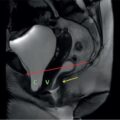
Anirudh Kohli This is probably the most dreaded form of cancer with a dismal outlook. It is the fourth most common cancer. The 5-year survival rate is 15% when the tumour is small and confined to the pancreas with no peripancreatic extension. The 5-year survival rate drops to 6.8% when there is peripancreatic invasion and 1.8% when distant metastases are present. The only option for cure is surgical resection, with a survival rate of 15%–27%. Unfortunately, only 10%–15% of patients with pancreatic adenocarcinoma are eligible for resection. Imaging is important to detect disease as well as to determine resectability. Most patients with recurrent disease following surgery recur due to inoperable disease. Ninety per cent of pancreatic adenocarcinomas present as a focal mass in the head of the pancreas. The remaining 5%–10% present as a diffuse involvement of the gland. A total of 60%–65% of these focal lesions arise in the head of the pancreas, while 20%–25% in the body and 5%–10% in the tail of the pancreas. The most frequent appearance is of a hypodense mass lesion relative to the normal enhancing pancreatic parenchyma on pancreatic phase of enhancement. The decreased attenuation is attributable to fibroblastic proliferation and decreased vascularity. There may be dilatation of the pancreatic duct distal to the mass lesion as the mass lesion obstructs the pancreatic duct. The pancreatic ductal dilatation is smooth and homogenous. Lesions in the head of the pancreas may obstruct the distal common bile duct with resultant upstream biliary dilatation. The distal common bile duct demonstrates a sudden cut-off. A few pancreatic tumours may be isodense; these are recognized only by secondary signs such as loss of lobular texture, contour change, dilatation of pancreatic or bile ducts. Small tumours in the uncinate process may be totally inconspicuous. In addition to detecting pancreatic adenocarcinoma, imaging plays a key role in assessing, if the neoplasm is amenable to resection. As the tumour is seated deep in the retroperitoneum, it typically infiltrates the adjacent superior mesenteric vessels, portal vein or mesenteric neural plexus. Presence of distant metastases also indicates inoperability. To determine vascular invasion, the venous system and arterial system needs to be studied in detail. Multidetector computed tomography (MDCT) with thin isotropic imaging is particularly suited. Images are obtained in the pancreatic phase to study the arteries and in the portal venous phase to study the porto-mesenteric system. The portal vein, splenic vein, superior mesenteric vein and the tributaries of the superior mesenteric vein are evaluated on axial and multiplanar reformation or reconstruction (MPR) images, especially the gastrocolic trunk, inferior mesenteric vein and first jejunal branch. Vascular invasion is seen as encasement of the vessel, that is tumour encircling the vessel totally or vessel coursing through substance of tumour, occlusion of the vessel or contact with vessel wall greater than 180 degrees. Positive predictability for unresectability for MDCT is 89%–100% and for resectability is 45%–79%. Since the only hope for a patient with adenocarcinoma of the pancreas is surgical resection, new techniques have been introduced to perform vascular resection along with tumour with re-anastomosis or placement of grafts. The techniques available are venous resection and reconstruction, hepatic artery segmental resection and/or reconstruction. Venous resections are performed with short segments of superior mesenteric vein, portal vein and/or spleno-portal confluence excised and re-anastomosed. If sufficient length is not available, saphenous venous patches, interposition grafts from the jugular vein may be performed. Thus, patients with tumour encasing the vessel for a short segment or vessel contact greater than 180 degrees can be resected. The key to this is that the two venous ends to be joined should have only one lumen on either side, if the branches’ reconstruction is not possible. Most adenocarcinoma of the pancreas arise in the head of the pancreas; thus they tend to involve the gastroduodenal artery. Involvement of the gastroduodenal artery does not constitute inoperability as it would be resected in a Whipple surgery. The important aspect of gastroduodenal arterial involvement is that cephalad growth of tumour may occur along the gastroduodenal artery to involve the common hepatic artery. Additionally, if there are anomalous origins of the hepatic artery such as accessory or right hepatic artery or common hepatic artery arising from the superior mesenteric artery (SMA), these vessels course close to the posterior aspect of the pancreatic head and are commonly encased. These vessels can be excised for a short segment and primary anastomosis done or if inadequate length available, excised and a reverse saphenous vein graft placed. Though not routinely used by radiologists in reporting, there is value in classifying pancreatic carcinomas by the TNM (“Tumor”, “Nodes”, “Metastases”) classification. Routinely radiology reports essentially cover two important aspects: vascular invasion and distant metastases, which determine operability. Generally T1–T3 tumours are resectable. CT is not very accurate in N staging. This is due to the fact that the criteria for nodal involvement is size. Nodes larger than 10 mm in short axis are considered abnormal. Nodes that are less than 10 mm are considered normal on CT. However, metastases may be present in nodes less than 10 mm. Thus, CT is of limited value in detection of nodal metastases. Positron emission tomography–computed tomography (PETCT) and MRI are of great value in detecting lymph nodal metastases. Metastatic adenopathy smaller than the CT size criteria of 10 mm are detected as they are avid on F-fluorodeoxyglucose (FDG) and may show diffusion restriction/ADC on MRI. PETCT has a higher sensitivity than MRI. PETCT which should be considered as the gold standard for metastatic nodal detection. Infrapyloric, superior to pancreas, hilum of spleen, inferior to pancreas, pancreatoduodenal posterior, pancreatodoudenal anterior. Hepatic artery node is an important node. This node is located at the site of takeoff of the gastroduodenal artery. It is part of the coeliac drainage. Involvement of this node indicates a poor prognosis similar to prognosis when liver metastases are present. The most common site for metastatic disease spread is the liver. Small deposits to the liver and peritoneum may be missed on imaging. Hepatic metastases are seen as hypodense, hypovascular lesions, best demonstrated on the portal venous phase. CT is useful as a guide for performing CT-guided fine needle aspiration cytology (FNAC) of a pancreatic mass to obtain material for histopathology. The only care to be taken is not to transgress large bowel as coliform bacilli may be implanted into the pancreas resulting in secondary infection. Care also needs to be taken not to transgress a vascular structure. MRI is a very useful alternative to CT. MRI demonstrates pancreatic masses similar to CT, as well as is useful in determining resectability. MRI has the advantage of magnetic resonance cholangiopancreatography (MRCP) – therefore able to demonstrate the common bile duct and pancreatic duct very well. There is usually a sudden cut-off of the common bile duct by the pancreatic mass with upstream dilatation. There is also occlusion or narrowing of the pancreatic duct by the pancreatic mass with consequent smooth downstream dilatation of the pancreatic duct secondary to obstruction by the pancreatic mass. Chronic pancreatitis may present with a focal mass lesion in the head of the pancreas with associated pancreatic and biliary duct dilatation. MRCP helps differentiate between a mass lesion due to chronic pancreatitis and Ca pancreas. The pancreatic duct would be irregularly dilated, with possibly intraductal calculi and strictures in chronic pancreatitis as compared to Ca pancreas where the duct would be smoothly dilated. The common bile duct usually terminates abruptly in Ca pancreas as compared to chronic pancreatitis where due to a fibrous stricture there is smooth tapering of the common bile duct. The disadvantages of MRI are its longer acquisition time, slightly lower spatial resolution and inability to obtain material for histopathology. Previously known as solid and papillary epithelial neoplasm. Solid pseudopapillary neoplasms of the pancreas are tumours with a benign or a low malignant potential. These are rare tumours accounting for 9% of cystic pancreatic tumours. A total of 10%–15% of these have a malignant potential. They are usually discovered incidentally; large tumours may cause symptoms due to pain or mechanical obstruction. These tumours are mainly seen in young females, generally in the 20–40 age group, earning their nickname daughter tumours, though they may occur in younger or older individuals. These tumours are usually larger than 3 cm in diameter with an average size of 9 cm, well-defined round encapsulated masses with a heterogeneous consistency. Internally there are haemorrhagic, necrotic, cystic and solid components, contributing to the heterogeneous appearance. On histopathology, they demonstrate psuedopapillary architecture and do not demonstrate exocrine or endocrine cells raising the possibility that these arise from primordial pancreatic stem cells. Progestrone receptors are seen in 81% of cases. On imaging the heterogeneity of these lesions is demonstrated. The solid components tend to be along the periphery and enhance after administration of contrast. An important feature is the capsule of the lesion which is hypointense on T1 and T2 weighted images and enhances densely on the arterial phase with progressive enhancement on the venous phase. Peripheral calcifications may be present; the presence of calcifications may be an indicator of a more aggressive tumour. Smaller SPNs tend to be more solid and homogenous in enhancement. On MRI, these lesions are heterogeneous with bright areas on T1 weighted images due to haemorrhage. The rest of the lesion is usually heterogeneously hypointense on T1 weighted images. On T2 weighted images, the lesion turns heterogeneously hyperintense. Similar to as seen on CT, the lesions have well-defined margins and demonstrate early enhancement in the solid portions with delayed enhancement in the noncystic/haemorrhagic regions. The presence of haemorrhage is a diagnostic feature of these tumours. A small proportion of these tumours may metastasize to the liver. The pancreas may be a site for metastatic disease usually via hematogenous spread. Renal cell CA, lung, breast, ovarian, HCC, GI, thyroid, melanoma may metastasize to the pancreas. These lesions may be localized or multifocal masses resulting in diffuse enlargement of the pancreas. These resemble pancreatic neoplasms, when they are the sole site of metastases. On imaging, differentiation from pancreatic masses is not possible; differentiation can be done only at biopsy. Primary pancreatic lymphoma may occur but it is very rare. More commonly, the pancreas is involved secondarily as part of Non-Hodgkins lymphoma, involving the liver, spleen and lymph nodes. In Non-Hodgkins lymphoma, there is diffuse enlargement of the pancreas. This is hypodense on CT with mild enhancement. Similarly, hypointense to normal pancreatic parenchyma on T1 and T2 weighted images. The diffuse pancreatic enlargement on imaging may mimic acute edematous pancreatitis. The lack of acute symptoms and lack of peripancreatic inflammation help to differentiate. Following treatment, the pancreatic gland reduces in size and calcific foci may be seen in the pancreas. Primary pancreatic lymphoma presents as a mass lesion in the pancreas with peripancreatic adenopathy. This is visualized on imaging as a hypodense mass lesion. There is no dilatation of the pancreatic duct distal to the mass helping to differentiate from adenocarcinoma of the pancreas. An additional feature of note is that there is no hepatosplenomegaly or focal lesions in the liver/spleen; though a biopsy would be required to establish the diagnosis. More commonly, the pancreas is involved secondarily as part of Non-Hodgkins lymphoma. In addition to focal pancreatic involvement, there is focal involvement in the liver/spleen/bowel/mesentery/adenopathy, etc. PETCT is very useful to demonstrate the multifocal involvement. Neuroendocrine tumours (NET) are a heterogenous group of neoplasms which arise from the diffuse neuroendocrine system. These may be found throughout the body, in the lung, pancreas, gastrointestinal tract. Those arising in the pancreas are termed as pancreatic neuroendocrine tumours. Previously, they have been called islet cell tumours, but this is a misnomer as they arise from the ductal pluripotent cells rather than islets of Langerhans. These constitute 10% of all pancreatic tumours. There has been a substantial increase in the last few decades. All neuroendocrine tumours are potentially malignant but differ in their biological characteristics and probability of metastatic disease. Pancreatic NET occur sporadically but some may be associated with inherited genetic syndromes. They have no particular age or sex predilection but when they arise in younger individuals, they are usually part of a familial syndrome. The most common syndrome associated with pancreatic NET is MEN – 1. This syndrome has an autosomal dominant pattern of inheritance due to mutations on chromosome 11, characterized by tumours of the pituitary gland, parathyroid gland and NET of pancreas. Occasionally thyroid, adrenal and ovarian tumours also occur. Less commonly pancreatic NET are associated with VHL disease; this is also autosomal dominant in transmission due to mutation of chromosome 3. VHL is characterized by cerebellar and retinal haemangioblastomas, tumours and lymphoepithelial cysts of the pancreas, kidney and epididymis. Fourteen per cent of patients with VHL have pancreatic NET of which 50% are multiple NET. These are mainly nonfunctional NET. Other syndromes are NF-1 and tuberous sclerosis complex. These are essentially divided into two groups, functional and nonfunctional. Functional tumours hypersecrete hormones such as insulin, gastrin, glucagon, vasoactive intestinal peptide or adrenocortical hormone. These secreted hormones manifest as clinical syndromes with typical features related to the excess production of these hormones. These are usually well-defined rounded neoplasms ranging from 1 to 5 cm. Nonfunctioning tumours do not secrete hormones; therefore these are usually clinically silent. Since they are clinically silent, they are usually large in size at presentation, symptoms arising due to mass effect on adjacent structures. Nonfunctioning tumours constitute 30%–40% of pancreatic NET. Pancreatic NET are much less aggressive than pancreatic adenocarcinoma but often metastasize to the liver. In fact, they are the second most common tumour to metastasize to the liver after colon carcinomas. Imaging is important in detection, staging, preoperative assessment to determine the ideal operative technique – Whipple surgery, distal pancreatectomy or enucleation. Intraoperative ultrasound is also very important to localize nonpalpable tumours for the surgeon, as well as demonstrate relationship between splenic artery, superior mesenteric vessels, CBD and pancreatic duct. Functional tumours are:
9.18: Imaging in solid pancreatic masses
Introduction
Resectability
TNM staging
T staging
N staging
Nodes are classified based on location
M staging
Imaging-guided biopsy for establishing diagnosis
MRI.
Solid pseudopapillary neoplasm of pancreas
Pancreatic metastases
Pancreatic lymphoma
Pancreatic neuroendocrine tumours
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree