CHAPTER 51 Cochlear Implantation
Epidemiology
Cochlear implants (CIs) have become the accepted treatment in patients with severe to profound bilateral sensorineural hearing loss (SNHL) who receive little benefit from conventional hearing aids.
Clinical Features
For patients under consideration for a CI, a complete hearing history must be obtained, a neurotologic and head and neck examination must be performed, and a series of hearing tests must be administered. Certain levels of hearing loss are necessary to qualify for a CI; however, these levels are continually changing as both hearing aid and cochlear implant technology advances. The age at which the hearing loss occurred and whether it occurred before (prelingual) or after (postlingual) the acquisition of spoken language are important factors in assessing the potential success of a CI. Children and adults with postlingual deafness derive benefit from cochlear implantation. In children, there is rapid improvement in the first 6 months after implantation with continued improvement beyond 2 years, whereas in adults improvement usually plateaus during the second year after implantation. Study of children with prelingual deafness indicates that most experience benefit from their implant with regard to speech perception. The younger the age of the child at the time of implantation, the more benefit they obtain, as there is greater plasticity in the auditory system. However, progress can be slow and may not be appreciable for a year or more. Cochlear implantation is typically not performed in adults who are congenitally deaf or lost hearing at an early age. Although the procedure is occasionally performed, the outcome in this group of patients is poor due to prolonged auditory deprivation and presumably auditory neuronal atrophy.
Pathology
In the normal-hearing individual, transduction of sound waves into electrical activity that can be transmitted to the auditory nerve and then onto the brainstem and higher auditory centers occurs via depolarization of hair cells in the organ of Corti. Aging, chronic noise exposure and many disease processes (meningitis, labyrinthitis, viral inner ear infections, autoimmunity, ototoxic drugs, cochlear otosclerosis, and skull base fractures) can lead to the loss of these hair cells. Additionally, the organ of Corti may be absent in many cases of congenital deafness. The cochlear implant assumes the role of transduction, delivering a signal to the auditory nerve that can be transmitted to the auditory cortex.
Treatment
Most surgeons prefer to place the CI in the better hearing ear. A skin flap is made posterior to the ear and a canal wall down mastoidectomy performed. The internal receiver-stimulater component of the CI is placed in a recess created in the skull posterior and superior to the mastoidectomy. The facial recess is opened and a cochleostomy is made anterior to the round window into the basal turn of the cochlea to allow for placement of the electrode in the cochlea. More extensive surgery is required if the cochlea is obstructed or obliterated. A transmitter, held in place by a magnet, a microphone, and a speech processor are worn externally. Generally the skin flap is allowed to heal for 4 to 6 weeks before the external devices are fitted and activated.
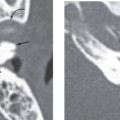
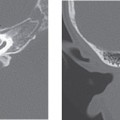
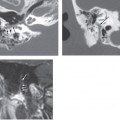
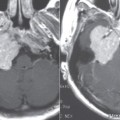
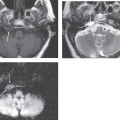
Imaging Findings
CT
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree