Imaging Presentation
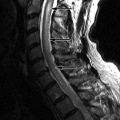
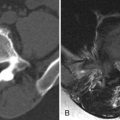
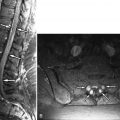
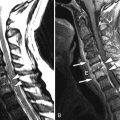
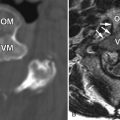
Radiographs of the spine revealed multilevel cervical spondylosis deformans, disc space narrowing. There is also narrowing of left C1-2 facet joint and multilevel facet and uncinate process hypertrophy. Bone scan reveals increased activity in the upper cervical spine on the left and mid cervical spine on the right ( Fig. 34-1 ) . Magnetic resonance (MR) imaging reveals a small effusion in the left C1-2 facet joint, thickened parafacetal soft tissues at C3-4 on the right, and enhancement of the parafacetal soft tissues posterior to the left C1-2 facets, surrounding the right C3-4 facets and in the right C3-4 neural foramen ( Figs. 34-2 to 34-6 ) .






Discussion
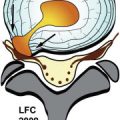
The cervical facet (zygapophyseal) joints are true diarthrodial joints, containing synovial fluid and lined by hyaline cartilage ( Fig. 34-7 ) . The cervical facets are oriented in an oblique coronal plane, which helps prevent translation of the cervical vertebrae along the anteroposterior axis ( Figs. 34-7 and 34-8 ). The degree of orientation of the cervical facet joints in the oblique coronal plane varies according to the cervical level (see Fig. 34-7 ). The C2 vertebra is unique because of the odontoid process but also because the lateral arch of C2 anatomically is like no other vertebra. The lateral atlantoaxial joint, that is, the C1-2 facet joint, is positioned more anteriorly than the cervical facets below the C1-2 level (see Fig. 34-7 ). The superior articular facet of C2 is nearly horizontally oriented and is positioned relatively far forward and superior to the inferior articular process of C2. The lateral arch of C2 is very unique because it is in reality an elongated articular pillar that embodies both the C2 pedicle and C2 pars interarticularis. The cervical neural foramen is located anterior to the cervical articular pillars and superior articular process and is bounded anteromedially by the uncinate process (see Fig. 34-8 ). The cervical neural foramen contains a ventral nerve root, the dorsal root ganglion, foraminal veins, and a small amount of fat. The vertebral artery traverses the anterior portion of the cervical neural foramen; at the vertebral body level, the vertebral artery courses through the transverse foramen. The dorsal root ganglion lies in a small concave depression along the anterior surface of the superior articular process. The cervical facet joints have a relatively thick capsule laterally (see Fig. 34-8 ). The cervical neural foramina are bounded superiorly and inferiorly by pedicles ( Fig. 34-9 ) .



The cervical facets undergo osteoarthritic degeneration in a similar manner as the lumbar facet joints and other synovial-lined joints. Abnormal acute or repeated stress upon the facet joint initiates a series of biomechanical events that cause an inflammatory process that involves the synovial lining of the joint, eventually leading to erosion of the facet articular cartilage, cortical facet erosions, facet joint narrowing, and cortical thickening ( Fig. 34-10 ) . Cystic erosions or geodes may occur in the facets similar to those that occur in other joints involved by osteoarthritis (see Fig. 34-10; Fig. 34-11 ). Eventually the facet capsules become thickened and redundant. In the cervical region, joint capsular inflammation and capsular thickening occurs, which is most obvious in the lateral facet capsule. Pain-sensitive nerve endings (nociceptors) exist in the facet capsules and synovium. Simultaneously, bony spurs develop along the margins of the facet joint and the articular processes enlarge overall, as a reactive response to the chronic inflammatory osteoarthritic process (see Figs. 34-10 and 34-11 ).


These enlarged facets are readily visible on routine radiographs, computed tomography (CT) and MR images ( Figs. 34-10 to 34-13 ). The enlarged (hypertrophic) cervical facets contribute to cervical foraminal stenosis along with uncinate process enlargement related to degeneration of the uncovertebral joints ( Figs. 34-12 and 34-13 ) . Hypertrophic facets and uncinate processes can also narrow the transverse foramen and thereby cause localized narrowing of the vertebral arteries (see Fig. 34-12 ). Enlarged cervical facets do not encroach significantly upon the vertebral (central) canal as is commonly the situation in the lumbar region. Therefore, cervical facet hypertrophy does not contribute appreciably to cervical central canal stenosis. Cervical central canal stenosis occurs in the anteroposterior (AP) dimension and is secondary to disc bulging or protrusion, posterior vertebral osteophytes, thickened posterior longitudinal ligament, and thickened ligamentum flava.


Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree