Technical Aspects
Technique
The patient is given sodium bicarbonate/dimethicone granules (Carbex), a gas-producing agent, to swallow and then drinks the E-Z HD 250% weight/volume 60 mL barium. Spot views of the esophagus are taken at the beginning (anteroposterior and right anterior oblique positions) while barium is being swallowed (if clinically indicated), and then the patient is asked to lie down on the left side (thus preventing the barium reaching the distal duodenum too quickly and obscuring views of the greater curvature and antrum of the stomach). The patient then is asked to lie slightly on the right so that the barium is against the gastroesophageal junction to check for reflux while screening. If reflux is not elicited, the patient may be asked to cough, swallow water, or tip the head down while being observed fluoroscopically and spot films are taken.
Stomach Views
- •
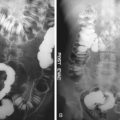
Antrum and greater curvature : Right anterior oblique ( Figure 19-1 )

Figure 19-1
Right anterior oblique view.
- •
Body and antrum: Supine ( Figure 19-2 )
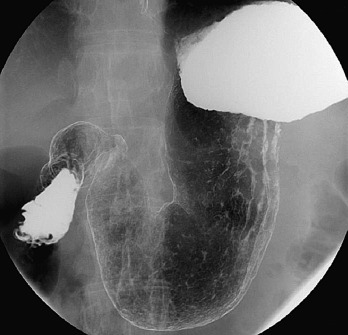
Figure 19-2
Supine view.
- •
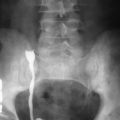
Lesser curvature en face: Left anterior oblique ( Figure 19-3 )

Figure 19-3
Left anterior oblique view.
- •
Left lateral: With head tilted up at 45 degrees
Duodenum Views
- •
Duodenal loop: The patient lies prone on the compression pad to prevent barium flooding into the duodenum (additional views of the anterior wall of the duodenal loop can be taken in the right anterior oblique position).
- •
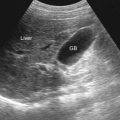
Duodenal bulb: The following spot views can help: prone, right anterior oblique, supine, and left anterior oblique (occasionally tilting the head up and allowing the air bubble to rise into the coated duodenal cap) ( Figure 19-4 ). The appearance of the duodenum varies according to the patient’s body habitus, and the gallbladder often indents the duodenal cap.

Figure 19-4
Duodenal view.
Single-Contrast Examination
A single-contrast examination can emphasize mucosal relief, compression, and barium filling. This includes spot views of the barium-filled stomach with the patient recumbent: prone, left posterior oblique, right lateral, and right anterior oblique. Mucosal relief radiographs are performed by giving the patient 60 to 90 mL of barium to drink, and then prone and supine spot views are taken to correctly demonstrate the gastric fold pattern. The anterior gastric wall is better seen on the single-contrast study than the double-contrast examination. Compression views require compression of the stomach, which is moderately distended with a small amount of barium to spread on the rugal folds. Overdistention makes it impossible to penetrate the barium radiographically, and the amount of barium used can be controlled by patient rotation or tilting the table. The views seen vary according to patient body habitus, and compression can be performed only below the rib cage; hence, often only the distal stomach can be identified. The compression view often demonstrates ulcers and masses, although small flat lesions can be missed and wall rigidity may occur from scarring or infiltration.
Normal Anatomy
When fully distended the stomach forms a J -shaped configuration and is divided into cardia, fundus, body, pyloric antrum, and pylorus ( Figure 19-5 ). The stomach has two surfaces: anterosuperior and posteroinferior, bounded by two borders, the lesser and greater curvatures, respectively. This hollow organ is completely covered by peritoneum, which passes as a double layer from the lesser curve (as the lesser omentum) and from the greater curve (as the greater omentum). The stomach is composed of four layers: the outer serosa layer, muscularis externa, submucosa, and mucosa. The outer serosal layer consists of layers of connective tissue continuous with the peritoneum. The muscularis externa consists of three layers: the inner oblique layer (thicker at the antrum to perform forceful contractions); a middle circular layer that is thickest at the pylorus, forming a pyloric sphincter; and an outer longitudinal layer. The stomach is lined by columnar cells (for acid protection), unlike the esophagus, which is lined with squamous cells.

The duodenum has a C -shaped configuration and is divided into four parts. The first (superior) portion extends from the pylorus to the neck of the gallbladder and consists primarily of the duodenal bulb. The second part ( Figure 19-6 ) lies to the right of the second/third lumbar vertebrae, running inferiorly lateral to the head of the pancreas and medial to the hilum of the right kidney. Posteromedially at the junction of the upper two thirds and the lower third of the duodenum lies the opening of the duodenal papilla or ampulla of Vater (opening of the bile and pancreatic ducts).

The third part runs from right to left below the lower margin of the head of the pancreas, whereas the fourth portion is 4 cm and runs craniad and lies medial to the left psoas muscle, fixed by the ligament of Treitz (a peritoneal fold that ascends to the right crus of the diaphragm). This is an important landmark when distinguishing malrotation of the small intestine in children. The first part of the duodenum is the only part that is intraperitoneal, whereas the rest are retroperitoneal structures, again an important point for localizing a pathologic process.
Normal Anatomy
When fully distended the stomach forms a J -shaped configuration and is divided into cardia, fundus, body, pyloric antrum, and pylorus ( Figure 19-5 ). The stomach has two surfaces: anterosuperior and posteroinferior, bounded by two borders, the lesser and greater curvatures, respectively. This hollow organ is completely covered by peritoneum, which passes as a double layer from the lesser curve (as the lesser omentum) and from the greater curve (as the greater omentum). The stomach is composed of four layers: the outer serosa layer, muscularis externa, submucosa, and mucosa. The outer serosal layer consists of layers of connective tissue continuous with the peritoneum. The muscularis externa consists of three layers: the inner oblique layer (thicker at the antrum to perform forceful contractions); a middle circular layer that is thickest at the pylorus, forming a pyloric sphincter; and an outer longitudinal layer. The stomach is lined by columnar cells (for acid protection), unlike the esophagus, which is lined with squamous cells.
The duodenum has a C -shaped configuration and is divided into four parts. The first (superior) portion extends from the pylorus to the neck of the gallbladder and consists primarily of the duodenal bulb. The second part ( Figure 19-6 ) lies to the right of the second/third lumbar vertebrae, running inferiorly lateral to the head of the pancreas and medial to the hilum of the right kidney. Posteromedially at the junction of the upper two thirds and the lower third of the duodenum lies the opening of the duodenal papilla or ampulla of Vater (opening of the bile and pancreatic ducts).
The third part runs from right to left below the lower margin of the head of the pancreas, whereas the fourth portion is 4 cm and runs craniad and lies medial to the left psoas muscle, fixed by the ligament of Treitz (a peritoneal fold that ascends to the right crus of the diaphragm). This is an important landmark when distinguishing malrotation of the small intestine in children. The first part of the duodenum is the only part that is intraperitoneal, whereas the rest are retroperitoneal structures, again an important point for localizing a pathologic process.
Patterns and Appearances on Barium Studies
Gastric Ulcers
The detection of gastric ulcers and the decision regarding whether these represent benign or malignant processes are a major part of the barium meal study.
Helicobacter is a gram-negative bacteria that is recognized as an important cause of 70% of peptic ulcer disease and 95% of duodenal ulcers in the United States. Patients infected with Helicobacter pylori have a six times risk for developing gastric carcinoma and a 90% association with mucosal-associated lymphoid tissue. Other causes of infectious gastritis include tuberculosis, histoplasmosis, and syphilis.
Ulcers are best identified on double-contrast studies. Often they are common on the posterior wall of the stomach and least common on the fundus. Ulcers secondary to nonsteroidal antiinflammatory drugs and alcohol are often seen on the greater curvature of the antrum, possibly owing to the direct toxic effects.
The en face radiologic signs of gastric ulcers are best seen on double-contrast studies. Primarily, the signs include pooling of barium within the ulcer crater (on the dependent wall). A thin radiolucent line is often seen separating the barium in the lumen from that in the crater and is referred to as Hampton’s line. If the ulcer is on the nondependent wall, the barium coats the “rim,” causing a ring-like effect. The patient can be turned prone or supine to fill the middle part of the crater. Often a small mound of edema is seen surrounding the crater, causing a circular filling defect. The folds radiating from this should be smooth and symmetric with normal areae gastricae, suggesting benignity. Classically, benign ulcers are seen on the lesser curvature ( Figure 19-7 ). Giant ulcers (≥3 cm) are virtually almost always benign. A healed ulcer is identified when folds converge to the site of the ulcer, whereas incomplete healing, irregularity of the folds, residual mass, or loss of mucosal pattern suggests malignancy.
Carman’s meniscus sign is diagnostic of a specific type of ulcerated neoplasm. When examined in profile with compression, the ulcer has a semicircular (meniscoid) configuration. The combination of this characteristic type of barium-filled ulcer and a radiolucent shadow of the elevated ridge of neoplastic tissue surrounding it is called the Carman-Kirklin complex. The inner margin of the barium trapped in the ulcer is usually irregular. It is always convex toward the lumen, in contrast to the “crescent sign” of a benign gastric ulcer in which the inner margin is concave toward the lumen.
An abrupt transition between the normal mucosa and the abnormal tissue surrounding a gastric ulcer is characteristic of a neoplastic lesion, in contrast to the diffuse, almost imperceptible transition between the mound of edema surrounding a benign ulcer and normal gastric mucosa. Nodularity, clubbing, and amputation of normal radiating folds also suggest a malignant lesion.
Duodenal Ulcers
Duodenal ulcers also can be identified by double-contrast studies, and sometimes complications are seen—for example, formation of a fistula with the biliary tree ( Figure 19-8 ).
Narrowing of the Stomach (Linitis Plastica Pattern)
A linitis plastica pattern refers to any condition in which marked thickening of the gastric wall causes the stomach to resemble a rigid tube. The most common cause is scirrhous carcinoma of the stomach ( Figure 19-9 ). The tumor invades the gastric wall, resulting in a desmoplastic reaction that leads to diffuse thickening and fixation of the stomach wall. At fluoroscopy, peristalsis does not pass the tumor.
Other lesions that can mimic this appearance are lymphoma, Kaposi’s sarcoma, and metastases. Sometimes benign causes such as ulcer disease, Crohn’s disease, sarcoidosis, and tuberculosis can cause this appearance.
Filling Defects in the Stomach
Areae gastricae are normal anatomic features of the gastric mucosa. On a double-contrast study they appear as a fine reticular pattern surrounded by barium-filled grooves. This appearance simulates multiple filling defects.
Hyperplastic polyps are the most common causes of discrete gastric filling defects, accounting for up to 90% of all gastric polyps. Most hyperplastic polyps appear as sharply defined, round or oval filling defects measuring less than 1 cm. They have smooth contours and no evidence of contrast material within them. They tend to be multiple and are clustered in the fundus or body of the stomach.
An adenomatous polyp is a true neoplasm; it shows a tendency to malignant transformation and is therefore vital to identify. Characteristic features include size greater than 1 cm, lobulated or pedunculated shape, and a variation in size over time.
Other lesions that can present as filling defects include lymphoma, carcinoid tumor, and metastases.
Thickening of Gastric Folds
Longitudinal folds traverse the stomach in the direction of its long axis. Folds in the fundus are thicker and more tortuous than distally. Folds in the antrum measuring more than 5 mm are considered abnormal. These folds may appear prominent in a nondistended stomach.
Extrinsic Lesions
Lesions outside the gastric walls could indent on the stomach and cause extrinsic impressions or apparent filling defects. Cysts arising from the kidney, spleen, and pancreas can produce these appearances.
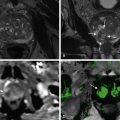
Widening of the Duodenal C Loop
Although widening of the duodenal C loop is often taken to represent pancreatic malignancy, benign conditions such as pseudocyst also may cause such an appearance. It is advisable to resort to cross-sectional imaging to resolve ( Figure 19-10 ).

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree