▪
Introduction
Thoracic interventions are performed for the diagnosis and treatment of focal lesions in the thorax. Image-guided percutaneous biopsy is used to obtain tissue for the diagnosis of benign and malignant conditions. Drainage of fluid or air from the pleural space or mediastinum can aid both diagnosis and therapy, and ablative therapies treat primary or secondary malignancy in lungs and chest wall.
▪
Lung and Mediastinal Needle Biopsy
Technical Principles
Tissue from a lesion in lung or mediastinum can be obtained percutaneously using CT guidance. A coaxial technique allows multiple biopsies to be performed with only one pleural puncture, thereby limiting complications. A 19-gauge introducer needle, in combination with a 22-gauge needle for aspirates, and a 20-gauge automatic, spring-loaded core needle provide adequate tissue for lung biopsies, but a larger gauge needle such as a 17-gauge introducer is advised for mediastinal biopsies, especially if lymphoma is suspected. Whenever possible, moderate sedation should be used because it will minimize respiratory motion and maximize patient comfort and immobility, without the need for breathing instructions. If the patient is cooperative, these biopsies can also be performed using local anesthesia only.
Indications and Contraindications for Lung and Mediastinal Biopsy
Indications for biopsy include establishing a diagnosis of infection and neoplasm and enabling the referring physician to determine the optimum management of a lesion.
In a nonoperative patient, biopsy can be performed to justify radiotherapy or demonstrate the feasibility of image-guided thermal ablation. In cases of known lung cancer, tissue analysis allows molecular testing for targeted chemotherapy and identification of mechanisms for resistance to targeted therapy. Mediastinal lesions can be biopsied to differentiate a thymic epithelial neoplasm from lymphoma because the latter requires chemotherapy rather than resection. Lung biopsy can also be performed to confirm a benign process, such as a hamartoma, and therefore save the patient from a surgical resection.
Severe cardiorespiratory compromise, uncorrectable coagulopathy, and an uncooperative patient are absolute contraindications. Relative contraindications include pulmonary hypertension with a right ventricular systolic pressure >50 mm Hg, prior pneumonectomy, severe emphysema, or interstitial lung disease with a forced expiratory volume in 1 second (FEV 1 ) <35% predicted. Patients on continuous positive airway pressure (CPAP) therapy for obstructive sleep apnea can undergo lung biopsy if they are able to manage without their CPAP machine and maintain adequate ventilation during the procedure and for 24 hours afterward.
Determining Which Patients Would Benefit From Alternative Means of Obtaining Tissue Rather Than Lung Biopsy
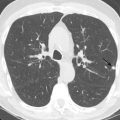
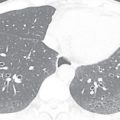
In patients with suspected lung cancer and extrapulmonary findings, the lesion that would result in the highest stage should be biopsied. Such lesions include masses in the adrenal glands and liver and mediastinal lymphadenopathy. For centrally located lung masses, endobronchial ultrasound or bronchoscopy is recommended. Navigational bronchoscopy can be used to sample more peripheral lung lesions, especially in emphysematous patients. In high-risk patients such as those with severe emphysema and a highly suspicious lung lesion, definitive therapy such as radiotherapy can be considered, even without tissue confirmation. Interval growth between CT scans and fluorodeoxyglucose (FDG) uptake is helpful in determining the probable cause. If infection is suspected, the patient is best served by a short-interval follow-up CT ( Fig. 42.1 ) after empiric treatment for community-acquired pneumonia.

Diagnosis of diffuse lung disease is best established with video-assisted thoracoscopic surgery wedge resection because limited tissue from a percutaneous needle biopsy is usually not adequate.
How to Determine if Biopsy Is Technically Feasible
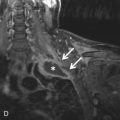
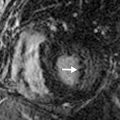
Needle biopsy of a mediastinal lesion is technically feasible if a needle can be directed into the lesion without causing injury to adjacent critical structures, particularly the internal mammary arteries, aorta, and heart. A parasternal approach with the needle directed away from the heart and aorta is usually safe ( Fig. 42.2 ).

The feasibility of lung biopsy depends on lesion size, location, and any concurrent lung disease, such as emphysema and interstitial lung disease. As a general rule, lesions larger than 1 cm are amenable to CT-guided needle biopsy. However, if a nodule lies in a particular location, such as the lung bases, respiratory motion may preclude successful biopsy. This explains why a small nodule located in the apex or superior segment of a lower lobe is easier to biopsy than if the same lesion were located at the lung base. A central lesion may not be accessible because of intervening vessels, airways, and fissures.
Preprocedure Checks Required for a Lung or Mediastinal Biopsy
Medications, platelet count, and coagulation parameters need to be reviewed to assess bleeding risk. Although low-dose aspirin is permissible, patients would ideally have stopped all anticoagulation in time for the effects to wear off at the time of biopsy. Specialty society recommendations include lung biopsy among procedures with moderate bleeding risk, for which a platelet count >50,000/µL is sufficient, but we prefer to biopsy patients with a platelet count >100,000/µL. The previous medical history needs to be reviewed for relative contraindications to moderate sedation, such as left ventricular ejection fraction <30%, recent myocardial infarction, or severe stenosis of the aortic valve or carotid arteries. Renal or liver failure would be another reason to consider not using moderate sedation. If moderate sedation is used, the patient needs to have had nothing by mouth for at least 8 hours and have an escort to accompany him or her home after the procedure. While obtaining informed, written consent, the operator should check whether somebody is available to stay with the patient overnight after the procedure in case a delayed pneumothorax develops.
How a Lung Biopsy Is Performed
The patient should be positioned comfortably on the CT table, and sedation should be started. A grid with radiopaque markers is positioned on the patient’s skin. Preliminary CT images are obtained with quiet respiration to assess for a clear path between the skin and the biopsy target ( Fig. 42.3 ).

Gantry angulation may be necessary to demonstrate a clear path between the skin and target. Angling the gantry may also be helpful to access an upper lobe nodule located just anterior to the fissure through a more superior intercostal interspace. Sagittal and coronal reformats can be helpful in conceptualizing how this maneuver could move ribs, fissures, and large vessels out of the biopsy path ( Fig. 42.4 ).

The skin overlying the target is then cleaned, and a sterile field is set up. Local anesthesia is administered to the skin with a 25-gauge needle, and the needle is left in place. Repeat imaging is performed to assess whether the skin entry site marked by the lidocaine needle can be lined up with the target and the distance between skin and pleura and skin to target lesion ( Fig. 42.5 ).

Local anesthesia is administered in the thoracic soft tissues. Subsequently, the introducer needle is advanced in parallel to the CT gantry. Care is taken to advance less than the distance from skin to pleura to avoid a pneumothorax ( Fig. 42.6 ). Repeat imaging is performed, as necessary, to check for alignment of the needle with the imaging plane and to measure the residual distance from the needle tip to pleura. If the introducer is no longer in plane, one can adjust either the orientation of the needle or the gantry angulation to achieve alignment of the introducer and target in chest wall soft tissues. It is key to align the introducer and target in chest wall soft tissues prior to puncturing the pleura. Injecting 1% lidocaine through the introducer needle once the tip is close to the parietal pleura anesthetizes this sensitive structure prior to the puncture.

Pleural puncture should only be done once the alignment between introducer and target in chest wall soft tissues has been confirmed to avoid having to pull out of the lung and risk additional pleural punctures. Deliberate advancement of the introducer by 2 to 3 cm will puncture the pleura ( Fig. 42.7 ). One may feel the pleura give way with a subtle pop.

The introducer is advanced incrementally into the lesion. Fine-needle aspirates are obtained while taking care not to advance the fine needle beyond the distal edge of the lesion. Filling the coaxial needle with saline will potentially protect against the risk of air embolism during needle exchanges. Repeat imaging should be performed to assess for complications such as pneumothorax, significant bleeding, and air embolus and confirm needle position. A small amount of blood products around the biopsy target can be expected ( Fig. 42.8 ).

Maximizing the Yield of Lung and Mediastinal Biopsy
Prior to the procedure, the most recent contrast-enhanced CT and/or positron emission tomography (PET)-CT examinations should be reviewed. Enhancement and/or FDG avidity indicate high-yield areas that should be targeted first. If the biopsy target is cystic, cavitary, or necrotic, viable cells are more likely present in the wall of the lesion than in the center ( Fig. 42.9 ). A trajectory should be chosen that shows a direct path from the skin into the lesion, clear of ribs, bulla, fissures, and vessels (especially those with a diameter larger than 5 mm).

Approaching lung lesions through the back, with the patient in the prone position, is advantageous because the patient does not see the needle and can recover in the supine position. Most patients are not comfortable lying in a prone position for several hours without moving. The posterior approach also minimizes respiratory motion and allows access to the intercostal spaces that are wider compared to an anterior approach while avoiding subclavian vessels and costal cartilages. This is why the posterior approach is preferred over the anterior approach for apical lesions, even though the trajectory may be longer. However, the anterior approach may be necessary for lesions in the anterior upper lobes, right middle lobe, and lingula to avoid crossing the major fissures.
Selection of the appropriate introducer needle length is important. Ideally, the introducer is at least 3 to 5 cm longer than the expected needle trajectory to provide the operator with enough needle length to account for gantry angulation, allow for needle repositioning, and guarantee that the nodule can be reached in the case of a pneumothorax. Positioning the patient at an angle may reduce the length of the biopsy tract, especially for central lesions ( Fig. 42.10 ).

Optimum sedation involves administration of incremental doses of narcotic and anxiolytic to achieve consistent, low-excursion respiratory motion and patient immobility. Excessive sedation can cause significant atelectasis, which may obscure the lesion or cause it to move out of the selected path. It can also lead to erratic deep respirations. Local anesthetic administered through the introducer needle just prior to crossing the pleura prevents pain and sudden patient movement.
Rapid on-site evaluation by a pathologist has been proven to decrease the rate of nondiagnostic lung biopsies. This can confirm that diagnostic material has been sampled and can help guide redirecting the introducer needle, if necessary. Based on this intraprocedural assessment, the radiologist can decide to proceed with a core biopsy to obtain more solid tissue or obtain dedicated fine-needle aspirates for microbiologic analysis, special stains, or flow cytometry. Tissue cores increase the chances of establishing the specific diagnosis of neoplasm and provide material for additional molecular analysis and subtyping. As a general principle, tissue cores should be obtained whenever it is safe, especially if no pathologist is available for preliminary interpretation during the procedure and if a benign entity is suspected, such as a hamartoma or granuloma.
Complications and Management of Lung and Mediastinal Biopsy
Complications associated with lung biopsy and their likelihood of occurrence are listed in Table 42.1 . A pneumothorax incurred prior to positioning the introducer needle close to the biopsy target poses a challenge because partially deflated lung will move away from the chest wall and will be difficult to puncture. In this case, a small chest tube can be placed to aspirate the air to continue the procedure ( Fig. 42.11 ). If an introducer needle crosses the pleura but is malpositioned and cannot be redirected, this needle should be left in the lung, and a second introducer needle should be placed. The first needle serves as an anchor while the biopsy is performed through the second needle, and both introducer needles can be removed at the end of the procedure.