Abdominal pain is a common occurrence in pregnant women and may have a variety of causes, including those that are specific to pregnancy (eg, round ligament pain in the first trimester) and the wide range of causes of abdominal pain that affect men and women who are not pregnant (eg, appendicitis, acute cholecystitis). Noncontrast magnetic resonance (MR) imaging is increasingly performed to evaluate pregnant women with abdominal pain, either as the first-line test or as a second test following ultrasonography. The imaging appearance of causes of abdominal pain in pregnant women are reviewed with an emphasis on noncontrast MR imaging.
Key points
- •
Determining the cause of abdominal pain in pregnant women can be challenging because of anatomic changes that make physical examination findings less reliable.
- •
Noncontrast magnetic resonance imaging is increasingly performed to evaluate for causes of acute abdominal pain in pregnant women, either as the first-line test or as a second-line test following ultrasonography.
- •
Accurately determining the cause of abdominal pain in pregnant women is important so that timely treatment can be initiated to benefit the mother and the fetus.
- •
The imaging appearances of common causes of abdominal pain are reviewed with example images provided.
Introduction
Abdominal pain is a common occurrence in pregnant women, and potential causes range from those specific to pregnancy (eg, round ligament pain in the first trimester; contractions in later stages of pregnancy) to the wide range of disorders that are not specific to pregnancy but can also cause abdominal pain in men and women who are not pregnant (eg, acute appendicitis, cholecystitis, nephrolithiasis). However, physical examination findings may be less reliable, especially in later stages of pregnancy, because of changes in anatomy that occur as the fetus grows and the uterus enlarges. For example, the cecum and appendix may be pushed from the right lower quadrant to the right upper quadrant by the enlarging uterus, thus confounding the physical examination in a pregnant woman with clinically suspected acute appendicitis.
In addition, physiologic changes result in symptoms that are considered normal during pregnancy, including nausea and vomiting in the first trimester and gastroesophageal reflux and constipation in later stages of pregnancy, but overlap with symptoms of more concerning causes of abdominal pain. Furthermore, normal physiologic changes of pregnancy, such as an increase in the pregnant woman’s white blood cell count and mild anemia, may also confound the diagnosis of intra-abdominal disorder.
Prompt and accurate diagnosis of the cause of abdominal pain in pregnancy is important so that appropriate management can be initiated for the health of the pregnant woman and the fetus. Recent years have seen a shift toward noncontrast magnetic resonance (MR) imaging for the evaluation of pregnant women with abdominal pain, either as a secondary test following an inconclusive ultrasonography scan or as the primary test for some indications, such as acute appendicitis. This article presents a general approach to the imaging evaluation of pregnant women with abdominal pain and then reviews the imaging findings of a variety of causes of abdominal pain with an emphasis on MR imaging.
Imaging approach
If a pregnant woman presents with localizing abdominal pain and the differential diagnosis is narrow (eg, acute cholecystitis), ultrasonography could be performed as the first-line test because it is readily available, rapidly performed, inexpensive, and does not expose the fetus or mother to ionizing radiation. Ultrasonography is reasonably accurate for diagnosing some causes of abdominal pain, such as hydronephrosis or acute cholecystitis. In centers with expertise, ultrasonography may the first-line test to assess for acute appendicitis in pregnant women.
When ultrasonography is inconclusive or does not identify a cause of acute abdominal pain, or if the mother’s symptoms are nonlocalizing and the differential diagnosis is broad, noncontrast MR imaging is the preferred modality because it also does not expose the fetus or mother to ionizing radiation and provides a comprehensive analysis of the abdomen and pelvis. In addition, noncontrast MR imaging may be the preferred test to evaluate for acute appendicitis in some institutions based on institutional expertise. Noncontrast MR imaging is not associated with increased harm to the fetus or in early childhood. On the contrary, gadolinium administered at any time during pregnancy was found to be associated with an increased risk of stillbirth, neonatal death, and rheumatological, inflammatory, and infiltrative skin conditions. Given these recent data and theoretic concerns from prior animal studies, gadolinium use should be limited to rare situations in which benefits clearly outweigh the potential risks.
A sample noncontrast MR protocol is provided in Box 1 . T1-weighted sequences are helpful for general anatomic assessment and for the identification of blood products that, depending on age, may show high signal intensity on T1-weighted imaging. T2-weighted sequences, including MR cholangiopancreatography (MRCP), are helpful to assess for disorders related to fluid-containing structures (eg, choledocholithiasis, hydronephrosis). Thick-slab MRCP images provide an overview of the biliary system, whereas thin slices are helpful to assess for intraductal stones, which can be obscured by thick-slab volumetric techniques or maximum intensity projection images from three-dimensional MRCP. T2-weighted sequences with fat saturation are key to assess for inflammation because the fluid signal intensity of inflammation is more conspicuous against a background of low-signal-intensity fat. In-phase images are helpful to assess for susceptibility artifacts. For example, the identification of blooming air within the appendix can help when trying to find the appendix on MR. Opposed-phase images are helpful to assess for fat-water interfaces and fat-containing structures such as dermoids or renal angiomyolipomas. Diffusion-weighted images are helpful to highlight areas of inflammation, abscesses, and tumors.
T2 (single shot; eg, half-Fourier acquisition single shot turbo spin echo [HASTE]/single shot fast spin echo [SSFSE]) axial and coronal, abdomen and pelvis
T2 (single shot; eg, HASTE/SSFSE) sagittal pelvis
T2 with fat saturation (single shot; eg, HASTE/SSFSE) axial and coronal, abdomen and pelvis
MR cholangiopancreatography (thick slab and thin cuts)
T1 with fat saturation gradient echo axial and coronal, abdomen and pelvis
In-phase and opposed-phase axial abdomen and pelvis
Diffusion-weighted abdomen and pelvis
Steady-state free precession abdomen plus/minus pelvis
In the setting of trauma, the risk/benefit profile of computed tomography (CT) may warrant performing a CT examination for pregnant women, with special attention to achieving a CT dose that is as low as is reasonably achievable. Because CT is typically more readily available and is performed with faster image acquisition times compared with MR, CT is often the preferred imaging modality for pregnant women who have experienced trauma. According to the America College of Obstetricians and Gynecologists, if CT is necessary in addition to ultrasonography or MR, or is more readily available for the diagnosis in question, it should not be withheld from pregnant women. Although iodinated contrast material crosses the placenta and enters the fetal circulation or amniotic fluid, it has not been shown to have mutagenic or teratogenic effects or adverse effects on the fetal thyroid.
Acute appendicitis
Acute appendicitis is the most common indication for nonobstetric surgery in pregnant women. Accurately diagnosing acute appendicitis in pregnant women is challenging because of anatomic changes rendering physical examination findings less reliable and physiologic changes in hematologic parameters such as the normal increase in serum white blood cell count that occurs in pregnant women. Accurate diagnosis is important because of the risk of fetal loss, which is greater for complicated (6% fetal loss) versus simple (2%) appendicitis. In addition, a negative appendectomy (defined as removal of a normal appendix in a patient suspected of having acute appendicitis) is also associated with an increased risk of fetal loss.
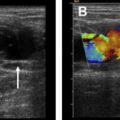
In centers with expertise, ultrasonography may be the first-line test to diagnose acute appendicitis in pregnant women because CT (the current first-line test in patients who are not pregnant) would expose the fetus to ionizing radiation. Ultrasonography is performed with graded compression, and a noncompressible blind-ending tubular structure that measures 7 mm or more in diameter is diagnostic of acute appendicitis ( Fig. 1 ). ,
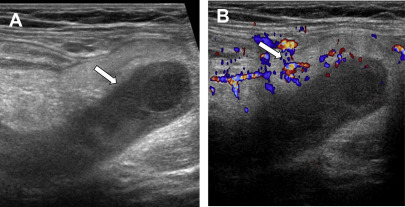
However, the appendix is not always identifiable with ultrasonography, and may not be identifiable in up to 97% of pregnant women during the second and third trimesters. However, if the appendix is visible and diagnostic criteria for acute appendicitis are met, the positive predictive value of ultrasonography is high (94%). However, the negative predictive value of ultrasonography is low (40%), and, if the appendix is not visualized with confidence, additional testing with noncontrast MR should be pursued.
MR is increasingly performed to evaluate pregnant women with suspected acute appendicitis either as the second-line test following inconclusive ultrasonography or as the first-line test. In a 2014 survey sent to the membership of the Association of University Radiologists, the Association of Program Directors in Radiology, and the Society of Radiologists in Ultrasound, 73% of respondents reported using MR imaging to evaluate for suspected acute appendicitis after an inconclusive ultrasonography scan in the first trimester and 67% in the third trimester, compared with 46% and 29% in a survey conducted in 2007.
T1-weighted and T2-weighted sequences are used to locate the appendix. Inflammatory changes are most conspicuous on T2-weighted images obtained with fat saturation ( Figs. 2 and 3 ). The accuracy of MR imaging for the diagnosis of acute appendicitis in pregnant women is 88% to 99% with 60% to 100% sensitivity, 92% to 100% specificity, 92% to 100% positive predictive value, and 94% to 100% negative predictive value.
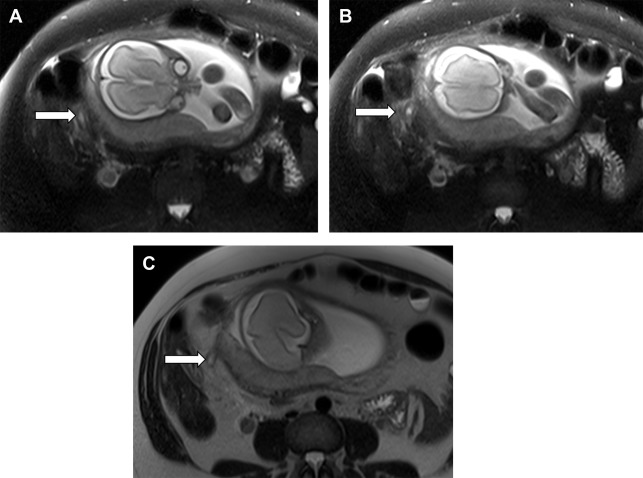
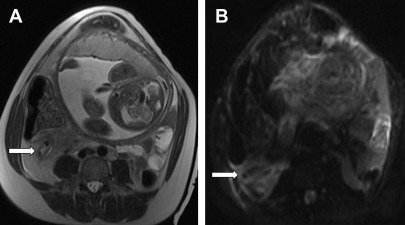
The appendix is visualized at MR in 60% to 76% of pregnant women with suspected acute appendicitis and may be more difficult to see in later stages of pregnancy. , In a series of 233 pregnant women with suspected appendicitis, a nonvisualized appendix or lack of inflammatory findings reliably excluded the diagnosis of acute appendicitis with high interradiologist agreement. In an evaluation of 58 pregnant women with suspected appendicitis, no patients with a nonvisualized appendix were ultimately diagnosed with acute appendicitis.
Alternative causes of abdominal pain are identifiable in 24% to 44% of MR examinations performed to assess for acute appendicitis, including hydronephrosis, degenerating fibroid, cholelithiasis, and pyelonephritis. , In an evaluation of 79 pregnant women of whom 31 underwent MR imaging and 34 had pathology-confirmed appendicitis, patients who underwent MR had shorter length of stay (33.7 vs 64.8 hours, P <.001) but clinical outcomes and hospital charges were not affected. MR was more cost-effective than CT imaging in a decision-analytical model analyzing preoperative imaging strategies for pregnant women in the second or third trimester of pregnancy after an indeterminate ultrasonography scan. The integration of MR imaging into the evaluation of pregnant women with suspected acute appendicitis resulted in a reduction of the negative laparotomy rate from 55% to 21% without a change in the perforation rate.
Cholelithiasis
Acute cholecystitis is the second most common indication for nonobstetric surgery in pregnant women. Gallstone formation is more common during pregnancy because of estrogen-related effects, including the formation of cholesterol-supersaturated bile and reduced gallbladder motility.
Ultrasonography is the first-line imaging test to evaluate for acute cholecystitis. Imaging findings of acute cholecystitis include gallbladder wall thickening (>3 mm), pericholecystic fluid, and a positive sonographic Murphy sign. In a meta-analysis, the sensitivity and specificity of ultrasonography for the diagnosis of acute cholecystitis were 88% and 80%, respectively. A pitfall is that gallbladder wall thickening can also be caused by chronic cholecystitis, liver disease, renal disease, and heart disease. Also, the sonographic Murphy sign may be unreliable if the patient has received pain medication before imaging.
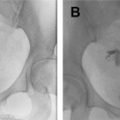
As a general rule, the bile duct normally measures up to 5 mm in diameter up to age 50 years, with an additional 1 mm in diameter increase considered normal per decade beyond age 50 years. A dilated bile duct may indicate a more distal gallstone within the duct or other obstructing lesion. MRCP is the preferred test to evaluate for choledocholithiasis, especially if not seen on ultrasonography. On MRCP, gallstones appear as rounded or angular geometric areas of low signal intensity ( Fig. 4 ). The sensitivity and specificity of MRCP for choledocholithiasis are 93% and 96%, respectively. Pitfalls include mistaking low signal intensity related to cholecystectomy clips in a slab MRCP image or flow-related artifact in thin-slice T2-weighted images for stricture or stones. Thin-cut MRCP images are helpful to localize stones, and steady-state images are helpful to confirm that an area of low signal intensity is a stone and not a flow void with low signal intensity.
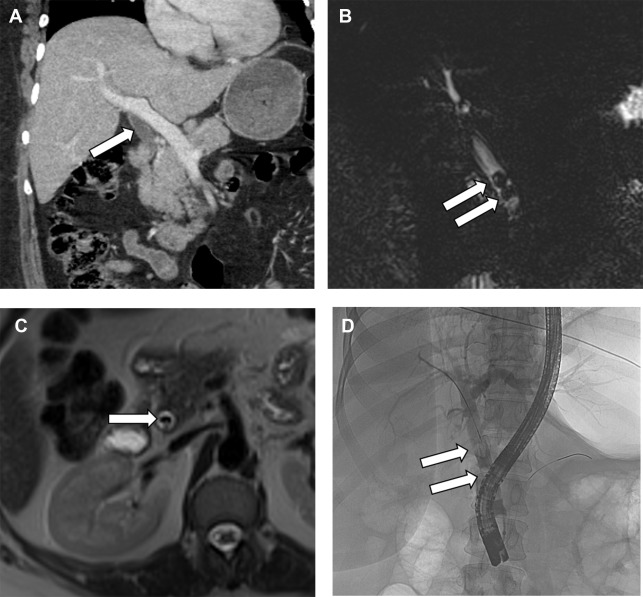
Endoscopic ultrasonography and endoscopic retrograde cholangiopancreatography (ERCP) and cholecystectomy can be safely performed in pregnant women. By comparison, conservative management of cholelithiasis and its complications is associated with frequent emergency department visits and recurrent biliary symptoms.
Small bowel obstruction
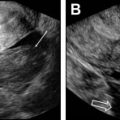
Although uncommon, the incidence of small bowel obstruction in pregnant women is increasing because of an increasing number of women of childbearing age undergoing bariatric surgical procedures and therefore being at increased risk for internal hernia or adhesive disease. , Adhesional disease (50%) is the most common cause of small bowel obstruction in pregnant women, followed by internal hernia (15%), intussusception (12%), and volvulus (9%). MR is the preferred modality to evaluate for small bowel obstruction in pregnant women because of its lack of ionizing radiation, superior soft tissue resolution, and multiplanar capabilities. Dilated bowel should be traced to the point where it transitions to decompressed bowel, and this transition zone should be carefully interrogated to determine the cause of the obstruction ( Fig. 5 ). In patients with adhesive disease, the culprit adhesion typically is not identifiable on imaging. However, once other causes of small bowel obstruction are ruled out in the transition zone (eg, hernia), adhesive disease may be assumed.
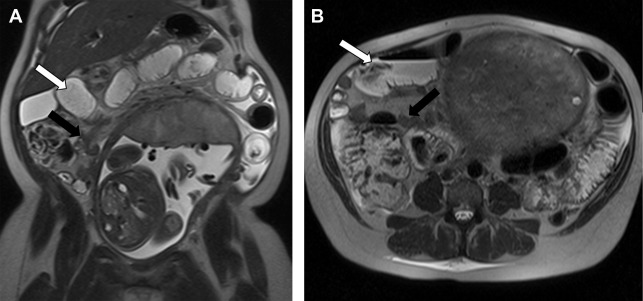
Internal hernias can be challenging to diagnose, and there is scant literature available on the appearance of internal hernias specifically in pregnant women. In the general population following Roux-en-Y gastric bypass, mesenteric swirling is the single best predictor of internal hernia (sensitivity, 61%–89%; specificity, 67%–94%). , However, some internal hernias are occult on imaging. Because internal hernia is the most common cause of small bowel obstruction following Roux-en-Y gastric bypass (42%), MR imaging showing a small bowel obstruction in a pregnant woman with prior gastric bypass should be interpreted with caution. A potential pitfall is the misattribution of bowel wall thickening to infection in the setting of an imaging-occult internal hernia with ischemic bowel. In addition, the distinction between a partial and complete obstruction is not readily made with MR because currently no oral contrast agent exists that is distinguishable enough from physiologic fluid to allow assessment of whether an oral contrast agent passes beyond the transition point.
Internal hernia is managed operatively because of the high risk of bowel ischemia, whereas a small bowel obstruction caused by adhesive disease may initially be managed conservatively (eg, bowel rest and nasogastric tube placement). In a recent series reviewing pregnant women with small bowel obstructions, most patients (91%) eventually underwent surgical intervention, and the rate of fetal loss was 17% with a maternal mortality of 2%.
Inflammatory bowel disease
Fertility rates of patients with inflammatory bowel disease in remission and who have never had prior pelvic surgery are similar to the general population. Patients with inflammatory bowel disease are advised to try to become pregnant while their disease is in remission because patients who become pregnant during a flare are more likely to experience poor fetal outcomes such as premature birth. Most patients who become pregnant while in remission remain in remission, whereas most patients who become pregnant experiencing active disease continue to have active disease during pregnancy. ,
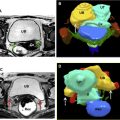
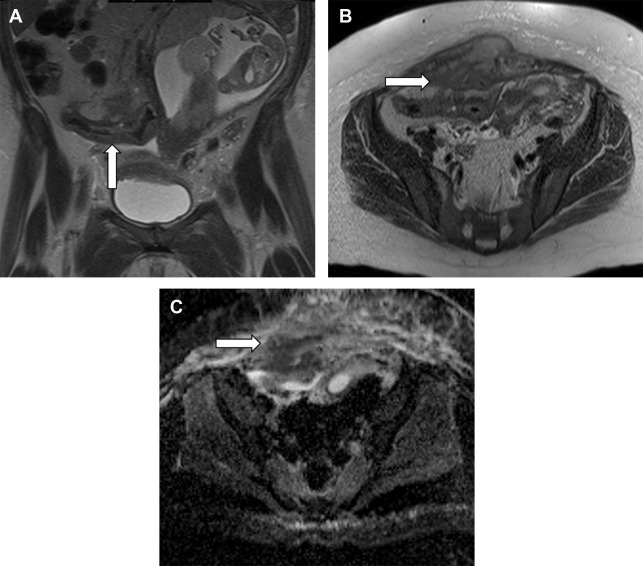
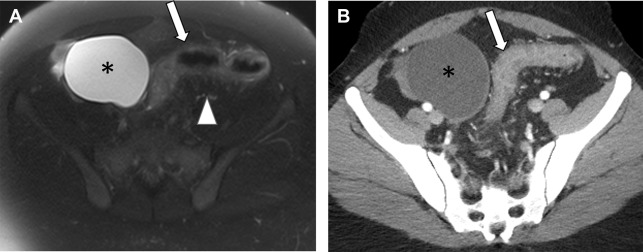
Noncontrast MR is the preferred modality to assess for active inflammatory bowel disease and its complications in pregnant patients. Active inflammatory bowel disease appears as areas of bowel wall thickening and edema, with edema most conspicuous on T2 images obtained with fat saturation ( Figs. 6 and 7 ). Diffusion-weighted imaging can be helpful. MR is also useful to assess for complications, including infected fluid collections, fistulae, and bowel obstruction. A pitfall of MR is that extraluminal air is less readily apparent compared with CT. Extraluminal air does not show signal in any pulse sequence. Assessment for extraluminal susceptibility artifacts that bloom on in-phase images may be helpful. In addition, direct demonstration of a bowel leak is typically not possible with MR imaging because there currently is not an oral contrast agent that is sufficiently distinguishable from intestinal contents to confirm a leak.

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree