The term nephrocalcinosis was coined in 1934 by Fuller Albright. Nephrocalcinosis refers to the deposition of calcium salts (oxalate and phosphate) in the renal parenchyma. It can be medullary, cortical or combined. Medullary nephrocalcinosis is the most common type and is seen in 98% of cases. Nephrocalcinosis can be incidentally detected on imaging in patients with normal kidney function or in patients with acute or chronic kidney injury. Multiple conditions can cause nephrocalcinosis, and prognosis depends on the underlying aetiology. Nephrocalcinosis is in most cases, an asymptomatic, chronic and slowly progressive disease that is discovered as an incidental finding during radiographic imaging. Such imaging may be obtained as part of evaluation of nephrolithiasis, which often coexists with nephrocalcinosis. However, some patients present with clinical symptoms that are related to nephrocalcinosis or to the causative process. These include renal colic, nocturia, polyuria and polydipsia. Some causes of nephrocalcinosis can present acutely with renal failure. Nephrocalcinosis can occur secondary to varying aetiologies. Based on the location of calcium deposition, nephrocalcinosis is classified as medullary, cortical or global (Box 10.12.4.1.1). Medullary nephrocalcinosis is further classified based on the underlying metabolic derangement. CAUSES OF NEPHROCALCINOSIS Conditions causing hypercalcaemia and hypercalciuria Conditions causing hypercalciuria In hypercalcaemia, metastatic calcification takes place in normal renal tissue, leading to medullary nephrocalcinosis. Hypercalcaemia results in hypercalciuria, leading to higher incidence of urolithiasis. Severe prolonged hypercalcaemia leads to irreversible renal impairment due to tubulointerstitial damage which can present as small smooth kidneys. On imaging, chronic hypercalcaemia is usually seen as diffuse, symmetric medullary nephrocalcinosis with small, smooth kidneys. Medullary nephrocalcinosis is seen only in with type I or distal renal tubular acidosis. There is progressive renal insufficiency in these patients. Urolithiasis is common due to hypercalciuria and hypocitraturia. Medullary calcifications are diffuse and symmetric, involving all renal pyramids of both kidneys. Kidneys are normal in size and maintain normal contour. Medullary sponge kidney is thought to be a congenital disorder in which there is ectasia of the renal tubules. It is often an incidental finding of little clinical significance. However, there is increased risk of urolithiasis and pyelonephritis. Ectasia causes urine stasis and precipitation of calcium and related minerals. Calcifications are usually rounded and multiple, arranged radially, emerging from the renal papilla. Calculi in dilated renal tubule appears to increase in size on postcontrast images, seen as growing calculus sign. Most patients with medullary sponge kidney have normal-sized kidneys. Analgesic nephropathy, secondary to prolonged intake of large doses of NSAIDs can cause medullary nephrocalcinosis and chronic renal insufficiency. Medullary nephrocalcinosis detected in combination with bilateral small, scarred kidneys strongly suggests analgesic nephropathy. In hyperoxaluria there is abnormality in the enterohepatic metabolic pathways. This leads to increased excretion of oxalates in urine, causing medullary nephrocalcinosis and formation of calcium oxalate stones. Hyperoxaluria can also cause cortical nephrocalcinosis. Primary hyperoxalosis is an irreversible condition and causes death at a young age. Secondary hyperoxaluria is caused by small bowel resection and extensive disease of the small bowel. Renal tuberculosis can cause calcifications of the urinary tract in 10% of cases. Renal TB is usually seen in one kidney and starts at a single renal papilla. As the infection progresses, it extends into the renal calyx and is associated with papillary necrosis. Infection can then extend along collecting system leading to inflammation and fibrosis. In later stages it presents as hydronephrosis, eventually leading to autonephrectomy. Asymmetric unilateral renal scarring or stricturing with associated nephrocalcinosis is highly indicative of renal tuberculosis. Cortical nephrocalcinosis is due to dystrophic calcification following renal parenchymal tissue destruction. Major cause of cortical nephrocalcinosis is chronic glomerulonephritis. It is associated with chronic renal failure. On imaging it can present as small smooth kidneys with shell-like calcifications involving the renal cortex. Acute cortical necrosis is another major cause of cortical nephrocalcinosis. It is caused by severe hypotension, secondary to complications of childbirth, sepsis or severe blood loss. It can also be secondary to ingestion of nephrotoxins, such as ethylene glycol. Medullary nephrocalcinosis can present as fine, stippled, coarse or confluent calcifications in the renal pyramids (Figs 10.12.4.1.1–10.12.4.1.2 and 10.12.4.1.5A). Cortical nephrocalcinosis presents as punctate or ‘tram line’ cortical calcifications. Nephrocalcinosis is not seen on plain radiographs if attenuation is less than 100 Hounsfield units (HU) or if the size is less than 2 mm.
1. Nephrocalcinosis
Introduction
Clinical features
Aetiology
Pathogenesis
Hypercalcaemia and hypercalciuria
Hypercalciuria without hypercalcaemia
Type I or distal renal tubular acidosis.
Medullary sponge kidney
Analgesic nephropathy
Hyperoxaluria
Renal tuberculosis
Cortical nephrocalcinosis
Imaging
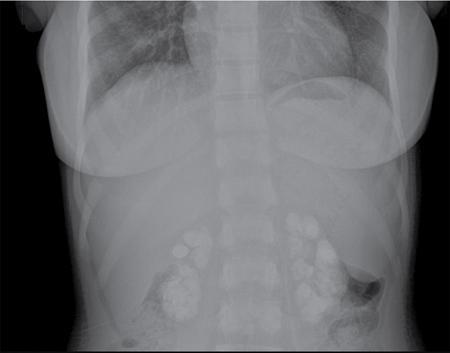
Radiography
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








