2 Risk Factors for Lung Cancer
Summary
This chapter discusses the most common cause of lung cancer, namely, cigarette smoking, and the numerous chemicals and carcinogens found in cigarette smoke. Other well-known and less well-known causative factors are also discussed.
Keywords: lung cancer, cigarettes, radon, secondhand smoke exposure, asbestos and other occupational carcinogens, COPD, interstitial lung disease
2.1 Introduction
Cigarette smoking remains the single most important risk factor for the development of lung cancer. The risk of lung cancer increases with both the quantity and duration of smoking. It is estimated that 10% of heavy smokers will develop lung cancer. Smoking contributes to 80% of lung cancer deaths in women and 90% of such deaths in men. Male heavy smokers are 23 times more likely to develop lung cancer than nonsmoking men. Female heavy smokers are 13 times more likely to develop lung cancer than nonsmoking women. The relative risk varies between 9- and 10-fold for average-heavy smokers and the relative risk is greatest for the development of squamous cell and small cell lung cancers (▶ Table 2.1). The relative risk associated with cigar and pipe smoking is about five times that of nonsmokers (▶ Table 2.1).
Cigarette smoke contains over 7,000 chemicals, about 250 of which are known to be harmful and 70 of which are recognized carcinogens. Cigarette smoke containing carcinogens include polycyclic aromatic hydrocarbons (PAHs), aromatic amines, N-nitrosamines, and other organic and inorganic compounds, such as benzene, vinyl chloride, arsenic, and chromium. Cigarette smoke also contains radioactive compounds, such as radon and its decay products, as well as bismuth and polonium 210. Some of the chemicals and other poisons found in cigarette smoke, which no person would otherwise ever consider ingesting or inhaling, include the following: turpentine (paint thinner), propylene glycol (preservative), butane (lighter fluid), cadmium (used batteries), lead (neurologic toxin), ammonia (household toilet cleaner), benzene (crude oil), formaldehyde (embalming fluid), acetone (finger nail polish remover), arsenic (rat poison), methane (sewer gas), hydrogen cyanide (poison and used in various pesticides), toluene (paint thinners), carbon monoxide (exhaust fumes), etc. Although cigarettes today contain less tar and nicotine, the lower level of nicotine compels smokers to smoke more intensely, drag, puff, or inhale more deeply and frequently. This results in the deposition of carcinogens in the more distal airways and the increased incidence of adenocarcinomas. These chemicals and poisons may be present in each inhaled and exhaled puff of cigarette smoke (▶ Fig. 2.1).

In 2014, nearly 17 of every 100 U.S. adults aged 18 years or older (16.8%) smoked cigarettes. This translates into an estimated 40 million adult smokers. Cigarette smoking is the leading cause of preventable disease and death in the United States, accounting for more than 480,000 deaths every year, or 1 of every 5 deaths.
2.2 Never Smokers
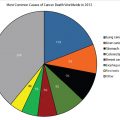
The term never smokers refers to those persons who have smoked fewer than 100 cigarettes in their lifetime, including lifetime nonsmokers. Globally, about 15% of lung cancers in men and up to 53% in women are unrelated to cigarette smoking. Never smokers comprise about 25% of all lung cancer cases worldwide. Interestingly, lung cancer in never smokers ranks as the seventh most common cause of cancer death. In South Asia, up to 80% of women with lung cancer are never smokers, whereas in the United States it is estimated that 19% of lung cancer in women and 9% of lung cancer in men occur in never smokers. The age-adjusted rate for lung cancer in never smokers (ages 40–79 years) ranges from 11.2 to 13.7 per 100,000 person-years for men and from 15.2 to 20.8 per 100,000 person-years for women. However, it should be stressed that the rates are 12 to 30 times higher in current smokers of the same age group. The most commonly diagnosed cell type of lung cancer in never smokers is adenocarcinoma.
2.3 Radon
The National Council on Radiation Protection and Measurements recognizes radon and its decay products as being the single largest source of environmental exposure to ionizing radiation among American citizens. Radon is a well-established carcinogen and radon exposure is the second most common cause of lung cancer in the United States, responsible for 7,000 to 36,000 lung cancer deaths each year.
Radon-222 is the natural odorless, tasteless, and colorless decay product of radium-226. The latter is the decay product of uranium-238. Both uranium and radium are ubiquitous in the earth’s crust found in variable concentrations in the soil, rock, and stone around us. Radon (t1/2 = 3.8 days) decays into polonium-214 and polonium-218, which emit α-particles that damage the respiratory epithelium when inhaled, causing genetic mutations. The continued decay process eventually forms polonium-210 (t1/2 = 22 years).
Occupational radon exposure is most frequently encountered in the mining industry. There is a linear relationship between exposure to radon and the risk of developing lung cancer in underground miners. Although uranium mining is no longer taking place in the United States, occupational radon exposure still occurs in the nonuranium mining industry in the United States and in both uranium and nonuranium mines around the world. The Biological Effects of Ionizing Radiation IV study estimated that a 40-year exposure to radon at a concentration above 0.3 work level with an annual cumulative exposure limit of 4 work-level months would increase an exposed individual’s lifetime risk of developing lung cancer twofold.
Domestic radon exposure is dependent upon the concentration of radon gas in the soil and rock beneath a given dwelling. Other less common sources of domestic radon gas exposure may include the particular home’s building materials (e.g., stone, brick, rock), the use of well water and natural gas, and the degree of ventilation in the home. Higher levels of domestic exposure have been reported to have a 1.14 overall relative risk for lung cancer (▶ Table 2.1). However, it has been reported that even a nonsmoker exposed to high levels of radon over a lifetime has a 1 in 20 chance of developing lung cancer. This risk can increase to 1 in 3 for a smoker exposed to high levels of radon over their lifetime. The U.S. Environmental Protection Agency (EPA) estimates the average concentration of radon in American homes to be on the order of 1.25 pCi/L, although there is much variation in levels from home to home. The EPA actionable level is 4 pCi/L. The EPA estimates that 1 in 15 U.S. homes exceeds this actionable level. Home radon gas levels can be easily measured via relatively inexpensive home test kits available through many hardware stores or available online. Certified inspectors can also be contacted to determine the radon level in a given home or living complex.
2.4 Environmental Tobacco Smoke (Secondhand Smoke Exposure)
Environmental tobacco smoke (ETS) is also sometimes referred to as secondhand smoke exposure (SHS). There is a reported dose-dependent relationship between the degree of ETS exposure and the relative risk of developing lung cancer. At least 17% of lung cancers in nonsmokers result from high levels of involuntary ETS exposure during childhood and adolescence. Studies have also revealed a dose-dependent increased risk of lung cancer in nonsmoking women married to men smokers based on the number of cigarettes smoked and the duration of their exposure. In particular, there is up to a 24% excess risk of lung cancer in nonsmokers who live with a cigarette smoker. Another study of nonsmoking women found smoking by their spouse was associated with a 30% excess risk for all cell types of lung cancer. The National Research Council (NRC) reports a 1.34 overall risk of lung cancer associated with ETS or an approximately 30% increased risk for lung cancer in nonsmokers (▶ Table 2.1). The EPA, the U.S. National Toxicology Program, the U.S. Surgeon General, and the International Agency for Research on Cancer have all classified ETS as a known human carcinogen. The American Cancer Society Cancer Prevention Study performed a prospective comparative analysis of 133,835 never smokers living with smoking spouses versus 154,000 never smokers living with nonsmoking spouses. The investigators found the relative risk for lung cancer in women with smoking husbands was 1.2. That is, a 20% increased incidence of lung cancer. Although slightly lower, the relative risk in nonsmoking men living with smoking wives was still elevated at 1.1 (▶ Table 2.1).
There is no risk-free level of ETS. Even brief or limited exposures can be harmful and is associated with an increased incidence of ear infections, sudden infant death syndrome (SIDS), bronchitis, pneumonia, severity and frequency of asthma exacerbations, lung cancer, stroke, and cardiac disease. ETS exposure may also increase the risk of breast cancer, nasal sinus cavity cancer, and nasopharyngeal cancer in adults and leukemia, lymphoma, and some brain tumors in children. Since 1964, approximately 2,500,000 nonsmokers have died from health problems caused by ETS. It is estimated that ETS was responsible for over 300,000 cardiovascular deaths during 2005 to 2009 among adult nonsmokers in the United States alone. Although it is difficult to calculate the precise number of lung cancers resulting from involuntary ETS, it is estimated that approximately 3,000 lung cancer deaths occur each year among adult nonsmokers in the United States as a result of ETS.
Most ETS exposure occurs in either the homes and or workplace. Additional sources of exposure include car vehicles and public places such as bars, restaurants, and casinos. Smoke-free laws are becoming more and more prevalent in public places with the goal of reducing the adverse respiratory and cardiovascular health consequences associated with ETS including cancer among nonsmokers.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree