Gastrointestinal Procedures
OBJECTIVES
After studying this chapter, the student will be able to:
1. Explain the radiographer’s teaching responsibilities before, during, and after imaging examinations of the gastrointestinal system.
2. Explain the correct order of scheduling radiographic imaging examinations if multiple examinations are ordered.
3. Differentiate between positive and negative contrast agents.
4. List the potential adverse effects of positive and negative contrast agents when they are used in imaging examinations of the gastrointestinal system.
5. Explain the precautions the radiographer must take during administration of a barium enema in an adult and pediatric patient.
6. Describe the patient care considerations for a patient with an ostomy who is having a barium enema.
7. Demonstrate the correct method of administering a barium enema.
KEY TERMS
Adverse effects: The development of undesired side effects or toxicity caused by the administration of drugs
Alimentary canal: The organs of digestion; the digestive tract
Colostomy: An artificial opening (stoma) created in the large intestine and brought to the surface of the abdomen for the purpose of evacuating the bowels
Diverticulitis: Inflammation of a sac or pouch protruding from the walls of the intestines, especially the colon
Flatus: Gas expelled from the digestive tract through the anus
Ileostomy: An artificial opening (stoma) erected in the small intestine (ileum) and brought to the surface for the purpose of evacuating feces
Nasogastric tube: A thin tube that is inserted through the nose and into the stomach for the purpose of instilling substances or for the removal of substances
Ostomy: General term for an operation in which an artificial opening is formed
Peritonitis: Inflammation of the serous membrane lining the abdominal cavity and surrounding the abdominal organs
Stoma: An opening in the body created by bringing a loop of bowel to the skin surface
Radiographic imaging procedures of the upper and lower gastrointestinal (GI) systems were once done in relatively large numbers. The use of computed tomography (CT) has largely replaced these studies, making the use of fluoroscopy to visualize the stomach, small bowel, and large bowel unnecessary. Although the studies are no longer routine, they may still be done on occasion. Therefore, the radiographer must understand the examination itself and the patients’ reactions to them. They can be stressful and uncomfortable examinations that may place the patient under physical and emotional stress. This is particularly true for the very young and the very old patient.
Contrast studies that include the use of high-density barium and air are effective methods of detecting conditions of the upper and lower GI systems. When imaging of the GI tract using barium is contraindicated, an iodinated contrast agent may be prescribed. Imaging of the liver, gallbladder, and biliary tree (all ancillary parts of the digestive tract) are now performed with ultrasound or nuclear medicine. These special methods of imaging are discussed in Chapter 18.
When working with contrast media, the radiographer must know the indications and contraindications for their use, the potential adverse reactions of each, safe method of patient care, and the patient teaching that must accompany their use. Most patients have had no experience with these procedures and the preparation that is required. The radiographer is responsible for educating the patient in these areas. There may be hesitation, and perhaps even revulsion, with the technical aspects of enema administration. Dietary restrictions and medication prescribed before these procedures are not unusual. A matter-of-fact, professional manner when instructing the patient will alleviate patient anxiety.
TYPES OF CONTRAST MEDIA
There are two types of radiographic contrast media: negative and positive. Negative contrast agents decrease organ density to produce contrast. The most commonly used negative agents are carbon dioxide and air. Positive contrast media are used to increase organ density and improve radiographic visualization. Positive contrast media are barium sulfate and iodinated preparations. Contrast media are discussed fully in Chapter 15. Discussions here pertain mainly to its use in the GI system.
Negative Contrasts
Carbon dioxide and air are the most frequently used negative contrast media. They may be used singly or in combination with a positive contrast medium for studies of the GI system. Complications associated with the use of negative contrast media can result from inadvertent injection of air into the bloodstream, producing an air embolus. Although the injection of negative contrast media into the bloodstream during GI procedures is unlikely, it is important to remember the complications associated with this.
Positive Contrasts
Positive contrast media create a density difference by attenuating and absorbing the ionizing radiographic beam. This reduces or stops the x-ray beam from hitting the image receptor, thereby creating a white or opaque area on the image. There are two types of positive contrast media: barium and iodinated contrast. While barium is relatively nontoxic, iodinated contrasts present a greater danger to the patient. The choice of which positive contrast medium to use is generally the decision of the radiologist; however, the radiographer must be familiar with all types of positive contrasts and their use.
Barium Sulfate
Barium sulfate is the most frequently chosen contrast medium for radiologic examination of the GI tract. It is a white (or pink), crystalline powder that is mixed with water to make a suspension. It may be administered by mouth for examination of the upper GI tract, by rectum for examination of the lower GI tract, or by infusion of a thin suspension through a duodenal tube to visualize the jejunum and ileum. The use of high-contrast barium solution in the alimentary canal reveals organ outlines and demonstrates pathologic conditions of the visceral walls. By using double contrast of barium and air, the ability to detect small lesions is improved.
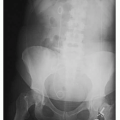
The toxic effects of barium are negligible if the suspension remains within the GI tract; however, if there is a break in the gastric mucosa caused by injury or disease, the barium sulfate may pass into the respiratory tract, the peritoneal cavity, or the bloodstream and cause adverse effects. Barium has been known to get into the bronchial tubes if there is a fistula from the esophagus to the trachea or if the barium is aspirated. Patients who are more prone to aspirating barium during a barium swallow study are the elderly and those with swallowing difficulties. Barium in the bronchi is dangerous from the standpoint that it will reduce the amount of air that will be taken into the alveoli. Barium will be retained in the lungs for a lengthy period and will interfere with subsequent chest radiographs (Fig. 12-1). Aspiration of oral or gastric contents into the tracheobronchial tree of older patients may represent a life-threatening situation. Although barium is not inherently toxic to lung tissue, patients will later exhibit a productive cough, fever, and elevated white blood cell as the body tries to rid the lungs of the foreign substance. Aspiration pneumonia is also a complication when barium sits in the bronchial tree.
If barium leaks into the peritoneal cavity, peritonitis may result. This possibility increases if the barium is mixed with fecal material. Fibrosis or formation of a barium granuloma may be a further complication. The possibility of leakage of the barium into the venous circulation through a perforation in the gastric mucosa as a result of trauma or disease must also be considered. This would produce an embolus that might be fatal. When perforation of the GI tract is suspected, an absorbable water-soluble iodinated contrast medium is used in place of barium.
Barium sulfate is often constipating. If the patient is not properly instructed following a procedure that involves its use, there may be a tendency to ignore the condition rather than have it treated, and fecal impaction or a bowel obstruction may result.
If the patient reports that a previous administration of oral barium suspension produced a sensation of nausea, the radiologist should be notified before it is administered again, because if the patient vomits, aspiration of barium may result. Although barium itself is rarely a cause for nausea, the patient may be convinced that it is the barium that is causing the nausea.
SCHEDULING DIAGNOSTIC IMAGING EXAMINATIONS
Patients often present for medical treatment with vague symptomatology that requires multiple imaging and direct-view examinations before an accurate diagnosis can be made. During the medical diagnostic process, one patient may have a series of examinations, some of which are performed in the radiographic imaging department and some elsewhere.
If the radiographer is responsible for scheduling radiographic imaging examinations, inquiries regarding other examinations that the patient may be expected to undergo must be made. Critical thinking and thoughtful planning are required to facilitate the patient’s speedy diagnosis.
1. Procedures that require fasting must be done in the morning. This is especially important when scheduling diabetic, elderly, or pediatric patients.
2. All examinations or procedures that do not require contrast media should be scheduled first.
3. Ultrasonography and nuclear medicine procedures must be scheduled prior to contrast studies, so that the contrast will not interfere with these examinations.
4. Iodinated contrast studies must be performed prior to barium studies because barium is denser and will obscure the iodinated contrast.
5. When a patient is scheduled for both the upper and lower GI systems with barium, the lower GI series should be scheduled first because barium clears quickly from the lower bowel, whereas if the upper GI study is done first, the barium will take days, perhaps several weeks for the barium to filter through lower system and be expelled. Retained barium in the lower GI study will inhibit visualization of that area.
PATIENT PREPARATION FOR STUDIES OF THE LOWER GI TRACT
Correct preparation of the patient for barium studies of the lower GI tract is essential and may seem relatively complex to the patient. This preparation varies across health care facilities and with each patient’s special needs. The radiographer’s responsibility is to learn the specific procedure where employed. If the patient is an outpatient, the radiographer may be responsible for giving the patient the appointment for the examination and the instructions for its preparation. The following directions generally apply at most institutions, with modifications for particular patients.
Pediatric and infant patient preparation is much less complex than for the adult patient. From the age of newborn to 2 years, usually no preparation is necessary. Up to the age of 10 years, the child should be on a low-residue meal the evening before.
If the appointment is made far enough in advance, the adult patient is instructed to eat foods low in residue for 2 to 3 days prior to the procedure. A low-residue diet
excludes tough meats; raw, cooked, and dried fruits; raw vegetables; juices containing the pulp of fruits or vegetables; whole-grain breads and cereals, especially bran and cracked wheat types; nuts, peanut butter, and coconut; olives, pickles, seeds, and popcorn; and dried peas and beans. The patient should drink no more than two cups of milk each day and avoid strong cheeses. The patient should be encouraged to increase fluid intake (water) for 2 to 3 days before the examination to assist in clearing the lower bowel of waste.
excludes tough meats; raw, cooked, and dried fruits; raw vegetables; juices containing the pulp of fruits or vegetables; whole-grain breads and cereals, especially bran and cracked wheat types; nuts, peanut butter, and coconut; olives, pickles, seeds, and popcorn; and dried peas and beans. The patient should drink no more than two cups of milk each day and avoid strong cheeses. The patient should be encouraged to increase fluid intake (water) for 2 to 3 days before the examination to assist in clearing the lower bowel of waste.
Twenty-four hours before the examination, a clear liquid diet is usually prescribed for all three meals. A clear liquid diet may include coffee or tea with sugar but no milk, clear gelatin, clear broth, and carbonated beverages. The patient should be instructed to drink five 8-oz (236.6 mL) glasses of water or clear liquids during these 24 hours. This will help not only flush out the lower digestive tract but also prevent dehydration.
The afternoon preceding the examination, 10 oz (295.7 mL) of magnesium citrate or its equivalent is prescribed. The evening before the examination, another laxative or cathartic such as magnesium citrate may be ordered. The morning of the examination, a rectal suppository or cleansing enema may also be necessary. Laxatives must never be given to a patient without the physician’s order. They can be harmful to persons with bowel obstructions and other pathologic conditions of the GI tract.
 Cultural Considerations
Cultural ConsiderationsCultural beliefs may have a strong influence on the performance of any diagnostic procedure of the lower bowel. The radiographer’s attention and understanding of these beliefs will go a long way in the cooperation and acceptance of the examination and the procedure necessary to perform it.
Family honor is one of the most important values in the Arab world. Tied to family honor is purity of the female. To do an enema on an Arab female may create a situation where the husband will not allow his wife or daughter to undergo the procedure or even have the preparation despite the benefit it might provide, such as diagnosing colon cancer.
Hispanic males are usually the decision makers in the family. The younger family members may not agree to have any type of procedure done without the consent of the patriarch of the family. However, the subgroups of the Hispanic population with their separate customs and beliefs may render widely held understanding of their culture incorrect. Asking the patient how best to proceed when the radiographer is not certain, is the best method to avoid misunderstandings and the possible refusal of the patient to do the study.
Shame may prevent those of Chinese cultures to refuse the traditional barium enema (BE). Russian immigrants may view medical care in the Unites States with distrust. African Americans and Native Indians may be more readily accepting of these procedures, but the radiographer must always be aware the patient’s body language and subtle spoken keys to the acceptance of the procedure. It is always better to ask before proceeding than it is to try to recover a patient’s trust and understanding in the middle of a procedure that is not acceptable within the culture of that patient.
There are religious beliefs that the body should always be covered with a type of undergarment. This must be taken into consideration during the performance of a BE. Talk to the patient to gain an understanding of how to best proceed.
Patients with insulin- and noninsulin-dependent diabetes mellitus require special pre-examination orders and instruction. Patients with heart disease and renal disorders may also need alternative preparations. The radiographer must ascertain the patient’s medical status before giving instruction in preparation for any GI series. Patients with diabetes mellitus must also be instructed concerning administration of morning insulin or other antidiabetic medications. Usually, these medications are postponed until the examination is complete and the patient is able to eat.
Cleansing enemas are generally prescribed the night before or early in the morning of the examination. Because there are several types and variations of cleansing enemas, the radiographer must become familiar with all of them and must be able to administer one of them, if necessary, in the imaging department. Occasionally, a patient comes to the radiographic imaging department poorly prepared for a radiographic study of the lower bowel, and the radiographer has to complete the preparation in the department by administering an additional cleansing enema. By learning the procedure, the radiographer is able to give clear, concise directions to the patient who needs instruction.
Cleansing Enemas
The type of cleansing enema to be used is always ordered by the physician. The most frequently used cleansing enemas include the saline enema, hypertonic enema, oil-retention enema, tap water enema, and the soapsuds enema.
Cleansing enemas can influence fluid and electrolyte balance in the body to varying degrees because they each
have a different degree of osmolarity, which influences the movement of fluids between the colon and the interstitial spaces beyond the intestinal wall. This means that, in the presence of some cleansing solutions that are instilled into the lower bowel, the bowel extracts fluid from the surrounding interstitial spaces. This happens because the higher osmolarity of the cleansing solution (hyperosmolar) induces the fluid to move across the semipermeable membranes of the intestinal wall. The body fluid that has moved into the large intestine is then excreted from the body along with the enema solution. Dehydration occurs if an excess of body fluid is excreted. This situation can be reversed.
have a different degree of osmolarity, which influences the movement of fluids between the colon and the interstitial spaces beyond the intestinal wall. This means that, in the presence of some cleansing solutions that are instilled into the lower bowel, the bowel extracts fluid from the surrounding interstitial spaces. This happens because the higher osmolarity of the cleansing solution (hyperosmolar) induces the fluid to move across the semipermeable membranes of the intestinal wall. The body fluid that has moved into the large intestine is then excreted from the body along with the enema solution. Dehydration occurs if an excess of body fluid is excreted. This situation can be reversed.
Another situation occurs when an excess of fluid with low osmolarity (hypo-osmolar) may be instilled into the lower bowel and absorbed into the interstitial spaces surrounding the colon, thus creating fluid excess in the body. This is called fluid toxicity. These potential hazards must be considered when the physician orders a particular solution for use as a cleansing enema.
Hyperosmolar fluids can create dehydration. Hypo-osmolar fluids can create fluid toxicity.
Saline Enemas
There are two types of saline enemas: normal saline and hypertonic saline. Normal saline is the safest solution to use for a cleansing enema because it has the same osmolarity as that in the interstitial spaces that surround the colon; therefore, it will not change the fluid balance in the body. It is the only safe fluid to use for cleansing enemas for infants and children because they can tolerate very little change in fluid and electrolyte balance. This solution is also used for elderly patients for the same reason.
Hypertonic saline solution can be administered quickly and easily and is effective for relieving constipation or eliminating barium sulfate residue after a barium study. Hypertonic solutions pull fluid from the interstitial spaces around the sigmoid colon and fill the bowel with fluid, thereby initiating peristalsis. Only a small amount of solution is required to do this (120 to 180 mL). Hypertonic saline enemas are often available under the name Fleet enema. Hypertonic enemas should not be administered to dehydrated patients or to infants and children.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree