Clinical Presentation
The patient is a 51-year-old male with 3-week history of mid back pain with radiation initially to the right side, but more recently the pain has migrated to the left side. The pain is moderate to severe in intensity. He has become weak in the legs in the past 36 hours, and over the past 12 hours he has become unable to move his lower extremities. He has no bladder or bowel dysfunction. The patient has a sensory deficit (absent pin prick sensation) at and below the T6 level. He has had intermittent fever for the past 3 weeks. Blood cultures confirmed presence of methicillin-resistant Staphylococcus aureus (MRSA) septicemia.
Imaging Presentation
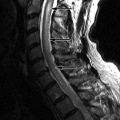
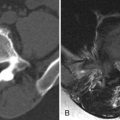
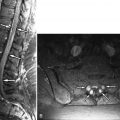
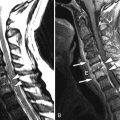
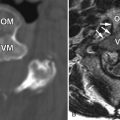
Magnetic resonance (MR) imaging revealed a fusiform right posterolateral epidural fluid collection with peripheral enhancement, extending from the T6 to T8 level ( Figs. 28-1 to 28-3 ) . The MR appearance is consistent with epidural abscess. The abscess is displacing the spinal cord anteriorly and to the left (see Fig. 28-2 ). A decompressive laminectomy was performed from T6 to T8 levels to débride and evacuate the thoracic epidural abscess. The patient was placed on intravenous antibiotics for 6 weeks, which was administered via a peripherally inserted central catheter (PICC) line.



Discussion
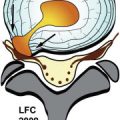
Spinal epidural abscess (epidural empyema) is an infection in the epidural space. This begins as a phlegmon that cavitates and fills with infectious liquid and necrotic debris. These abscesses most commonly arise in the anterior epidural space in the lower thoracic or lumbar region secondary to disc space infection and vertebral osteomyelitis (spondylodiscitis). Epidural abscess may also occur in the cervical or upper thoracic spinal canal secondary to spondylodiscitis or hematogenous dissemination ( Figs. 28-4 and 28-5 ) . Cervical epidural abscesses more commonly occur in the anterior epidural space, whereas thoracic epidural abscesses more commonly arise posteriorly (see Figs. 28-1 to 28-3 ).


Anterior epidural abscesses associated with spondylodiscitis are usually centered at an intervertebral disc level, but may extend over one to several vertebral levels. Posterior epidural abscesses occur by direct extension from paraspinal infections, hematogenous spread, or via the paravertebral venous plexus ( Figs. 28-6 and 28-7 ) . Posterior epidural abscesses may occur by direct extension after surgery, spinal anesthesia, or percutaneous spinal injections. Anterior or posterior epidural abscesses may arise from infections in the oral cavity, neck soft tissues, lungs, gastrointestinal (GI) tract (diverticulitis), genitourinary (GU) tract (bladder infection or pyelonephritis), from endocarditis, or secondary to septicemia. Spinal epidural infections may disseminate through the spinal canal diffusely along the leptomeninges.



Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree