Abstract
Cardiac imaging is an essential part of clinical cardiovascular medicine to identify disease, assess severity and make management decisions, guide interventions, and monitor progression or effect of therapy. In this chapter we introduce the noninvasive diagnostic techniques available today and discuss general topics that the different imaging modalities share, such as the challenges of imaging a moving organ, technical validation, image quality, and safety.
Keywords
Cardiac imaging, Multimodality imaging, Evidence-based diagnostics, Safety.
1.1
Introduction
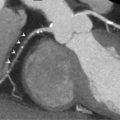
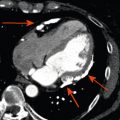
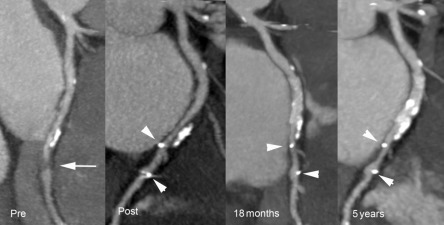
One cannot cure without knowing what is wrong, which is why diagnostic techniques are essential to practice medicine. The heart is a mechanical organ, a pump consisting of moving structures, directed flow, electric controls, and an efficient oxygen and nutrient supply system. These physical phenomena can be investigated in many ways, externally by physical examination, auscultation, or electrocardiogram; invasively using catheters; and more recently by various types of noninvasive cross-sectional imaging modalities. In this book we focus on the fast-developing field of noninvasive cross-sectional imaging of the heart. There is perhaps no other organ where imaging is more important for the clinical management than the heart. While the principal purpose of cardiac imaging is the diagnosis of disease, its impact reaches further than that. Imaging provides information on the severity of disease, the prognostic consequences of abnormalities, and thereby guides imaging decisions. Nowadays, arrhythmia, coronary disease, and an increasing number of structural cardiovascular conditions can be treated by minimally invasive intervention procedures. These catheter-based procedures rely on noninvasive imaging for patient selection, preparation, and direct procedural guidance. While for most healthcare professionals imaging is most tangible in clinical care, diagnostic techniques are becoming more important in research as well. Imaging can improve our understanding of cardiovascular physiology and disease and serve as a noninvasive monitor of disease progression—for instance as a surrogate marker to assess the effect of pharmacological or mechanical interventions ( Figure 1.1 ).
1.2
Imaging the heart
The notion that imaging of the heart is important does not imply that it is easy. As a matter of fact, the heart was rarely the first organ to be interrogated by new imaging techniques. There are several reasons why the heart is more difficult to image in comparison to other parts of the body, although the gravity of these limitations varies between modalities and applications. The most distinguishing characteristic of the heart is its perpetual movement, by contraction, but also as a result of respiration. To visualize the heart, images need to be taken very quickly (echocardiography) and the acquisition needs to be synchronized to the rhythm of the heart (CT, CMR, nuclear imaging), unless one is willing to accept the motion blurring when larger structures are investigated (nongated nuclear and CMR techniques). The heart’s position fairly deep within the body, protected by the rib cage, poses additional challenges, limiting the acoustic windows for echocardiography, creating excessive image noise on CT, reducing the radiofrequency signal for CMR, or causing attenuation artifacts on nuclear images. Respiratory motion is relevant for longer imaging protocols involving smaller structures. Particularly for angiographic studies using arterial contrast enhancement, short scans are preferable, necessitating very fast acquisition of imaging data.
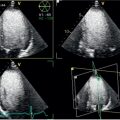
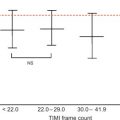
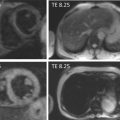
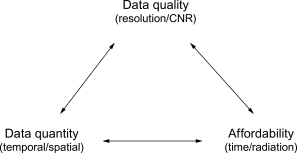
When imaging techniques are described, or perhaps compared, a number of image quality parameters are taken into account. The temporal resolution is the time needed to acquire a single image, which resembles the shutter time of an optical photo camera. Obviously fast-moving structures (valves) require a high temporal resolution. The scan time generally refers to the entire or a specific part of the examination. The spatial resolution refers to the ability to differentiate small structures, while the contrast resolution describes how well tissue types can be distinguished. Imaging of the coronary arteries or suspected endocarditis demands high spatial resolution, while myocardial infiltration benefits from high sensitivity to detect variation in tissue characteristics. Stochastic variance of the imaging signal, or irregularities arising elsewhere in the process, causes image noise. The noise level is often reported in relation to the image signal (signal-to-noise ratio) or (tissue) contrast (contrast-to-noise ratio). Performance parameters are interchangeable within a range, and trade-offs are often necessary ( Figure 1.2 ). During echocardiography, the sector width can be narrowed to increase the frame rate. During CMR, the spatial resolution can be increased, but at the price of a longer scan time. Reconstruction of thicker CT cuts will improve the contrast-to-noise ratio, but sacrifice in-plane spatial resolution. Particularly for techniques involving radiation, image quality needs to be balanced against radiation dose, and the challenge is to provide diagnostic image quality at the lowest possible dose.
1.3
Techniques
1.3.1
Echocardiography
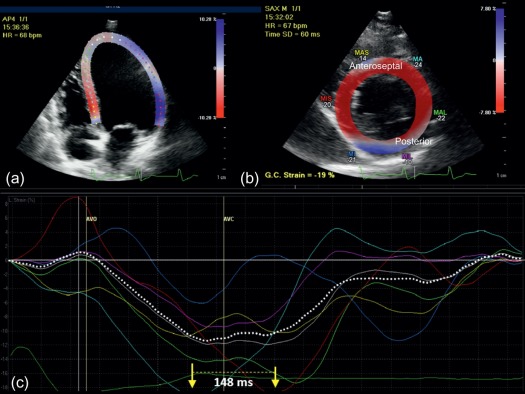
In the early 1950s, Edgler and Hertz described for the first time the use of cardiac ultrasound for assessing mitral valve movement. Since this landmark event, many discoveries have been made in the field of echocardiography that are presently used in daily practice. M-mode echocardiography was supplemented by 2D echocardiography in the mid 1960s, with the important additions of Doppler signals (1970s) and the combination of color Doppler (1980s) with 2D imaging. In the late 1980s, the transeosophageal approach completed the armamentarium of echocardiography. With the help of engineers, transeosophageal echocardiography quickly evolved from monoplane to biplane to present-day multiplane imaging. In parallel to the developments in transducer technology, image quality was consistently improved by using native second harmonic imaging and contrast agent. A significant step forward has been the development of 3D echocardiography and the possibility to quantitatively evaluate regional myocardial deformation by 2D/3D speckle tracking ( Figure 1.3 ). 3D echocardiography provides surgeons planning to repair a valve with images very similar to what they see at the time of surgery. Deformation imaging allows characterization of cardiac mechanics and detection of subclinical myocardial dysfunction. Echocardiography is harmless and combines low-cost high-quality technology with easy accessibility. It provides rapid quantitative information about cardiac structure and function at the bedside. It is the first-line imaging test in the diagnostic work-up and monitoring of most cardiac diseases.