Abstract
Radiation risks are of concern to the pregnant patients due to the potential of harmful effects on the fetus. A balance between appropriateness of the exam to be performed on the mother and overutilization of imaging techniques needs to be maintained to provide the best care to the patient. Any imaging technique performed on a pregnant patient should adhere to the “as low as reasonably achievable” (ALARA) principle. When appropriate, ultrasound should always be the first-line modality in imaging the pregnant patient. Before performing any exam on a pregnant patient, a discussion of the benefit versus the risks of the exam should be performed with the referring clinician and pregnant patient. If an exam with ionizing radiation is performed on a pregnant patient, it is imperative that estimation of fetal dose be performed with radiation dose monitoring to provide appropriate counseling and management to the pregnant patient. Iodinated contrast can be used in a pregnant patient; however, gadolinium-based contrast should be avoided as much as possible due to the effects on the fetus. Lactating mothers can be given both iodinated and gadolinium contrast media since the risk to the breastfeeding infant is very low. Breastfeeding should be continued when these agents are given if the mother has normal renal function. Only a high-risk contrast medium such as gadodiamide, gadoversetamide, or gadopentetate dimeglumine requires breastfeeding to be discontinued for 24 hours.
Keywords
contrast, CT, lactation, MRI, pregnancy, radiation, ultrasound, women
Introduction
Radiation risks are of concern in pregnant patients due to the potential of harmful effects on the fetus. However, due to referring physician concerns about maternal health, some exams using ionizing radiation have to be performed in pregnant patients. A balance between appropriateness and overutilization of imaging techniques needs to be maintained to provide the best care to the patient. Any imaging technique performed should adhere to the “as low as reasonably achievable” (ALARA) principle. This chapter discusses the risks and safety issues related to imaging pregnant and lactating patients; reviews the evidence-based imaging recommendations, issues related to contrast administration, counseling, and informed consent and risk management; and discusses modality-specific considerations.
Radiation Dose Risk and Pregnancy
Almost any activity carries certain inherent risks, and the medical use of ionizing radiation is no exception. The mechanism of biological damage from x-ray interactions is well known. Although extensively studied, the risks from low doses of radiation in the ranges typically used in a clinical imaging setting remain highly controversial. Despite the controversy, it is important to recognize that the benefits of medical radiation are clear, and every effort should be made to ensure that these benefits continue to far outweigh any possible risk.
Maternal Risk
The detrimental effects of radiation are due to ionization within tissues, which occur directly with the genetic material itself, or more commonly through formation of free radicals in water molecules, which then react with DNA as shown in Fig. 19.1 . This damage is typically repaired, but unrepaired reactions fall into two categories of biological harm: cell death, which leads to deterministic or tissue effects, or alterations in the genetic code, which leads to stochastic effects.
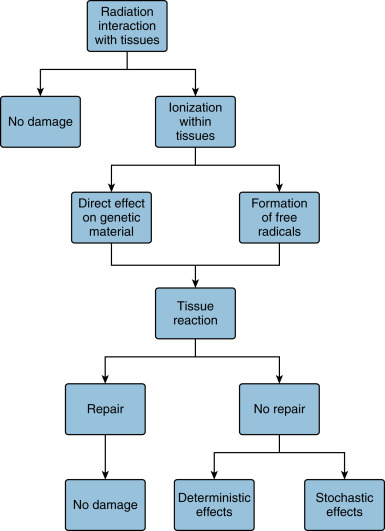
Deterministic or tissue effects are rarely seen in adults at diagnostic exposure levels. These effects are associated with a threshold dose below which no effect is seen, and the severity of the effect increases with the dose. Although quite rare, the adult patient is at some risk of tissue effects due to complications or errors, particularly in interventional radiology cases or perfusion computed tomography (CT). Examples include erythema, epilation, or skin necrosis. Transient skin effects have an approximate threshold of 2 Gy single-site acute skin dose, while effects that may cause longer-term issues do not appear until 5 Gy.
At the low doses seen in diagnostic imaging, most of the risk to the adult is due to stochastic effects. Although highly debated, the scientific community generally assumes that stochastic effects have no dose threshold; therefore even the smallest radiation dose carries a nonzero risk. The stochastic effect of primary concern is cancer induction. Many factors significantly influence the risk of cancer development from exposure to radiation, including age, sex, the rate of exposure, and genetic considerations. As far as a risk estimate, the most widely used figure is a 5% risk of radiation-induced detriment per 1 Sievert (Sv) dose for the adult general population. It should be noted that the radiation-induced excess cancer risk associated with low levels of radiation as used in diagnostic imaging are orders of magnitude smaller than the spontaneous cancer risk.
Fetal Risk
Due to their high rate of cellular proliferation, developing organisms are much more sensitive to the effects of radiation, and thus the fetus is much more sensitive than adults or children. The potential risks include deterministic effects such as microcephaly, mental retardation, organ malformation, fetal death, and stochastic effects such as carcinogenesis. The relative risk of effect depends primarily on gestational age and the total absorbed dose. Although the fetal risks at typical diagnostic imaging dose levels (as well as occupational levels) are minimal, careful consideration should be taken to maintain the fetal dose as low as possible while achieving the greatest diagnostic value from the exam.
In the preimplantation stage (0–2 weeks postconception), the developing embryo is very radiosensitive. The only potential risk is of fetal death, because the radiation-induced effects in this period are considered to have an all-or-none effect. Any nonlethal damage will be repaired to the extent that it will not manifest in any way after birth. The dose threshold for fetal death in this stage is 50 to 100 mGy. After the preimplantation stage, the threshold for fetal death rises to 250 mGy.
During organogenesis (2–8 weeks postconception), the main risk is for teratogenic effects such as microcephaly and organ malformations. The affected organ systems are at most risk during the period of their peak differentiation. The threshold for affects is 100 mGy. The organ group most at risk in humans is the central nervous system, which has a comparatively longer differentiation period.
The effects most likely during the fetal growth stage (weeks 8 to term) are neuropathologies such as mental retardation and lowering of IQ. Most of the risk is negligible unless the doses are very high (>100–200 mGy). The most susceptible period is from weeks 8 to 16, after which the threshold dose for these effects is believed to be 500 mGy.
Carcinogenic risk is assumed to be constant post implantation, though some animal studies suggest a stronger sensitivity in the late fetal growth stage. The excess risk of childhood cancer incidence for exposures of 10 mGy is estimated to be 0.06%, compared to the background risk of 0.14%.
Fetal doses due to diagnostic imaging are rarely high enough to significantly increase risk to the fetus. If the fetus is not in the primary beam of the x-ray, the contribution from scatter radiation is insignificant. Typical fetal absorbed doses for abdominal exams range from 1 to 3 mGy for planar radiography to 16 to 31 mGy for a CT exam, depending on scan parameters and maternal size. Interventional cases can carry a greater radiation burden depending on the duration and complexity of the case, but it is rare for the total fetal dose to exceed 50 mGy.
The American College of Obstetrics and Gynecologists has stated, “Fetal risk of anomalies, growth restriction, or abortion have not been reported with radiation exposure of less than 50 mGy.” The 50-mGy threshold under which prenatal effects of ionizing radiation are considered negligible or nonexistent is echoed in similar position statements issued by other regulatory and professional groups.
Fetal Dose Estimation
Estimation of the fetal dose is required for appropriate counseling and management of pregnant patients who undergo imaging exams. There are many factors that play a part in the estimation, including gestation age, depth and position of the fetus, entrance skin dose to the patient, radiation quality and quantity, geometry of the patient and beam, and others. Due to the complexity of the calculation, it is best to consult with an experienced medical or health physicist for detailed fetal dose estimates. However, a rule of thumb that may be used for gross estimation is that the fetus will receive one-third of the skin entrance dose for radiographic or fluoroscopic procedures. For CT exams or interventional procedures, or any set of exposures that approach 50 mGy, a more detailed estimate should be made to provide the most accurate information possible to the patient and physician.
In an ideal scenario, the pregnancy will be known in advance, and an estimate can be made using a direct measurement method such as placement of a thermoluminescent dosimeter on the abdomen before the exposure. This, in conjunction with other details, will allow an accurate estimation. In the more likely event of an unknown pregnancy that is revealed later, it is best to gather as much information about the case as soon as possible, interviewing anyone present about information they can recall that will aid in the calculation. Modern equipment should provide a detailed record of the exposure that is accessible. There are several methods that can be employed to estimate the fetal dose, depending on the amount of information that is available as shown in Table 19.1 .
| Prospective Dose Estimation | Retrospective Dose Estimation |
|---|---|
|
|
|
|
|
|
|
|
| |
|
Modality-Specific Considerations
Specific issues apply to modalities that use ionizing radiation (i.e., radiography, CT, nuclear medicine, and fluoroscopy) and those that do not use ionizing radiation (i.e., magnetic resonance imaging [MRI] and ultrasound).
Computed Tomography: Indication for Use
Currently, CT is mainly used in evaluating pregnant patients with trauma or suspected pulmonary embolism, which are the two main causes of maternal mortality.
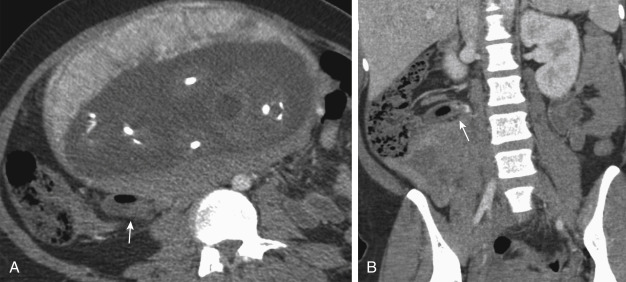
Both major and minor trauma result in an increased risk of loss of pregnancy. The risk of pregnancy loss in trauma is reported to be between 1% and 34%; however, penetrating trauma has a higher rate of pregnancy loss, reaching almost 73%. Maternal death almost always results in fetal loss, although rare instances of emergency caesarean section despite lethal maternal injuries have been reported. The best chance of fetal survival is maternal survival. After maternal stabilization, imaging of the mother is performed with radiography, CT, or angiography as is necessary. Focused abdominal sonography for trauma is performed at the bedside for findings of free intraperitoneal or pericardial fluid. In cases of a positive focused abdominal sonography for trauma exam or if the suspicion is high, CT is the preferred modality for evaluation of hollow or solid organ trauma and vascular injury. In major trauma, risk of radiation exposure is small compared to the risk of maternal mortality or injury from missed or delayed diagnosis. Appropriate technique is used in imaging pregnant trauma patients, like nonextreme low-dose exams to ensure diagnostic quality of the exam, single-phase exams to decrease the radiation risk, and appropriate coverage of the anatomy. If delayed scans are required, they are focused on the area of interest and are performed at a lower dose than the initial scan. CT cystography ( Fig. 19.2 ) may be necessary in cases where bladder rupture is suspected and can be performed with low-dose techniques.
In cases with suspected pulmonary embolism, a positive diagnosis of deep venous thrombosis can obviate further workup, and therefore a chest radiograph with abdominal shield and vascular ultrasound are the first-line exams of choice. If the results of these exams are unavailable or equivocal, a CT pulmonary angiogram with abdominal shield is performed.
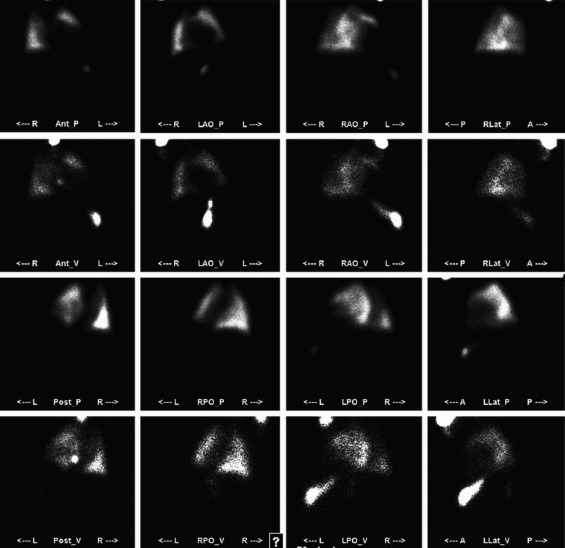
CT pulmonary angiogram has a dose similar to a ventilation-perfusion (V/Q) scan; however, CT is capable of providing an alternative diagnosis in cases of negative pulmonary embolism exams. The radiation dose in the first and early second trimesters is also low due to low scatter. If the patient is allergic to contrast, a V/Q scan ( Fig. 19.3 ) can be performed. The American Congress of Obstetricians and Gynecologists and the Fleischner Society recommend CT pulmonary angiography for pregnant patients with suspected pulmonary embolism.
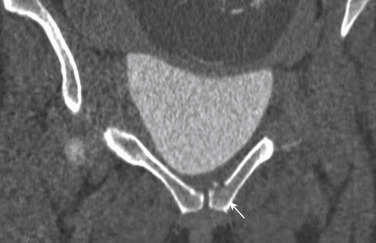
Another indication for using CT in pregnant patients is acute abdominal pain. In these cases, an attempt should be made to evaluate the pathology with ultrasound (e.g., appendicitis [ Fig. 19.4 ]) and, if unsuccessful, a CT should be performed. Low-dose strategies should definitely be used when scanning the abdomen and pelvis in pregnant patients.
Dose Considerations and Dose Reduction Strategies
Even though the radiation exposure to the fetus is low when the fetus is not in the field of view, adhering to the principle of ALARA is important. Standard protocols should not be used in pregnant patients and should be replaced with low-dose protocols. To achieve this, the technologist should lower the tube potential (kilovolts) based on the patient’s weight, decrease tube current-time product (milliampere second [mAs]), limit image length, increase pitch, and limit the number of acquisitions to one. Additional techniques like automated exposure control, automated tube potential selection, and iterative reconstructions should also be used. Techniques for reducing dose to the pregnant patient are listed in Box 19.1 .