Fig. 3.1
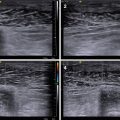
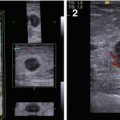
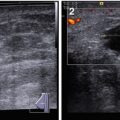
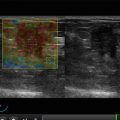
(1, 2) Breast US in a man
According to the standard procedure recommended for women, in describing the location of pathological process in men, the breast is conventionally divided into four quadrants: upper (superior)–outer (lateral), upper (superior)–inner (medial), lower (inferior)–inner (medial), and lower (inferior)–outer (lateral). The subareolar area (central portion) and the nipple are described separately. The terminology of “clock positions” is appropriate as an additional subsite descriptor to indicate the exact location of an abnormality (Fig. 3.2).
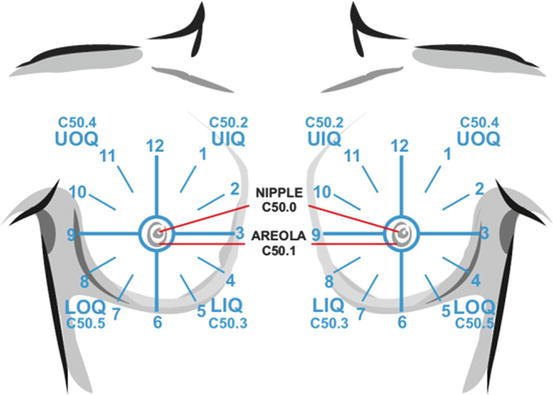

Fig. 3.2
Clock positions and quadrants of breasts
The examination generally begins with the intact/healthy breast, or with either the right or left breast in cases of no complaints. The US specialist should understand that the breast region in men is not limited to the area of the nipple, areola, and retroareolar space. A roundish region approximately 7–10 cm in diameter should be scanned from periphery to the nipple, analogous to the female breast.
The direction of scanning does not matter. Breast US often begins with the upper–outer quadrant of the right breast and follows clockwise with the probe movements in a radial direction from the periphery to the nipple area along the course of lactiferous ducts. The examination of the left breast often starts with the upper–inner quadrant and proceeding clockwise. For a more detailed examination, the scans are repeated in a clockwise circular direction from the periphery to the nipple area. Special attention is paid to the subareolar and nipple areas, because the acoustic shadow from the nipple can hide various pathological processes.
If an area suspicious for pathological process is detected within the breast, other US options should be applied. They may be time-consuming and may require additional software. Moderate compression with the probe is applied to assess the mobility of the lesion against the surrounding tissues and its density (deformation) and to decrease US artifacts resulting from connective tissue elements (e.g., lateral acoustic shadows). It is necessary to assess the status of regional lymph nodes (axillary, supraclavicular, subclavial, and parasternal) during breast US.
The absence of clinical signs and masses in the breast and axillary areas, accompanied by normal oncomarkers, requires no further US follow-up. In cases of doubt, the doctor can recommend repeated US in a specific period of time to analyze changes in the pathological process or differentiate it from physiological features (typically, one to two times a year; rarely, two to four times a year).
3.2 Healthy Male Breast with Ultrasound Examination and Reporting
The US image of a healthy male breast, unlike in women, is usually constant and often does not depend on the age and cyclic physiological features of the patient. A variability in US images is quite small and can be caused by the patient’s constitutional features (the development of subcutaneous fat) or could also depend on the class of US scanner or the US regimens and options.
US typically shows the status of the following male breast structures (Fig. 3.3):
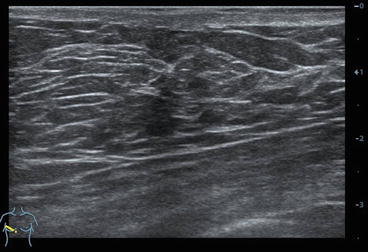

Fig. 3.3
Normal ultrasound anatomy of the breast
Subcutaneous adipose layer
Superficial leaf of the fascia
Presence and degree of development of the lactiferous ducts (if any are imaged)
Back leaf of the fascia
Retromammary space
Regional lymph nodes
Whether the breast skin is assessed depends on the frequency of the US probe and the class of the US scanner. Healthy skin is imaged as a homogeneous echogenic layer of 0.5- to 7-mm thickness. Before puberty, the thickness of the skin usually ranges from 0.5 to 2 mm. It reaches 2–4 mm after puberty (Zabolotskaya and Zabolotsky 2010). Inflammatory process, condition after radiation therapy, and postoperative edema are accompanied with thickening and a rough echostructure of the skin. The echodensity typically decreases. Irregular anechoic fluid collections may be observed in some cases. The margin between the skin and subcutaneous fat is not always possible to differentiate with a 5–7.5-MHz probe.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree