OMS = oral mucosal space; PMS = pharyngeal mucosal space; SLS = sublingual space; SMS = submandibular space; ROT = root of tongue; BOT = base of tongue (lingual tonsil); BMT = benign mixed tumor; SCCa = squamous cell carcinoma; NHL = non-Hodgkin lymphoma.
Approaches to Imaging Issues in the Oral Cavity
There are 3 main OC imaging indications: (1) Staging of primary SCCa and nodes, (2) searching for abscess and its cause, and (3) evaluating an SMS mass to determine if the mass is nodal or glandular. Knowing the clinical context can affect the type of exam (CECT vs. MR) and facilitate the creation of a highly relevant radiology report. Without clinical history, assigning a lesion to a space of origin (OMS, SLS, ROT, SMS) and comparing its radiologic features to those of the space-specific differential diagnoses is an alternative approach to analyzing OC images.
OMS SCCa is known at the time of imaging. The mucosal extent of the SCCa is best determined by the clinician. Imaging is critical to evaluate deep soft tissue extent, bone involvement, perineural tumor, and nodal spread. Small tumors may be extremely subtle or even occult to imaging, and for this reason it is very helpful to know the primary subsite when reading OMS SCCa scans. This allows careful evaluation for features that are key to surgical management, such as cortical bone erosion. Each OC primary SCCa subsite has its own set of imaging questions that should be considered at the time of primary tumor staging. Refer to the module on each of these primary sites in the SCCa content area to review these imaging questions.
When a lesion is found in the SLS, check to see if it has spread to the contralateral SLS via the connection anteriorly under the tongue frenulum. Also look to see if the lesion has spread posteriorly into the SMS.
SMS masses usually arise from either the submandibular gland or the submandibular nodal chain (level IA and IB). Making this distinction allows the imager to develop a differential diagnosis based on glandular disease or nodal disease. Note that a smaller submandibular gland tumor may be difficult to see on CECT. US or MR may be used in the cases where the clinician is certain a lesion is present and CECT is equivocal.
ROT lesions are rare. The differential diagnosis of ROT lesions is short, as can be seen by the global differential diagnosis table. If a lesion appears to bow the genioglossus muscles laterally away from each other, then it should be considered primary to the ROT.
Differential Diagnosis
When there is no history available and a lesion is found within the OC, assigning it a space of origin and reviewing that space-specific differential diagnosis can be a very useful strategy for evaluating the imaging exam findings. Review of the global differential diagnosis table provided here shows the space or spaces where the OC lesions are found. This global differential diagnosis can be subdivided into 4 distinct differential diagnoses lists based on the 4 major OC anatomic areas (OMS, SLS, SMS, and ROT).
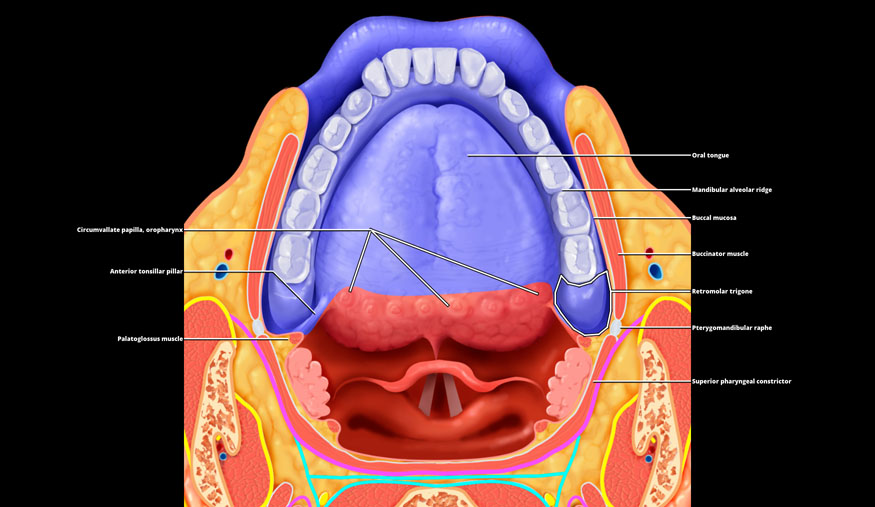
Anterior tonsillar pillar
Palatoglossus muscle
Oral tongue
Mandibular alveolar ridge
Buccal mucosa
Buccinator muscle
Retromolar trigone
Pterygomandibular raphe
Superior pharyngeal constrictor
Axial graphic shows oral mucosal space &/or surface (OMS) shaded in blue. Notice that the circumvallate papilla, a superficial line of taste buds, divides anterior oral cavity (OC) from posterior oropharynx. The lingual tonsil is part of oropharynx, not the OC. Four of the 6 squamous cell carcinoma (SCCa) subsites are labeled on the right, including the oral tongue, alveolar ridge, buccal mucosa, and retromolar trigone (RMT). The floor of mouth (FOM) and hard palate subsites are not shown. Note that the pterygomandibular raphe (PMR) connects the posterior margin of buccinator muscle to anterior margin of the superior pharyngeal constrictor muscle. The RMT represents a key route of perifascial spread of SCCa of the RMT.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree



