NASOLACRIMAL APPARATUS: ACUTE AND CHRONIC INFECTIONS AND NONINFECTIOUS INFLAMMATORY CONDITIONS
KEY POINTS
- Imaging is not required in the vast majority of patients with acute and chronic infections and noninfectious inflammatory conditions of the nasolacrimal apparatus.
- Imaging can be used to identify the level of obstruction and complicating factors that will alter medical decision making in selected cases.
- Imaging can help exclude dangerous confounding factors such as an obstructing mass.
Any orbital mass or disease process may be approached by first establishing whether it is preseptal (Chapters 70 and 71) or postseptal (Chapters 57–60, 62, and 64). Nasolacrimal apparatus problems are generally predominantly preseptal in their manifestations. The vast majority of these do not come to imaging. This chapter considers nasolacrimal apparatus inflammatory processes as well as those arising in this location that might spread across the orbital compartments and related spaces.
Noninfectious inflammatory diseases may be local or related to systemic disease. Practically the only specific ones that involve the nasolacrimal system with any significant incidence are sarcoidosis and Wegener granulomatosis. Primary acquired nasolacrimal duct obstruction (PANDO) is an idiopathic inflammation, and fibrosis may cause stenosis or obliteration of the nasolacrimal duct; its specific etiology is not known.
Infections, like noninfectious inflammatory conditions, may be local or related to systemic disease. The vast majority of these conditions arise within the nasolacrimal system with few due to secondary spread from conditions of the sinonasal region (Chapters 84–86) and lacrimal gland (Chapter 65).
Secondary acquired nasolacrimal duct obstruction (SALDO) may be due to an unknown infectious or noninfectious inflammatory process. This can also be caused by dacryoliths, tumor (Chapter 69), radiation therapy, systemic and topical medicines, trauma, and a host of other etiologies.
ANATOMIC AND DEVELOPMENTAL CONSIDERATIONS
Applied Anatomy
The relevant anatomy of the nasolacrimal drainage system is discussed in detail in Chapter 44.
IMAGING APPROACH
Techniques and Relevant Aspects
The nasolacrimal drainage pathways are studied with computed tomography (CT) and magnetic resonance (MR) techniques described in detail in Chapters 44 and 45. Specific CT protocols by indications are detailed in Appendix A. Specific MR protocols by indications are outlined in Appendix B. Almost all studies to investigate potential lacrimal drainage system inflammatory pathology are done with contrast.
Pros and Cons
Disease of the lacrimal drainage is studied primarily with CT, with magnetic resonance imaging (MRI) held in reserve for highly selected cases.
CT typically is used to identify bone changes and exclude abscess or an obstructing mass.
Dacryocystography might be avoided in acutely inflamed systems but can be useful to show concretions that may need to be surgically removed.
Dacryoscintigraphy may be used to noninvasively determine the level and degree of obstruction as discussed in Chapter 5.
CT-dacryocystography or MR-dacryocystography may be performed by either directly injecting contrast into the lacrimal system or by administering an eye drop. It gives additional cross-sectional soft tissue information and may help to identify the level of obstruction.
Ultrasound is of no real clinical decision-making benefit.
SPECIFIC DISEASE/CONDITION
Noninfectious Inflammatory Disease
Etiology
PANDO is an idiopathic inflammation, and fibrosis may cause stenosis or obliteration of the nasolacrimal duct; its specific etiology is not known.1
Other noninfectious inflammatory diseases may be local or related to systemic disease. The nasolacrimal drainage system may be involved with granulomatoses that infiltrate the orbit and appear identical to lymphoma. These diseases are discussed in general in chapters on sarcoidosis (Chapter 18), Wegener granulomatosis (Chapter 17), and Langerhans histiocytosis (Chapter 19). These may produce SALDO. More commonly, noninfectious SALDO is associated with prior exposure to toxic agents such as radiation, chemotherapy, or certain topical medicines such as those once commonly used to treat glaucoma.
Prevalence and Epidemiology
PANDO is most common in middle-aged women, perhaps due to the smaller dimensions of their ductal system. SALDO has no particular age or gender predilection.
Clinical Presentation
Nasolacrimal obstruction/inflammation presents sometimes with bloody tearing (epiphora), epistaxis, medial canthal region pain, recurrent conjunctivitis, and nasolacrimal sac distension (Figs. 68.1–68.8). Purulent discharge (from secondary development of infection) is not uncommon, and pressure over the nasolacrimal sac may induce reflux of purulent material into the eye.
Pathophysiology and Patterns of Disease
These conditions produce inflammation and various degrees of obstruction of the lacrimal drainage system. This may eventually lead to fibrosis and chronic obstruction (Fig. 68.9).
Manifestations and Findings
Computed Tomography and Magnetic Resonance Imaging
CT and MRI will show a dilated lacrimal sac (Figs. 68.1–68.8) and possibly bony erosion along the duct or of the lacrimal bone (Figs. 68.4 and 68.5). Bone changes may not be as apparent on MRI since this is cortical bone being demineralized. The CT and MRI findings in inflammatory disease are discussed in general in Chapters 13 and 16 and with regard to sarcoidosis (Chapter 18), Wegener granulomatosis (Chapter 17), and Langerhans histiocytosis (Chapter 19) in those chapters noted.

FIGURE 68.1. Computed tomography study of a patient with an antrochoanal polyp (arrowhead) causing distention of the lacrimal sac (arrow). This produced a compressible mass in the inner quadrant of the orbit.

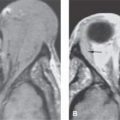
FIGURE 68.2. Computed tomography study of patient with preseptal swelling and pain. A: There is soft tissue swelling and possible lucency in the lacrimal sac on the left (arrow) compared to the normal air-filled sac on the right (arrowhead). B: Axial section confirms fluid in a distended lacrimal sac (arrow) compared to the normal side (arrow). The source of this preseptal infection was the lacrimal drainage system.

FIGURE 68.3. Computed tomography of an immune-suppressed patient with preseptal orbital cellulitis. A: Extensive swelling is present in the inferior medial portion of the orbit (arrow). B: Axial section shows soft tissue swelling in the preseptal soft tissues (white arrows) and extending posterior to the posterior lacrimal crest (arrowhead) indicating early postseptal involvement. There is also fluid in the conjunctival sac (black arrow). C: Coronal images show that the source of this infection was sinus disease with secondary involvement of the lacrimal sac region. (NOTE: Clinically, it is often difficult to determine the source of infection in lacrimal sac region infection. Imaging can frequently help make this distinction.)

FIGURE 68.4. Computed tomography of a chronic cocaine abuser with swelling and pain in the inferior medial orbital region due to secondary acquired nasolacrimal duct obstruction. A: The lacrimal sac is distended with pus (white arrow). The infectious source is the extensive disease within the nasal cavity that produced the obstruction/infection (white arrowhead). Note that the disease also causes distention of the nasolacrimal duct on the left (black arrowheads). B: Axial section clearly shows that the disease is centered in the lacrimal sac (arrows) and that it erodes the lacrimal bone (white arrowhead). C: Sagittal reformation shows the extent of disease in the lacrimal sac (arrow) as well as in the nasolacrimal duct (arrowheads).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree