis | Gallstones obstructing the common bile duct |
| Cholangitis | Infection of the bile ducts after obstruction possible |
| Acute pancreatitis | Probably secondary to transient obstruction of the main pancreatic duct |
| Gallstone ileus | Follows perforation of the duodenum or bowel by gallstone; classic plain film triad: small bowel obstruction, biliary tract air, and an opaque concretion in the small bowel |
From Johnston DE, Kaplan MM: Pathogenesis and treatment of gallstones, N Engl J Med 328:412, 1993.
Colon Polyps
Background
Colon polyps are found in up to 12% of the population.34 The adenomatous polyp is considered the precursor to colorectal cancer.17 Therefore, detection of colonic polyps is extremely important. Polyp size is a critical biomarker guiding clinical management. The incidence of malignancy increases with increased size of the polyp (Table 30-6). Most polyp development is incidental, but polyps may also appear as part of familial polyposis syndrome. Table 30-7 reviews the characteristics of several polyposis conditions.
TABLE 30-6
INCIDENCE OF MALIGNANCY IN RELATION TO POLYP SIZE
| 5 mm or less | 5 mm to 10 mm | 10 mm to 20 mm | More than 20 mm |
| <0.5% | 1%–2.5% | 10% | 46% |

From Thoeni RFL, Bischof TP: Colonic polyps. In Traveras JM, Ferrucci JT, editors: Radiology diagnosis-imaging-intervention, vol 4, Philadelphia, 1996, Lippincott-Raven.
TABLE 30-7
REVIEW OF POLYPOSIS CONDITIONS
| Complications | Comments |
| Nonfamilial adenomatous polyps | Present in 30% of adults older than 50 years of age; malignancy correlates with polyp size, villous features, and degree of dysplasia |
| Familial adenomatous polyposis | Autosomal dominant; it begins to appear between ages of 10 and 35 years; colon cancer usually occurs by age 50 years |
| Gardner syndrome | Variant of familial adenomatous polyposis; it is characterized by extraintestinal osteomas, fibromas, and desmoid tumors |
| Familial juvenile polyposis | Autosomal dominant; most common—colon |
| Peutz-Jeghers syndrome | Autosomal dominant; mucocutaneous pigmented macules appear on the lips, buccal mucosa, and skin; 50% of patients develop malignancies in gastrointestinal and nonintestinal organs |
| Turcot syndrome | Autosomal recessive; central nervous system neoplasm |
Imaging Findings
Conventional (optical) colonoscopy and barium examination are the most important methods for detecting polyps.33 CT colonography is a newer, minimally invasive method for examination the colon for colorectal polyps; however, it is not widely accepted beyond the current indications of incomplete optical colonoscopy or patients unsafe for optical colonoscopy.
Polyps appear as discrete masses, sessile or pedunculated, which protrude into the lumen of the gut (Figs. 30-8 to 30-10
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree