ORAL CAVITY AND FLOOR OF THE MOUTH: BENIGN TUMORS
KEY POINTS
- Computed tomography and magnetic resonance imaging are valuable diagnostic tools for evaluation and planning the next steps in the diagnostic management of submucosal oral cavity masses that are eventually shown to be benign.
- Such imaging can help to avoid possible complications, such as excessive bleeding from endoscopic biopsy.
The pathophysiology of benign tumor growth and how it is expressed on imaging studies is discussed in detail in Chapters 21 and 22. Chapters 9 (for proliferative hemangioma), 25, 29, and 39 through 41 provide a more specific account of those growth patterns that are more tissue specific.
Most of the benign tumors discussed in this chapter are held in a common anatomic framework between the oral cavity, mandible and maxilla (especially with regard to odontogenic tumors), oropharynx, and submandibular and sublingual glands and spaces because these sources of tumors are so closely allied. This chapter will summarize both in illustrative and text material those disease tumors that have been discussed and illustrated more completely in previous chapters named in the opening paragraph and as follows:
- Mandibular and dental tumors (Chapters 99 and 100)
- Oropharyngeal tumors (Chapter 194)
- Submandibular gland and space tumors (Chapter 182)
- Sublingual gland and space tumors (Chapter 183)
Those chapters should be used as other sources of case material to round out the exposure to the tumors summarized in this chapter.
After physical examination, it may be difficult to decide whether an area of oral cavity swelling is neoplastic, inflammatory, traumatic, or degenerative. Even after biopsy, the etiology may remain obscure.
Many benign tumors or focal areas of swelling in the oral cavity will have a nonspecific imaging appearance. On occasion, imaging findings will be specific enough to allow an etiologic or sometimes a very likely specific tissue diagnosis. The most fitting and usual use of computed tomography (CT) and magnetic resonance imaging (MRI) is to show the extent of the lesion and to identify the likely etiology of a submucosal mass.
ANATOMIC AND DEVELOPMENTAL CONSIDERATIONS
Applied Anatomy
The critical anatomic knowledge necessary for the evaluation of oral cavity tumors is summarized here. The detailed anatomy of this region and the related oropharynx and related deep tissue spaces are reviewed in chapters indicated below in parentheses. A detailed working knowledge of all of this anatomy is necessary to evaluate images of patients with known or suspected oropharyngeal benign tumors if the evaluation of the image is expected to contribute measurably to medical decision making.
The general anatomic knowledge necessary to evaluate benign tumors of the oral cavity includes the following:
- Regional anatomy of the oral cavity, including the floor of the mouth, oral tongue, gingiva, and related deep spaces (Chapters 142 and 190)
- Related regional anatomy of the structures adjacent to the oral cavity, including the oropharynx (Chapter 190) and nasopharynx (Chapter 184)
- Bony anatomy, including the hard palate, pterygoid plates, mandible, and maxilla (Chapter 196)
- Neurovascular bundles, including the facial, lingual, and hypoglossal nerve and greater and lesser palatine and posterior superior alveolar neurovascular bundles
IMAGING APPROACH
Techniques and Relevant Aspects
Computed Tomography and Magnetic Resonance Imaging
Benign lesions of the oral cavity are studied with CT and MRI in essentially the same manner as the oral cavity cancers, except the neck may not be included. The specifics and relative value of using these studies in this anatomic region are reviewed in Chapter 196. Problem-driven protocols for CT and MRI are presented in Appendixes A and B. In general, MRI is more definitive than CT in the evaluation of submucosal oral cavity and deep space masses at this level of the suprahyoid neck since these images are usually of good quality above the hyoid.
Other
Ultrasound can be used to visualize well-demarcated soft tissue lesions in the oral part of the tongue and floor of the mouth. However, the effect on the airway and/or extension into neighboring spaces may be difficult or impossible to evaluate using this technique alone. Radionuclide studies have little or no diagnostic use for the evaluation of benign oral cavity masses, and the normal variations in this region seen on fluorine-18 2-fluoro-2-deoxy-D-glucose positron emission tomography (FDG-PET) studies significantly limit any potential value. Catheter angiography is used rarely when imaging suggests a primarily vascular mass and/or as a prelude to definitive or adjunctive endovascular management.
Pros and Cons
Evaluation of a Submucosal or Other Mass of Uncertain Etiology
Benign masses limited to the oral cavity often mimic the initial presentation of oral cavity cancer. Any mass, regardless of etiology, that is suspicious for deep infiltration or cancer should be studied primarily with CT if imaging is desired as part of the evaluation. MRI can be used initially if preferred, especially in young patients. Supplemental magnetic resonance (MR) study, in the situations where it might add meaningful incremental data, is best directed by CT findings to a localized area of interest where its strengths related to better soft tissue contrast resolution may be exploited.
Integrity of the Airway
In any imaging study of the oral cavity, the diseased condition must be evaluated for its effect or potential effects of diagnostic or therapeutic efforts on the airway. The anatomic status of the airway as well as the risk of any acute adverse complication, such as the potential for rapidly progressive airway obstruction either by the mass or a potential airway complication that might arise as a result of biopsy, should be reported. For instance, biopsy of an unanticipated vascular malformation could lead to an unfortunate amount of hemorrhage and aspiration of blood or rapid airway compromise.
Evaluation of Pharyngeal Dysfunction Possibly Due to Submucosal Masses
Some patients have processes predominantly occurring beneath intact oral cavity mucosa that cause interference with swallowing, chewing, and speech with no visible mass. Imaging is particularly valuable to the head and neck surgeon to detect or exclude a submucosal lesion that may spread underneath intact and normal-appearing mucosa causing such symptoms.
SPECIFIC DISEASE/CONDITION
Benign Tumors of the Oral Cavity
Etiology
Benign tumors of the oral cavity are rare and typically have no particular etiology. A neurogenic tumor might be associated with neurofibromatosis (Fig. 199.1).
Prevalence and Epidemiology
Minor salivary gland tumors (Fig. 199.2), rhabdomyomas (Fig. 199.3), leiomyomas, lipomas (Fig. 199.4), neurogenic tumors (Figs. 199.1 and 199.4), and those of fibrous origin (Fig. 199.5) are all very rare lesions that may present in the oral cavity. Sublingual and submandibular gland and space masses that may cause bulging of the oral cavity contours are discussed in Chapters 182 and 183.
Clinical Presentation
A benign oral cavity mass may produce problems with speech, chewing, and swallowing as the initial symptom. Sore throat, referred ear pain, and/or pain localized to the oral cavity region would suggest a malignant rather than benign tumor.
Physical examination is mainly done by direct inspection and palpation. The physical examination should establish whether there is a visible mucosal lesion. A bluish or reddish hue or abnormal vascularity may be noticed in hypervascular tumors (Fig. 199.6). Occasionally, there will be a palpable upper neck mass presenting near the angle of the mandible or in the submandibular space.
Pathophysiology and Patterns of Disease
These masses tend to grow as well-circumscribed spheroids displacing surrounding anatomic structures. They may cause remodeling of adjacent bone but should not appear frankly invasive of surrounding soft tissues or bone.
Vascular lesions may produce enlargement of the facial and lingual vascular pedicles.
Otherwise, the pathophysiology of benign tumor growth and how it is expressed on imaging studies is discussed in detail in the Chapters 21 and 22. Chapters 9 (for proliferative hemangioma), 25, 29, and 39 through 41 provide a more specific account of those growth patterns that are more tissue specific.
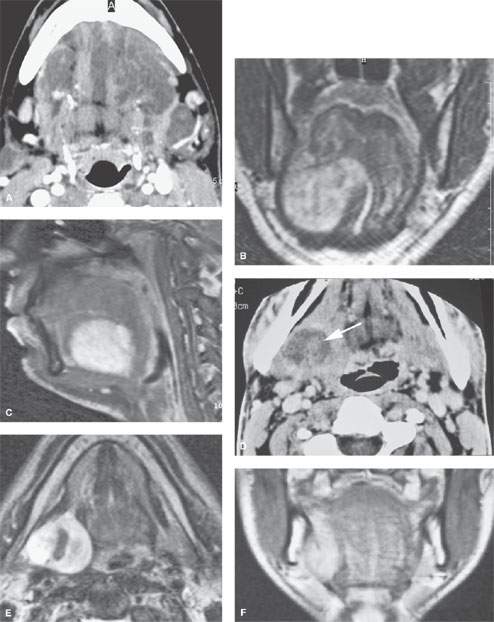
FIGURE 199.1. Three patients with neurogenic tumors presenting in and around the oral cavity. A: Patient 1. Contrast-enhanced computed tomography (CT) scan on a patient with multiple plexiform neurofibromas. B, C: Patient 2. A T2-weighted (T2W) coronal image and a contrast-enhanced T1-weighted (T1W) image of a neurofibroma on the floor of the mouth. D–F: Patient 3 presenting with a mass in the posterior aspect of the floor of the mouth and tongue base region. The CT study with contrast in (D) shows the mass with likely minimal enhancement. The T2W (E) and contrast-enhanced T1W (F), however, show an enhancement pattern and morphology consistent with the eventual tissue diagnosis of a schwannoma.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree