BENIGN AND MALIGNANT PERIPHERAL NERVE SHEATH TUMORS
KEY POINTS
- Nerve sheath tumors are common benign tumors in the head and neck.
- Schwannomas and neurofibromas often have distinctive appearances.
- Malignant nerve sheath tumors are uncommon.
- These masses are associated with the relatively common genetic disorder neurofibromatosis type 1 and the less common neurofibromatosis type 2 and others.
INTRODUCTION
Prevalence and Etiology
The Schwann cell is of neuroectodermal, neural crest derivation and is the cell of origin of schwannomas and neurofibromas. Schwann cells are felt to be homologous to the oligodendroglia of the central nervous system. The distinction between neurofibromas and schwannomas is that neurofibromas have a mixed cell population and behave differently in their growth patterns from schwannomas.
These neurogenic tumors occur virtually anywhere that there are nerves. In particular, they involve the peripheral nerves of the head and neck and all cranial nerves except the olfactory. Autonomic nerves are involved as well. A significant proportion of all reported schwannomas are found in the head and neck region.1 Preferred sites in the head and neck include intracranial lesions as well as those arising from the vestibular division of the eighth cranial nerve (Fig. 29.1). Extracranially, the lateral neck is the most common site of presentation in those arising from spinal roots (Figs. 29.2–29.5), the vagus nerve (Figs. 29.6 and 29.7), and the sympathetic plexus2,3 (Fig. 29.8). Other sites of origin are less common and include the face, orbit (Fig. 29.9), scalp (Fig. 29.10), nasal and oral cavity (Fig. 29.11), parapharyngeal space (Fig. 29.12), and the facial nerve course through the temporal bone (Fig. 29.13). In the oral cavity, the tongue is the most common site of origin. In the larynx, the lesions are usually supraglottic and of the paraglottic space and/or aryepiglottic fold (Fig. 29.14). Posttraumatic “neuromas” can rarely manifest themselves as masses at the site of previous surgery or injury. These are disordered attempts at repair rather than true neoplasms.
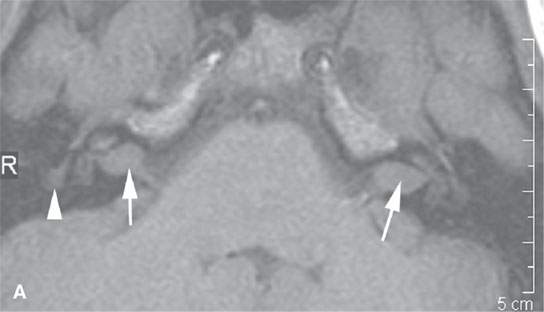
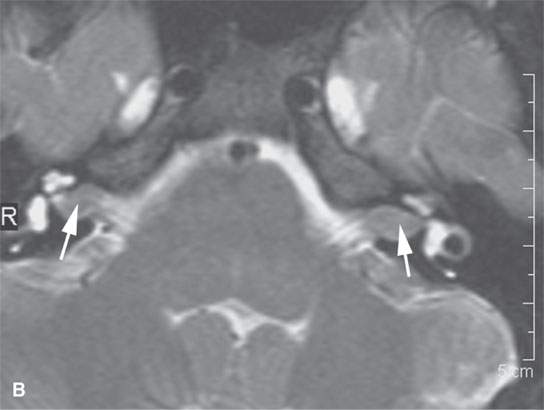
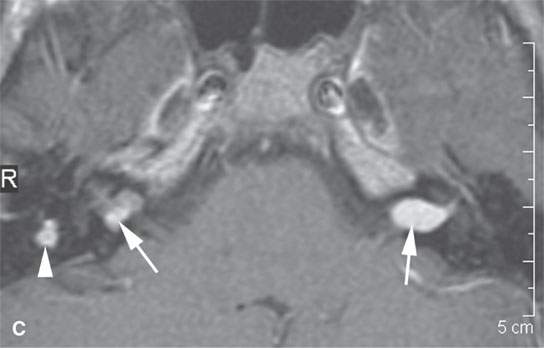
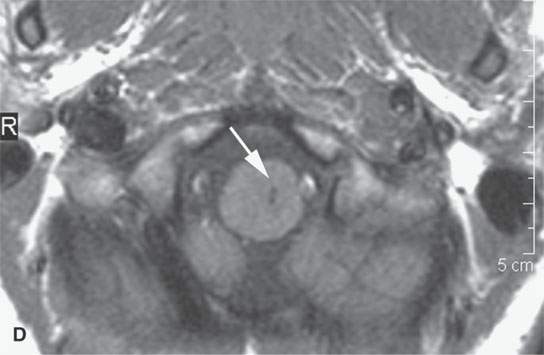
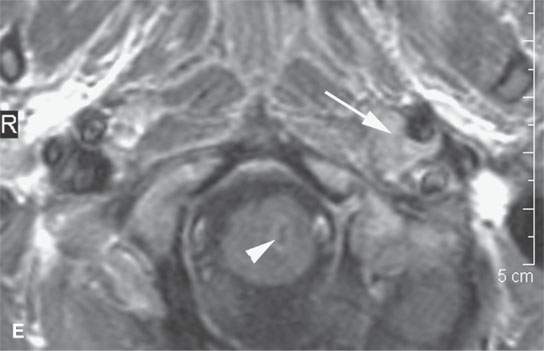
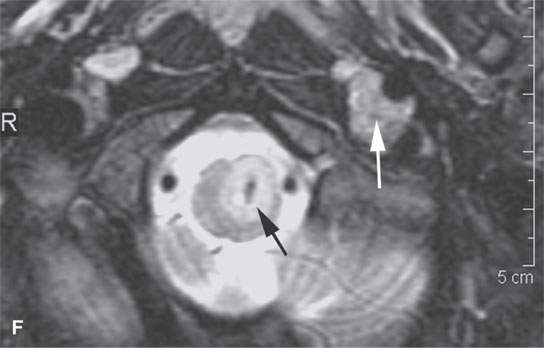
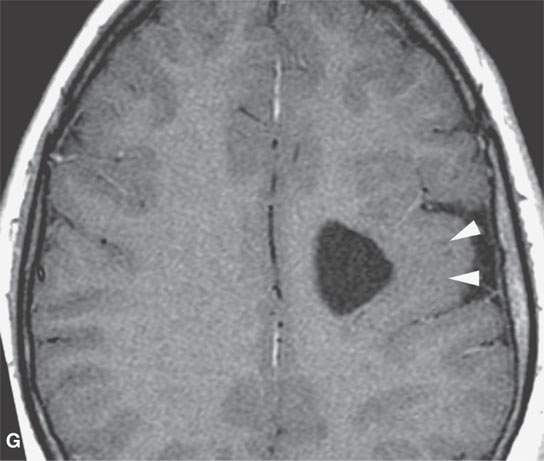
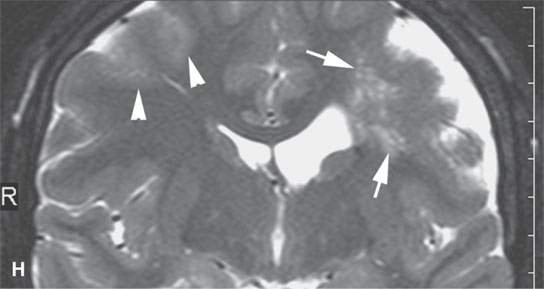
FIGURE 29.1. A patient with neurofibromatosis type 2. This magnetic resonance study illustrates findings commonly seen with that disease and the morphology of related nerve sheath tumors. A: Non–contrast-enhanced T1-weighted (T1W) image showing bilateral eighth cranial nerve schwannomas (arrows) and a facial nerve schwannoma (arrowhead). B: T2-weighted (T2W) image showing the bilateral eighth cranial nerve schwannomas equivalent in signal intensity to the brain. C: Contrast-enhanced T1W images showing the enhancement pattern of the eighth nerve schwannoma on the right to be somewhat different from that on the left (arrows) and enhancement of the facial schwannoma (arrowhead). D: T1W non–contrast-enhanced image shows an intra-axial lesion with a low signal intensity center within the medulla (arrows). E: Contrast-enhanced T1W image shows minimal enhancement of this relatively rarely associated low-grade glioma of the medulla (arrowhead shows a low signal intensity center). F: T2W image shows the periphery of the mass to be bright relative to brain and the center likely calcified based on low signal intensity on all images. G: Migrational abnormality of left frontal gray matter shown on a T1W image. H: Coronal T2W image showing migrational abnormalities of the left frontal region (arrows) to be more severe than those of the right frontal cortex (arrowheads).
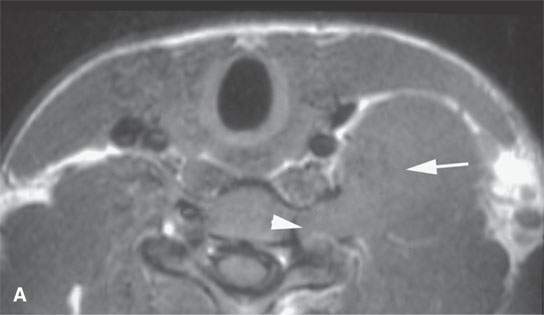
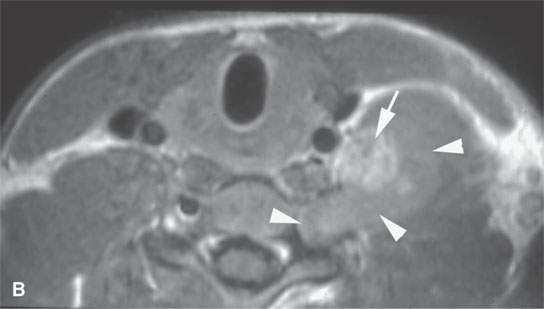
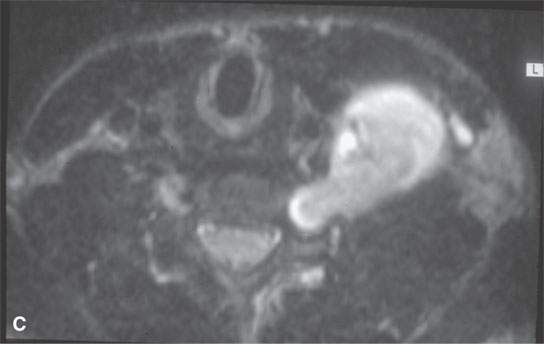
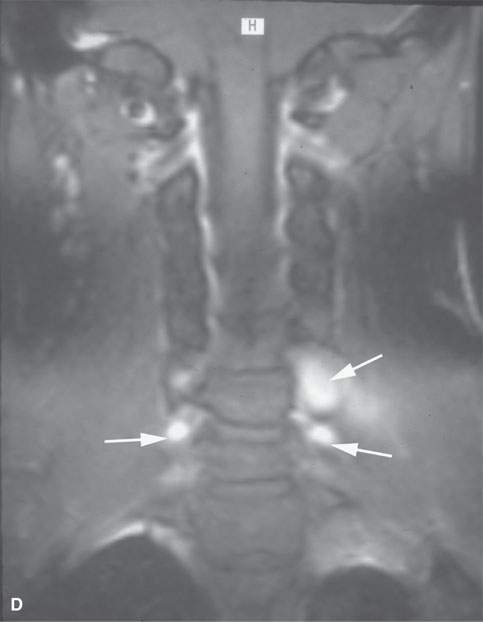
FIGURE 29.2. A patient presenting with a supraclavicular and left lower neck mass with no history of neurofibromatosis. Needle biopsy was unsuccessful. The patient was referred to our institution and had this magnetic resonance study. A: Posterior compartment mass obviously lies within the scalene muscles (arrow) and extends into the adjacent foramen (arrow) on this T1-weighted (T1W) non–contrast-enhanced image. B: Contrast-enhanced T1W image to compare with (A) shows central brisk enhancement (arrow) and less enhancement of the mass peripherally. C: T2-weighted image to correlate with (A) and (B) shows the more enhancing portion of the mass to be different in signal intensity compared to the less enhancing portion. D: Coronal T1W contrast-enhanced image shows multiple lesions confirming the diagnosis of neurofibromatosis type 1 unknown prior to this examination.
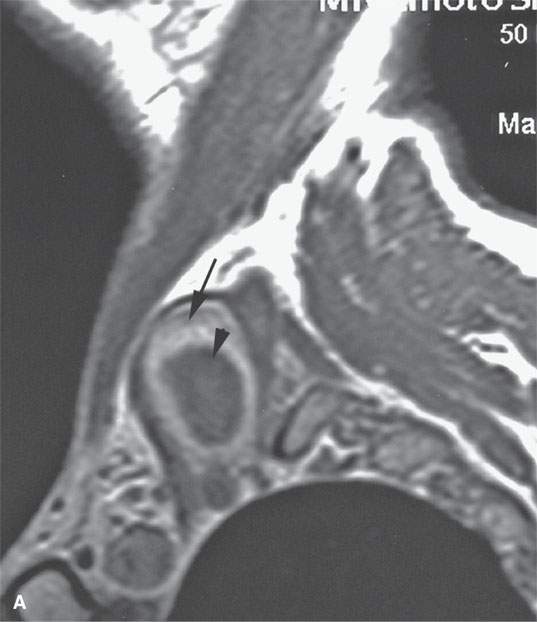
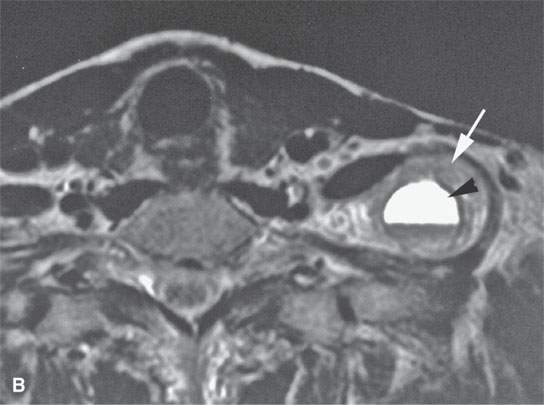
FIGURE 29.3. A patient with a low neck mass. A: T1-weighted sagittal image shows the mass within the scalene musculature with peripheral contrast-enhancing (arrow) and central nonenhancing component. B: Axial T2-weighted image shows the solid portion of the tumor peripherally more intense than muscle (arrow) and the central necrotic portion of the nerve sheath tumor with a fluid level likely due to prior hemorrhage.
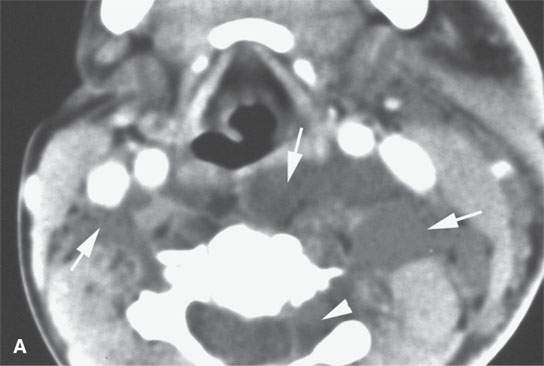
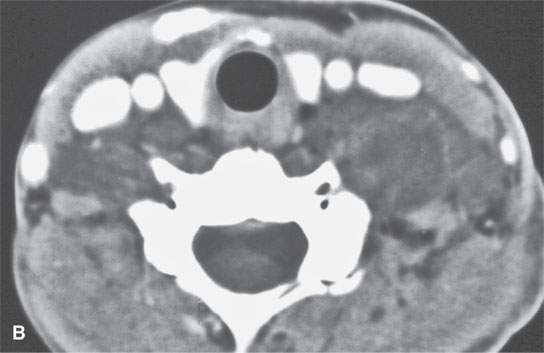
FIGURE 29.4. Contrast-enhanced computed tomography of a patient with neurofibromatosis type 1 showing essentially nonenhancing plexiform neurofibromas within the posterior compartment of the neck and extending posterior to the pharynx either in the retropharyngeal or prevertebral space or both (arrows). Extension along a nerve root sheath on the left is present in (A) (arrowhead). In (B), there is some slightly higher signal intensity in portions of the mass, but essentially they are nonenhancing and of almost fluid density.
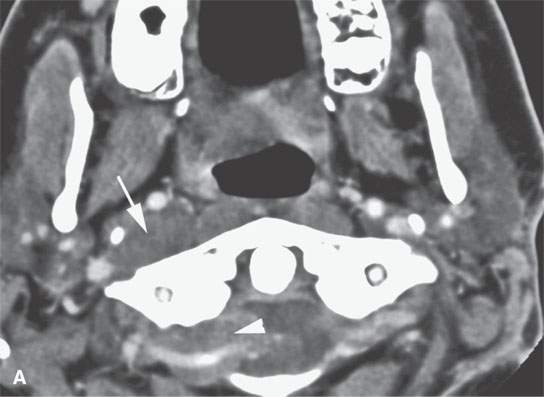
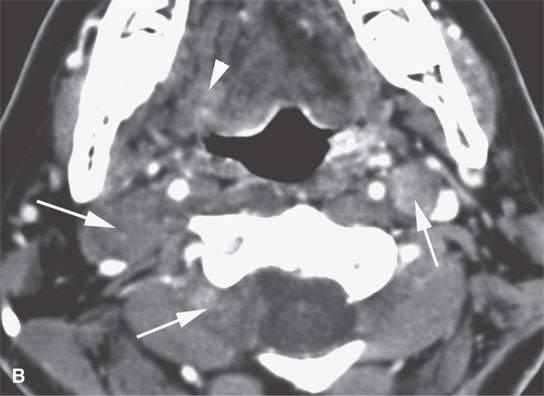
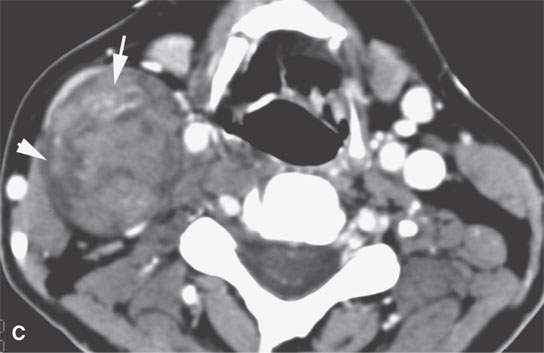
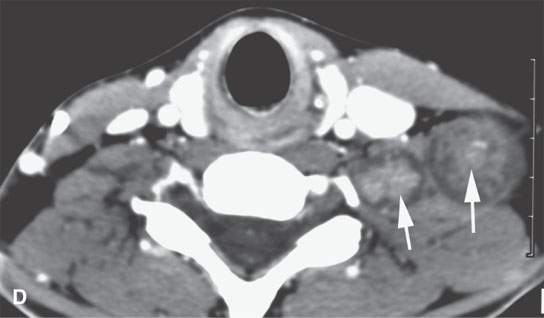
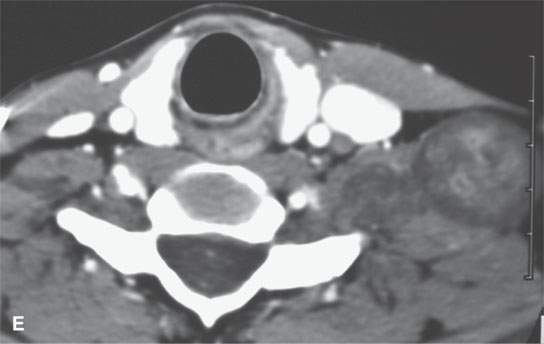
FIGURE 29.5. Contrast-enhanced computed tomography in a patient with neurofibromatosis type 1 demonstrates multiplicity and variable enhancement pattern of nerve sheath tumor. A: Non-enhancing tumors are present in the carotid sheath and retrostyloid parapharyngeal space on the right and into an adjacent neural foramen, likely a second lesion (arrows). B: Inferior continuation of the nerve sheath tumor, probably a neurofibroma that is nonenhancing and extending into the adjacent neural foramen; there is a second neurofibroma on the right showing minimal enhancement. There is a third lesion in the left carotid sheath showing some generalized low-grade enhancement (arrows show all findings). C: A large neurofibroma in the lateral neck affecting the carotid sheath possibly arising from the vagus nerve shows areas of enhancement (arrow) and lack of enhancement (arrowhead). D: An additional lesion in the upper brachial plexus on the left showing a dumbbell configuration within the neck and variable internal enhancement pattern. E: Inferior continuation of the lesion seen in (D) to demonstrate variability in enhancement pattern.
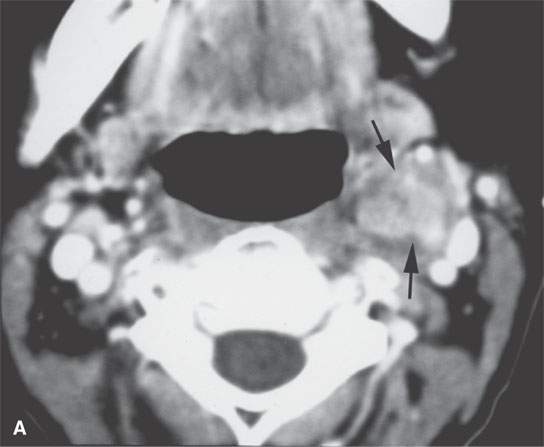
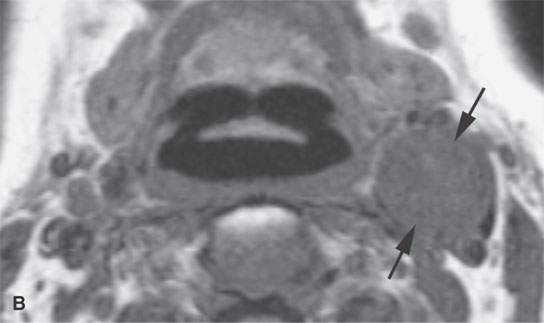
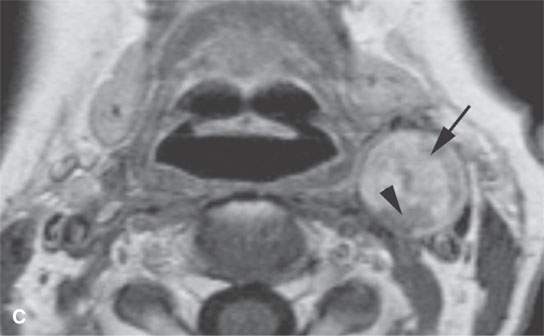
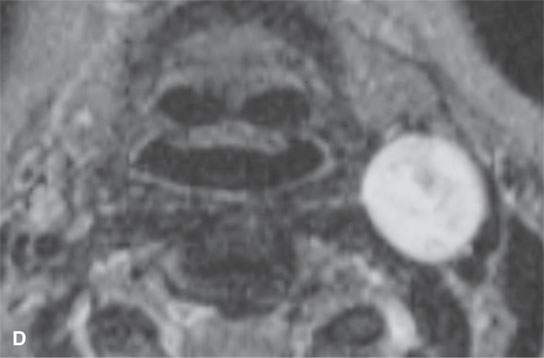
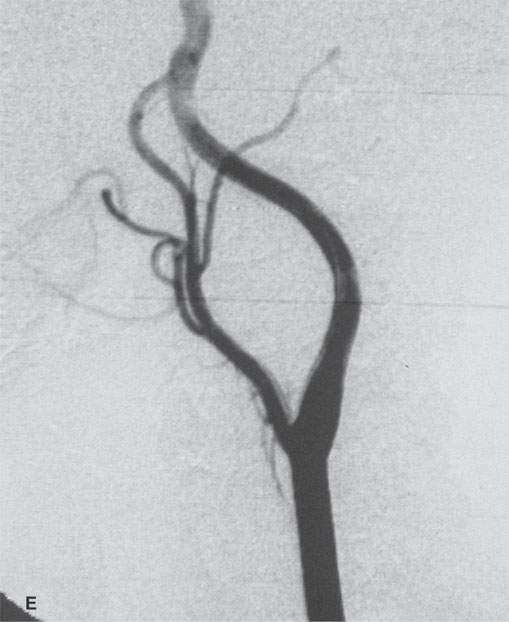
FIGURE 29.6. Contrast-enhanced computed tomography (CECT) and magnetic resonance imaging study in a patient presenting with a left level 2 mass. A: CECT shows a heterogeneous enhancing mass within the carotid sheath (arrows). B: T1-weighted non–contrast-enhanced MRI shows the mass to be homogeneously muscle equivalent. C:–Contrast-enhanced MRI shows relatively diffuse enhancement (arrow) with small zones of lack of enhancement (arrowhead). D: The mass appears to be homogeneously bright relative to fat on this T2-weighted image. E: Catheter angiogram shows no evidence of hypervascularity to suggest carotid body tumor. This was a schwannoma of the vagus nerve.
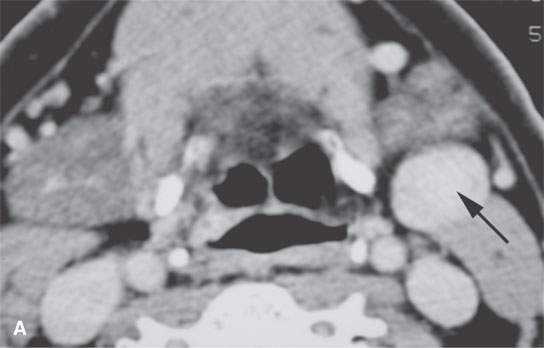
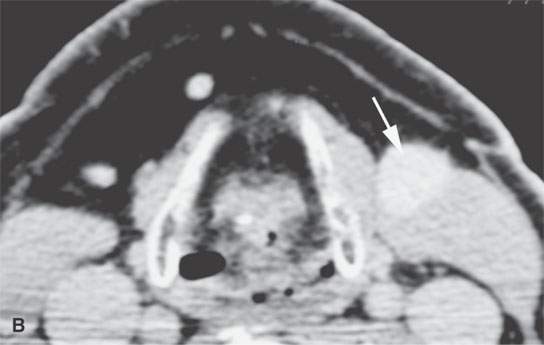
FIGURE 29.7. Contrast-enhanced computed tomography of a patient presenting with a level 2 neck mass. A homogeneously enhancing mass is seen in both (A) and (B) (arrows). The mass was removed, and diagnosis was an ancient schwannoma. This mass had been present for many years and had not changed in size.
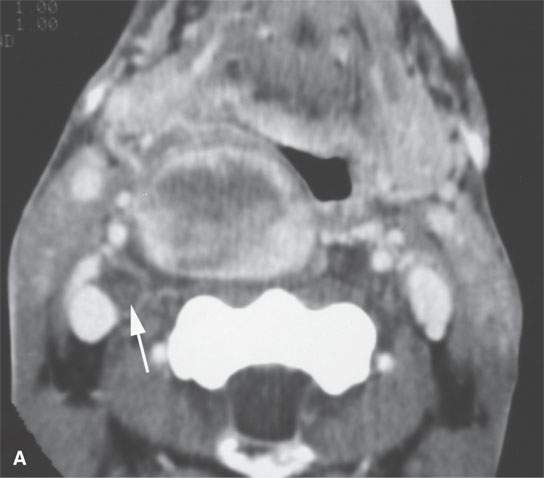
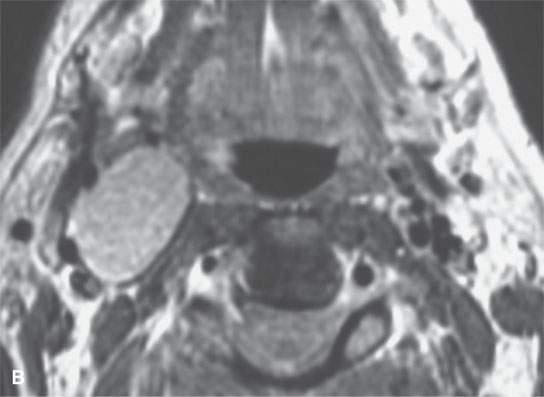
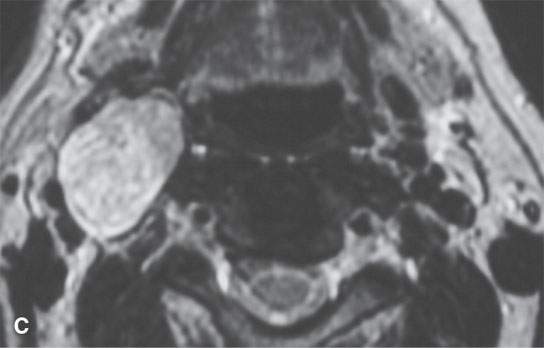
FIGURE 29.8. Two patients with schwannomas arising from the sympathetic plexus. A: Contrast-enhanced computed tomography shows an obviously enhancing mass medial to the carotid artery projecting into the retropharyngeal space. A second smaller, nonenhancing mass (arrow) is present; this confirmed neurofibromatosis. The larger lesion was of the sympathetic plexus. The smaller was of the vagus nerve. B, C: A second patient with a sympathetic schwannoma. Contrast-enhancedT1-weighted image (B) showing the mass displacing the carotid artery laterally along with styloid musculature localizing the lesion to the expected course sympathetic plexus.T2-weighted image (C) showing the mass to be homogeneously bright relative to fat typical of schwannoma. Surgery confirmed schwannoma of the sympathetic plexus.
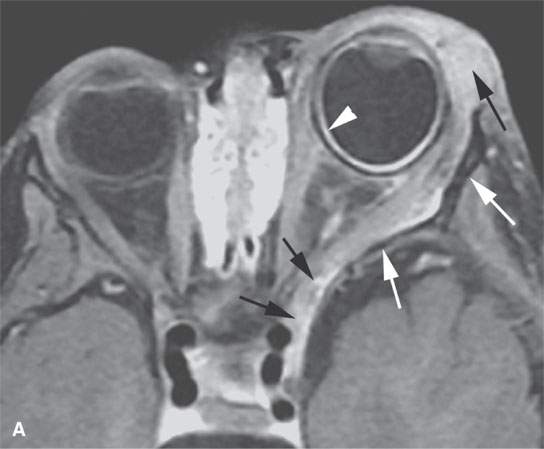
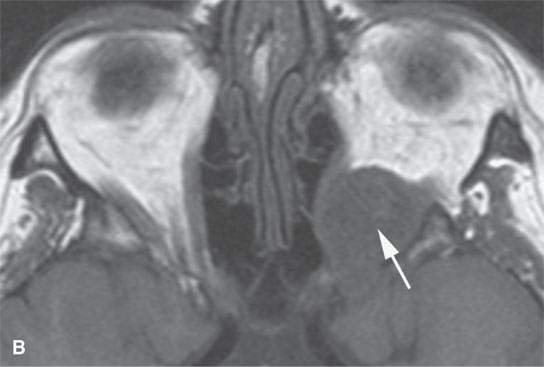
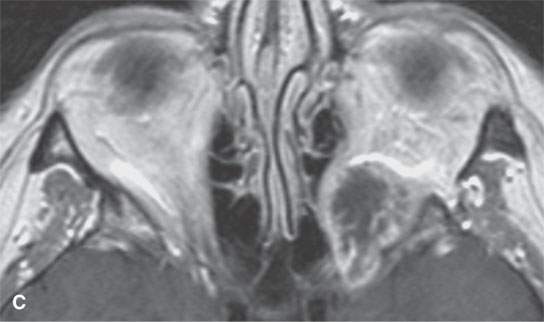
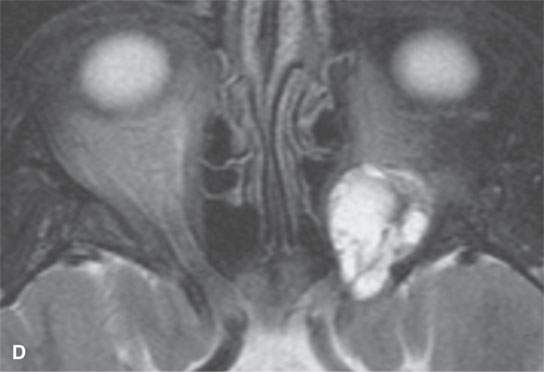
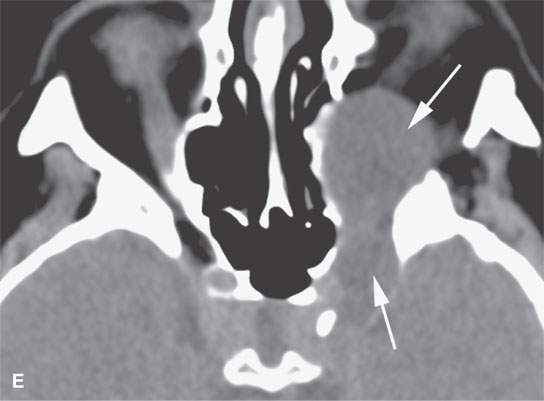
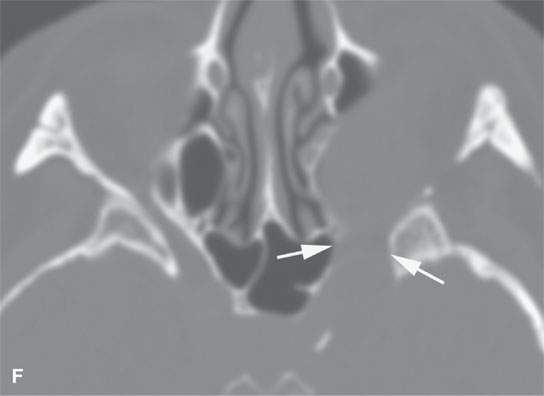
FIGURE 29.9. Multiple nerve sheath tumor patients with the masses involving the orbit. A:–Contrast-enhanced T1-weighted (T1W) magnetic resonance of the most frequent orbital involvement with nerve sheath tumors—that of a patient with neurofibromatosis type 1. The bony orbit is dysplastic (white arrows). A plexiform neurofibroma grows from the preseptal soft tissue region anteriorly and laterally to the orbital apex junction with the anterior cavernous sinus (black arrow). The eye is buphthalmic, and there is a cyclitic membrane present (white arrowhead). B–F: A patient with a schwannoma at the orbital apex.T1W non–contrast-enhanced image (B) shows a homogeneous mass of slightly diminished signal intensity compared to brain (arrow).Contrast-enhanced T1W image (C) shows mainly peripheral enhancement.Correlating T2-weighted (T2W) image (D) shows the more solid peripheral enhancing component to be lower in signal intensity than the nonenhancing more central cystic component. Non–contrast-enhanced computed tomography&(E, F) showing the homogeneous-appearing mass causing remodeling of the bone around the orbital apex (arrows) in a pattern consistent with a benign slow-growing lesion.
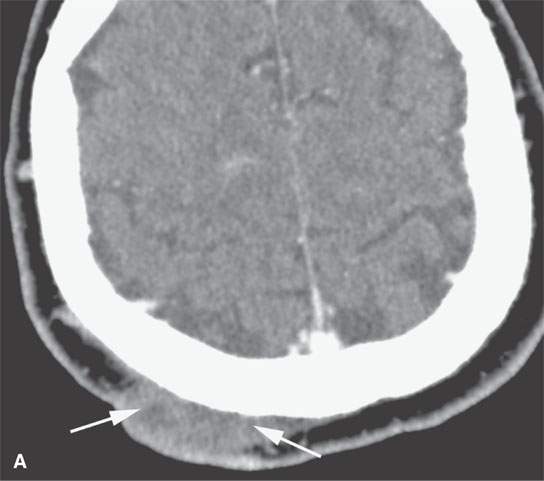
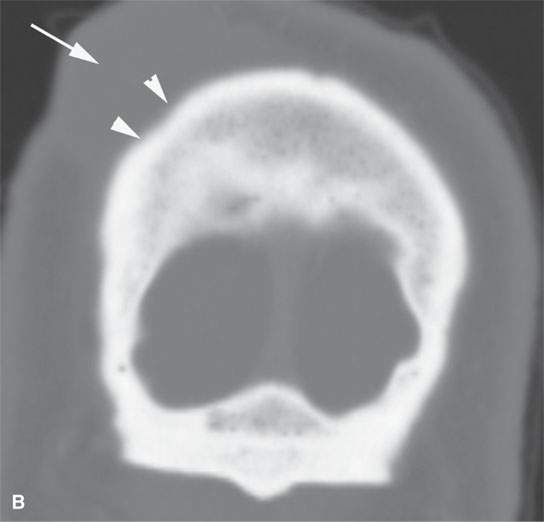
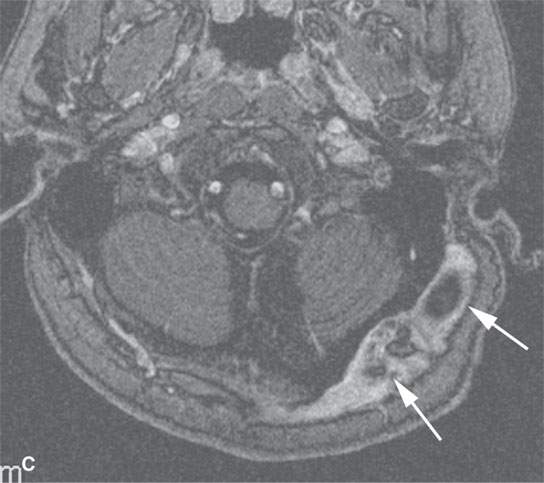
FIGURE 29.10. Imaging studies of patients with nerve sheath tumors of the scalp. A, B: Computed tomography examinations showing a neurofibroma in the scalp (A) with remodeling of underlying bone (arrowheads). C: T1-weighted contrast-enhanced image showing a plexiform neurofibroma in the scalp (arrows) causing remodeling of the underlying skull.
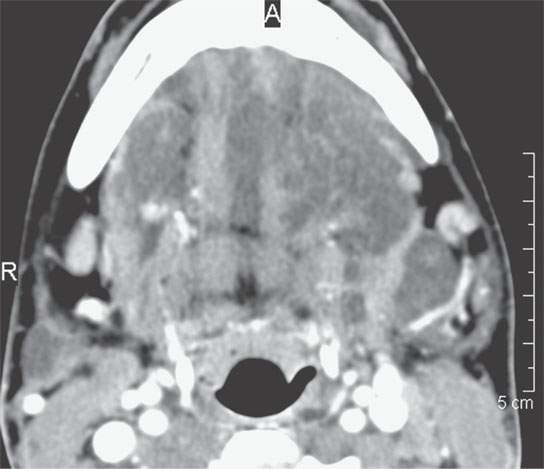
FIGURE 29.11. Contrast-enhanced computed tomography showing plexiform neurofibroma of the oral cavity, floor of the mouth, and submandibular space, which shows little if any enhancement.
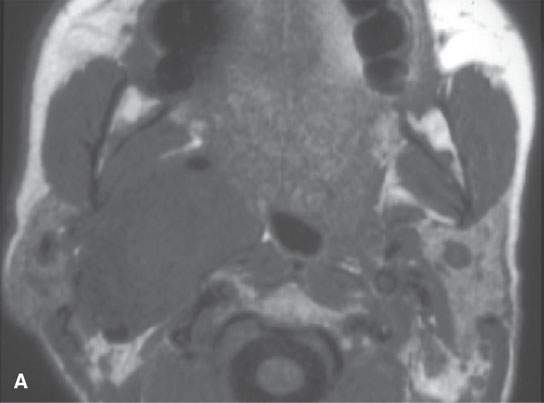
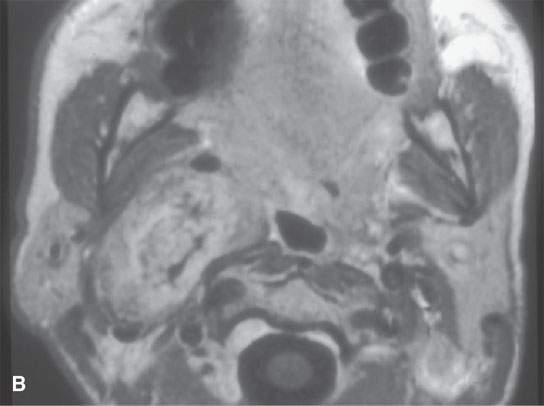
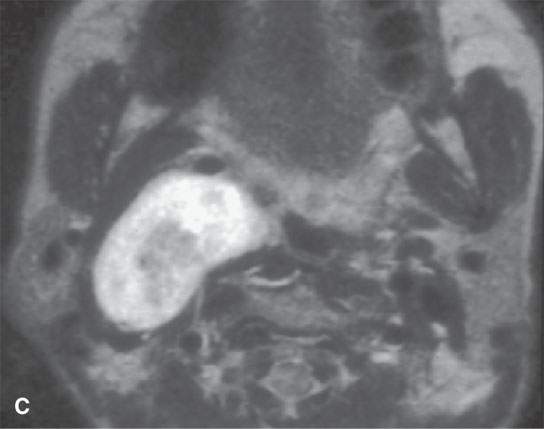
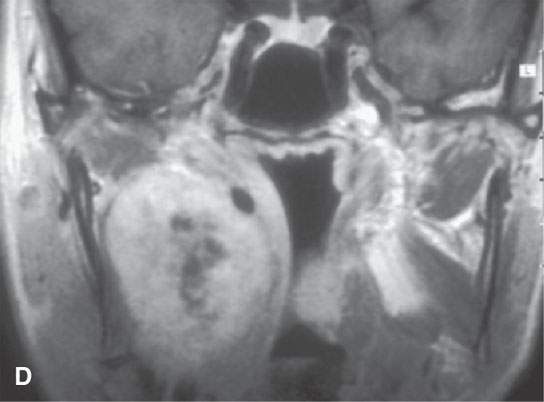
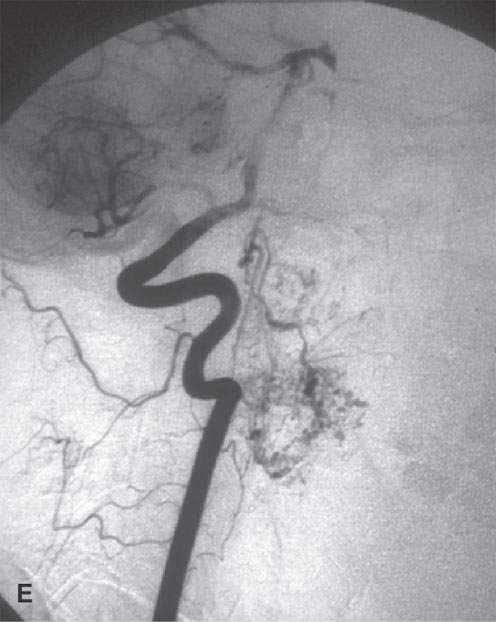
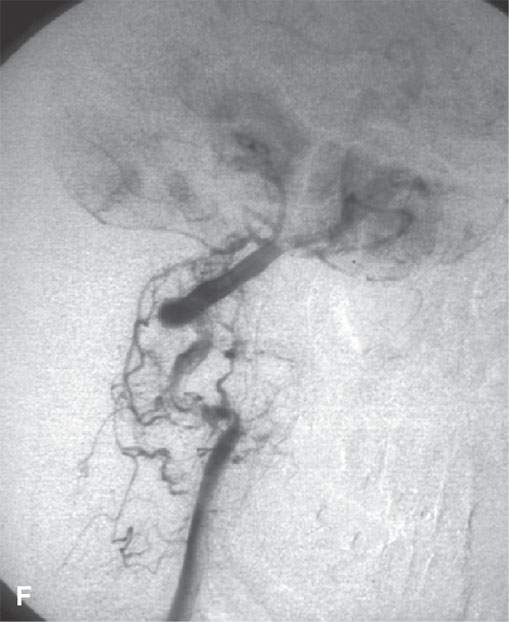
FIGURE 29.12. Schwannoma of the retrostyloid parapharyngeal space. A: T1-weighted (T1W) non–contrast-enhanced image. B: Contrast-enhanced T1W image shows the mass to enhance and displace the carotid artery anteriorly, the jugular vein posteriorly, and the styloid musculature laterally. C: T2-weighted image to correlate with (B). D: Coronal T1W contrast-enhanced image shows inhomogeneity centrally within the mass as seen in (B) suggesting either a prominent vascular pedicle and/or some fibrosis within the lesion. E, F: &Catheter angiogram showing the mass to be relatively hypervascular and to have several prominent vascular pedicles. This raises the possibility of a malignant nerve sheath tumor, but this tumor was excised and was entirely benign histologically.
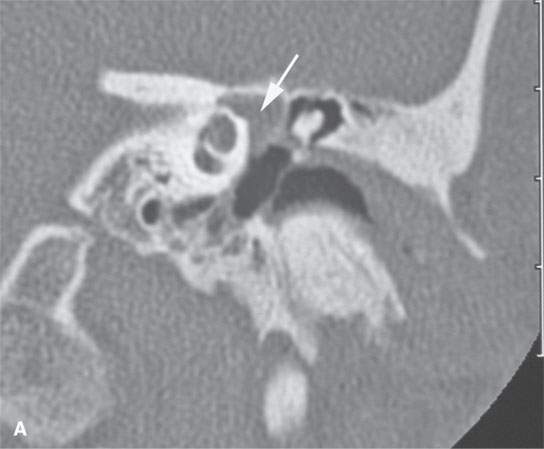
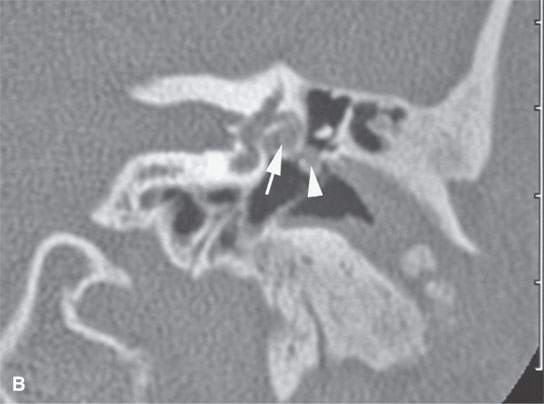
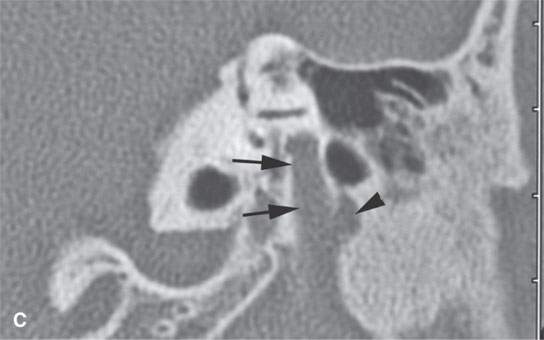

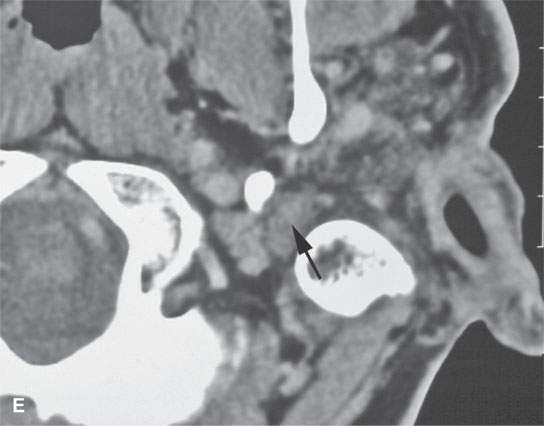
FIGURE 29.13. Plexiform neurofibroma of the facial nerve within the temporal bone.Contrast-enhanced computed tomography study using both soft tissue and bone reconstructions. A: The plexiform neurofibroma involves the first genu of the facial nerve (arrow). B: There is marked enlargement of the tympanic segment of the facial canal (arrow) as well as enlargement of the chorda tympani branch within the middle ear (arrowhead). Also, note the dystrophic calcification and changes in the external auditory canal, which is filled with soft tissues due to an adjacent plexiform neurofibroma and dysplastic bony changes. C: The plexiform neurofibroma enlarges the main portion of the descending facial canal (arrows) as well as an adjacent canal associated with a branch of the nerve (arrowhead). D: Below the stylomastoid foramen, the facial nerve is greatly thickened within that fat pad (white arrow), and the main trunk of the facial nerve is more than ten times its normal size (arrowheads) with its course typically identified just lateral to the retromandibular vein (black arrow). E: The enlarged nerve still visible just below the digastric groove (arrow).
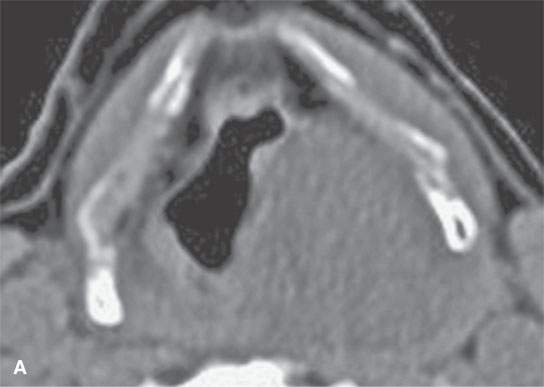
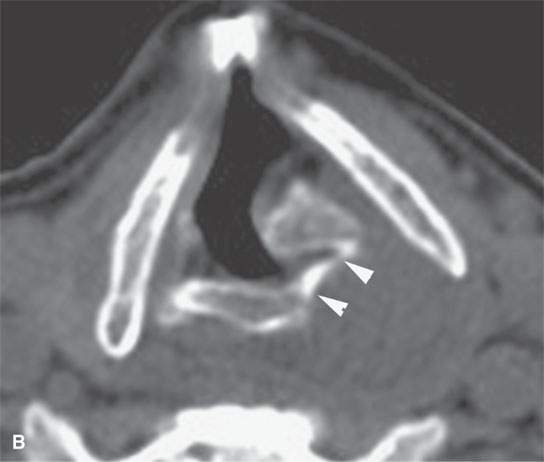
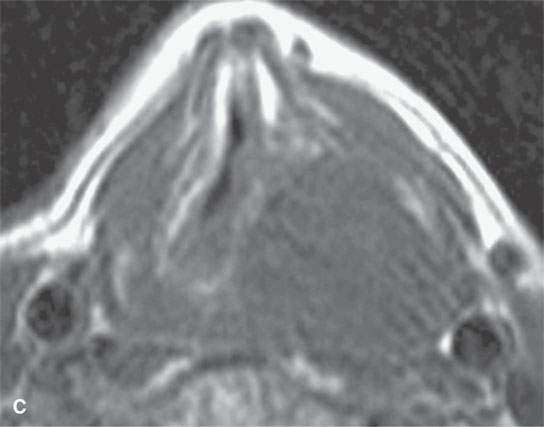
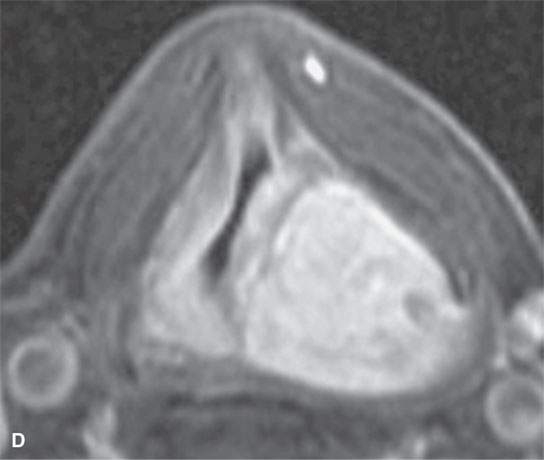
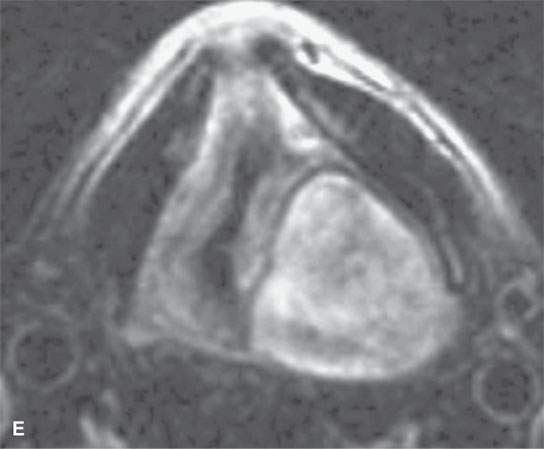
FIGURE 29.14. Schwannoma of the larynx arising from the aryepiglottic fold. A: Non–contrast-enhanced CT image. B: Non–contrast-enhanced CT at the level of the pyriform sinus apex showing remodeling of the cricoid cartilage in the region of the cricoarytenoid joint (arrowheads). C: Non–contrast-enhanced T1W image. D: Contrast-enhanced fat-suppressed T1W image showing the mass at the lower supraglottic region just above the pyriform sinus apex to homogeneously enhance. E: T2-weighted image showing internal characteristics consistent with schwannoma.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








