Epidemiology
Synthetic ossicular protheses are commonly indicated in patients with ossicular disruption or destruction caused by chronic otitis media and cholesteatoma. They may also be used in patients with congenital ossicular malformations, posttraumatic injuries, and otosclerosis. The prosthesis is used to restore the integrity of the ossicular chain and allow sound waves to be transmitted to the inner ear.
Clinical Features
The type of synthetic ossicular prosthesis used is generally determined by the extent of ossicular damage or disease, the properties of the device, and the surgeon’s preference. In disease limited to the oval window, a stapedectomy or stapedotomy is usually performed and the stapes superstructure (head, neck, and anterior and posterior crura) replaced by a prosthesis. For incudostapedial joint disease, a synthetic prosthesis or autologous bone may be used. A partial ossicular replacement prosthesis (PORP) or total ossicular replacement prosthesis (TORP) is employed when more extensive ossicular reconstruction is necessary. Although the terms PORP and TORP are registered trademarks, they are commonly used to refer to two basic prosthetic configurations used to reconstruct the ossicular chain. The term PORP is commonly used when the stapes is intact and mobile, whereas the term TORP is used when the superstructure of the stapes is absent, but the footplate is present and mobile.
Malfunction of ossicular prostheses can occur and should be clinically suspected when there is an increase in conductive hearing loss. Malfunction can be the result of recurrent middle ear disease (otitis media or cholesteatoma), granulation tissue or adhesions, or displacement (subluxation, dislocation, or extrusion) of the prosthesis.
Treatment
Otosclerosis and congenital abnormalities are the most common indications for stapes reconstruction with prosthesis placement. Other indications include posttraumatic injuries, adhesions, and tympanosclerosis. In a stapedectomy, the stapes superstructure and part or all of the footplate are resected to open the oval window and allow sound to enter the labyrinth. A wire or piston prosthesis is used to reconstruct a conductive bridge between the incus and labyrinth. A stapedotomy is a newer procedure in which the stapes superstructure is resected, but the footplate preserved. A small hole is drilled in the footplate, and a wire piston is advanced through this small opening. Studies comparing the two procedures have revealed slightly better early and late postoperative air-conduction thresholds and a lower rate of postoperative sensorineural hearing loss in patients undergoing a stapedotomy. Vertigo and reparative granuloma formation are also less frequent with stapedotomy. Complications related to the stapes prosthesis include displacement, migration, or extrusion; resorption of the long process of the incus by direct pressure or foreign-body reaction; fracture or bending of prosthesis; vestibular perforation, often in the setting of increased negative middle ear pressure caused by eustachian tube dysfunction; perilymphatic fistula; post-stapedectomy granuloma; and fibrosis.
The incus is the most vulnerable ossicle with regard to traumatic and infectious injury. Damage to the incus can occur with an intact malleus handle and stapes. Three main types of incus prostheses—homograft, autograft, or allograft—may be used in this setting. Usually, an incus interposition procedure is performed, in which the native incus is removed, sculpted to a suitable size and shape, and interposed between the malleus and stapes. Potential complications of incus interposition include displacement, absorption, and harboring microorganisms. Alternatively, a homologous ossicle or synthetic prosthesis may be used. With homologous ossicular prostheses there is the risk of transmitting disease such as HIV, hepatitis, or Creutzfeldt-Jakob disease and the need to store and reconstitute the prosthesis. Subluxation, incudal necrosis, granuloma formation, recurrent cholesteatoma, and ankylosis are potential complications of incus interposition.
Synthetic prostheses are now the most commonly used and are available in two basic tack-like configurations: a PORP and a TORP. A PORP extends from the medial surface of the tympanic membrane or occasionally the malleus to the head of the stapes, whereas a TORP extends from the tympanic membrane or malleus to the stapes footplate or oval window. Synthetic prostheses are generally a composite, with the head made of hydroxyapatite, a biocompatible material that can bond to tissue, but is difficult to sculpt and modify. The shaft of the prosthesis may be made of Plasti-Pore (Medtronic Xiomed, Minneapolis, Minnesota), a high-density polyethylene sponge product, a fluoroplastic or a polymer of hydroxyapatite and polyethylene, all of which can be easily cut to the appropriate length. The specific shape of the prostheses varies among manufacturers. More recently titanium ossicular prostheses were introduced, their use first being reported in 1999. They also come in a TORP and PORP configuration.
Postoperative complications following placement of TORP or PORP include subluxation and extrusion. Encasement of the prosthesis by granulation tissue or recurrent cholesteatoma may result in subluxation. Extrusion of the prosthesis occurs most commonly with allografts that directly abut the tympanic membrane. The incidence of extrusion is less if a cartilage graft is placed between the tympanic membrane and the prosthesis or if the prosthesis abuts the undersurface of the manubrium, rather than the tympanic membrane directly.
Imaging Findings
CT
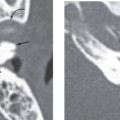
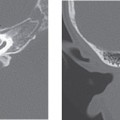
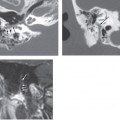
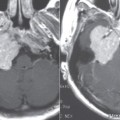
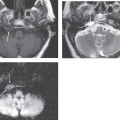
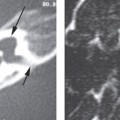
Once ossicular prostheses are implanted, computed tomography (CT) is the main imaging modality used to assess the position of the prosthesis and evaluate any complications. Regardless of composition, ossicular prostheses appear as radiodensities on CT. The various proprietary protheses have a characteristic configuration that can be identified on CT. Postoperative imaging is usually obtained in patients who present with new conductive hearing loss, in which case CT is useful in identifying the cause.
Stapes Prosthesis
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree