This article discusses the broad topic of thyroid cancer, with a focus on giving the reader an understanding of the basis for surgical decision making. The reader will gain an understanding of the embryology, anatomy, and various cancer pathologies than can affect the thyroid gland. The reader will also be exposed to clinical correlations that greatly assist in management of these cancers. Planning and rationale for various surgical procedures are also discussed.
According to several studies, the incidence of thyroid nodules is anywhere from 50% to 70% in the adult population, whereas the incidence of silent malignancy ranges between 3% and 5%. At the same time, the incidence of clinically evident thyroid cancers ranges from 0.5 to 10 cases per 100,000 people. Most of the patients who have cancer have well-differentiated cancers, with an excellent long-term prognosis. Some patients have well-differentiated cancers with a poor prognosis, and some have other less common types of thyroid cancers. The challenge for the clinician is to identify the patients who have cancers, to treat them according to the extent and aggressiveness of their disease, and to limit morbidity and mortality as much as possible.
Etiology of thyroid cancer
An increase in the incidence of thyroid cancer has been associated with exposure to ionizing radiation. This association has been demonstrated most profoundly in the Ukraine, after the Chernobyl nuclear reactor disaster in 1986. Ongoing studies from this region have shown an increased incidence of thyroid nodules and cancer in these populations, with a 7 to 15 year latency in general.
An increased risk for thyroid carcinoma among women suggests a possible role for hormones in increasing the risk, but no such link has been definitely identified. Studies have also investigated the role of radioactivity from I131 in increasing the risk for thyroid cancer, but to date have concluded that it does not increase the risk. Countries with iodine deficiency have a higher incidence of follicular thyroid cancers compared with non–iodine-deficient countries, but the cause is unclear.
There are certain genetic syndromes that increase the risk for thyroid cancer, or are associated with thyroid cancer, especially medullary thyroid cancer, which has been linked to several specific genetic abnormalities. In some cases, papillary thyroid cancer follows a familial pattern also. Several rare genetic disorders, including Cowden disease, multiple endocrine neoplasia (MEN), and Gardner syndrome, are also associated with a higher incidence of thyroid cancer.
Epidemiology of thyroid cancer
Over the last several decades, the incidence of thyroid cancer has increased dramatically. It is unclear if this increased incidence is real or if it may be attributable to more sensitive diagnostic techniques. Autopsy studies have shown that up to 30% of adults have incidental cancers smaller than 1cm at the time of death. This finding may imply that our more sensitive methods of detecting cancers may not affect overall prognosis. According to the SEER database, there are approximately 37,340 people who will be diagnosed with thyroid cancer in the United States in 2008. Approximately 1530 people will die of thyroid cancer during the same year. The average age of diagnosis is 47 years, and the average age of death is 74 years. (NCI SEER Cancer Statistics Review).
The most common type of thyroid cancer is papillary thyroid cancer (PTC). It represents approximately 70% of thyroid cancers. Follicular thyroid carcinoma (FTC) represents approximately 15% of cancers and in combination with PTC composes the category of well-differentiated thyroid carcinomas (WDTC). Grouped into the less common cancers are medullary (4%–6%), anaplastic (3%–4%), and others (up to 5%). This group may include lymphoma, sarcoma, squamous cell carcinoma, and metastases.
Epidemiology of thyroid cancer
Over the last several decades, the incidence of thyroid cancer has increased dramatically. It is unclear if this increased incidence is real or if it may be attributable to more sensitive diagnostic techniques. Autopsy studies have shown that up to 30% of adults have incidental cancers smaller than 1cm at the time of death. This finding may imply that our more sensitive methods of detecting cancers may not affect overall prognosis. According to the SEER database, there are approximately 37,340 people who will be diagnosed with thyroid cancer in the United States in 2008. Approximately 1530 people will die of thyroid cancer during the same year. The average age of diagnosis is 47 years, and the average age of death is 74 years. (NCI SEER Cancer Statistics Review).
The most common type of thyroid cancer is papillary thyroid cancer (PTC). It represents approximately 70% of thyroid cancers. Follicular thyroid carcinoma (FTC) represents approximately 15% of cancers and in combination with PTC composes the category of well-differentiated thyroid carcinomas (WDTC). Grouped into the less common cancers are medullary (4%–6%), anaplastic (3%–4%), and others (up to 5%). This group may include lymphoma, sarcoma, squamous cell carcinoma, and metastases.
Embryology of the thyroid gland
The thyroid gland has two separate sites of origin embryologically. Most of the gland is derived from endodermal anlage of the primitive gastrointestinal tract. The parafollicular, or C cells, are derived from the ectodermal neural crest. The thyroid descends from the region of the foramen cecum to rest in its normal anatomic position, just beneath the cricoid and along the anterior and lateral surfaces of the upper trachea.
Understanding the embryology of the thyroid gives an appreciation of the many abnormalities that can be seen in children and adults when the migration of the thyroid is incomplete. As the thyroid descends, it normally loses its attachment to the tongue at the foramen cecum when the thyroglossal duct fibroses. The thyroglossal duct may remain patent and remain lined with a ciliated pseudostratified epithelium. This phenomenon can lead to the midline thyroglossal duct cyst, which can be located anywhere between the normal anatomic location of the thyroid and the base of the tongue.
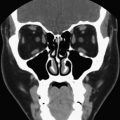
The descent of the thyroid into its normal anatomic position is profoundly affected by the heart, and as such, aberrant thyroid tissue can be found in many locations in the neck and mediastinum. Locations, including the esophagus, the larynx, the trachea, the lateral cervical lymph nodes, the pericardium, the aortic arch, and the base of tongue, have been well documented. A lingual (base of tongue) location of the thyroid may represent the only undescended thyroid tissue in the body ( Fig. 1 ).
Anatomy of the thyroid gland
The thyroid consists of two lateral lobes, an isthmus, and, in about one third of patients, a pyramidal lobe. The average gland weighs between 15 and 25 g. The gland sits over the midline of the trachea, and is attached to the cricoid and tracheal wall by a ligament of Berry, which represents condensations of the deep cervical and pretracheal fascia. The inferior border of the gland varies in location, but can be below or above the sternal notch.
The arterial supply to the gland is derived from two separate paired vessels. The inferior thyroid vessels come directly off of the thyrocervical trunk and enter the thyroid at approximately the midsection of the lateral lobe. They tend to supply both the superior and the inferior parathyroids. The superior thyroid arteries come off the carotid, usually as the first branch of the external carotid, but sometimes off the common carotid. Rarely, a small artery or pair of arteries may come directly from the aorta or brachiocephalic trunk, named the thyroid ima.
There are three main paired veins that drain the thyroid. There is some variability in location and presence, but they generally drain into the internal jugular veins and innominate vein.
The lymphatics of the thyroid consist of intraglandular and extraglandular components. Extraglandular lymphatics generally follow venous flow. The inferior portions of the lateral lobes drain along the tracheoesophageal groove into the central neck. The superior parts of the lobes drain toward the superior thyroid veins, and the isthmus may drain toward the delphian (prelaryngeal) lymph node or central neck nodes. More unusual, but clearly documented, are lymphatic pathways to the retropharyngeal region, accounting for metastases to the skull base. Based on clinical and anatomic review, the central lymphatics are generally considered the primary drainage pathways for thyroid cancers, with the lateral neck nodes being considered secondary levels of lymphatic spread. These facts are important from an imaging and a treatment perspective.
Two sets of nerves are intimately associated with the thyroid gland: the superior and the recurrent laryngeal nerves. They are branches of the 10th (vagus) cranial nerve. The recurrent laryngeal nerves have slightly different courses as they enter the larynx just under the thyroid gland. On the left, the nerve courses into the chest, around the aortic arch, and back up into the larynx. On the right, the nerve passes around the subclavian artery to course back up into the neck and into the larynx. Rarely, patients present with nonrecurrent laryngeal nerves. This presentation usually occurs on the right side, and is often associated with a retroesophageal subclavian artery. In rare cases of transposition of the great vessels, a left nonrecurrent nerve has been identified.
The parathyroid glands are also closely related to the thyroid anatomically. They tend to lie on the undersurface of the thyroid, and receive their blood supply from the inferior thyroid artery. Their anatomy is discussed in detail in another article in this issue.
Anatomy of the neck
The relevant anatomy of the neck for the thyroid surgeon and head and neck radiologist includes the entire anterior neck, from one trapezius muscle to the other, and from the base of skull to the mediastinum. Most important are the various lymphatic compartments of the neck, which have conventionally been divided into numbered compartments to aid in standardizing locations ( Fig. 2 ). The lymphatics of the neck are divided into seven compartments. Level I includes the submental and submandibular nodes. They are located above the anterior and posterior bellies of the digastric muscle, which insert on the hyoid bone. This level is subdivided into level IA (submental), which is anterior to the digastric muscle, and level IB (submandibular), which is behind the digastric. Levels II, II, and IV are all deep to the sternocleidomastoid muscle (SCM). The anterior and posterior border of all of these lymphatic groups is the anterior and posterior border of the SCM. Level II is the upper jugulodigastric group of nodes. Its superior boundary is the skull base, and its inferior boundary is at the level of the hyoid. It is subdivided by the 11th cranial nerve into an anterior (level IIA) and posterior (level IIB) compartment. Level III is the middle jugular nodal basin. Its inferior boundary is at the level of the cricoid. Level IV is the inferior jugular nodal basin. Its inferior boundary is the clavicle. Level V is the posterior triangle group of nodes. It lies between the posterior border of the SCM and the anterior border of the trapezius. Level VI is the anterior compartment, or central neck nodal basin. It is bordered laterally on both sides by the carotid sheath, superiorly by the hyoid, and inferiorly by the sternal notch. It is sometimes divided into the pretracheal (anterior to the trachea) and paratracheal (lateral to the trachea) compartments. Finally, Level VII is the anterior mediastinal compartment of nodes. It remains between the carotids, from the sternal notch to the level of the aortic arch, in the superior mediastinum.
Dissecting the lymph nodes to remove cancer or suspected cancer from patients who have thyroid abnormalities remains a mainstay in therapy. Determining which levels of the neck to dissect is greatly aided in many cases by the results of radiologic studies and understanding of the patterns of nodal metastasis. In cases of suspected pathologic adenopathy, it is helpful to include specific descriptors of a node’s location. This description includes the anatomic level of the node and the relationship of the node to surrounding structures, such as the bifurcation of the carotid artery and the hyoid bone. Especially in cases of suspected cancer recurrence, this additional information is critical.
The pattern of spread of thyroid cancer to the lymph nodes is well documented. Initially, most thyroid cancers metastasize to the central compartment nodes (level VI). Several sentinel node studies have shown that in patients who have metastases, more than 80% are in the central neck. Unfortunately, thyroid cancer often demonstrates “skip” metastases, making it hard to predict which levels of the neck will have metastatic nodes. In large series, the lateral neck nodes are involved to varying degrees. Most commonly involved is level IV, followed by levels III, V, II, and I. Level I nodal metastases are rare from thyroid cancer.
Contralateral metastases are most common in larger tumors, tumors that cross the midline, and recurrent cancers. The most commonly involved contralateral compartment is the paratracheal region. When this is positive, the risk for metastases to the lateral neck is higher.
There is significant controversy regarding if and when to dissect the lymph nodes in the neck, especially in necks without evidence of disease in the pretreatment setting. For this reason, it is especially important to thoroughly evaluate the thyroid itself and the central neck (as much as possible) and lateral neck in patients who have known or suspected thyroid cancers. Nodal metastasis, although common in thyroid cancer, has little prognostic implication in well-differentiated thyroid cancer.
Staging of thyroid cancer
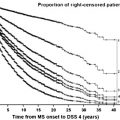
As with all cancers, staging systems for thyroid cancer not only help clarify and standardize reporting of these cancers but also attempt to predict prognosis and outcome. Several staging systems have been developed over time, using various factors to help stratify patients into higher and lower risk categories. One of the most widely accepted systems is the TNM staging. The T stage refers to the largest extent of tumor in the thyroid itself, the N to size and location of lymph nodes in the neck, and the M to the presence or absence of distant metastasis. Most staging systems, including the TNM, account for patient age in their determination of final stage, because of large studies that have shown the profound effect that age has on prognosis. The TNM staging has a cutoff of 45 years of age. Patients younger than age 45 who have any T stage and any N stage are still stage I, and even distant metastasis only places them in stage II. Older patients tend to have a poorer prognosis ( Fig. 3 ). This staging system generally refers to WDTC only. Medullary, anaplastic, and other less common cancers are not accounted for in this staging.
Pathology of thyroid cancer
Papillary Thyroid Cancer
Papillary thyroid cancer is the most common of thyroid cancers, but the true incidence is unknown, partly because of the often indolent nature of this cancer and because it often presents incidentally during workup or surgery for another diagnosis, or at the time of autopsy. Most patients diagnosed and treated for this cancer are either cured of the disease or live for many years after the diagnosis. Less than 50% of recurrences occur within the first 5 years, and it is not unusual for recurrences to present several decades after the initial diagnosis.
Pathologically, this cancer resembles the cell from which it is derived, the follicular cell. It often retains the ability to concentrate iodine, secrete thyroglobulin, and even produce thyroid hormone. It often retains its ability to respond to thyrotropin (TSH) stimulation. Grossly, these tumors are poorly encapsulated, firm, and often have calcifications (psammoma bodies) within their substance. The presence of these calcifications is of diagnostic significance, because they are rarely present in other thyroid pathologies. These tumors, especially larger ones, may contain focal areas of hemorrhage and necrosis. PTC demonstrates papillary fronds along with follicular components. The nuclei have a characteristic appearance, with a feature described as “Orphan-Annie eyes” used to refer to the relatively empty appearance of the nucleoplasm.
Histologically, there are several variants of papillary thyroid carcinoma. Follicular variant of papillary thyroid carcinoma has a pattern of neoplastic follicles that are small with little colloid. They contain relatively fewer nuclear inclusions and psammoma bodies. The prognosis and biologic behavior is similar to that of papillary thyroid cancer. The tall cell variant of papillary thyroid carcinoma has neoplastic cells in which the height is twice the width. It is associated with more aggressive biologic characteristics and tends to metastasize earlier in its course. Overall, the prognosis is poor compared with classic papillary thyroid carcinoma.
It is common for PTC to demonstrate multifocal disease within the thyroid gland at the time of histologic examination. The incidence has been reported to be as high as 80% in the literature. This fact has led to recommendations by many authors to consider total thyroidectomy at the time of initial presentation. They cite an incidence of recurrence of 5% to 20% in patients who have partial thyroid surgery. Other authors, however, have demonstrated that locoregional recurrence does not affect long-term survival, and thus they advocate less aggressive surgery to minimize morbidity in select patients.
Extrathyroidal extension of the tumor has demonstrated prognostic significance, and thus helps determine extent of surgical and medical treatment. Although the overlying strap muscles in the neck are the most commonly invaded structures, there are many cases of tracheal, laryngeal, esophageal, and other soft tissue extensions in the neck.
Regional metastasis to the neck and mediastinal lymph nodes is common for PTC. The published incidence varies from 40% to more than 75%, if one includes subclinical metastases Abundant literature has investigated the role that regional metastasis has on prognosis, and there is no consensus. Although some studies have demonstrated a poorer prognosis for elderly patients who have nodal metastasis, several studies have demonstrated that neck metastases do not adversely affect long-term survival or prognosis. A few have demonstrated that nodal metastasis improves prognosis, and still others suggest that the more nodes with metastasis, the better the prognosis.
Age has proved to have prognostic significance in PTC and in other thyroid cancers. In general, younger age is associated with an improved prognosis.
Unlike regional metastasis, distant metastasis does seem to adversely affect prognosis. Approximately 10% of patients demonstrate metastasis to distant sites. Most commonly this involves the lungs, but the central nervous system and bones are common sites also. Studies have demonstrated that the volume of disease seems to affect prognosis, and macrometastases have been associated with almost a 50% 1-year rate of death.
Follicular Thyroid Carcinoma
Follicular thyroid carcinoma (FTC) is the second most common type of thyroid cancer. It represents about 15% of thyroid cancers. Many authors have suggested that the prognosis is slightly poorer than that for papillary thyroid cancer, but others suggest that when matched for age and stage, the prognosis is similar. They contend that the differences in overall survival represent presentation of follicular cancers at later stages and in older patients in general. Grossly, on examination, these tumors are thickly encapsulated with focal necrosis and cystic changes. The cells are small and monotonous. Psammoma bodies are rare, and the cells are organized into follicles that contain sparse colloid.
Both benign and malignant follicular lesions demonstrate follicular cells arranged in microfollicles, rosettes, or spindles, and thus they cannot be differentiated on fine needle aspiration. Capsular invasion is the only current method of distinguishing between the two. Because this can only be done once the entire capsule of the tumor has been evaluated histologically (unless gross invasion is visible before removal of the tumor), it is not uncommon for this diagnosis to be made after surgery.
Like PTC, FTC portends overall a good prognosis. In patients who have minimal capsular invasion, the prognosis is excellent, and few patients develop distant metastases or die of disease. In patients who have capsular or vascular invasion, however, the prognosis is much worse. Similar to PTC, patients who have FTC do better at younger ages, and women may have a slightly better prognosis than men.
Clinically, follicular carcinomas tend to present with solitary thyroid mass. The incidence of multicentric disease within the thyroid is much lower than with PTC. Although the rate of regional lymphatic metastasis is low, presence of lymph nodes positive for follicular carcinoma is a poor prognostic indicator. The rate of local invasion into trachea, pharynx, and so forth, is higher in patients who have nodal metastases.
Distant metastases are more common with FTC than with PTC. They tend to spread primarily to bone, and may present with pathologic fractures. These cancers also tend to spread to lung, liver, and brain. The prognosis is poor for patients who have distant metastasis.
Hürthle Cell Carcinoma
Hürthle cell carcinoma is a variant of follicular carcinoma. It accounts for 3% to 5% of thyroid cancers. It is composed of large acidophilic or oncocytic cells and does not generally take up radioiodine as well as classic follicular cancers. Like follicular carcinomas, the diagnosis can only be made after examination of the entire tumor capsule. The cancers generally have a slightly worse prognosis than other follicular carcinomas. They are associated with a higher rate of lymph node and distant metastasis than other follicular carcinomas.
Insular Thyroid Carcinoma
Although this cancer is listed as a variant of follicular thyroid carcinoma by the World Health Organization, it does not have many of the features associated with follicular or papillary thyroid cancers. Rare follicular structures are seen, and the cells may be arranged in trabeculae of cells surrounded by connective tissue. Sometimes referred to as poorly differentiated carcinoma, this lesion has a poorer overall prognosis than other well-differentiated thyroid cancers. It is rare, and in limited studies it has demonstrated a 10-year mortality rate of 10% to 46%.
Medullary Thyroid Carcinoma
Medullary thyroid carcinoma is unique among thyroid cancers in that it is derived from the parafollicular or C cells, which are a part of the amine precursor uptake and decarboxylation (APUD) cell system. These cells produce calcitonin and are unrelated to the iodine concentrating and thyroid hormone production of the gland. They are more closely related to other tumors of the neuroendocrine system, including carcinoid tumors and pheochromocytomas.
MTC is rare, and accounts for 3% to 5% of thyroid cancers. It comes in two forms, familial and sporadic. The familial form, which is less common than the sporadic form of MTC, is inherited as an autosomal dominant trait. It can be inherited as a part of three distinct entities. The most common, multiple endocrine neoplasia 2A (MEN2A), is associated with pheochromocytoma and hyperparathyroidism. The second most common, MEN2B, is associated with pheochromocytoma, mucosal neuromas, and marfanoid body habitus. The least common, familial medullary thyroid cancer (FMTC), consists of medullary thyroid cancer only.
The presence of MTC has been strongly linked to the RET oncogene, located on chromosome 10. Different mutations to this gene have been demonstrated, and have variable effects on activating the RET tyrosine kinase. The discovery of this gene mutation has been studied extensively, and has had a significant effect on diagnosis, management, and our understanding of MTC. RET mutation is important to evaluate family members and consider prophylactic total thyroidectomy.
Grossly, medullary thyroid cancer is often well encapsulated. Histologically, the tumors demonstrate amyloid depositions in 60% to 80% of cases, which is helpful in making the diagnosis. The tumors often display nuclear pleomorphism, necrosis, and multiple mitosis. Calcitonin staining is also helpful, and the level of staining may reflect level of cellular differentiation. Serum calcitonin levels are useful as a diagnostic and measure of response to therapy.
Medullary thyroid cancers, as a part of the APUD system, have been reported to secrete multiple polypeptide hormones besides calcitonin. Adrenocorticotropic hormone, somatostatin, vasoactive intestinal peptide, chromogranin A, neuron-specific enolase, and substance P have all been demonstrated. Carcinoembryonic antigen is also secreted by many MTCs, and has been used as a tumor marker and a receptor for nuclear imaging with octreotide imaging.
Clinically, patients tend to present with a solitary thyroid nodule, although initial presentation with a neck mass is not uncommon. Rarely, patients present with signs of local invasion, including hoarseness or dysphagia. Because of the secretory nature of these tumors, patients may present with paraneoplastic syndromes, such as Cushing or carcinoid syndrome.
Anaplastic Thyroid Cancer
Anaplastic thyroid cancer is an aggressive disease, usually proving fatal within several weeks to months of diagnosis. It represents about 3% to 5% of thyroid cancers. Pathologically, the tumor consists of grossly infiltrating tumor with areas of necrosis and hemorrhage. It often has a grey/white color and may be calcified and fibrotic. Tumors generally have high mitotic rates, marked cellular pleomorphism, necrosis, vascular invasion, and tumor emboli. It may be difficult, on fine needle aspiration, to distinguish from lymphoma or other poorly differentiated thyroid cancers.
This cancer tends to affect elderly patients, and the peak incidence is in the seventh decade. Several studies have shown that most patients who have this cancer have had goiter or other thyroid lesions for many years before the diagnosis of anaplastic cancer. This finding leads investigators to believe that anaplastic carcinoma may represent a dedifferentiation of well-differentiated cancers.
Clinically, patients present with rapidly growing neck mass, often in the context of a slow-growing mass or goiter for several decades. Patients often present with dysphagia, dyspnea, hoarseness, sore throat, and neck pain. These are all related to the aggressive nature of the disease. Physical examination demonstrates a large, irregular neck mass, often fixed to the surrounding structures. Patients may have tracheal and esophageal involvement, and unilateral or bilateral vocal fold paralysis is not rare. Patients may demonstrate cervical metastasis. Distant metastasis tends to be to the lungs, although other sites, including bone, brain, and mediastinum, have been demonstrated.
Lymphoma of the Thyroid Gland
Lymphoma of the thyroid has been reported to make up 2% to 5% of thyroid cancers. It tends to be non-Hodgkin B-cell type, although other types do occur. Patients who have a diagnosis of Hashimoto disease (chronic lymphocytic thyroiditis) have a 70-fold increased incidence of thyroid lymphoma compared with the general population. It is suspected that chronic autoimmune stimulation is responsible for the development of this cancer, much the same as Sjögren disease increases the risk for lymphoma in the salivary glands. Diagnosis of lymphoma in the thyroid gland requires a workup to confirm the lack of other sites of lymphoma in the body, because up to 15% of systemic lymphomas involve the thyroid gland.
Many lymphomas can be diagnosed cytologically, based on their monoclonality. Differentiating them from anaplastic carcinoma is often challenging, however, and it is not uncommon to require core or open biopsy to make an accurate diagnosis.
In the clinical setting, lymphoma also mirrors anaplastic carcinoma in many ways. It tends to present with a rapidly expanding mass in the neck, often fixed to surrounding structures. Patients often have neck pain, hoarseness, dysphagia, and even facial edema. The tumor is often fixed to surrounding structures, including the trachea and larynx, the esophagus, and the skin.
Other Cancers of the Thyroid
Although rare, several other cancers can involve the thyroid, either primarily or through metastasis. Squamous cell carcinoma is a rare primary cancer of the thyroid. Once diagnosed, a thorough workup must be performed to rule out a head and neck primary that has merely metastasized to the thyroid.
Metastatic cancer to the thyroid is also rare, although well documented. It is suspected that the significant vascularity of the gland accounts for these metastases. Cancers of the kidney, lung, breast, and melanoma are the most commonly documented. In patients who have a known history of other primary cancers who have a new thyroid mass, the possibility of metastatic disease must be entertained.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree