Diseases of the Airways
BRONCHOPULMONARY SEQUESTRATION
Atelectasis
Background
General.
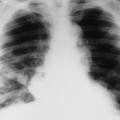
Atelectasis is defined as incomplete air filling and underexpansion of pulmonary tissue. It should be distinguished from consolidation, which also represents incomplete air filling of the lung. However, in consolidation, the missing air is replaced by blood, edema, pus, or other space-occupying substance, but missing air of atelectasis is not replaced, resulting in segmental collapse. Atelectasis may involve the entire lung or appear localized to a lobe, segment, or subsegment of the lung. It is not a disease itself but rather a radiographic sign suggesting the presence of another pathology. Based on the underlying mechanism, atelectasis is divided into five categories: obstructive, passive, compressive, adhesive, and cicatrization.
Obstructive Atelectasis.
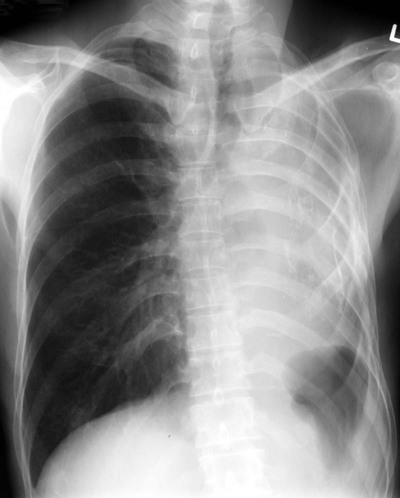
The most common form of atelectasis is obstructive or resorptive atelectasis. It is caused by intrinsic or extrinsic obstruction of an airway by conditions as neoplasm, infection, foreign body, or heavy secretions.2,6 Over time, air distal to the airway obstruction is resorbed and not replaced, leading to an airless, radiolucent, collapsed portion of lung tissue (Figs. 22-1 to 22-5). Often, the lung distal to bronchial obstruction exhibits increased radiopacity correlating to replacement of the alveolar air with inflammatory transudate, exudate, or other substance. Less commonly, a check valve or obstruction develops, creating a hyperlucent, overinflated portion of lung tissue.
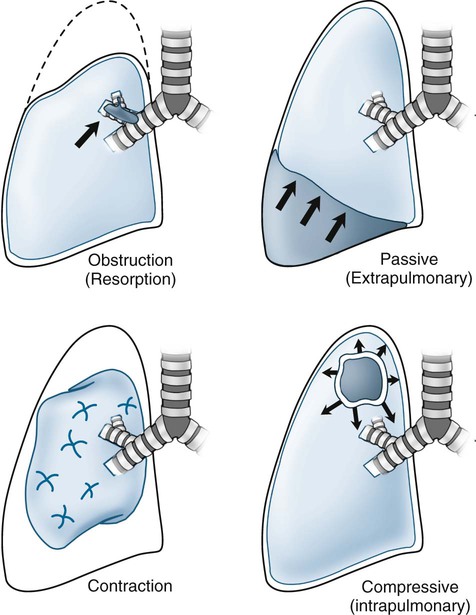
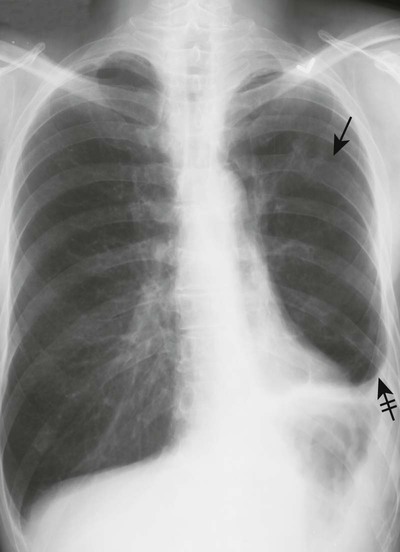
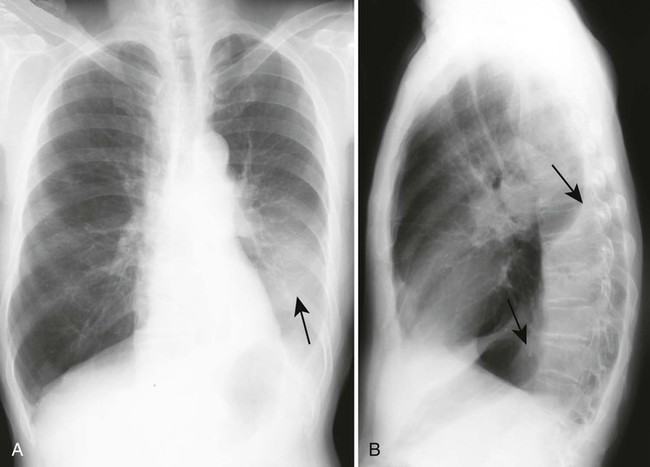
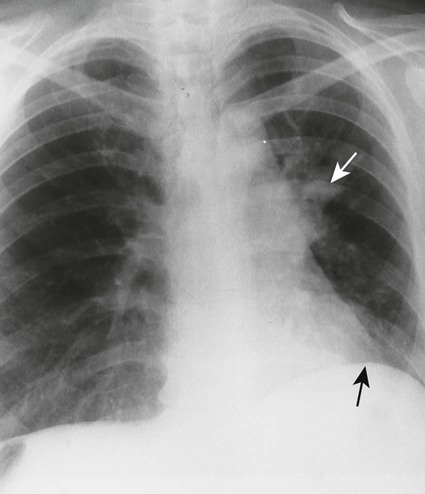
A check-valve mechanism involves accumulation of air distal to an airway obstruction. Airways dilate during inhalation, permitting air to pass by a partial bronchial obstruction. Airways constrict tightly around an obstruction during exhalation, effectively limiting the expiration of air distal to the obstruction. With each breathing cycle, more air is “pumped” into the overinflated lung tissue distal to the obstruction. Check-valve obstructions in a small airway are of limited clinical significance; however, they may result in respiratory distress when occurring in a large airway.
Passive Atelectasis.
Passive (relaxation) atelectasis is the second form of atelectasis. It results from the presence of a space-occupying lesion external to the lung. Pleural fluid (blood, exudate, transudate, and chyle) or air may accumulate to such an extent that the adjacent lung is “pushed” aside, resulting in partial or complete pulmonary collapse. Diaphragmatic elevation or herniation of abdominal viscera also may compress the lung. The amount of collapse is proportional to the size of the space-taking lesion.
Adhesive Atelectasis.
Adhesive atelectasis is nonobstructive, noncompressive pulmonary collapse secondary to decreased surfactant production by the type II pneumonocytes.31 Pneumonocyte damage results from genetic defects, general anesthesia, ischemia, or radiation damage. Adhesive atelectasis is seen in neonates with hyaline membrane disease.
Cicatrization Atelectasis.
Finally, cicatrization atelectasis represents scarring and contracture of pulmonary tissue after infection, pneumoconioses, scleroderma, radiation, idiopathic pulmonary fibrosis, and so on. This may appear localized (tuberculosis in the lung apices) or generalized (interstitial pulmonary fibrosis).
Imaging Findings
The presence of atelectasis is suggested by direct and indirect radiographic signs (Box 22-1). Displacements of intralobar fissures are the most reliable findings. The radiographic appearance differs based on the degree of lung involvement, location, and type of atelectasis (Table 22-1). Combined lobar collapse may complicate the radiographic appearance.16 Rounded atelectasis is a form of peripheral pulmonary collapse that must be differentiated from neoplastic masses with similar radiographic appearance.20,32
TABLE 22-1
RADIOGRAPHIC APPEARANCE OF ATELECTASIS
| Atelectasis | Imaging Findings |
| Lung | Opacification of the entire hemithorax, compensatory shift of the mediastinum with overinflation, and herniation of opposite lung toward collapsed lung side |
| Lobe* | |
| Right upper lobe | Radiodense lobe displaced superomedially, superiorly displaced diaphragm, oblique and horizontal fissures; can see the characteristic reversed “S shape of Golden sign”10 when a central mass is found in combination with the displaced horizontal fissure |
| Right middle lobe | Best demonstrated on the lateral projection, where the minor and major fissure approximate one another, bordering a thin, oblique-to-horizontal density; loss of silhouette of the left heart border on the frontal projection; on frontal projection, lordotic projection best for visualizing a wedge-shaped density with base adjacent to heart border |
| Right lower lobe | Radiodense lobe displaced posteromedially with posterior displacement of oblique fissure noted on lateral projection |
| Left upper lobe | Radiodense lobe displaced anterolaterally with overinflation of lower lobe occasionally located between collapsed upper lobe and mediastinum, “Luftsichel” sign35 |
| Left lower lobe | Radiodense lobe displaced posteromedially, often obstructed by heart shadow; posterior displacement of the oblique fissure on the lateral projection |
| Segment | Increased radiodensity and volume loss that correspond to region collapsed and appear less marked than lobe involvement |
| Subsegment | Also known as plate-like, discoid, or linear atelectasis; represents peripheral atelectasis of small areas of pulmonary tissue appearing as 2 to 10 cm horizontal linear density in the lower lung field |
| Round (folded lung) | Rare form of atelectasis associated with asbestosis-related pleural disease, in which the involved lung appears as a round mass (2–7 cm) in the lower lung |
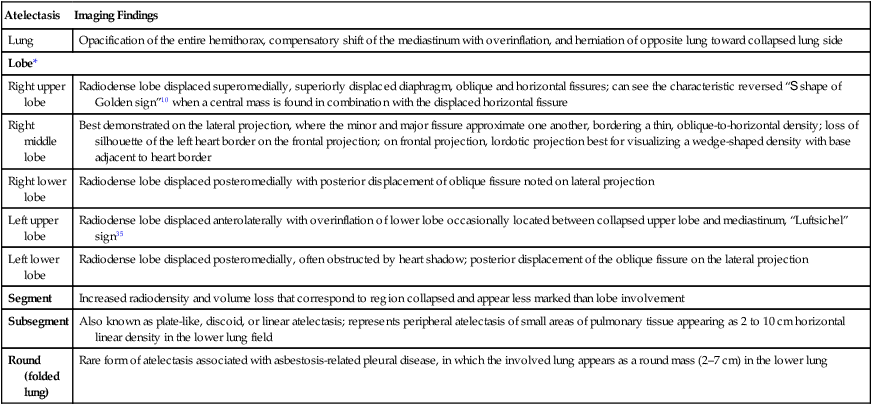
*Multiple lobes may be collapsed, yielding a combination of findings.
Clinical Comments
Whenever atelectasis is found, it should prompt a vigorous search for a cause. Although several mechanisms of collapse have been identified, obstruction of the airway resulting from neoplasm is another common cause of lobar or segmental atelectasis that should direct patient management.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree