Chapter 12 Ultrasound safety
INTRODUCTION
There has been a considerable and rapid growth in the use of ultrasound as a diagnostic imaging tool over the past 50 years since it was first used to image the unborn fetus. This rapid growth has resulted in millions of people worldwide being scanned every year. Changes and advances in technology are leading to increasing power levels being used to obtain diagnostic information. The interaction of ultrasound with biological tissue can result in effects which may cause heating, interfere with the normal functioning of cells, and cause structural damage. The potential damaging nature of ultrasound leads to concern over its safety. All operators therefore need to have an understanding of the safety implications in order to practice safely.
WHY ARE WE INTERESTED?
Important Parameters
Amplitude, power, and intensity are parameters used to describe the strength of an ultrasound beam.
Amplitude
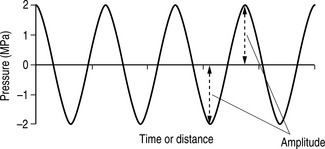
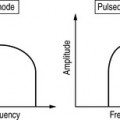
Amplitude is a measure of a wave’s magnitude of oscillation, that is, the magnitude of the maximum disturbance in the medium, and in ultrasound often refers to the maximum variation (see Fig. 12.1). Amplitude is measured in units of pressure: MPa (megapascals).
Intensity (I)
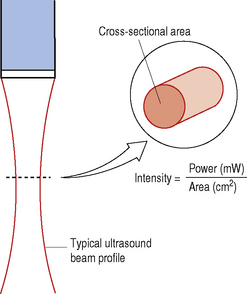
From the equation in Figure 12.2 we can identify that the intensity of an ultrasound beam is directly proportional to its power, i.e. if beam power increases, then intensity increases and, conversely, if beam power decreases, the intensity decreases.
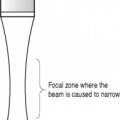
The maximum intensity along an ultrasound beam lies at the focus (the narrowest part of the beam)where all the power is concentrated into a small cross-sectional area.
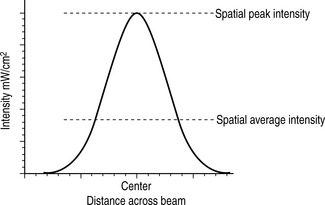
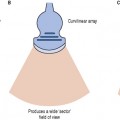
The intensity within an ultrasound beam also varies from point to point across the beam (spatial considerations), as demonstrated in Figure 12.3. Two values of intensity can de defined:
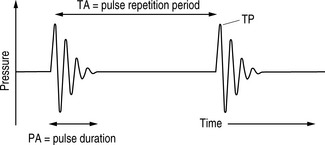
Because of the pulsed nature of ultrasound, the intensity of the ultrasound beam also varies over time (temporal considerations). Figure 12.4 shows the relevant times for three intensities:
| Highest intensity |  | ISPTP – Spatial peak-temporal peak (SPTP) |
| ISATP – Spatial average-temporal peak (SATP) | ||
| ISPPA – Spatial peak-pulse average (SPPA) | ||
| ISAPA – Spatial average-pulse average (SAPA) | ||
| ISPTA – Spatial peak-temporal average (SPTA) | ||
| Lowest intensity | ISATA – Spatial average-temporal average (SATA) |
ISPTA is the measure most associated with temperature rises.
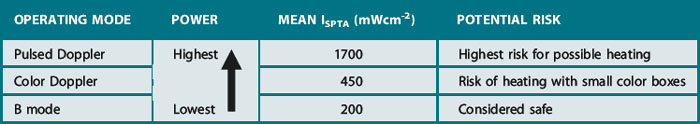
OPERATING MODES AND THEIR POTENTIAL RISK
B modes
Uses the lowest output power and intensities and is generally considered safe in all applications.
Pulsed Doppler
Dwell time, i.e. the length of time that the ultrasound beam is fixed on a specific tissue area, is an important factor when considering the potential for heating. This is particularly relevant for spectral pulsed Doppler where the beam is held in a fixed position during an investigation; this leads to a further increase in temporal average intensity and therefore increased risk of causing a temperature rise.