CHAPTER 20 Chronic Otitis Media
Epidemiology
Chronic otitis media (COM) is an unresolved inflammatory process of the middle ear and mastoid. Early theories proposed that eustachian tube dysfunction was the primary cause of COM. Such dysfunction was thought to lead to collapse of the eustachian tube and result in negative intratympanic pressure. This resulted in fluid transudation and accumulation of fluid in the middle ear cavity. More recent data suggests that there is also likely an infectious etiology, as COM generally begins as an acute middle ear infection that can persist and evolve over time.
Clinical Features
Clinically, patients complain of otorrhea and hearing loss. Hearing loss is usually conductive, although a sensorineural component may be present in advanced cases. Patients with COM may have middle ear mucosal proliferation, which predisposes the formation of acquired cholesteatoma. Effusions may be serous, mucoid, or purulent. Patients may also complain of otalgia during acute exacerbations. On otoscopic examination, the eardrum may be retracted or perforated. There may also be tympanosclerosis. Associated abnormalities include cholesteatoma (with or without ossicular erosion), granulomas, or polyps.
Pathology
While the effusions associated with COM may be of variable consistency, bacteria are usually present. Pseudomonas aeruginosa is the most common bacteria, being present in 40 to 65% of cases, with Staphylococcus aureus present in 10 to 20%. Anaerobic bacteria are also frequent pathogens in COM, being found in 8 to 59% of patients. Over half the cases of COM may be polymicrobial.
These pathogens, along with the chronic effusion, induce changes in the middle ear mucosa, including a chronic inflammation and granulation tissue. Middle ear mucosal hyperplasia and formation of gland-like structures in the submucosa can occur, with the latter being responsible for the persistent effusions. These changes can be extensive and irreversible. Adhesions and scars can form in quiescent periods. Ossicular erosions may result from direct infection, vascular thrombosis, and subsequent necrosis, or cholesteatoma. Bone changes are prominent in the mastoid with initial destruction, followed by osteoneogenesis, resulting in dense, sclerotic bone formation. Patients with long-standing COM may also develop hyperostosis of the ossicles, especially the stapes.
Treatment
Medical management usually consists of routine cleaning and topical solutions containing one or more antibiotic and possibly corticosteroids. Systemic antibiotics may also be given for COM. Surgery is usually recommended only if medical therapy fails. Surgery may consist of tympanostomy tube placement if there is insufficient middle ear ventilation, or adenoidectomy if reflux of nasopharyngeal organisms, resulting in middle ear infection, is the problem. Both conditions often coexist, necessitating a combined procedure.
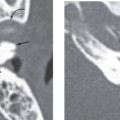
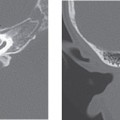
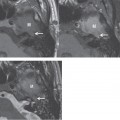
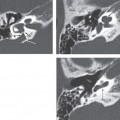
Imaging Findings
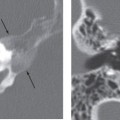
CT
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree