8 High-Riding Jugular Bulb
8.1 Case Presentation
8.1.1 History and Physical Examination
A 26-year-old woman presents for a CT status-post penetrating trauma to her neck. A “mass” was seen in right external auditory canal on otoscopic examination. Her neurologic examination was normal.
8.1.2 Imaging Findings and Impression
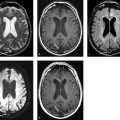
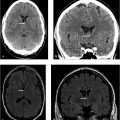
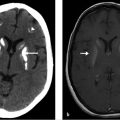
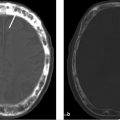
Axial and coronal images (▶ Fig. 8.1a,b) of a contrast CT of the head and neck show the jugular bulb (white arrow) extending superior to the floor of the external auditory canal. An axial contrast MR image (▶ Fig. 8.1c) of the same patient re-illustrates the findings. The left-sided internal jugular vein and jugular bulb are hypoplastic.
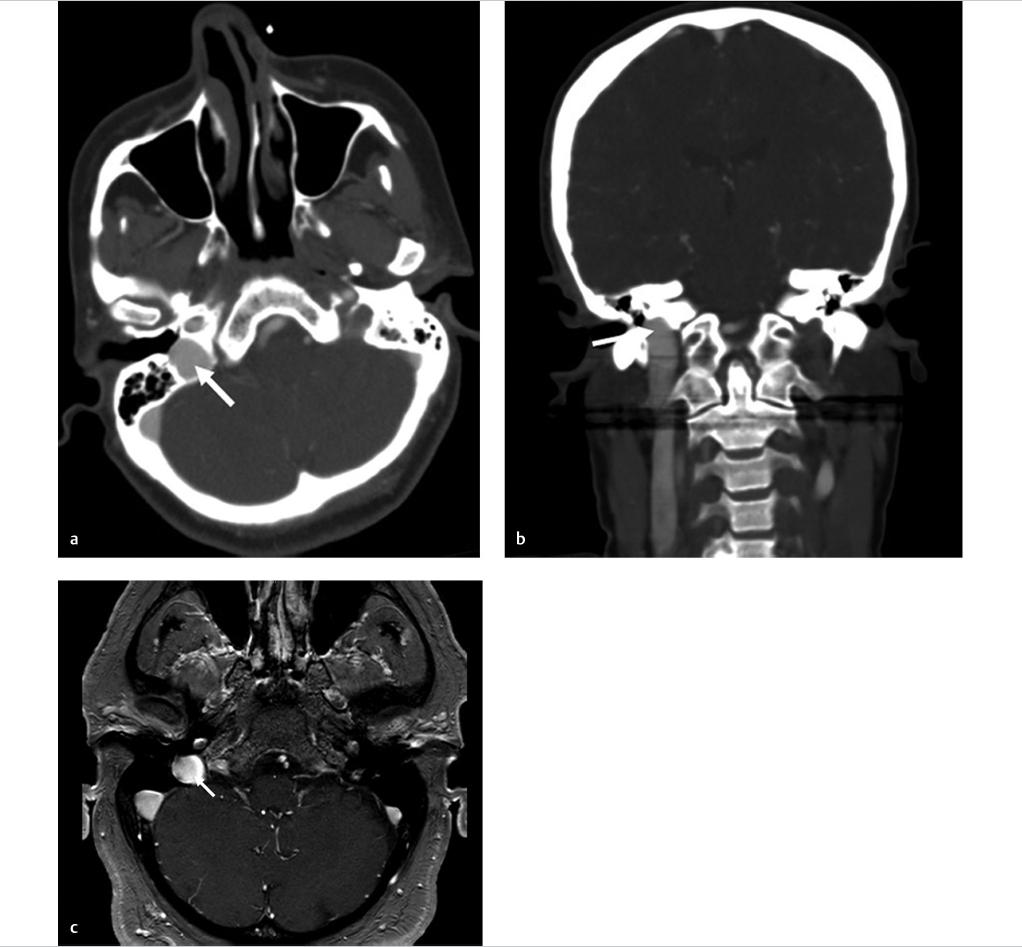
In this case, the thin bony septum separating the jugular bulb from the external auditory canal was be dehiscent. Special care should be taken during examination of the ear to avoid puncturing the jugular bulb.
8.2 Differential Diagnosis
High-riding jugular bulb:
A high-riding jugular bulb is defined as a jugular bulb reaching above the floor of the middle ear cavity. In this case, the sigmoid plate which is normally present between a high riding jugular bulb and middle ear cavity, is absent which defines this as a focal dihiscence. In this case, the patient was asymptomatic. In other cases, this may be a cause of pulsatile tinnitus or even conductive hearing loss if the bulb extends into the middle ear cavity.
Asymmetrical large jugular bulb:
It is a normal variation and usually asymptomatic.
It has been shown that the right-sided jugular bulb in two-thirds of the population is larger compared to the left side.
Glomus jugulare:
It is a paraganglioma confined to the jugular fossa, which may arise from the jugular bulb, the tympanic branch of CN IX, or the auricular branch of CN X.
Patients usually present with tinnitus and hearing loss and commonly show some patterns of cranial nerve palsies (Vernet’s syndrome, Horner’s syndrome and Collet–Sicard syndrome).
It should be fully assessed on CT as it usually manifests with irregularly moth-eaten bony margins and an eroded jugular spine.
It enhances on postcontrast MR images and shows low signal intensity on T1-weighted images and high signal intensity on T2-weighted images.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree