Introduction
Doppler ultrasound is extremely useful in the evaluation of the many problems facing the hemodialysis patient. It is a noninvasive technique that demonstrates vascular detail without the risk of phlebitis or contrast reaction associated with contrast venography. Current Dialysis Outcome Quality Initiative (DOQI) guidelines encourage the placement of arteriovenous fistulas (AVFs) rather than grafts because of their greater longevity and decreased incidence of infection. Detailed evaluation of arterial and venous anatomy prior to hemodialysis access placement improves the characterization of arteries and veins suitable for native AVF placement, particularly in the patient with a history of prior failed access and/or prior placement of central catheters.
Vascular mapping before hemodialysis access may also change the surgical procedure because the identification of a suitable efferent vein would favor the placement of an AVF rather than a graft. In addition, there is an increased likelihood of selecting the most functional vessels preoperatively, with a subsequent decrease in unsuccessful surgical explorations. Vascular mapping can increase the proportion of patients in dialysis with a fistula, and decrease the number of early postoperative failures.
Despite preoperative vascular mapping, up to 60% of AVFs still fail to mature adequately to support hemodialysis. In these patients, ultrasound can determine the potential cause of an immature AVF. It can also determine whether the AVF should be treated by an endovascular (angioplasty of a stenosis) or open surgical (AVF revision or accessory vein ligation) approach. Ultrasound is also useful in the evaluation of patients with a hemodialysis graft to assess for the presence of a stenosis or vascular steal and to determine the etiology of perigraft pulsatile masses (hematoma versus pseudoaneurysm). After AVF and graft sites are exhausted in the upper extremity, placement of a thigh graft is a viable option that is more effective than use of hemodialysis catheters.
This chapter describes hemodialysis access anatomy and the preferred order of access placement. It also describes current protocols for the sonographic vascular evaluation of the end-stage renal patient, both before and after hemodialysis access placement.
Basic Concepts of Hemodialysis Access
Hemodialysis is the lifeline by which the patient with end-stage renal disease eliminates excess fluid and decreases the level of various undesirable substances in the blood. The central circulation is accessed, and the blood is cleansed by diffusion across a semipermeable membrane, termed the dialyzer. Direct access to the circulation is accomplished by an AVF, a graft, or a central venous dialysis catheter. A native AVF is a surgically created, direct anastomosis between an artery and a vein, placed in either the forearm or upper arm. When AVF creation is not possible, an artificial graft consisting of polytetrafluoroethylene (PTFE) or other material may be tunneled in the superficial soft tissues of the forearm, upper arm, or upper thigh, with surgically created arterial and venous anastomoses.
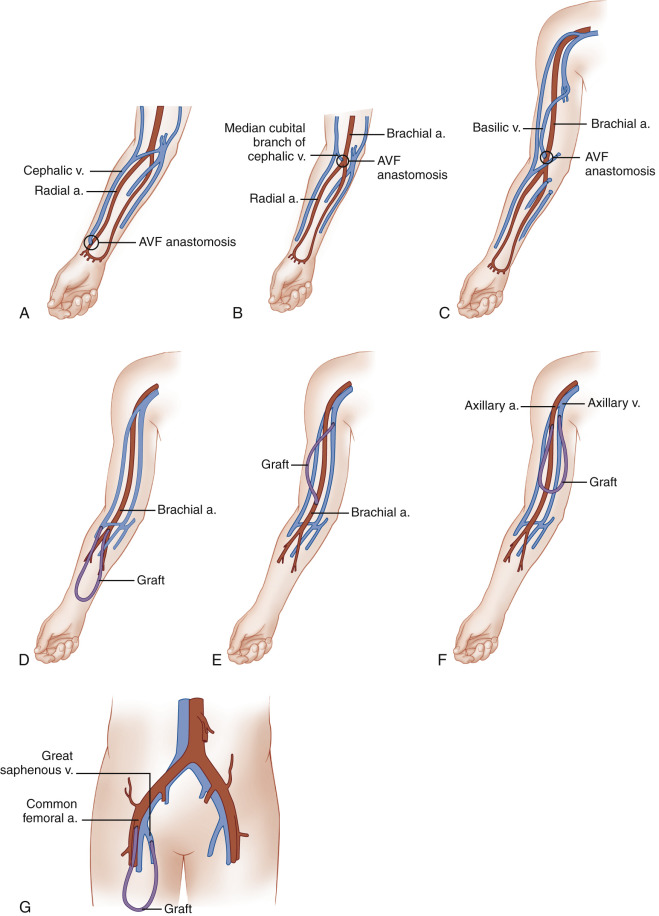
During hemodialysis, two 15-gauge needles are placed into the mature AVF or graft, with the more distal needle (pointing toward the artery) carrying blood from the patient to the dialyzer. The second needle is placed more proximally (closer to the venous outflow) in the AVF or graft and returns the blood to the patient’s circulation. The AVF and hemodialysis graft artery/vein configurations that are most commonly used are described in Table 14.1 and shown in Fig. 14.1 . Surgeons prefer to create a hemodialysis access in the nondominant arm because the activities of daily living can be carried out with the dominant arm while the nondominant arm is healing after surgical access placement. However, most will put an AVF in the dominant arm before a graft is considered. An AVF is placed first in the forearm, if the patient has suitable anatomy, and the upper arm is then saved for future potential dialysis access. Likewise, if an AVF cannot be placed, a forearm graft is preferred to placement of an upper arm graft. If no upper extremity graft options are available, a thigh graft is preferable to dialyzing with an indwelling venous catheter. A list of the preferred order of access placement is given in Table 14.2 . In general, an AVF or hemodialysis graft will provide higher dialysis flow rates than a tunneled catheter while having lower infection rates.
| AVF types | Artery | Vein |
| Forearm cephalic vein | Radial | Cephalic |
| Forearm vein transposition | Radial | Ulnar, dorsal, or volar vein |
| Upper arm cephalic vein | Brachial | Cephalic |
| Basilic vein transposition | Brachial | Basilic |
| Graft types | Artery | Vein |
| Forearm loop | Brachial | Antecubital |
| Upper arm straight | Brachial | Basilic |
| Upper arm loop | Axillary | Axillary |
| Thigh graft | Common femoral/superficial femoral | Great saphenous/common femoral/femoral |
| Order of Access Placement Type |
|
|
|
|
|
|
|
Descriptive Terminology
The conventional way to describe vascular anatomy uses the terms proximal and distal, meaning closer and farther from the heart, respectively. We find that these terms can be confusing when used in describing dialysis access anatomy. Therefore in some circumstances we prefer the terms cranial and caudal, meaning toward the head and toward the lower end of the body. We will use these terms in selected locations throughout this chapter, realizing that more conventional terms are used elsewhere in this text.
Vascular Mapping Before Hemodialysis Access Placement
General principles
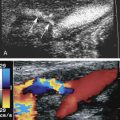
The protocol for vascular mapping before hemodialysis access placement has been previously described. A high-resolution linear array ultrasound transducer is used to evaluate the vessels (generally 9 MHz or higher). Gray-scale transverse plane imaging is used to identify arteries and veins and to evaluate their diameter and wall thickness. Sequential vein compression is used to assess for compressibility, indicating patency, or loss of compressibility because of acute or chronic thrombus. The depth from the skin surface of the anterior wall of the cephalic vein is measured. Color Doppler images and Doppler spectral waveforms are obtained in the longitudinal plane of vessels selected for potential vascular access.
Typically, the entire arm is assessed, according to department protocol. The forearm veins and arteries are first assessed to determine whether the patient is a candidate for a forearm AVF, the most desirable initial type of hemodialysis access. Arteries should be assessed for intimal thickening, calcification, and stenosis. The presence of significant concentric calcification should be noted because the artery may be too calcified for successful surgical access creation. An important aspect of planning for AVF and dialysis graft creation is vessel size assessment. Minimum artery and vein diameters are shown in Table 14.3 . It is important to note that upper extremity vessel mapping should be performed with the patient sitting upright so that the arm veins are dependent to the heart. This position will optimize vein diameter, along with the placement of a tourniquet. Ambient room temperature should not be cold, and warm blankets or warm compresses can be used as necessary to induce vasodilation.
| Vessel | Minimum Diameter (mm) |
|---|---|
| Vein used for AVF | 2.5 |
| Vein used for AVG | 4.0 |
| Artery used for either AVG or AVF | 2.0 |
Forearm assessment
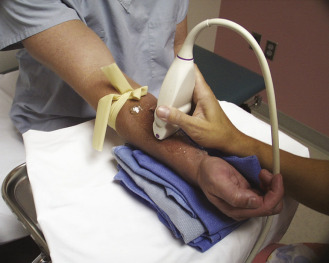
The nondominant forearm is assessed first. The patient’s arm is placed in a comfortable position on towels on top of a procedure stand ( Fig. 14.2 ) or the armrest of a phlebotomy chair. The internal diameter of the radial artery at the wrist should measure at least 2 mm ( Fig. 14.3 ). If the radial artery internal diameter is not satisfactory ( Fig. 14.4 ) within several centimeters of the wrist, the internal diameter of the ulnar artery at the wrist is measured. If the diameter of the ulnar or radial artery is not at least 2 mm in the lower third of the forearm, the forearm radial and ulnar arteries are assessed on the dominant side. If no forearm artery is satisfactory, the patient is not a candidate for a forearm AVF.




If the radial or ulnar artery at the wrist meets size criteria, the cephalic vein is the next vessel that should be evaluated. A tourniquet is placed moderately tightly at the mid-forearm. The entire distal forearm is percussed, as if starting an intravenous line, for approximately 3 minutes. All wrist veins greater than 2 mm after the 3-minute tapping are evaluated. Veins smaller than 2 mm will probably not dilate up to an adequate size. However, veins greater than 2 mm may dilate to greater than 2.5 mm with more focused tapping and/or a warm compress. Special attention is given to the cephalic vein, as this is the preferred venous outflow conduit. The cephalic vein area is assessed for the presence of a continuous vein up to the tourniquet with a diameter of at least 2.5 mm ( Fig. 14.5 ).

If the forearm portion of the cephalic vein is adequate, the vein is followed in a cephalad direction to the elbow after a tourniquet is placed at the elbow. If the vein is discontinuous or stenotic, it is not suitable for fistula creation. A search is then made for another adequate forearm vein. Branch points should be assessed carefully because short segments of vein narrowing below 2.5 mm may occur close to them. Following examination of the forearm veins, the tourniquet is moved to the axilla, and then the vein of interest is followed centrally to ensure that it empties into the deep venous system. The tourniquet must be removed to evaluate the cephalic vein insertion into the subclavian vein. Occasionally, overlying muscle may compress the vein and mimic the appearance of a stenosis at the insertion of the cephalic vein into the subclavian vein. Placing the patient’s arm by his/her side (rather than in an abducted position) may alleviate an apparent cephalic vein stenosis.
If the cephalic vein is not adequate, the basilic vein in the forearm is assessed. If the basilic vein is not adequate, the volar surface of the forearm, followed by the dorsal surface of the forearm, is assessed for a suitable vein.
Upper arm assessment
If a forearm fistula is not possible, the upper arm should be assessed for vascular anatomy suitable for fistula creation. A tourniquet is placed at the axilla. The brachial artery is measured (usually at 2 cm cranial to the antecubital fossa), above its bifurcation into the radial and ulnar arteries. Satisfactory internal diameter of the brachial artery should be 2 mm or greater ( Fig. 14.6 ).

The cephalic vein diameter is then measured at the antecubital fossa. For a brachiocephalic fistula, it should measure at least 2.5 mm and extend approximately 2 cm below the antecubital fossa because several centimeters of vein are needed to create the anastomosis with the brachial artery near the antecubital fossa. Alternatively, the surgeons may use a median cubital branch of the cephalic vein as it travels close to the brachial artery; therefore this branch can also be evaluated, depending on the surgeon’s preference.
If an adequate cephalic vein is not found ( Fig. 14.7 ), the basilic vein ( Fig. 14.8 ) is evaluated. A basilic vein suitable for a basilic vein transposition must extend at least 4 cm caudal to the antecubital fossa to provide a suitable length to loop around and connect with the brachial artery. A surgeon may also create an anastomosis with the brachial artery using a large antecubital vein such as the median antecubital vein that drains into the basilic vein. If the basilic vein does not extend 4 cm below the antecubital fossa, it may still be suitable for the creation of a dialysis graft if its diameter is 4 mm or more.


If a suitable vein is found, its continuity with the deep venous system must be confirmed. To this end, the vein is followed cephalad to ensure that it is continuous and of adequate size along its entire course, until it empties into the deep venous system. The diameter of the deep vein is also evaluated to the point where it joins the subclavian vein. The largest of the paired brachial veins may also be measured for potential brachial vein transposition AVF. If a suitable site is not found for an AVF, forearm loop, or upper arm straight graft placement, the axillary vein and axillary artery diameters are measured because an upper arm loop graft may still be possible.
Subclavian, internal jugular, and central vein assessment
The subclavian and internal jugular (IJ) veins are then evaluated for the presence of stenotic lesions, occlusions, or thrombus. It is easiest to perform this portion of the study in the supine position to increase venous filling. Doppler spectral waveforms should be assessed in the medial portion of the subclavian vein and the caudal portion of the internal jugular vein for respiratory phasicity and transmitted cardiac pulsatility ( Fig. 14.9 ). If normal blood flow features are absent and a monophasic flow pattern is demonstrated, central venous stenosis or obstruction is inferred. The contralateral subclavian and IJ should then be examined. If the flow abnormality is unilateral, brachiocephalic vein stenosis or occlusion is likely. If bilateral, a superior vena cava (SVC) stenosis or occlusion is likely. Fig. 14.10 shows abnormal unilateral blood flow pattern in the right subclavian vein, consistent with a brachiocephalic vein stenosis or occlusion. Occasionally, the brachiocephalic veins and SVC can be directly visualized with ultrasound. In such cases, they are best seen with a small-footprint transducer placed above the medial clavicle or in the sternal notch, using central angulation. Assessment of the brachiocephalic veins and SVC, if visible, should be performed with gray-scale, color Doppler imaging, and acquisition of Doppler spectral waveforms.