Normal Anatomy and Imaging Techniques
The normal anatomy and configuration of the heart on a chest x-ray and on a computed tomography (CT) scan were discussed in Chapter 3 . Imaging of the heart also can be done with magnetic resonance imaging (MRI). This modality provides good visualization of the cardiac anatomy. The lungs are not well seen on these scans because respiratory motion causes image degradation. The anatomy of the heart at several different levels on an MRI scan is shown in Fig. 5.1 . Computed tomography (CT), magnetic resonance (MR), and nuclear medicine images can be gated to the cardiac cycle, allowing images to be produced in systole and diastole, as well as in the phases in between ( Fig. 5.2 ). Transthoracic ultrasound (echocardiography) also can be used to image through those portions of the heart that are in contact with the chest wall. This method is generally considered within the practice of cardiologists and is discussed here only when it is the appropriate test to order.


Imaging of the peripheral vascular system has changed dramatically over the last several decades. Historically, good spatial resolution was achieved only with invasive techniques that used direct arterial access and the injection of contrast material through a catheter. With the advent of faster CT and MRI scanners, both venous and arterial anatomy can be visualized adequately for most diagnostic purposes. Even though CT and MRI scans are typically displayed as slices of the anatomy, the vascular image data are often manipulated to display rotating three-dimensional images of the vascular anatomy. Invasive procedures are normally reserved for therapeutic intervention (such as balloon dilation of a stenosis or stent placement). Appropriate imaging indications for cardiovascular problems are shown in Table 5.1 .
| Clinical Problem | Imaging Study |
|---|---|
| Most cardiac problems | Initial posteroanterior and lateral chest radiography |
| Congestive heart failure (new or worse) | Chest radiography and ejection fraction; wall motion evaluation by nuclear medicine or echocardiography |
| Congestive heart failure (chronic) | Chest radiography |
| Hypertension (suspected essential) | No imaging indicated |
| Hypertension (suspected renal artery stenosis) | Nuclear medicine captopril renogram or MR angiogram |
| Left ventricular ejection fraction | Nuclear medicine multiple gated acquisition study or echocardiography |
| Chest pain or shortness of breath (suspected pulmonary embolism) | Chest x-ray and CT angiogram (if pregnant, initially chest x-ray and lower extremity Doppler ultrasound) |
| Shortness of breath (suspected cardiac origin) | Chest x-ray and transthoracic echocardiography |
| Blunt chest trauma (suspected aortic injury) | Chest x-ray, CT angiogram |
| Acute chest pain | |
| Suspected myocardial infarction | Electrocardiography, chest radiography, coronary angiography |
| Suspected myocardial ischemia (acute coronary syndrome) | Electrocardiography, cardiac biomarkers, nuclear medicine SPECT, myocardial perfusion at rest, stress or coronary angiography |
| Suspected aortic dissection | Chest x-ray, CT or MR angiogram of chest and abdomen |
| Nonspecific; low probability of coronary disease | Electrocardiography, chest x-ray, CT angiogram of coronary arteries or chest, transthoracic echocardiography; can be done sequentially and are nonoverlapping |
| Chronic chest pain | |
| Low to intermediate probability of coronary disease | Chest x-ray, transthoracic echocardiography or nuclear medicine cardiac perfusion scan; CT angiogram of chest to exclude PE, aneurysm, and lung pathology |
| High probability of coronary disease | Nuclear medicine cardiac perfusion scan at rest and stress or coronary angiogram or transthoracic echocardiography |
| Coronary ischemia | Electrocardiography; if negative, then stress electrocardiogram, nuclear medicine, myocardial perfusion study, or stress echocardiogram; if positive, then coronary angiogram |
| Congenital heart disease | Chest x-ray, resting transthoracic echocardiography |
| Endocarditis | Resting transthoracic echocardiography |
| Valvular disease | Echocardiography |
| Pericardial effusion | Echocardiography |
| Constrictive pericarditis | Echocardiography; if equivocal, then CT |
| Aortic trauma | Angiography or CT with contrast |
| Thoracic aortic dissection | CT with IV contrast or transesophageal ultrasonography |
| Abdominal aortic aneurysm | |
| Symptomatic | CT with IV contrast or MRA of abdomen, with and without IV contrast |
| Asymptomatic | Ultrasonography for screening; ultrasound or noncontrast CT for follow-up |
| Suspected mesenteric ischemia | CTA of abdomen and pelvis with IV contrast |
| Deep venous thrombosis | Duplex ultrasonography |
| Sudden painful cold leg | Digital subtraction arteriography if clinical suspicion of arterial obstruction is high or moderate; CT angiogram or MR angiogram if is suspicion is low |
| Carotid bruit | Duplex ultrasonography; if high-grade stenosis, then contrast angiography |
| Claudication | Doppler ultrasonography of lower extremity |
| Penetrating neck injury | CTA of neck with IV contrast |
Evaluation of the Cardiac Silhouette
Generalized Cardiomegaly
Examination of the shape of the heart on a chest x-ray can sometimes provide clues to the type of cardiac disease present. If the heart appears large in most dimensions, it is often difficult to tell whether multichamber enlargement, myocardiopathy, or pericardial effusion is present. If acute (within several days) and marked enlargement of the cardiac silhouette is seen, the most likely diagnosis is a pericardial effusion. Under these circumstances, the heart has a pendulous appearance and is much wider at the base. This is often referred to as a water bag appearance ( Fig. 5.3 ). Pericardial effusions must be greater than 250 mL to be detectable radiographically. Effusions are sometimes visible on CT scans of the chest, but if you suspect a pericardial effusion, the imaging procedure of choice is echocardiography. After penetrating trauma or surgery, air may be seen within the pericardium ( Fig. 5.4 ).


Constrictive pericarditis is most commonly due to tuberculosis and viral and pyogenic infections. It also may occur after radiation therapy. Of patients with constrictive pericarditis, 90% will have pericardial calcification, which may be visible only on CT, and 60% will have a pleural effusion. Of those patients with pericardial calcification, 50% also will have constrictive pericarditis.
Cardiomegaly can be due to valvular disease, cardiomyopathy, congenital heart disease, pericardial effusion, or mass lesions. Cardiomyopathy and pericardial effusion both generally lead to symmetric enlargement, whereas valvular disease and congenital heart disease often have specific chamber enlargement. Dilated cardiomyopathy is caused by ineffective contraction during systole and most commonly results from an infection or a metabolic disorder. It also may be caused by collagen vascular disease or toxic agents such as alcohol and chemotherapeutic drugs. An example of the latter is doxorubicin (Adriamycin), one of the most widely used chemotherapeutic agents ( Fig. 5.5 ).

Use of the cardiothoracic ratio to assess heart size and the effect of cardiac failure on the appearance of the pulmonary vessels and lungs was discussed in Chapter 3 . The width of the heart should not exceed half the width of the chest at its widest point. This measurement is reliable only on an upright posteroanterior (PA) chest image; on an anteroposterior (AP) chest x-ray, the heart will often exceed this measurement, owing to magnification. On a supine image, there is even more magnification, and high position of the hemidiaphragms occurs. This high position will push the heart upward and outward, making it appear wide. A note of caution should be inserted here about patients who have chronic obstructive pulmonary disease (COPD). The shape of the heart is determined by external forces and internal factors. One factor relates to the level of the hemidiaphragms. The measurement of cardiothoracic ratio assumes that the hemidiaphragms are in normal position. With COPD, the hemidiaphragms are driven inferiorly (often to the level of the posterior 12th rib). The heart then sags and elongates. This can make an enlarged heart appear normal in size, especially considering the cardiothoracic ratio. It follows, then, that if the heart appears too wide in a patient who has COPD, it is really very large.
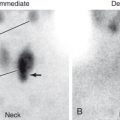
Because assessment of cardiac function by chest x-ray is rather poor, quantitative evaluations of cardiac ejection fraction are usually made by nuclear medicine multiple gated acquisition (MUGA) scanning, gated single-photon emission CT (SPECT) studies, or echocardiography. In the nuclear medicine MUGA procedure, red cells are labeled with radioactive material, and images of the heart are obtained in a gated fashion. Computer analysis enables construction of a time-activity curve showing the amount of activity in the left or right ventricle in both diastole and systole, allowing for the calculation of an ejection fraction. The normal left ventricular ejection fraction (LVEF) is between 55% and 75%. In older persons, the lower limit of LVEF is probably about 50%. Both nuclear medicine gated SPECT ( Fig. 5.6 ) and echocardiography produce visualization of the myocardium. The ventricular cavity is then measured at various portions of the cardiac cycle, and the ejection fraction is calculated. All these studies also can detect regional wall motion abnormalities.

Left Atrial Enlargement
Isolated left atrial enlargement occurs most commonly in mitral stenosis. The earliest sign is displacement of the esophagus posteriorly ( Fig. 5.7A ). Enlargement of the left atrial appendage on the PA view is the next sign to appear (see Fig. 5.7B ). As the left atrium enlarges further, the esophagus becomes more posteriorly displaced, splaying or widening of the inferior carinal angle is seen, and the enlarged left atrium can be seen on the PA x-ray as a double density behind the heart and below the carina (see Fig. 5.7C ). The normal inferior carinal angle should not exceed 75 degrees.

Rheumatic heart disease most often affects the mitral valve and, to a lesser extent, the aortic valve. The classic appearance of a mitral heart on a PA chest x-ray is easily recognized by four bumps along the left cardiac border. This also is sometimes called the ski mogul heart . Going from superior to inferior, the bumps represent the aortic arch, pulmonary artery, left atrial appendage, and left ventricle (see Fig. 5.7B ). Left atrial enlargement also is seen with congenital cardiac lesions that have intracardiac shunts, as well as in patients who have left ventricular failure.
As rheumatic heart disease progresses, mitral stenosis and mitral insufficiency develop. The heart becomes very large because of dilatation and hypertrophy of the left ventricle. In the combined form of mitral disease, the left atrium becomes even larger than what is seen in mitral stenosis alone. Typical findings are a straightening of the left cardiac border due to left atrial enlargement, left ventricular enlargement, as evidenced by leftward and downward displacement of the cardiac apex and, if left ventricular dilatation becomes massive, rightward displacement of the right ventricle. On the lateral view, in addition to the obvious left atrial enlargement, the posterior displacement of the heart continues down inferiorly, indicating left ventricular enlargement as well. In severe mitral disease, the mitral valve and aortic and tricuspid valves are affected. In general, the manifestations of the more proximal valve lesion are the most prominent. With mitral and tricuspid disease, enlargement of the left atrium, left ventricle, right atrium, and right ventricle occurs.
Many radiologists say that you cannot differentiate right atrial from right ventricular enlargement on a chest x-ray, and this is probably true. Fortunately, in most adults, when one of the right chambers is enlarged, so is the other. On the frontal chest x-ray, right atrial enlargement is suggested by an increased convexity of the right heart border. Isolated right ventricular enlargement is very difficult to appreciate because it overlaps the right atrium and left ventricle on the frontal view. On the lateral view, both right ventricular and right atrial enlargement will cause a filling in of the anterior clear space behind the sternum ( Fig. 5.8 ). Normally, on the lateral view, the anterior portion of the heart fills in only approximately one-third or less of the anterior clear space unless enlargement of the right atrium or right ventricle is found.

Prosthetic tricuspid and mitral valves are often used for the treatment of rheumatic heart disease. You should be able to recognize these valves by their size, location, and orientation ( Fig. 5.9 ). The valve with the largest area is the tricuspid valve, the mitral valve is intermediate in size, and the smallest is the aortic valve. You also should be able to recognize prosthetic mitral and tricuspid valves. As expected, the mitral valve is located posteriorly and to the left in the heart, and the tricuspid valve is anterior and toward the right side.

Left Ventricular Enlargement
On a frontal chest x-ray, left ventricular enlargement, as already mentioned, produces a round left cardiac border as well as downward displacement of the apex. On the lateral view, the posterior aspect of the heart, where it intersects the hemidiaphragm, is usually posteriorly displaced behind the inferior vena cava. The Hoffman-Rigler sign also can be used. To use this, find the intersection of the inferior vena cava with the hemidiaphragm on the lateral image, and then measure 2 cm up and 2 cm back. If the heart projects posteriorly, left ventricular enlargement probably is present. A note of caution should be inserted here because an enlarged right heart can sometimes push the left ventricle back. To exclude this, look at the space behind the sternum: only the lower one-third should be filled by soft tissue.
Left ventricular dilatation can be due to a number of causes, including coronary artery disease, aortic stenosis, and aortic regurgitation. You should take care to consider the possibility of a left ventricular aneurysm before you suggest left ventricular enlargement and quit. Ventricular aneurysms most commonly occur near the apex and anteriorly and have a high rate of mortality. Left ventricular hypertrophy is difficult to detect radiographically. It may be present in patients who have a normal cardiac configuration on chest x-ray. If this is suspected, an echocardiogram (ultrasound) is the test of choice.
Aortic Stenosis and Insufficiency
Aortic stenosis is most commonly valvular, although in a smaller number of patients, it may be either subvalvular or supravalvular. Valvular stenosis can be due to rheumatic heart disease, a bicuspid (rather than tricuspid) aortic valve, or degenerative changes (usually in patients older than 70 years). It may be difficult to detect this condition from findings on a plain x-ray of the chest, and sometimes the only finding is a calcified aortic valve. Initially, with aortic stenosis, left ventricular hypertrophy is noted. The heart will be normal in size and may show a slight rounding of the cardiac apex. When left ventricular dilatation occurs, the left cardiac border elongates and the apex of the heart moves downward toward the left hemidiaphragm. The aortic knob will be normal in size, although the ascending aortic arch is enlarged, causing a convexity of the right upper cardiac margin. The enlargement of the ascending aorta is due to poststenotic dilatation.
With aortic insufficiency, the left ventricle becomes much larger and, on a PA chest x-ray, the apex of the heart may project below the most superior portion of the left hemidiaphragm. The ascending aorta still shows some enlargement ( Fig. 5.10 ). Prosthetic aortic valves are relatively easy to recognize by their relatively small size and their location at the root of the ascending aorta ( Fig. 5.11 ).


Pulmonary Artery Enlargement
Enlargement of the pulmonary artery is fairly easy to recognize on the PA chest x-ray by a bulging along the left cardiac border, just below the aortic arch ( Fig. 5.12 ). Pulmonary artery enlargement can be due to a number of causes, but probably the three most common are pulmonic stenosis (with poststenotic dilatation), pulmonary artery hypertension, and abnormalities in which increased flow through the pulmonary artery occurs, such as a patent ductus arteriosus or an atrial septal defect (ASD).

If enlargement of both the left and right main pulmonary arteries is present, consider the diagnosis of pulmonary arterial hypertension. In this entity, in addition to the very large central pulmonary arteries, rapid “pruning” of the vessels occurs as they proceed peripherally in the lung. Even though the central vessels are extremely large, it is unusual to be able to see vessels at the edge of the lung. The chest x-ray is relatively insensitive for detecting mild or moderate pulmonary hypertension, but it is still the recommended initial recommended imaging test. Pulmonary hypertension is a complex disorder and may be idiopathic or due to a number of causes, including ASD or ventricular septal defect (VSD), patent ductus arteriosus, arteriovenous shunt, left ventricular failure, mitral valve disease, pulmonary emboli, parenchymal lung disease, COPD, and other less common entities. Exertional dyspnea is the most frequent presenting symptom but also may be accompanied by syncope, fatigue, weakness, angina, and peripheral edema.
Congenital Cardiac Disease
Rather than including every entity, I present a few examples here to give you an approach to interpretation. Several important factors to assess in the evaluation of congenital cardiac disease include the age of the individual, the clinical findings, such as murmurs, whether the patient is cyanotic or acyanotic, specific chamber enlargement, and pulmonary vascularity (increased, decreased, or normal).
Probably the easiest place to begin is to determine whether or not the individual is cyanotic. A cyanotic infant who has normal or decreased pulmonary vascularity and a normal heart size probably has a tetralogy of Fallot. Tetralogy of Fallot includes pulmonic stenosis, VSD, an overriding aorta, and right ventricular hypertrophy. On the x-ray, decreased pulmonary vascularity and a boot-shaped heart with an uplifted apex and a concavity along the left cardiac border are seen ( Fig. 5.13 ). If cardiomegaly with right atrium enlargement is noted, the differential diagnosis includes Ebstein malformation, tricuspid atresia, and pulmonic atresia. In Ebstein anomaly, a giant right atrium appears, with a shoulder along the right side of the heart and a very small pulmonary artery. In this entity, downward displacement of the tricuspid valve occurs, with the right ventricle being partially atrialized ( Fig. 5.14 ).


Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree