Abstract
Twin-twin transfusion syndrome (TTTS) is a serious condition that complicates roughly 8% to 15% of monochorionic, diamniotic twin pregnancies. Although the pathophysiology of TTTS remains incompletely understood, intertwin vascular connections (anastomoses) within the placenta are critical for its development. When TTTS develops early in pregnancy, it is associated with high rates of twin perinatal mortality and, among survivors, substantial risk for long-term neurological morbidity. Ultrasound is the mainstay of prenatal TTTS diagnosis and staging, with evidence of recipient twin polyhydramnios and donor twin oligohydramnios necessary to secure the diagnosis. In the second trimester, ultrasound surveillance on an every-other-week basis is recommended to identify pregnancies with TTTS or other pathology. Fetal echocardiography is additionally recommended, as it may detect structural and functional heart abnormalities. While early-stage TTTS may be managed conservatively with close observation, referral to a fetal therapy center that offers laser photocoagulation is advisable for further consultation and to discuss management options. Fetoscopic laser therapy is the optimal treatment for advanced-stage TTTS presenting by 26 weeks. Neuroimaging should be considered in pregnancies complicated by TTTS due to risk of major neurological morbidity among survivors.
Keywords
twin-twin transfusion syndrome, TTTS, monochorionic, diamniotic
Introduction
Twin-twin transfusion syndrome (TTTS) is a serious condition that can complicate twin pregnancies with monochorionic diamniotic (MCDA) placentation. MCDA twin pregnancies should be monitored for TTTS with serial ultrasound (US) scans beginning in the second trimester. Early-stage TTTS can be managed conservatively, but because of the unpredictable risks of disease progression and intrauterine fetal demise, prenatal testing and delivery before term should be considered. Limited data from randomized trials and retrospective experience suggest that fetoscopic laser photocoagulation may be the best available treatment for advanced TTTS diagnosed in the second trimester. Despite the availability of laser treatment, a significant risk of twin demise and neurologic handicap remains among survivors. Early detection, intervention for advanced disease, serial surveillance, and timed delivery can improve the prognosis for TTTS.
Disease
Definition
TTTS is diagnosed prenatally by US and staged based on various US findings. The initial staging of TTTS, as described by Quintero et al., was judged to have prognostic significance and thought to provide a method to compare outcome data between different therapeutic interventions. Although the staging system may not correlate perfectly with perinatal survival, it improves communication between patients and providers and identifies a subset of cases that may benefit from treatment. TTTS has five stages ranging from mild disease with isolated discordant amniotic fluid volume to severe disease involving demise of one or both twins ( Table 162.1 ).
| Ultrasound Parameter | Staging Criteria | |
|---|---|---|
| Stage I | MVP of amniotic fluid | MVP <2 cm in donor sac; MVP >8 cm in recipient sac |
| Stage II | Fetal bladder | Nonvisualization of fetal bladder in donor twin over 60 min of observation |
| Stage III | Umbilical artery, ductus venosus, and umbilical vein Doppler waveforms | Absent or reversed umbilical artery diastolic flow, reversed ductus venosus a-wave flow, pulsatile umbilical vein flow |
| Stage IV | Fetal hydrops | Hydrops in one or both twins |
| Stage V | Absent fetal cardiac activity | Fetal demise of one or both twins |
Prevalence and Epidemiology
In general, only twin gestations with MCDA placentation are at significant risk for TTTS. The number of TTTS cases is increasing secondary to the increase in monozygotic twinning associated with in vitro fertilization. Overall, about two-thirds of monozygotic twins are MCDA, and 8% to 15% of these pregnancies develop TTTS. TTTS is rare in monozygotic twins with dichorionic or monoamniotic placentation.
The presentation of TTTS is highly variable, and TTTS does not always progress in a predictable manner. The natural history of advanced TTTS is bleak, with reported perinatal loss rates of 70% to 100%, particularly when disease manifests early in gestation. It is estimated that TTTS accounts for 15% to 20% of the total perinatal mortality in twins and for about half of all perinatal deaths in MCDA twins. Although TTTS may manifest at any point in pregnancy, most cases are diagnosed in the second trimester. Without treatment, the loss of at least one fetus is very common with significant risk of co-twin demise or neurologic handicap in cases of co-twin survival. Overall, single twin survival rates in TTTS vary widely between 15% and 70%, depending on gestational age at diagnosis and the severity of disease. However, two-thirds of early-stage TTTS remains stable or regresses without invasive interventions. The lack of predictability of TTTS poses a significant challenge to clinicians caring for MCDA twins.
Etiology and Pathophysiology
Although the pathophysiology of TTTS is not completely understood, intertwin vascular connections within the placenta are critical for its development. Virtually all MCDA placentas have anastomoses that link the circulations of the twins, yet not all MCDA twins develop TTTS. There are three main types of anastomoses in monochorionic placentas: venovenous anastomoses (VVA), arterioarterial anastomoses (AAA), and arteriovenous anastomoses (AVA). AVA are found in 90% to 95% of MCDA placentas, AAA are found in 85% to 90%, and VVA are found in 15% to 20%.
Both AAA and VVA are superficial connections on the surface of the placenta with the potential for bidirectional flow ( Fig. 162.1 ). AVA are deep within the placenta and can result in unidirectional flow from one twin to the other and, if uncompensated, may lead to an imbalance of volume flow between the twins. In contrast to AAA and VVA, which are direct vessel-to-vessel connections, AVA are linked through large capillary beds deep within a cotyledon. AVA are believed to be essential, but not sufficient alone, for the development of TTTS, which explains why they have been found in more than 90% of MCDA placentas with TTTS and in more than 90% without TTTS. These deep AVA are usually multiple and overall balanced by AVA coursing in the opposite direction so that TTTS does not occur. Although the number of AVA from donor to recipient may be important, their size and placental resistance likely influence the volume of intertwin transfusion that occurs. Placentas in cases of TTTS are also more likely to have VVA but less likely to have AAA. It is thought that AAA may compensate for the unidirectional flow through AVA, preventing the development of TTTS or decreasing its severity when it does occur. Mortality is highest in the absence of AAA and lowest when these anastomoses are present. However, the presence of AAA is not completely protective because 25% to 30% of TTTS cases also have these anastomoses. Although chronic TTTS seems to be the result of deep AVA, acute TTTS may occur when there is rapid intertwin transfusion through superficial anastomoses. This uncommon complication, referred to as twin anemia-polycythemia sequence, is most often observed at the time of delivery and is rarely detected prenatally.

Although the primary problem lies with the placenta, additional factors beyond placental morphology appear to be involved in the development of TTTS. The simple imbalance of blood flow through placental anastomoses may lead to a more complex interplay between fetal adaptations and altered vascular reactivity. Donor twins exhibit evidence on US of volume depletion with oliguria and oligohydramnios, whereas recipient twins exhibit fluid overload with polyuria, polyhydramnios, and acquired cardiac dysfunction ( Fig. 162.2 ). Hypovolemia in donor twins leads to upregulation of the renin-angiotensin system (RAS) with increased renal renin production and angiotensin synthesis with subsequent vasoconstriction and hypertension. In contrast, hypervolemia in recipient twins results in downregulation of the RAS with decreased renin production and suppression of antidiuretic hormone to increase diuresis and reduce blood pressure. This discordance in the RAS in MCDA twins may occur by 13 to 14 weeks’ gestation. Vasoactive hormones produced by the donor may affect placental resistance resulting in changes in the umbilical artery waveforms. These vasoactive hormones can also reach the recipient through placental anastomoses resulting in worsening hypertension and cardiac dysfunction. Discordant endothelin levels have also been reported, and elevated levels in recipient twins may contribute to the development of systemic hypertension and diastolic dysfunction. Although renin levels are higher in both donor and recipient twins compared with controls, recipient twins are exposed to the highest levels of renin-angiotensin effectors, suggesting that regional RAS upregulation in the placenta may also contribute to the elevated RAS effectors found in recipient twins. Discordant activation of the RAS in MCDA twins and in the placenta may play an important role in the development of TTTS.

Manifestations of Disease
Clinical Presentation
Although monthly US scans were previously considered standard surveillance for twin pregnancies regardless of chorionicity, more recent studies suggest that this frequency is insufficient for the prompt detection of acute complications in twins with MCDA placentation. TTTS is a dynamic condition that can remain unchanged throughout gestation, progress slowly over numerous weeks, or develop quickly within days with rapid deterioration in fetal well-being. US surveillance every 2 weeks and patient education about the signs and symptoms of polyhydramnios have been shown to increase the early detection of TTTS. Although early-stage TTTS resolved in 41% of cases and remained stable in 28%, cases that progress to advanced TTTS usually do so within 2 weeks. Given that TTTS usually manifests in the second trimester and that a subset of pregnancies rapidly deteriorates to advanced disease, serial US scans every 2 weeks beginning at 14 to 16 weeks’ gestation is reasonable until better risk stratification is established.
Some first-trimester and second-trimester findings may warrant increased surveillance of MCDA gestations. Intertwin discrepancies in amniotic fluid volume, crown-rump length, nuchal translucency thickness, placental cord insertion (PCI), and abdominal circumference each independently increases the risk of TTTS. Nuchal translucency measurements greater than the 95th percentile and discordant nuchal translucency measurements of 20% or more between MCDA twins have been associated with TTTS. Reversed a-wave in the ductus venosus waveform in MCDA twin pregnancies at 11 to 13 weeks’ gestation is another risk factor for TTTS, with the condition developing in about one-third of cases. The detection of membrane folding in the second trimester is a sign of developing fluid discordance between the two sacs, and about half of all MCDA twins with membrane folding develop TTTS ( Fig. 162.3 ). Changes in middle cerebral peak systolic flow may also indicate discordance in fetal hemoglobin between the twins. Abnormal PCI and, in particular, velamentous insertion may also increase the likelihood of TTTS. Velamentous PCI is found in one-third of TTTS placentas compared with an incidence of 10% in placentas without TTTS ( Fig. 162.4 ). In addition, donor twins are more likely to have velamentous PCI compared with recipients when TTTS is diagnosed. In contrast, marginal PCI is found at a similar rate in placentas with TTTS and without TTTS.


It has been reported that AAA can be identified by US, and if AAA are detected in MCDA gestations, the risk of TTTS is decreased. If TTTS develops, the finding of AAA may confer a more favorable prognosis. However, US is best at detecting these anastomoses late in gestation, limiting the clinical usefulness of this assessment.
Intertwin transfusion appears to be a fragile equilibrium that can result in a spectrum of TTTS severity; TTTS can regress, remain stable, progress slowly, or deteriorate rapidly. Although several markers may help identify a subset of MCDA twins at increased risk, no marker performs well enough to change current surveillance or clinical care of MCDA gestations. Although uterine distention secondary to polyhydramnios, preterm contractions, and pelvic pressure may be recognized clinically, many patients are asymptomatic at the time of presentation. A high level of suspicion and serial US evaluations are necessary for timely diagnosis and management of TTTS.
Imaging Technique and Findings
Ultrasound.
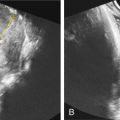
A necessary finding for the US diagnosis of TTTS is the presence of the polyhydramnios-oligohydramnios sequence, or significant amniotic fluid volume discordance. Defined as a maximal vertical fluid pocket of less than 2 cm in the donor sac and greater than 8 cm in the recipient sac, these findings represent less than the fifth percentile (<2 cm) and greater than the 95th percentile (>8 cm) for amniotic fluid measurements, and are used to define stage I TTTS. In the setting of otherwise discordant amniotic fluid volume that fails to meet staging criteria, progression to TTTS occurs in less than 15% of cases. In cases of TTTS, polyhydramnios-oligohydramnios sequence is usually followed by marked oliguric oligohydramnios in the donor twin represented by nonvisualization of the urinary bladder (stage II) ( Fig. 162.5 ). Absent or reversed end-diastolic flow in the umbilical artery of the donor and absent or reversed a-wave in the ductus venosus of the recipient can subsequently develop (stage III) followed by hydrops (stage IV) ( Figs. 162.6 and 162.7 ). Although growth discordance and intrauterine fetal growth restriction (IUGR) may complicate TTTS, growth disorders are no longer used to establish the diagnosis or to stage disease. Despite the debate over the merit of TTTS staging, it appears to be useful in diagnosing the condition, monitoring progression, and providing a common framework for research.



Magnetic Resonance Imaging.
Although fetal magnetic resonance imaging (MRI) is not commonly used in the initial evaluation of TTTS, fetal MRI has been shown to be superior to obstetric US in the identification of cerebral ischemia and intraventricular hemorrhage in TTTS. Fetal MRI may also show evidence of altered hemodynamics as suggested by enlargement of the cerebral venous sinuses in donor and recipient twins and dilatation of the renal collecting system in recipient twins. Given that the risk for adverse neurologic outcome is significant in TTTS, MRI may prove useful in the evaluation of the fetal brain, but further studies are needed to define its role in the workup of TTTS. Despite a lack of compelling data, fetal MRI is often performed after invasive therapy for TTTS or after death of one twin to document an absence of resultant central nervous system ischemic or hemorrhagic injury.
Other Applicable Modality.
Screening for congenital heart disease is warranted in all monochorionic twins because the risk of cardiac anomalies is increased ninefold in MCDA twins and 14-fold in cases of TTTS. Overall, the incidence of congenital heart disease in TTTS has been reported to be about 5%. It is theorized that the abnormal placentation that occurs in monochorionic twins, particularly in cases in which TTTS develops, contributes to abnormal fetal heart formation.
In addition to congenital heart defects, structural cardiac abnormalities can also be acquired in TTTS; this phenomenon is virtually exclusive to recipient twins. The discordant cardiovascular physiology in MCDA twins appears to be related both to unbalanced flow through AVA and to changes in the RAS. The initial hypervolemia in the recipient results in endocrine dysregulation, systemic hypertension, and cardiac dysfunction. Volume overload causes increased pulmonary and aortic velocities, cardiomegaly, and atrioventricular valve regurgitation ( Fig. 162.8 ). Over time, recipient twins can develop progressive biventricular hypertrophy and diastolic dysfunction and poor right ventricular systolic function that can lead to functional right ventricular outflow tract obstruction and pulmonic stenosis ( Figs. 162.9 and 162.10 ). The development of right ventricular outflow obstruction, observed in almost 10% of all recipient twins, is likely multifactorial, a consequence of increased preload; afterload; and circulating factors such as renin, angiotensin, endothelin, and atrial and brain natriuretic peptides. The cardiovascular response to TTTS contributes to the poor outcome of recipient twins, whereas recipients with normal cardiac function have improved survival.




Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree