10 Carotid Occlusion, Unusual Pathologies, and Difficult Carotid Cases
We emphasize the typical appearance and Doppler characteristics of these uncommon and rare cases.
Carotid Occlusion
Distinguishing a complete carotid artery occlusion from a subtotal carotid artery occlusion is one of the most important differential diagnoses made during a carotid evaluation. The finding of carotid occlusion carries significant clinical implications since this diagnosis precludes therapeutic options, including endarterectomy and stent placement. The diagnosis requires careful evaluation of the occluded segment as well as the inflow and outflow vessels. Review of the technical parameters must be performed to avoid pitfalls and misdiagnosis. Absence of blood flow in the carotid artery may be related to low-flow state, poor Doppler sensitivity, limited visualization of the carotid artery, near-total occlusion, or carotid occlusion.1–4 In this section, we review the findings and pitfalls associated with confirming the presence of a carotid artery occlusion.
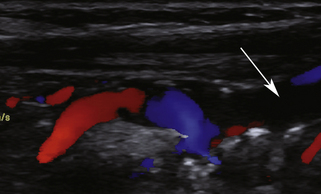
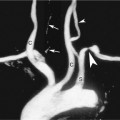
Atherosclerosis is by far the most common cause of carotid artery occlusion, but fibromuscular dysplasia and arterial dissection (discussed later) are additional causes. Patients may be acutely symptomatic or asymptomatic during presentation. Most occlusions in the carotid system occur in the internal carotid artery (ICA), but occlusion also may occur in the common carotid artery (CCA) or external carotid artery (ECA). The incidence of CCA occlusion occurs approximately one-tenth as often as ICA occlusion5 but is sufficiently common to be seen in a typical community-based vascular practice. CCA occlusion is frequently accompanied by stroke or other neurologic events but may also be encountered in the absence of neurologic symptoms.5 The ICA may remain patent in spite of CCA occlusion (Figure 10-1), because collateral supply to the ICA develops through the ipsilateral or contralateral ECA branches. Flow reverses in the collateral ECA branches and remains cephalad in the ICA.
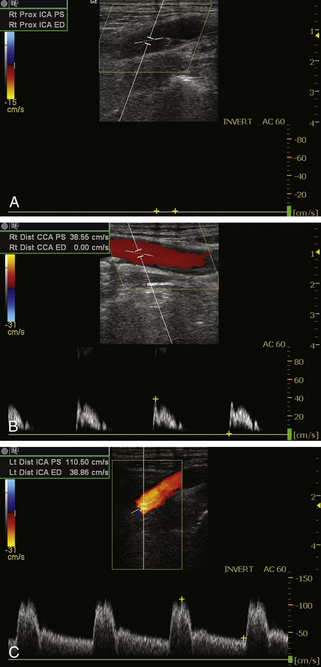
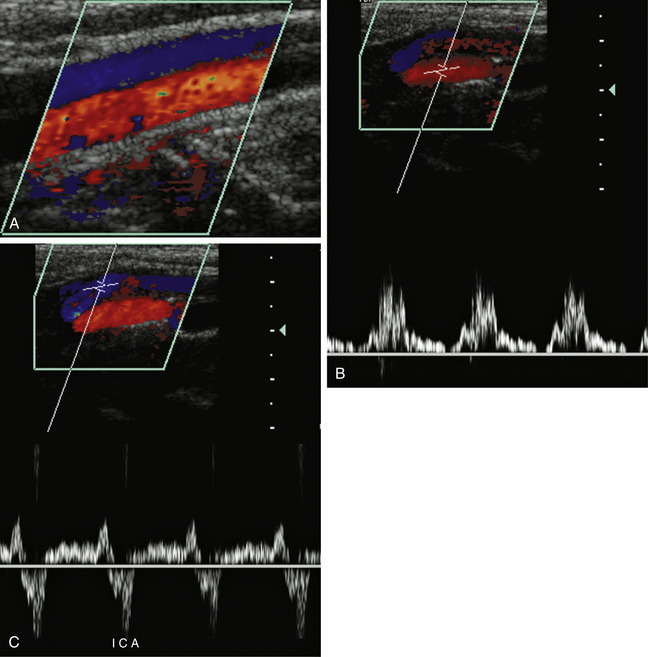
There are important secondary signs of ICA occlusion. Besides the absence of flow on Doppler examination, a pulsatile or rocking flow pattern is seen in the distal CCA proximal to the site of occlusion. This is related to antegrade blood flow striking the obstructing segment in systole and reversing in diastole. The Doppler waveforms obtained in the CCA show a low-velocity, high-resistance waveform with decreased, absent, or reversed flow in diastole (Figure 10-2). Increasing resistance is usually noted in the distal CCA, closer to the occlusion, because of outlet obstruction. There may be increased, low-resistance flow in the ECA as collaterals attempt to increase blood flow on the ipsilateral side. This is called “internalization of the ECA” and reflects collateral flow to the brain. Increased flow velocities may be seen in the contralateral ICA with ipsilateral ICA stenosis or occlusion. This is referred to as “compensatory flow of the contralateral ICA” and is another mechanism to increase blood flow to the brain.
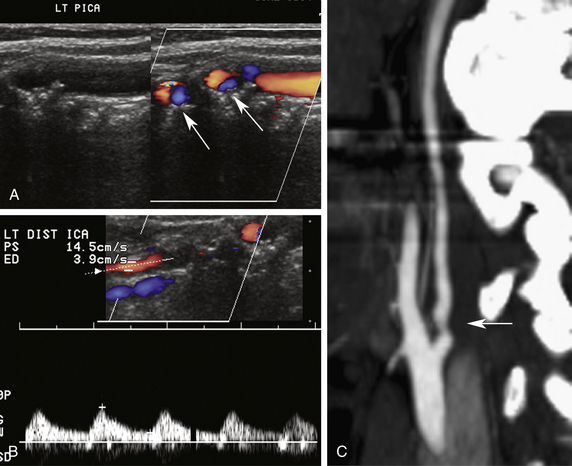
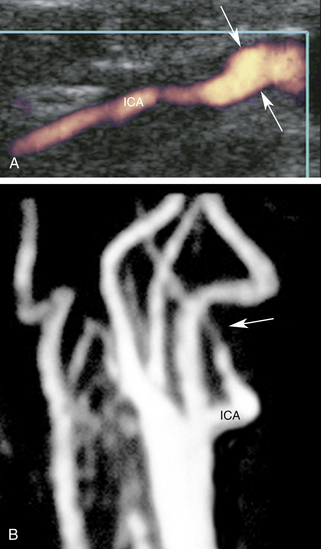
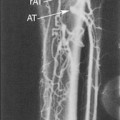
False-positive diagnoses may occur when the artery is obscured by acoustic shadowing, when image quality is poor, when Doppler signals are weak, and especially when the vessel is nearly occluded and only a “trickle” of flow is present in near-total occlusion of the artery. A near occlusion of the ICA often produces the angiographic “string sign” (Figure 10-3). It is important to realize that the apparent small caliber of the arterial lumen represented by the “string” of contrast is an artifact. The string sign results from puddling of the slow-moving contrast agent in the dependent (posterior) portion of the arterial lumen with the patient supine. The distal lumen may in fact be widely patent, and the stenosis localized at the ICA origin.
Distinguishing carotid occlusion from high-grade carotid stenosis can be a challenging task for the sonographer or sonologist. Low flow in a near-total occlusion may be difficult to detect with preset Doppler parameters and requires optimization of color, power, and pulsed Doppler settings. The use of power Doppler imaging is recommended because of its sensitivity to low flow rates, and studies using color or power Doppler6,7 report close to 100% sensitivity and specificity in the diagnosis of near occlusion of the ICA. To attain this level of accuracy, however, several technical details must be followed. First, adjust the instrument to detect minimum flow velocity. The PRF should be as low as possible, and the low-frequency filter should be minimized so that low-frequency signals are not excluded. Second, obtain the best possible view of the occluded vessel and scrutinize the lumen for any hint of blood flow. Remember that the view chosen should optimize the Doppler angle of the color flow image. Toggling between color and power Doppler is helpful especially when motion artifacts are a problem. Third, interrogate the visualized segments of the carotid artery with spectral Doppler. The signals obtained may be very weak, so high Doppler gain settings are needed.
Carotid Artery Dissection
Arterial dissection refers to the entry of blood into the wall of the artery, separating the layers of the wall and creating a false lumen through which blood flows.8–14 For blood to enter the wall and cause dissection, there must be a rent in the intima, which may be caused by violent trauma, iatrogenic trauma, or an underlying weakness of the muscular layer that allows the intima to tear. The location at which the wall layers separate varies. In some cases, only the intima is dissected from the wall, while in other cases, portions of the media or the media and adventitia may delaminate. Thus, the thickness of the membrane separating the true and false lumens varies. Dissection through the adventitial layer may allow pseudoaneurysm formation adjacent to the artery.
Carotid artery dissection usually originates in the aortic arch and extends only to the carotid bifurcation, but dissection can extend into the ICA. Three to seven percent of aortic arch dissections are complicated by stroke or transient cerebral ischemia.12–14 Common carotid extension most commonly occurs with ascending arch dissection (Stanford’s type A), which usually is related to atherosclerotic disease but also may be caused by elastic tissue degeneration, as seen with Marfan’s or Ehlers-Danlos syndrome. Stanford’s type B dissection, occurring distal to the aortic arch, usually does not affect the carotid arteries. Considering that neurologic symptoms are uncommon when carotid dissection extends from the aortic arch, carotid dissection is occasionally an incidental finding at carotid sonography.
Carotid dissection may also originate within the ICA, usually beginning at the skull base.8,10 This dissection may occur either spontaneously or following trauma. Some “spontaneous” dissections may not really be spontaneous and may actually result from nonviolent trauma, such as unusually strenuous exercise or rapid neck motion. In some cases, the precipitating trauma may be unrecognized by the patient. Arterial pathology may also lead to atraumatic ICA dissection, including fibromuscular dysplasia (FMD), Marfan’s syndrome, cystic medial necrosis, and Ehlers-Danlos syndrome. Unlike CCA dissection, the false lumen of ICA dissection is almost always occluded by thrombus.
Seventy percent of spontaneous ICA dissections or those following minimal trauma occur in patients 35 to 50 years of age, with an equal incidence in men and women. Systemic hypertension is present in one of three cases and is considered a predisposing factor. Presentation includes headache, neck and facial pain, hemispheric ischemic symptoms, and cranial nerve palsy. Seventy percent of ICA dissections resolve with mild or no neurologic deficit, but 25% of patients suffer disabling neurologic consequences and 5% of cases are fatal.8,10 Spontaneous restoration of ICA flow occurs in many cases of high-grade stenosis or occlusion through retraction of the thrombus in the false lumen, relieving compression of the true lumen. Therapies employed for carotid dissection are usually antithrombotic and antihypertensive medications.
Carotid dissection resulting from violent trauma most commonly originates with direct injury to the ICA, either from stretching of the artery across cervical spine structures or from direct arterial compression by cervical spine elements or the mandible.11,13 Trauma causes a rent in the intima and an injury that weakens the underlying wall structure, permitting delamination. Serious neurologic consequences are more common with traumatic carotid dissection than with atraumatic dissection.10
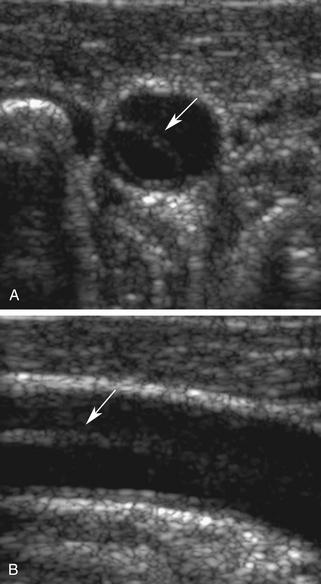
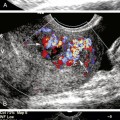
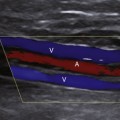
The ultrasound findings associated with common carotid dissection9,10,12 may be dramatic when the intima is separated from the rest of the wall and flutters in the flow stream with each cardiac cycle (Figure 10-4). Severe flow disturbances are caused by the flapping intima (Figure 10-5). However, if the tissue between the true and false lumens is thick, the intervening membrane is stiffer and dissection is indicated simply by duplication of the carotid lumen on color Doppler.
The classic sonographic presentation of ICA dissection is a smooth, tapering stenosis (Figure 10-6) occurring in a patient who is younger than the typical patient with atherosclerotic stenosis (i.e., <50 years of age). Regardless of age, however, consider dissection in any patient with a smooth, tapering ICA stenosis without visible atherosclerotic plaque. In other cases of ICA dissection, the sonographic findings may be subtle and easily overlooked. The ICA lumen may be normal in the area just above the bifurcation if dissection beginning at the skull base does not extend down to the point of sonographic visualization. In such instances, the only detectable abnormality is increased flow resistance seen in the Doppler waveforms and possibly reduced flow velocity overall due to distal ICA obstruction. In some cases, a thin intimal flap may not be appreciated during color Doppler examination because of color-blooming artifact. That is, the color will write over the thin flap, and only the color flow disturbance is seen. The flap is better seen when the examiner turns off the color display and examines the vessel with gray-scale imaging. Another presentation is ICA occlusion with no apparent cause. Again, the absence of atherosclerotic plaque or youthful presentation should suggest the diagnosis of dissection.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree