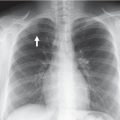
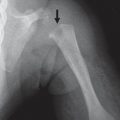
Normal variation in skeletal maturation
Fig. 5.52 |
Irregular ossification at the border between the epiphyseal ossification center and epiphyseal cartilage. |
Classically described at the medial condyle of the distal femur, medial aspect of the proximal tibia, and distal fibula. |
Osteochondrosis
Fig. 5.53
Fig. 5.54a–c, p. 530
Fig. 5.55a–e, p. 531
Fig. 5.56a–d, p. 532 |
Focal lucency and sclerosis of the secondary ossification centers and apophyses. |
Common sites are distal femoral condyle and olecranon of the elbow. Other sites are shown in Fig. 5.53 . |
Steroid therapy |
Generalized osteopenia with bone infarcts. |
MRI usually shows much more extent of involvement than radiographs alone. |
Physiologic epiphyseal defect (femoral notch)
Fig. 5.57a–d |
Characteristic focus of lucency and sclerosis at the boundary of the secondary ossification center and epiphyseal cartilage. Heterogeneously increased T2-weighted signal intensity at characteristic location at distal femur. |
Younger patients than with osteochondritis dissecans. Controversial whether it is a result of normal maturation or region of ischemia. |
Sickle cell anemia |
Bone infarct due to AVN. |
|
Maternal ingestion of certain anticoagulants |
Stippled epiphyses. |
Dicoumarol or warfarin taken in early pregnancy. |
Meyer dysplasia of the hip
Fig. 5.49, p. 528 |
Delayed or smaller multiple ossification centers of the femoral head. No collapse or metaphyseal abnormality. |
Symptomless developmental disorder of the hip. Forty to sixty percent are bilateral. Heals completely. May be mistaken for Legg-Calvé-Perthes disease. |
Chondrodysplasia punctata
Fig. 5.58a, b |
Punctate calcifications in cartilage. |
Multiple genetic forms. Type I: stippled foci of calcification in hyaline cartilage, coronal vertebral clefts, dwarfism, and joint contractures. X-linked: hypoplasia of the distal phalanges of the fingers. |
Mucopolysaccharidosis |
|
|
Dysplasia epiphysealis hemimelica (Trevor disease)
Fig. 5.46, p. 526 |
Irregular ossification at sites of epiphyseal enchondromas. Cartilage may be seen capping the stalks of the enchondromas on MRI. |
Osteochondromas of the epiphyses usually restricted to one side of the body. |
Kniest dysplasia
Fig. 5.23, p. 514
Fig. 5.47, p. 527 |
Large epiphyses at the knees, large flattened proximal femoral epiphyses with broad metaphyses. |
Spondyloepiphyseal dysplasia associated with deafness or myopia. |