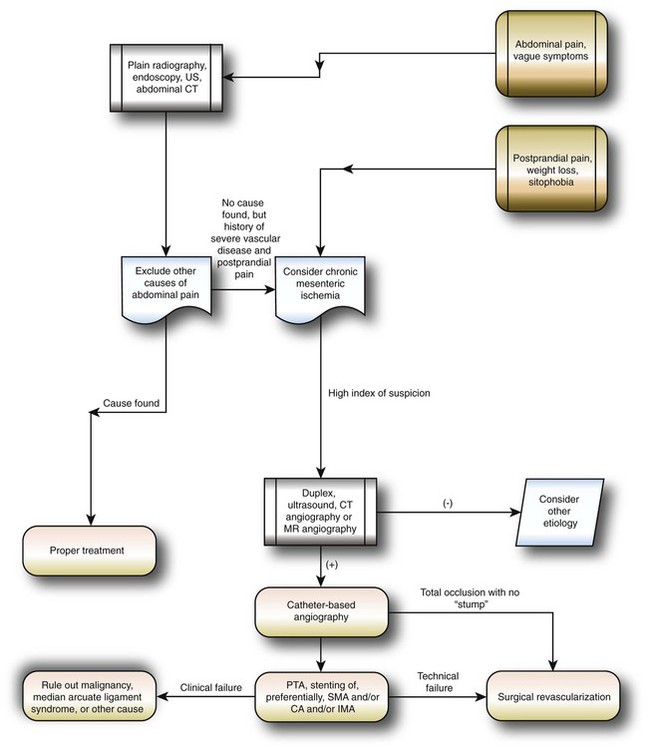
Chapter 56 Ulku C. Turba, H. Omur Sildiroglu and Alan H. Matsumoto Although chronic mesenteric ischemia (CMI) is a relatively uncommon entity owing to the robust mesenteric arterial collateral circulation, detection of intestinal angina and CMI is of critical importance. If the diagnosis is overlooked or missed, acute mesenteric ischemia can result. Once acute mesenteric ischemia develops, patient mortality rates become very high. In addition, an accurate diagnosis and pretreatment noninvasive evaluation will facilitate treatment planning and affect optimal clinical outcomes (Fig. 56-1). The natural history of mesenteric arterial disease is not well defined. In the only study published to date, a retrospective analysis revealed that 23% of asymptomatic patients who were noted to have disease of all three mesenteric arteries at the time of aortography (performed for other reasons) developed symptoms of, or sequelae related to, mesenteric ischemia during a 7-year period of follow-up.1 Therefore, given the paucity of data about the natural history of mesenteric arterial occlusive disease, the most common indication for treatment of stenoses or occlusions of the mesenteric arteries is the presence of ischemic symptoms. Based on the surgical literature, during aortic reconstruction for aneurysmal or occlusive disease, mesenteric arterial reconstruction should be routine even in asymptomatic patients because these patients have a worse postoperative course if their mesenteric vascular disease is not corrected at the time of their aortic surgery.1,2 The topic of aggressive treatment in asymptomatic patients with mesenteric arterial occlusive disease when there is no need for aortic reconstruction is where the controversy begins. We believe that even in asymptomatic patients, the presence of significant three-vessel mesenteric arterial occlusive disease warrants strong consideration for revascularization, especially if endovascular therapy is feasible. An isolated asymptomatic mesenteric arterial stenosis should be managed on a case-by-case basis because many of these patients may never become symptomatic, especially those with an isolated stenosis of the celiac or inferior mesenteric arteries. • 50 to 100 mL of iodine-based contrast. Alternatively, CO2, may be used judiciously in patients at risk for contrast-induced nephropathy. • A multi-sidehole catheter for aortography and selective catheters (RC 1, Simmons 1, Rosch Inferior Mesenteric [RIM], or SOS Omni 2 [AngioDynamics, Glen Falls, N.Y.]), depending on the anatomy, are used for selective catheterization of the mesenteric arteries. • A guiding sheath or guiding catheter of proper size and shape will facilitate delivery of a balloon catheter and/or stent (Fig. 56-2, A, B, and D) and allow for contrast injections to assess results of the intervention. In mesenteric arteries that have an acute caudal orientation off the aorta, an 8F tip-deflecting catheter (Morph catheter [Biocardia Inc., Mountain View, Calif.]) has been employed to aid the intervention for a femoral access. • Pressure transducers for translesion pressure gradient measurements, as needed, to determine the hemodynamic significance of questionable stenoses will be useful. • A variety of 0.035-inch, 0.018-inch, or 0.014-inch guidewires and compatible balloon and stent platforms are recommended. • Heparin, nitroglycerin, conscious sedation medications, oral antiplatelet agents, prophylactic antibiotics prior to stent placement, and possibly a closure device for the arteriotomy are often used or administered before, during, or after completion of the endovascular procedure. • High-resolution angiography equipment that allows for multiplanar imaging, an experienced interventionalist, a nurse dedicated to patient monitoring during the procedure, and a well-trained technologist are also essential for procedural success. Once the clinical indication is established, treatment planning becomes crucial. Computed tomographic angiography (CTA) and magnetic resonance angiography (MRA) are excellent roadmaps for treatment planning (Fig. 56-3, A). With the availability of preshaped guide sheaths and guiding catheters (see Fig. 56-2), most patients can be treated from a femoral artery approach. In the presence of an infrarenal aortic occlusion, an approach from an upper extremity may be necessary, and the profile of the system used should be minimized. There is one observational study that suggests that an upper extremity versus a femoral approach to mesenteric artery stenting may be associated with better outcomes.8 However, these findings have not been corroborated by other investigators. A reverse-curve catheter such as an SOS Omni 2, RC 1, or Simmons 1 catheter is typically used to catheterize the celiac artery or superior mesenteric artery (SMA) from the femoral artery approach, and a selective angiogram is obtained to better define the arterial anatomy and ensure an intraluminal location prior to proceeding to an intervention. For catheterization of the IMA, a RIM or SOS 2 catheter is preferred. An appropriately shaped guiding sheath or catheter is then advanced over the guidewire to the level of the origin of the mesenteric artery. The angioplasty and stenting procedure can then be performed in a similar fashion to a renal revascularization procedure, using 0.035-inch, 0.018-inch, or 0.014-inch guidewire platforms. Because of the resistant nature of many ostial mesenteric arterial stenoses, balloon-expandable stents are preferred. For truncal lesions, either balloon-expandable or self-expandable stents are used, depending on the length and configuration of the lesion (Fig. 56-4; also see Fig. 56-3). Covered stents (iCast [Atrium Medical, Hudson, N.H.]) may be used in a selected subgroup of CMI patients where aortic/ostial soft plaque might be at risk for causing cholesterol emboli, or in small mesenteric arteries at risk for developing in-stent restenosis. However, these theoretical advantages of using covered stents have not been established with data from well-designed clinical trials. We do use covered stents in the subgroup of CMI patients who present with restenosis in an existing mesenteric artery stent or in mesenteric arteries less than 6 mm in diameter, owing to high rates of in-stent restenosis in arteries less than 6 mm in diameter. Devices compatible with 0.014-inch guidewires are typically more flexible, easier to deliver, and track better in acutely oriented arteries compared with 0.035-inch platform devices. However, 0.014-inch balloons tend to be more compliant and tend to “dog bone” within a resistant lesion, and 0.014-inch stents do not have as much hoop strength and are less visible than 0.035-inch stents. Therefore, 0.014-inch balloon and stent systems are less likely to provide optimum luminal diameters in very resistant ostial mesenteric artery lesions. In cases in which advancement of the balloon and stent across the lesion into the parent SMA, IMA, or celiac artery is not possible owing to tortuous iliac arteries, acute angulation of the artery from the aorta, and the presence of a tight stenosis or chronic total occlusion, use of a deflectable braided 8F guide catheter (Morph catheter) may be helpful. Its shape can be manually changed to optimize the catheter angle and provide stability within the aorta to allow for advancement of the balloon and stent across the lesion (see Fig. 56-2, D). Extensive collateral networks between the mesenteric arterial beds make the incidence of symptomatic CMI relatively uncommon. Given the poorly defined natural history of occlusive mesenteric arterial disease and the increasing number of asymptomatic patients with mesenteric arterial stenoses detected on CTA and MRA obtained for other reasons, the discussion around mesenteric revascularization in asymptomatic patients remains controversial.1–3 Having said that, there is a consensus among vascular specialists that mesenteric revascularization should be performed on patients with asymptomatic mesenteric arterial disease who will be undergoing reconstruction of their abdominal aorta, especially if the IMA is likely to be sacrificed. However, whether revascularization of a critical stenosis of the SMA should be performed in an asymptomatic patient who is otherwise having no vascular issues remains controversial, with no proven benefit or clinical outcomes studies. Although some authors suggest that surgery for the treatment of patients with CMI is a better option than endovascular therapy, the risk of significant postoperative morbidity and mortality favors an endovascular approach as the first treatment option.4 Primary assisted clinical success rates with endovascular therapy approach 90% at 5 years, with 5-year survival rates of 76%.5,6
Chronic Mesenteric Ischemia
Indications
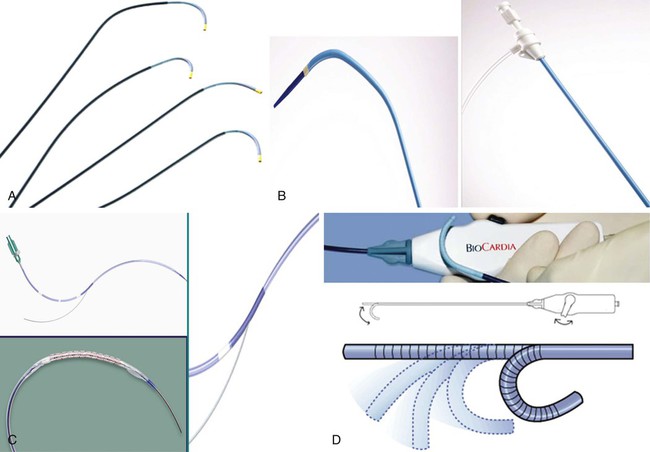
Equipment
Technique
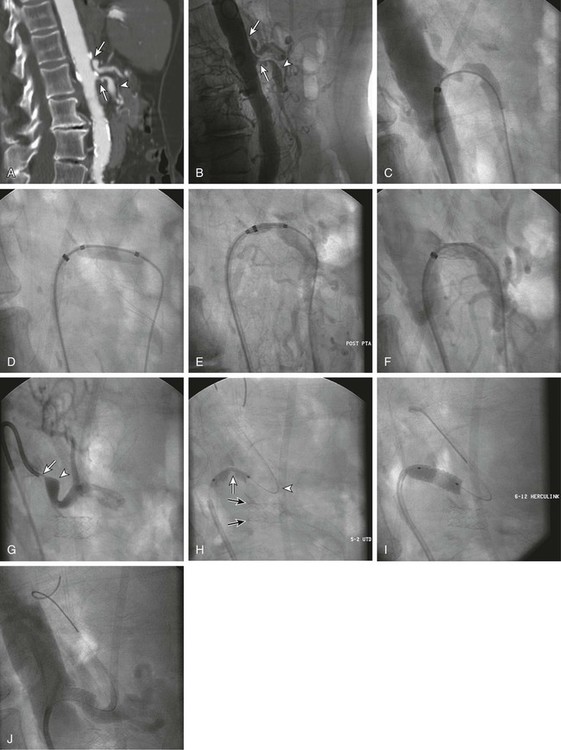
Anatomy and Approaches
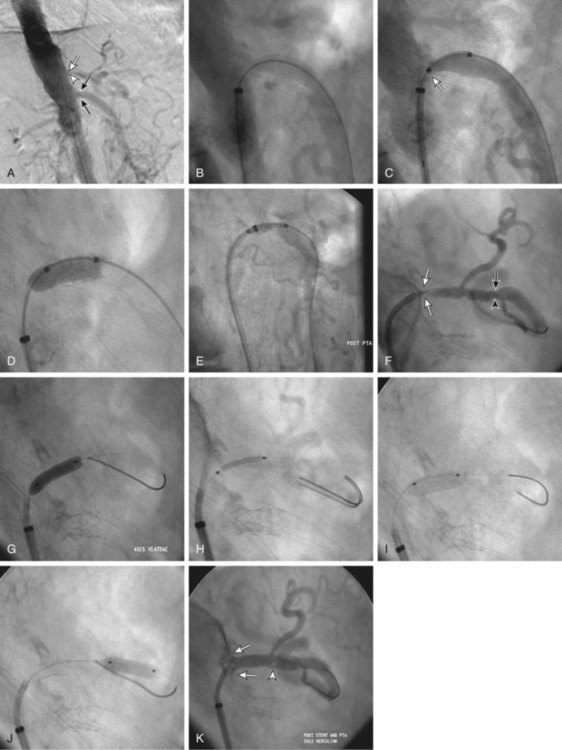
Technical Aspects
Controversies
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Radiology Key
Fastest Radiology Insight Engine