Abstract
A cloaca is a common chamber into which some or all of the digestive, urinary, and reproductive tracts discharge their contents. A cloaca exists in all human embryos up to 4–6 weeks, at which time it becomes partitioned into the urogenital sinus and the rectum. A cloaca forms when the cloacal membrane does not recede or the mesoderm does not invade. While the exact etiology of cloaca is unknown, some evidence suggests disruptions in hormonal or genetic signaling.
The majority of fetuses with cloacal anomalies have abnormalities noted on ultrasound (US). While definitive diagnosis is difficult prenatally, prenatal recognition of cloacal abnormalities may impact prenatal and neonatal care and has the potential to improve outcomes. Patients are often referred secondary to a pelvic mass noted on prenatal imaging.
Cloacae are rarely diagnosed in the first trimester, but by the second trimester many of the associated anatomic defects are visible. Urologic anomalies are frequent, with up to 90% of patients with cloacal anomalies having concurrent urologic abnormalities. It is important to note that cloacae can be mistaken for ambiguous genitalia, hydrocolpos, pelvic masses, and bladder obstruction, and whereas US is the standard imaging modality, magnetic resonance imaging (MRI) can be helpful in distinguishing milder forms of cloaca from other anomalies.
Outcomes are directly related to the severity of the malformation. Even in patients with milder cloacal anomalies, significant bowel and bladder deficits are common. The two factors that most predict functional outcome are anal position and cloacal length.
Keywords
cloacal exstrophy, OEIS, omphalocele, bladder exstrophy, ambiguous genitalia, hydrocolpos
Introduction
Cloaca is derived from the Latin word for sewer or drain. Anatomically, it is used to describe a confluence of the urinary, genital, and gastrointestinal (GI) tracts. While this is the norm in birds, reptiles, and amphibians, most mammals have separate outlets for each system. In humans, there is a wide range of cloacal abnormalities. Mild forms may involve only a persistent urogenital sinus opening in combination with an anteriorly displaced anus. More severe varieties involve all three tracts converging in the pelvis. The most extreme type of cloacal anomaly is termed cloacal exstrophy, and includes a large midline abdominal defect.
Cloacal abnormalities were first described in humans over 300 years ago. Historically, these anomalies were fatal because of GI and/or urinary obstruction. With advancements in neonatal management and surgical intervention, children born with these anomalies are now able to survive, and often thrive.
Disease
Definition
A cloaca is a common chamber into which some or all of the digestive, urinary, and reproductive tracts discharge their contents. Cloacal abnormalities present in a spectrum of mild to severe forms and all share a common etiology (see later section). In humans, the most extreme cloacal abnormality, cloacal exstrophy, is often referred to as the OEIS complex. The OEIS complex includes the midline abdominal defect of omphalocele (O), exstrophy of the bladder (E), imperforate anus (I), and spine (S) abnormalities.
Prevalence and Epidemiology
The prevalence of cloacal exstrophy was initially estimated as 1 : 200,000–1 : 250,000 births and all cloacae as 1 : 50,000 births. More recent studies have found a significantly higher prevalence, ranging from 1 : 9715 births to 1 : 27,174 births. The increased incidence may be caused by more accurate diagnosis and record keeping.
Males seem equally affected compared to females ( Table 19.1 ). Cloacal malformations are nonhereditary, as no familial cases have been described. Large cohort studies have not elicited any epidemiologic trends. In particular, no maternal factors, including maternal age, appear to increase the risk for cloaca. Of note, more cases are seen in twin pregnancies than might be expected.
| Study | Total With Cloacae ( n ) | Male (%) | Twins (%) | Percent Genetically Normal |
|---|---|---|---|---|
| Evans et al. | 10 | 50 | NA | NA |
| Mathews et al. | 38 | 53 | NA | NA |
| Lund and Hendren | 20 | 65 | NA | NA |
| Ricketts et al. | 12 | 50 | 17 | NA |
| Hendren | 41 | 59 | NA | NA |
| Keppler-Noreuil et al. | 15 | 42 | 20 | 100 |
| Meizner et al. | 6 | 66 | 33 | 100 |
| Total, % (95% CI) | 139 | 55 (47–63) | 21 (11–38) | 100 |
Etiology and Pathophysiology
A cloaca exists in all human embryos up to 4–6 weeks, at which time it becomes partitioned into the urogenital sinus and the rectum. Failure of this partitioning is one reason the term “persistent cloaca” is sometimes used for fetuses and newborns. The cloacal membrane is a transitory bilaminar structure composed of endoderm and ectoderm. As the embryo develops, mesodermal in-growth leads to the cloacal membrane receding and the formation of the urorectal septum. The posterior area of the cloaca becomes the anus and the anterior portion becomes the urogenital sinus. When the cloacal membrane does not recede and/or the mesoderm does not invade, or if the cloacal membrane is too large, cloacae form. The exact cause of the interruption in normal development is unknown, but it does not appear to be teratogenic or familial; some evidence suggests disruptions in hormonal signaling as well as with homeobox and sonic hedgehog gene signaling.
As noted in Table 19.1 , a cloaca frequently occurs in one embryo of twin gestations. It has been theorized that a cytoplasmic deficiency associated with asymmetric splitting may place these fetuses at increased risk for midline defects. It has also been suggested that a single embryonic disc may increase the risk of mesodermal insufficiency.
Manifestations of Disease
Clinical Presentation
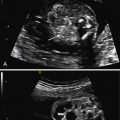
The majority of fetuses with cloacal anomalies have abnormalities noted on ultrasound (US). However, definitive diagnosis can be difficult. In fact, retrospective analyses suggest that among patients with a diagnosis of cloaca at birth, as few as 6% are suspected prenatally. Mild forms of cloaca may be the most difficult to diagnose prenatally. Patients may be referred secondary to a pelvic mass formed by the confluence of the genital, urinary, and GI tracts. This mass can be septated or can mimic a hydrocolpos ( Fig. 19.1 ). Because the urogenital and GI tracts drain into a common chamber, urine and meconium collect in the tract and this can result in an apparent hydrocolpos. The common channel is usually patent but with varying degrees of obstruction at the perineum. In a published series of six proven cases of cloacal malformation, on prenatal imaging, a central cystic pelvic mass with a fluid-debris level was seen in all six cases, and in all but one case this mass was septated. Because of the variability of perineal outlet obstruction, in total, only 30% to 50% of fetuses will have the apparent hydrocolpos on ultrasound.

Cloacal anomalies may also be suspected in cases of ambiguous genitalia. Some patients do not present until the late second or early third trimester when ascites is identified. In these patients, the cloacal anomaly is thought to be obstructive, resulting in the urine escaping through the fallopian tubes and creating ascites. Urologic anomalies are frequent, with up to 90% of patients with cloacal anomalies having concurrent urologic abnormalities; hydronephrosis is most common.
Cloacal exstrophy or OEIS typically presents as a constellation of anomalies on ultrasound. The most common clinical findings are listed by frequency in Table 19.2 . Omphalocele is present in 100% of cloacal exstrophies. Imperforate anus is also present in almost all cases, although this diagnosis is usually not made until after birth. Spinal anomalies are present in 64% to 100% of cases. However, there is significant variability in the literature regarding long-term neurologic outcomes. Much of this variability may be caused by the morbidity historically associated with the treatment of these children, among whom preterm birth and sepsis were common. Lower extremity abnormalities are also frequent, including clubbing. In one review of 38 patients, 9 were wheelchair-bound and 19 required orthopedic devices. Upper urinary tract and renal anomalies are common and diverse, as are genital anomalies. Genetically male neonates have sometimes been raised as females because of the severity of their genital abnormalities, though this strategy is controversial.