Abstract
Now more than ever, the requisite skills and responsibilities of radiologists extend well beyond their foundation of interpretive skills. Importantly, the field of radiology has made progress in quality and effectiveness over the past 2 decades. Validated standards have been established to help unify disparate practices. The science of quality improvement, honed in private industry, has been increasingly applied to medicine, and more specifically radiology, with encouraging results. Multiple initiatives, including increased implementation of dose-reduction technologies, have improved patient safety. Adoption of picture archiving and communication systems and structured reporting has increased the efficiency and availability of patient data within an increasingly interconnected healthcare landscape. Continued improvement in all of these areas is both necessary and expected.
The recent passage of the Patient Protection and Affordable Care Act has accelerated the movement toward evidence-based quality care while aiming to place the patient at the center of healthcare delivery. It has also begun to drive the development of new quality-based payment systems, within which radiology will need to define its role. As we look to the future, patient-centered and outcomes-based research will be an active and important area of healthcare quality improvement, and today’s radiologists would be wise to be active participants in this movement. Adherence to these themes can ensure that the next generation of radiologists are accessible, marketable, and indispensable to a dynamic and increasingly complex healthcare system.
Keywords
Ethics, History, Outcomes, Patient-Centered, Professionalism, Quality, Safety
To Err is Human
When the Institute of Medicine (IOM, now the Academy of Medicine) first released its report, To Err Is Human , in 1999, headlines were made throughout the world. The notion that our healthcare delivery system was not only not achieving the positive exceptionalism that one might expect from the most expensive system in the world, but also guilty of contributing to the demise of nearly 100,000 people each year, was more than unsettling. The report was widely credited for blowing the whistle on an immense problem with our healthcare system. Many knew of these errors few had an idea of the scope, but all wanted to reduce them. Improvement would never come about if the collective knowledge of medical errors was sequestered to the confines of morbidity and mortality talks, hospital board rooms, and isolated court cases. The report better defined the magnitude of the issue and ultimately helped to bring about a change in attitude; this was a monumental problem, and a difficult one, that required candid discussion, accurate quantification, effective collaboration, and measureable solutions.
After the whistle was blown, 2 years later the IOM released a second report, Crossing the Quality Chasm . With this, the IOM threw down the gauntlet, challenging the leadership of US healthcare delivery to make good on its promises. The report issued six aims for improvement:
- 1.
Healthcare must be safe.
- 2.
Healthcare must be effective.
- 3.
Healthcare must be patient centered.
- 4.
Healthcare must be timely.
- 5.
Healthcare must be efficient.
- 6.
Healthcare must be equitable.
Realizing the magnitude of the systemic dysfunction and the enormity of the task that healthcare faced, the IOM rightfully made no attempt to specify a plan for improvement. Rather, they set forth 10 rules for redesign, looking to establish a framework within which individuals and entities would be free to innovate their own solutions. Although all 10 of these rules are important, we feel there are a few that should be stressed as paramount principles considered when undertaking quality improvement initiatives:
- •
It must be patient centered.
- •
Free exchange of patient information and knowledge (including errors) is a necessity.
- •
Safety should focus on systems rather than individuals.
- •
Transparency must exist for patients (and clinicians).
- •
Waste should be continually decreased.
Together, the IOM reports successfully kick-started a culture of patient safety. It is a culture that has begun to permeate the halls of all healthcare institutions, public and private, as the field seeks to achieve these aims. Quality improvement initiatives have been undertaken and published with increasing frequency. To Err Is Human has served as the de facto benchmark against which progress can be measured. How is the healthcare sector doing? Results are mixed to say the least. There are published accounts of meaningful progress but often at a brutally slow pace. Some suggest that problems are worsening. Others, such as the Consumers Union Safe Patient Project 10-year review of the industry response to the IOM reports are not shy in giving the healthcare response a failing grade.
How can this be? Although some problems appear to be worsening, it is logical to conclude that some of this can be attributed to better recognition, measurement, and reporting of the issues at hand, something that should be taken as a positive and worthy step on the road to better healthcare. The number of and use of incident report systems have grown, in large part secondary to the Joint Commission requiring their use by hospitals. Despite this, (1) accurate and well-defined measurement, (2) standardization of data, and (3) proper implementation of this data-driven improvement continue to be an issue for a multitude of reasons. These include underreporting, lack of accepted standards, fragmentation of systems, and the inherent variability among different patient populations and care settings. There is increasing need to identify data that actually affect patient outcomes, and, of course, balance quality data with the cost and time required to collect it. In the continued efforts for improvement, healthcare has begun to embrace the practice of high-reliability organizations (HROs), learning from multiple other industries. The application of this concept to healthcare has been summarized based on three main tenets: (1) strong and committed leadership at all levels, (2) an institution-wide culture of safety, and (3) a methodical identification of root problems allowing for robust process improvement.
Better quantification of errors and their prevention in the delivery of care are only part of the problem. Some patients are directly or indirectly harmed before any attempt at treatment is even made. The need for improvements in patient diagnosis, of particular interest to the field of radiology, was recently examined in a 2015 IOM publication, Improving Diagnosis in Health Care . It is currently estimated that on a yearly basis, 5% of adults seeking outpatient care are improperly diagnosed. This harms the patient and adds cost to the system in the form of wasted resources. Much like To Err Is Human , perhaps this will serve as another much-needed benchmark for improvement.
Radiology’s Preemptive Work in Quality Improvement
To Err Is Human was a major wakeup call to medicine. It was a necessary call to attention to the fact that physicians and other care providers, no matter how skilled or competent, do not operate in a bubble. Despite their best intentions, care providers were still at risk of causing substantial harm, even if it was mainly secondary to systemic problems. Healthcare workers needed to be aware of the care settings, systems, and governing policies that were a part of their daily clinical duties and how each of these impacts the quality of care they were delivering. As such, many of the principles written about in To Err Is Human and Crossing the Quality Chasm could and would parallel the extradiagnostic aspects of radiology that are important today. That being said, the field of radiology was not oblivious to the issues at hand in 1999.
Just prior to the publication of To Err Is Human , through the leadership of Philip Alderson, noninterpretive skills for radiologists—in particular residents—was getting attention. He rightfully questioned the growing gap between a radiologist’s adequate interpretation skills and a lack of understanding of one’s place within the general healthcare delivery system. This was recognized in 1997 by the Association of Program Directors in Radiology (APDR), which later collaborated with the American College of Radiology (ACR) to produce a curriculum of noninterpretive skills that was further publicized by the American Journal of Radiology (AJR).
Much of this series focused on aspects of radiology care delivery that correlated with the IOM’s call for a more effective and patient-centered approach to healthcare. In particular, there was an in-depth look at the ACR’s efforts to create practice standards, accreditation of subspecialty programs, and the appropriateness criteria for imaging that had already been instituted. These published standards provided radiologists and other care providers with practice guidelines that, if followed, would increase the quality of care provided by radiologists. Accreditation programs, the first being the program in radiation oncology in 1966, ensured that techniques or practices underwent an evidence-based formal review process to ensure that specific quality standards were met. The widely recognized success of the mammography accreditation program, established in 1985 in response to disparities in mammography quality, led to measurable improvements in the quality of mammography throughout the United States and was eventually adopted by the US Food and Drug Administration (FDA). The ACR Appropriateness Criteria, introduced in 1993 and continually refined, defined evidence-based best use standards for selection of imaging exams or therapeutic processes for specific clinical conditions. This not only allowed radiologists and medical clinicians to deliver the most appropriate and effective care to each patient, but also preempted yet-to-be implemented future developments in healthcare that would require valid justification for and evidence supporting tests ordered prior to payment.
Around the same time that the IOM was releasing these pivotal reports, the American Board of Radiology (ABR) also recognized the importance of noninterpretive skills in the education and competence of our workforce. Today, the Diagnostic Radiology Boards include examination in noninterpretive skills, as does the Maintenance of Certification (MOC) Program. Recently, the number of ways to fulfill this requirement has greatly expanded, giving radiologists more flexibility and allowing for more creativity in fulfilling the required competencies in practice quality improvements. The ABR has maintained a syllabus, the Noninterpretive Skills Domain Specification and Resource Guide, which is available online and continually updated. The syllabus directly addresses the IOM aims for quality care and embraces the 10 guidelines for healthcare redesign. It provides valuable information for today’s radiologist and serves as a framework within which to examine efforts made by the field over the past 2 decades in addressing the IOM aims. The syllabus is divided into six sections, each of which receives a brief overview in the following pages and helps introduce some of the concepts that will be evaluated in this text. Despite the value and wealth of information provided by the syllabus, it is by no means a comprehensive work; it is the intention of this book to fill in the gaps and further develop these important aspects of radiology.
Part I: General Quality Improvement
The complexity of healthcare demands a continuous effort of all involved parties to achieve meaningful quality improvement . The unremitting nature of improvement can be contrasted with the more traditional, and much more static notion of quality assurance, in which the goal is merely compliance with predefined standards. There are multiple approaches to quality improvement. One of the most recognized is the Plan-Do-Study-Act (PDSA) cycle, which by its very name implies continuous improvement efforts. It embraces the isolation of and quantification of a specific problem, targeted interventions, and measurable outcomes. “Lean” process improvement focuses on elimination of waste and an institution-wide culture of mutual trust and continual improvement. Failure mode and effect analysis can be used to proactively assess complex processes for possible errors. Innumerable other methodologies exist and can be used to complement one another. Specific quality improvement tools that can be applied to any of these methods include establishing key performance indicators, value stream maps, cause-and-effect diagrams, time series plots, Pareto charts, prioritization matrices, and simulation walk-throughs.
Regardless of the methods and tools used, there are key components in all successful quality improvement projects. A specific opportunity for improvement should be identified. A qualified and inclusive team should be assembled. A clear aim statement should define specific goals of the project. Appropriate measures and benchmarks should be selected. Objective data sources should be identified and appropriately collected, including baseline values. Thorough process analysis should be performed to obtain a complete understanding of specific problems that are obstacles to improvement. A project plan should be constructed, implemented, and continuously evaluated. Initially, when doing quality improvement projects, things may appear to get worse before they get better. This situation is probably due to the Hawthorne effect, which is the initial part of the Abujudeh curve and results from an increase in awareness and observations ( Fig. 1.1 ). When appropriate, the project should be closed, at which time there is documentation of what was learned, proposals for other areas in which this change could be applicable, and ideas for future exploration.

Part II: Patient Safety
There are a multitude of errors that can result in harm to a patient and they can be grouped into a few categories. Diagnostic errors encompass incorrect or missed diagnoses, failure to select appropriate tests, and outdated studies and therapy. Treatment errors include technical mistakes, administration errors, incorrect dosing, unnecessary delay, and nonindicated care. Preventive errors include lack of indicated prophylactic treatment and inadequate screening or follow-up. Systemic errors include, but are not limited to, breakdowns in the chain of communication, equipment malfunction, and process failure. Recent progress in the field of radiology related to safety will be explored later.
Part III: Professionalism and Ethics
A seminal publication on modern professionalism, titled Medical Professionalism in the New Millennium: A Physician Charter , was published in 2002 and was a joint project of multiple medical societies. This charter has been adopted by many medical societies including, in 2005, the Radiological Society of North America (RSNA) Professional Committee. Professional responsibilities in today’s complex healthcare climate are too numerous to adequately detail here. However, they are best summarized as the basis of medicine’s contract with society. This contract is composed of three fundamental principles: primacy of patient welfare, patient autonomy, and social justice.
More recently, Halpern and Spandorfer sought to better frame professionalism within the context of the radiologist. They expanded on some of the more opaque concepts not fully described, such as the learning, teaching, and evaluation of professionalism. Even more importantly, they brought attention to some of the challenges to professionalism faced by current physicians. Managing conflict of interest has become increasingly significant because healthcare is, without a doubt, big business. The dangers of self-referral are still present, especially for those practicing in independent groups. Teleradiology has furthered the loss of contact between radiologists and clinicians and often driven contracts to the lowest price rather than the highest quality. Efforts to incentivize clinical productivity, without caveat, will apply negative pressure to the important but non–revenue-generating aspects of radiology such as resident education and clinician consultation.
Diagnostic errors occur in radiology that are often not discovered until subsequent examinations. There are currently no guidelines for error disclosure by the major radiologic societies. The idea of personally communicating errors to patients, who almost certainly have never met the radiologist and may even be unaware of his or her role, creates complex situations, not to mention potentially litigious challenges. However, simply ignoring that these errors occurred directly refutes the Physician Charter, potentially eroding patient and societal trust. At least one large-scale case study at the University of Michigan, although not specific to radiology, demonstrated that medical error disclosure programs can be implemented without increasing total claims and liability costs. Equitable allocation of limited resources is yet another ethical challenge for radiology as a profession. As a supplemental source to the information provided in this book, the ACR offers a set of online ethics and professionalism courses for its members, most recently revised in January 2015.
Part IV: Compliance, Regulatory, and Legal Issues
Compliance, regulatory, and legal issues are topics typically neglected by many medical schools and residencies. However, that does not diminish their importance and makes self-education all the more crucial. It is nearly impossible to eliminate diagnostic errors in radiology and the resulting litigation that may arise from them, but there are ways to minimize their occurrence as well as their effects on patients and practices. Not surprisingly, diagnostic errors, the genres of which were discussed previously, are the most common cause of malpractice suits against radiologists. An additional pitfall are lapses in communication with providers and patients. Departments or hospitals should have systems in place to prevent this from occurring. It is important to keep accurate documentation of communication efforts, even so-called curbside consultations. Radiologists often engage in activities that involve direct patient care, and, whenever possible, authorized chaperones should be used during these encounters.
While the appropriateness criteria are aimed at improving compliance with best use practices of imaging, there are a multitude of extradiagnostic clinical duties that also warrant standardized conduct. The ACR publishes General Practice Parameters and Technical Standards to provide goals for competency in these areas. The practice parameters offer guidelines on topics including, but not limited to, communication of findings, properly obtaining informed consent, imaging of pregnant patients, patient sedation, and even more unique circumstances such as proper conduct and responsibilities of expert witnesses. The Technical Standards are provided to set necessary levels of performance, mainly regarding equipment specifications. This includes requirements for imaging acquisition equipment as well as diagnostic workstations.
Part V: Research and Screening
Evidence-based medicine, formulated from the reported outcomes of quality research, is the foundation for the proper practice of medicine. With this in mind, it is important for all physicians to understand how appropriate research is conducted and how to properly evaluate new research findings that could impact changes to their practice. The noninterpretive skills domain provides radiologists with a primer on the essentials of research terminology and practice. At a minimum, radiologists should understand the strength of various types of research ranging from cross-sectional studies to randomized controlled trials. Additionally, familiarity with statistical basics such as P values, confidence intervals, sensitivity, specificity, odds ratios, and relative risks will allow one to evaluate the presented data beyond what is described in the discussion or conclusion.
Part VI: Imaging Informatics
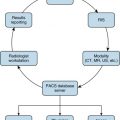
A 2003 national survey attempted to gauge physician involvement in quality improvement. It concluded that the majority of physicians do not routinely use data to assess their performance and are reluctant to share available data. In many industries, especially those in the technology sector, the concept of quarterly and yearly performance reviews is quickly falling out of favor; medicine should take notice and be a part of this trend. The amount of real-time data at our fingertips is growing exponentially. Electronic medical record (EMR) integration is allowing radiologists to access vast amounts of patient data; arguably, the format, ease of access, and usability of this data are varied, but that is outside the scope of this discussion. Picture archiving and communication systems (PACS) and workflow managers are increasingly robust, offering tools for tracking personal performance, seamless follow-up of interesting or indeterminate cases, and alerts for pathology/surgical reports of previously viewed studies. Peer-review systems can tap into the knowledge and expertise of our colleagues. Radiologists must make it a priority to use all tools at their disposal in an effort to measure and improve personal performance. In the spirit of transparency, practice-wide data, anonymized or not, should also be made available.
As we attempt to harness this data to drive improvement, informatics systems and the information technology personnel who build and manage these systems, will become increasingly important. Making sense of this data will not only drive quality improvement, it can also demonstrate the value and effectiveness of care, an increasingly important metric as payment models continue to evolve. Informatics systems can be harnessed by radiologists to track exam appropriateness, patient wait times, timely result communication, and patient safety to name just a few such metrics. It can also be used to evaluate the ordering patterns of clinicians. By identifying trends pertaining to inappropriately ordered exams or nonindicated imaging studies, the radiologist can help better direct hospital initiatives on clinician imaging education, providing value to patients and their referring caregivers, while having the added benefit of saving money.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree