Abstract
Fetal hepatic calcifications are present in less than 1% of pregnancies. They may be associated with aneuploidy and fetal/placental viral infections. When isolated, they are usually benign. This chapter reviews the epidemiology, pathophysiology, clinical and ultrasound presentation, and differential diagnosis of fetal hepatic calcifications.
Keywords
fetal liver, intrahepatic calcifications, liver calcifications, prenatal diagnosis, ultrasound, perinatal viral infections, aneuploidy
Introduction
Fetal hepatic calcifications are divided into three categories: peritoneal, parenchymal, and vascular. This chapter addresses parenchymal hepatic calcifications and, to a lesser degree, vascular calcifications, which may be included in the differential diagnosis of parenchymal calcifications.
Disorder
Definition
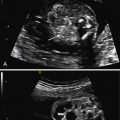
Fetal hepatic calcifications are single or multiple echogenic areas of various sizes (usually small, punctate) within the fetal hepatic parenchyma detected by ultrasound (US). They can be isolated or associated with other anomalies.
Prevalence and Epidemiology
In autopsy studies, intrahepatic calcifications (IHCs) are found in 2.2% to 4.2% of cases, and are often associated with aneuploidy and/or fetal anomalies. Most cases included in these studies are the result of spontaneous abortions, fetal demises, or termination of pregnancies for fetal anomalies. In contrast, and despite the near routine use of prenatal ultrasound, prenatal diagnosis of fetal IHC is less common, with an incidence of 1 : 260 to 1 : 1750. In a retrospective study of 24,600 routine US scans done between 14 weeks’ and 26 weeks’ gestation, Bronshtein and Blazer identified 14 cases of intrahepatic calcifications for an incidence of 1 : 1750 (0.057%). In another retrospective study, Achiron et al. reviewed 7500 routine US scans from 14 to 24 weeks’ gestation and reported five fetuses with liver calcifications (0.06% or 1 : 1666). Pata et al, reported a higher incidence (1 : 260) from a referral center where most ultrasounds are done for suspected fetal anomalies.
Etiology and Pathophysiology
Fetal intrahepatic parenchymal calcifications have classically been attributed to transplacental infection, vascular events, or hepatic tumors (primary or metastatic, benign or malignant); however, this was based on studies in neonates and a few prenatal case reports. With the now almost universal use of prenatal US, IHCs are often diagnosed prenatally either as an isolated finding or in association with other anomalies. Parenchymal liver calcifications have been linked to aneuploidy, particularly if other anomalies are present. In a large retrospective case-control study of autopsy specimens, 51% of the 85 fetuses with IHCs were aneuploid in contrast to 21% of those without IHCs. 17 Seventy-two percent of the fetuses with IHCs had associated anomalies, compared to 55% of the controls. In that study, the presence of a calcification in a fetus with malformation doubled the likelihood of aneuploidy compared to those without calcification. Vascular calcifications may result from calcified portal or venous clots secondary to either hypoperfusion or thromboembolism. The causes, outcome, and prognosis of prenatally diagnosed IHCs were not well established until studies of prenatal US were published.
In the largest six studies of prenatal diagnosis of fetal IHCs published in the literature since 1990, 44% of cases had associated anomalies, at least 11% were shown to have an abnormal karyotype (karyotypes were unavailable in one study and universally obtained in only one ), and 2.3% had a proven transplacental infection ( Table 23.1 ). At neonatal follow-up, 57% had a normal outcome. The prognosis was better in cases of isolated IHCs, with a survival rate of 90% to 100%. In cases of isolated IHCs, postnatal follow-up, when available, either confirmed the presence of calcifications or showed their disappearance. The etiology of isolated IHCs is unclear and has been attributed to vascular events or fibrosis by exclusion of other mechanisms such as infection or aneuploidy. Because viral serologies are not universally obtained in cases of isolated IHCs, it is also possible that transient infection from which the fetus may have recovered are underestimated. That question could be answered by a prospective trial.
| First Author (Year), Location | No. Cases | Incidence | GA at Diagnosis (weeks) | Associated Anomalies, n (%) | Aneuploidy, n (%) | Infection, n (%) | Normal Outcome, n (%) |
|---|---|---|---|---|---|---|---|
| Bronshtein (1995), Israel | 14 | 1 : 1750 | 14–26 | 3 (21) | 2 (14) trisomy 18 | 0 | 10 (71) |
| Achiron (1996), Israel | 5 | 1 : 2000 | 14–24 | 1 (20), attributed to vascular accident | 0 | 0 | 4 (80) |
| Simchen (2002), Canada | 61 | ? | ? | 40 (65) | 11 (18); 4 trisomy13, 2 trisomy 21, 2 trisomy 18, 1, 45,XO, 2 other | 2 (3.2); 1 CMV, 1 parvovirus B19 | 19 (31); 90% (19/21) if isolated |
| Stein (1995), United States | 33 | ? | 16–38 | 8 (24) | Unknown | 1 (3); CMV, NND at 3 months | 29 (87); 96% (24/25) if isolated |
| Koopman (1998), the Netherlands | 7 | 1 : 1037 | 20–32 | 2 (28) | 1 (14); trisomy 18 | 0; only 1 tested | 5 (71); 100% if isolated |
| Pata (2012), Turkey | 7 | 1 : 260 | 18–23 | 2 (28) | 2 (28) 1 Tri 18 1 Tri 21 | 0 all tested | 5 (71) 100% if isolated (5/5) |
| Total | 127 | 14–38 | 56 (44) | 14 (11) | 3 (2.3) | 72 (57) Higher if isolated |
a Note: Studies 4, 5, 7, and 8 are retrospective reviews of prenatal diagnosis of intrahepatic calcifications; studies 4 and 5 are general population studies. In studies 3 and 6, cases of intrahepatic calcifications in a referral population were followed prospectively.
Bronshtein and Blazer suggested that scattered nodular calcifications may indicate local hemorrhage rather than a thrombus, given the fact that even a small calcification in a 15-week fetal liver is much larger than the vascular diameter. These authors raised the possibility that regeneration of the liver and hepatic growth may explain the decrease in size and even disappearance of IHCs in some cases. This theory could explain why calcifications that are visible in a fetus are often no longer visible in the neonate.
In contrast to the aforementioned prenatal studies, one pathologic study of 1500 cases of spontaneous abortions showed a high incidence (90%) of vascular IHCs in the 33 cases reported ( Table 23.2 ). Of these fetuses, 85% had associated anomalies, in particular, “meconium intraluminal calcifications (27%), cystic hygromas (18%), and metaphyseal defects (18%).” Parenchymal or mixed (parenchymal and vascular) IHCs were present in only 9% of abortuses. Chromosomal studies were unavailable. Kidron and Sharony confirmed these findings in their retrospective review of 827 fetal autopsies, where the majority of the 35 cases of IHCs were of the vascular type. They suggest that fetal IHCs may be the result of circulatory compromise preceding death.