Lymphoid Follicular Pattern and Lymphoid Hyperplasia
Lymphoid follicles are a normal feature of the gastrointestinal tract and are much more prominent in children than in adults. The lymphoid follicular pattern is best appreciated on double-contrast barium enema studies and may be seen in 50% to 70% of such examinations in children ( Fig. 118-1 ). Normal follicles are 2 mm in diameter, are uniform in size, and often have central umbilications. They can simulate familial polyposis in the way they carpet the colon. Follicles larger than 2 to 3 mm are associated with nodular lymphoid hyperplasia, which occurs in response to a number of immunologic, infectious, inflammatory, or allergic stimuli.

Anterior Anus
The anterior anus, an organic cause of constipation, is seen in some children who were previously said to have psychogenic constipation or suspected of having Hirschsprung’s disease (HD). The anterior anus may be a mild variant of imperforate anus with perineal fistula.
The amount of anal displacement may be minimal and difficult to appreciate by physical examination. The external changes may be more difficult to discern in boys than in girls. The position of the anus does not by itself determine the degree of dysfunction. Affected children may have an abnormal evacuation history from birth or may evacuate normally for several months. A long interval between bowel movements, straining with defecation, and fecal soiling are also common complaints.
Treatment is surgical. The anorectal canal and internal anal sphincter are mobilized, and a neoanus is created in a normal location. The surgery has a low complication rate and allows development of nearly normal evacuation patterns.
The differential diagnosis of anterior anus includes HD, neurologic constipation, and psychogenic constipation. These disorders can usually be excluded on the basis of physical examination, spine radiographs, rectal manometry, and rectal biopsy.
Radiologic Findings
Conventional radiographs are used to evaluate the amount of stool present and to detect spinal anomalies. If a large amount of stool obscures the sacrum, a lateral spine radiograph may be necessary to exclude sacral deformities that may be associated with neurogenic rectal dysfunction.
On barium enema examination, the lateral rectal view is key in diagnosis. In children with anterior anus, there is a deep posterior recess or shelf behind the rectal catheter ( Fig. 118-2 ). The rectum descends below the last turn of the colon as it passes anteriorly to become the anus. Postevacuation radiographs, with the rectal tube removed, show that the anus is more anterior than usual and lies at an angle to the posterior rectal shelf, which is in a normal position a few millimeters anterior to the sacrum.

Hirschsprung’s Disease
Pathologic Findings
HD is characterized by absence of ganglion cells in Auerbach’s and Meissner’s plexus in the affected bowel. The process is probably caused by arrest of the usual craniocaudal migration of primitive neuroblasts, which in some children is associated with other abnormalities of the neural crest. Research indicates that children with central hypoventilation syndrome have an increased incidence of HD.
The involved segment is of variable length and is always distal. Approximately 85% of cases are limited to the descending colon and distal segments; 55% of all cases involve the rectosigmoid colon and distal segments. Total colonic aganglionosis, with or without small bowel involvement, is seen in 8% of affected children. Extensive aganglionosis is a rare, usually lethal variant in which the entire small bowel and even the stomach lack normal ganglion cells. Zonal aganglionosis is rare and may be an acquired lesion or have a different embryologic basis.
Clinical Findings
Two thirds to three fourths of children with classic HD are male. Boys and girls are equally affected with total colonic aganglionosis. HD is the most common cause of neonatal obstruction of the colon, and more than 70% of cases are diagnosed in this period. Neonates present with delayed passage of meconium, abdominal distention, or vomiting. Delay in diagnosis can lead to bowel perforation or potentially fatal enterocolitis. About 5% of children with HD die of enterocolitis, usually within the first 3 months of life, and about 10% of children with HD develop enterocolitis before surgery. Pseudomembranous colitis may also occur in these children, even without recent exposure to antibiotics, and it can lead to perforation of the appendix and proximal colon in 5% of cases. Because pseudomembranous colitis is treatable, it may be useful to obtain stool cultures in children with HD and “typical” colitis.
Older children with undiagnosed HD usually have an abnormal neonatal stooling history and unremitting constipation. On occasion, the diagnosis is delayed until the second and third decades of life, leading to chronic constipation, chronic laxative abuse, and colonic distention, which predispose the colon to volvulus.
The clinical history and physical examination findings usually are specific. In contrast to children with psychogenic constipation, whose symptoms begin at the time of toilet training, children with HD have an abnormal stooling history as neonates and rarely have fecal soiling. On physical examination, the rectal ampulla is full in children with psychogenic constipation and empty in those with HD.
Distention of the rectum fails to produce normal reflex relaxation of the internal sphincter in children with HD. Rectal manometry may be performed if the diagnosis remains uncertain, particularly in children with a normal barium enema result who do not respond to medical therapy for constipation. Rectal manometry may give equivocal or incorrect results in approximately 18% of those younger than 1 month and in 10% older than this.
Suction biopsy of the rectal mucosa excludes the diagnosis of HD by histologic demonstration of ganglion cells. Full-thickness biopsy of the rectum is reserved for problem situations, such as when the radiologic pattern is atypical or when the mucosal biopsy is inconclusive.
In most children, HD is an isolated finding, but there is an increased incidence of this disorder among children with trisomy 21, Waardenburg’s syndrome, Smith-Lemli-Opitz syndrome, and several other syndromes. In some families, HD appears to be genetically transmitted. Genetic factors may be present in up to 20% of patients, and a dominant inheritance pattern has been identified in several families. Multiple genes have been implicated in HD, and many mutations have been observed with neurodevelopmental genes.
There is an increased incidence of malrotation in children with HD. In utero, this malrotation may lead to volvulus and ischemia and contribute to the increased incidence of intestinal atresia in children with HD. The association of HD with intestinal atresia also suggests that the ischemic event that produced the atresia might have interfered with the craniocaudal migration of neuroblasts.
Therapy
Initial treatment of HD is directed toward decompressing the colon to prevent enterocolitis. Although this can be achieved with saline solution enemas, a one-stage neonatal repair may be done. This consists of a transanal endorectal pull-through without or with laparoscopic assistance by intraoperative pathologic guidance to define the true transition zone. In children with markedly dilated colon or those weighing less than 2 kg, a colostomy is performed. Definitive or corrective surgery is usually delayed several months. All operations (i.e., Swenson, Soave, and Duhamel procedures) attempt to restore normal function by removing or bypassing the aganglionic segment. Postoperative complications include leakage at the anastomosis, continued obstruction, and, rarely, development of secondary aganglionosis in a previously normal segment.
When HD is diagnosed in an older child, a colostomy is performed before corrective surgery to enable the enlarged colon to normalize in caliber. This makes later surgery easier. Children with total colonic aganglionosis undergo ileostomy under histologic intraoperative guidance to enable placement of the ileostomy in a segment that contains ganglion cells. Later, these children undergo total colectomy and ileoanal endorectal pull-through.
Radiologic Findings
Early diagnosis of HD can be lifesaving. Unfortunately, radiologic diagnosis is more difficult in the neonatal period than in later life. Conventional radiographs show changes of distal bowel obstruction. Rarely, calcifications may be present in bowel lumen.
Contrast enema examination is performed for diagnosis and to exclude other causes of distal obstruction, such as meconium plug, small left colon syndrome, and ileal atresia. When HD is suspected, a small-caliber enema tip may be used to avoid dilating the rectum.
The enema is begun with the infant or child in the left lateral decubitus position to improve visualization of the segments most likely to be abnormal: the rectum and the rectosigmoid ( Fig. 118-3 ). In infants, a funnel- or cone-shaped appearance suggests HD ( Fig. 118-4 ). Despite reports that delayed abdomen radiographs demonstrating retained barium are valuable in confirming the diagnosis, filling of the colon proximal to an abnormal configuration is not recommended in case the barium becomes impacted. A lateral radiograph of the rectum obtained after the enema tip has been removed may be key to appreciating the abnormally small rectal vault and demonstrating the abnormal rectosigmoid index. A crinkled appearance of the distal colon, the corrugated rectum, is another finding of aganglionosis and may become more apparent after the catheter tip is removed.


In the neonate with total colonic aganglionosis, the colon may fill easily with rapid reflux into the small bowel, with a transition zone demonstrated between normal and dilated bowel in the ileum and with loss of the normal colonic redundancy. The abnormal colon may instead appear normal, have a meconium plug, or be a microcolon.
HD-induced colitis produces a spastic, difficult to distend colon with a spiculated or saw-toothed mucosa ( Fig. 118-5 ). Active colitis produces rapid expulsion of barium, which accounts for false-negative, delayed postevacuation radiographs in children with HD.

In the older child with a history of constipation, the contrast enema is performed in an unprepared colon because decompression of the dilated colon and dilation of the rectum may decrease the abrupt changes that produce the classic transition zone. Transition zone is the term applied to the region in which there is a perceptible change in caliber, with the dilated normal colon above and the narrowed aganglionic colon below. The dilated segment may contain aganglionic bowel because the innervated enlarged colon pushes its contents distally and dilates the abnormal segment. Pathologic confirmation of the true transition zone is always obtained before palliative or corrective surgery is performed.
When barium enema examination shows a dilated rectum and sigmoid colon, classic HD has been excluded; the colon above is filled to see the extent of colonic distention and to evaluate bowel rotation. Parents should be instructed in ways to enhance the passage of barium afterward. When the child undergoes a bypass procedure as the initial surgical therapy, the distal segment is usually studied with contrast enema before gastrointestinal continuity is reestablished. It may appear poorly distensible and rigid with mucosal thickening, nodularity, and polypoid lymphoid hyperplasia. Redundancy, if present, is a result of prior dilation of the ganglionic portion of this segment.
After definitive corrective surgery, there is no routine time or indication for radiologic study. If the child is septic in the immediate postoperative period, gentle instillation of water-soluble contrast material into the rectum through a small catheter can demonstrate an anastomotic leak. Alternatively, contrast-enhanced computed tomography (CT) of the pelvis may demonstrate the suspected collection or abscess and better define its extent and secondary complications.
Inflammatory Bowel Disease
The pathology, epidemiology, and radiographic findings in ulcerative and Crohn’s colitis are discussed in Chapter 57 . This short discussion focuses on a few aspects of ulcerative colitis in the child. Pediatric Crohn’s disease is presented in Chapter 116 .
Ulcerative colitis is rare during the first and uncommon in the second decade of life. The symptoms of diarrhea with blood or mucus, abdominal pain, and fever suggest a juvenile polyp, Meckel’s diverticulum, or infectious or allergic colitis. Anemia and weight loss may also develop.
The radiographic findings in children with ulcerative colitis are identical to those in adults. Toxic megacolon, however, occurs much less commonly in children.
Other Colitides and Causes of Diarrhea
Persistent bloody or watery diarrhea is unusual in children and is a cause for concern because it may lead to electrolyte abnormalities, protein and weight loss, and irritation of the buttocks. Viral, bacterial, or parasitic processes are frequently the source of the problem. In up to 28% of children, the cause of the diarrhea may elude diagnosis despite numerous diagnostic tests. Celiac disease, usually considered to be a small bowel disorder, may be the most common noninfectious cause of diarrhea. Diagnosis is based on response to a gluten-free diet and results of a small bowel biopsy.
Milk allergy and lactose intolerance can cause diarrhea in children. The inability to digest lactose can cause diarrhea in the first year of life. Removal of the offending disaccharide results in remission of symptoms. The proteins in cow’s milk and soy-based milk can damage the gastrointestinal mucosa in some children with allergy to these foods. Rectal biopsy may show diagnostic histologic changes. Barium enema examination may show nonspecific changes of colitis: narrowing, thumbprinting, and spasm. Although these changes usually involve the entire colon, segmental changes have been described. The small bowel may also be affected, producing thickening of the valvulae conniventes or narrowing of involved segments.
A rare cause of diarrhea in children is collagenous colitis. This colitis is associated with watery diarrhea and colicky pain. Microscopic analysis of biopsy specimens of mucosa is necessary for diagnosis. Widening of the collagen band of the basement membrane, few inflammatory cells, and edema of the lamina propria are observed. Symptoms usually respond to corticosteroids or sulfasalazine but may recur after the medications have been withdrawn.
Tumor is a rare cause of watery diarrhea. A few ganglioneuroblastomas and ganglioneuromas secrete vasoactive intestinal polypeptide, which, as its name suggests, produces increased intestinal motility. This disorder is often unsuspected, but the diagnosis is made when the conventional radiograph preceding barium enema reveals paravertebral mass or calcifications. Plasma levels of vasoactive intestinal polypeptide can be measured to confirm the diagnosis, and CT or sonography may be useful in delineating tumor size and tissue of origin. Removal of the tumor is followed by cessation of the diarrhea.
Kawasaki’s disease may cause a variety of physical and physiologic changes: abdominal pain, serum abnormalities indicative of liver disease, frank organ necrosis, and atypical colitis simulating ischemic colitis.
Hemolytic Uremic Syndrome
Clinical Findings
Hemolytic uremic syndrome (HUS) is a pathologic entity with two different groups of affected patients. In some, an infection with a specific Escherichia coli is associated with the development of HUS. In others, especially those with relapses of the disease, there may be a genetic component. Both groups suffer an acute microangiopathic hemolytic anemia, oliguric renal failure, and thrombocytopenia. HUS usually occurs in toddlers and children between 2 and 10 years old, who present with an influenza-like illness, gastroenteritis, and bloody diarrhea that precede the more striking renal and hematologic manifestations by several days or weeks. The gastrointestinal manifestations of the prodromal period are protean, requiring differentiation from ulcerative colitis, pseudomembranous colitis, granulomatous colitis, shigellosis, salmonellosis, intussusception, and causes of an acute surgical abdomen. Diagnosis is often delayed until anemia, thrombocytopenia, or renal failure appears. Urinalysis provides vital information because most patients have proteinuria, hemoglobinuria, or hematuria (microscopic or gross) early in the course of the disease. Those who present without diarrhea have a worse prognosis for renal disease than those who have diarrhea at presentation. The peripheral blood smear is also suggestive when schistocytes and burr cells are present. Patients may experience central nervous system symptoms, sometimes associated with abnormal findings on CT and magnetic resonance (MR) examinations.
The vigorous fluid therapy given to children with active peritoneal signs typical of HUS may result in overhydration and cause peripheral and pulmonary edema when acute renal failure develops. Prompt diagnosis may avert an unwarranted laparotomy and contribute to the proper management of fluid needs. Dialysis is necessary until renal function resumes.
Most patients recover without sequelae. Death, more frequent in children with anuria, is attributable to the manner in which the thrombotic process affects organs other than the kidneys.
Radiologic Findings
Conventional radiographs often have abnormal findings but are nondiagnostic. A disordered bowel gas pattern and thickening or thumbprinting of affected bowel loops may be observed.
The colon may demonstrate spasm, thumbprinting, ulceration, straightening, and narrowing of edematous segments ( Fig. 118-6 ) on barium enema examination. Later, strictures may form.

Sonography is useful in excluding causes of a surgical abdomen and in showing changes that suggest the diagnosis: peritoneal fluid, bowel wall thickening, and increased echogenicity of the renal parenchyma. During periods of oliguria or anuria, there are profound abnormalities of systolic and diastolic blood flow on Doppler studies. A return of normal blood flow heralds impending diuresis, useful information in children undergoing dialysis.
Appendicitis
Clinical Findings
The most common indication for emergency laparotomy in children is an inflamed or ruptured appendix. The diagnosis is based on symptoms (e.g., abdominal pain, vomiting, low-grade fever), signs (e.g., pain on palpation of the right lower quadrant, rebound tenderness), and laboratory data (e.g., low-grade leukocytosis, absence of urinary tract infection). When the presentation is classic, surgery is usually performed without radiologic studies. Imaging is performed in those whose atypical presentation suggests the possibility of other, even nonsurgical, diagnoses. Sonography has demonstrated that alternative diagnoses may be established in up to 25% of the patients with suspected appendicitis.
Infectious enteritis, Crohn’s disease, mesenteric lymphadenitis, intussusception, acute pyelonephritis, omental infarction, and Meckel’s diverticulitis are other possibilities that can be suggested with sonography or CT in the setting of suspected appendicitis. In teenage girls, gynecologic conditions, including pelvic inflammatory disease, ovarian cyst, hematometrocolpos, ovarian torsion, and pregnancy, may be diagnosed.
Rupture or perforation occurs more commonly in children than in adults. In pediatric patients who have had preoperative imaging studies, the perforation rate at surgery is as high as 50%. After rupture, the abdominal symptoms may temporarily diminish, which obscures the diagnosis.
If rupture has occurred, the inflammation of the local soft tissues (e.g., bowel, omentum) is called a phlegmon. Phlegmon or periappendiceal abscess is reported in as many as 37% of children with acute appendicitis and is more common in those whose symptoms are of longer duration. Phlegmon or periappendiceal abscess may be palpated as a right lower quadrant mass. A complete discussion of the diagnosis, treatment, and prognosis of appendiceal abscess is presented in Chapter 56 .
Radiologic Findings
The radiologic findings in children with appendicitis are identical to those in adults and are discussed in Chapter 56 . Certain features of pediatric appendicitis should be considered. Appendicoliths are more common in children than in adults with appendicitis and, when present, are more likely to be associated with appendiceal rupture ( Figs. 118-7 and 118-8 ).


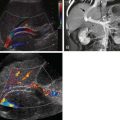
The choice of imaging modality (and even whether to image) can be confusing. In some series, the use of preoperative imaging has increased the number of alternative, nonsurgical diagnoses and decreased the number of negative appendectomies, but others have opposite results and see a negative value in waiting for the study to be done. When cross-sectional imaging is indicated, sonography ( Fig. 118-9 ) and CT ( Figs. 118-10 and 118-11 ) have a specificity and sensitivity of more than 90%. A normal appendix may be identified on sonography in up to 81% of children who do not have appendicitis ( Fig. 118-12 ).




In thin children, ultrasound is a reasonable first-line choice. In heavier children or when ultrasound is not readily available, CT has been equally successful in diagnosing or excluding appendicitis or detecting alternative disease processes. MR imaging may be useful in the diagnosis of appendicitis when ultrasonography is equivocal. Controversy about how the CT study should be done (i.e., full abdomen and pelvis or focused to the abdomen and pelvis below the lower pole of the right kidney) and what is the proper preparation (i.e., rectal, oral, intravenous, or some combination of these) indicates that many techniques produce excellent diagnostic results.
An acutely ruptured appendix may be challenging to diagnose with sonography for a number of reasons. The decompressed appendix may have a diameter of less than 6 mm, an appendix may not be identified because of overlying bowel gas, and only questionable appendiceal remnants may be present after the inflammatory response develops in the surrounding tissues. Sonography and CT are helpful in differentiating Yersinia enterocolitis (frequently associated with right lower quadrant pain) from appendicitis ( Fig. 118-13 ). In addition to imaging of appendicitis, radiologists can percutaneously drain the appendiceal abscesses.